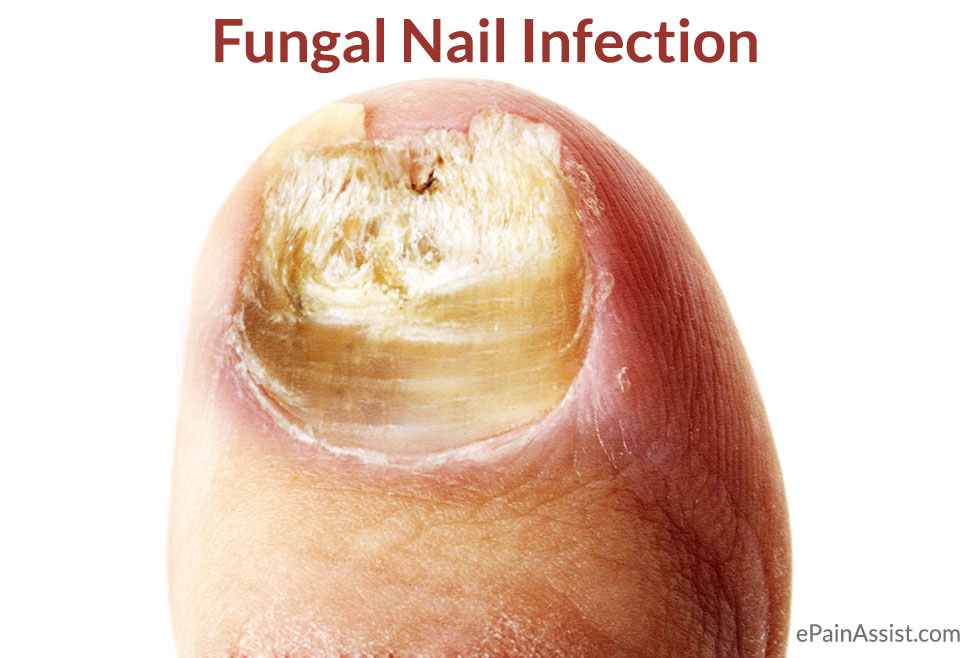
Fungal infection of the nail starts as a yellow or white spot beneath the tip of the finger or toenail. Fungal nail infection is more common in toe nails than finger nails.1 When the nail fungus extends deeper into the nail, it changes the nail color, and the nail thickens with crumbling or deteriorating edges. This condition can be quite unsightly, embarrassing and painful for the patient. Fungal nail infection is quite difficult to treat and the chances of recurrence are very high.
Treatment comprises of oral anti-fungal medicines, topical anti-fungal medicines, antifungal lacquer or nail polish, laser or photodynamic therapy and surgery.
Causes of Fungal Nail Infection
Fungus belonging to a category of fungi known as dermatophytes is commonly responsible for fungal nail infections. Other than this, molds and yeasts can also cause nail infections. Fungi are the microscopic organisms, which can survive without sunlight. Some fungi are beneficial, whereas, some are harmful and cause infection or illness. Fungi live in moist warm environments, such as swimming pools, shower rooms etc. They can enter the skin through any minor cuts or injuries, such as separation of the nail and nail bed. Continuous exposure of the nails to moist and warm environment causes the ideal environment for spread and growth of fungi.
Toenails are more prone to having fungal infection in them than fingernails, as they are more confined to warm, dark and moist environment inside the shoes creating a thriving environment for fungi.1 The blood circulation to the toes is also lesser when compared to the fingers making it harder for the immune system to identify and fight against fungal infection.
Risk Factors for Fungal Nail Infection
- Aging process is the commonest risk factor for fungal nail infection, as it causes diminished blood circulation, increased exposure to fungi, slow growth and thickening of the nails.
- Men are at an increased risk for fungal nail infection, especially those with a family history of fungal infection.
- Excessive perspiration increases the risk for developing Fungal Nail Infection.
- Wearing ill fitting or tight shoes and socks which restrict ventilation and do not absorb perspiration increases the risk for developing Fungal Nail Infection.
- Having other skin conditions such as psoriasis, athlete’s foot, increases the risk for developing Fungal Nail Infection.
- Individuals who walk barefoot in moist public places like gyms, swimming pools, shower rooms etc. are at an increased risk for developing fungal nail infection.
- Individuals who work in moist, humid environments are at a greater risk for developing Fungal Nail Infection.
- Skin or nail causing damage or other types of infection to the nails increases the risk for Fungal Nail Infection.
- Medical conditions such as diabetes or having circulation problems or a compromised immune system increases the risk for developing fungal nail infection.
- Individual suffering with chronic disease causing low immunity and body resistance like HIV infection.M
Signs and Symptoms of Fungal Nail Infection
- Thickening of the nail(s).
- The nail is dull in appearance without its healthy shine.
- There is discoloration of the affected nail due to accumulation of debris under the nail.
- The nail edge becomes ragged and brittle and starts to crumble.
- The shape of the nail becomes distorted.
- There may be separation of the affected nail(s) from the nail bed.
- Patient may also experience pain in the fingertips or toes with a slight foul odor.
Investigations for Fungal Nail Infection
Examination of the nail is done. Some of the debris is scraped from beneath the nail and sent for testing and culture to confirm the diagnosis. Other conditions, such as psoriasis need to be excluded as they can resemble a Fungal Nail Infection.
Treatment for Fungal Nail Infection
It is quite difficult to treat a fungal nail infection and moreover it can be very persistent with a high tendency of recurrence. Over-the-counter antifungal nail ointments and creams can be used; however, they are not very effective. If a patient has athlete’s foot along with nail fungus, then the athlete’s foot should be treated first with topical medication.
- Oral medications such as itraconazole (Sporanox) and terbinafine (Lamisil), are prescribed, especially if the patient has diabetes or has risk factors for or a history of cellulitis. Oral anti-fungals are also prescribed if the patient is having pain or discomfort in the affected nail. Azoles and allylamines are widely used to treat the fungal infection of nails.N These medications should be taken for six to 12 weeks, and it takes more than four months to eliminate the infection. Side effects of antifungal medications include skin rashes and liver damage. These medications are not recommended for patients having congestive heart failure or liver disease.
- Antifungal lacquer or nail polish, such as ciclopirox, is prescribed for mild to moderate fungal infection of the nail. This medicine is painted on the affected nail(s) and the surrounding skin. After a week, the buildup of the medicine is cleaned using alcohol and fresh application of the medicine is started.
- Topical antifungal medications can be used with oral medications.N The doctor will debride some of the affected part of the nail before the patient starts using topical antifungal. This will increase the efficacy of the medicine. Newer more effective topical medications are under investigations and shows better outcome after topical therapy.P
- Surgery is recommended if the fungal nail infection is causing severe pain. The infected nail is removed so that a new nail will grow in its place; however, it can take almost a year for the new nail to completely grow back. Surgery can also be done in combination with the medicine ciclopirox for treating the nail bed.
- Laser or photodynamic therapy can also be done to treat nail fungus. However, this is a relatively new treatment and is not available easily.
Home Remedies and Prevention of Fungal Nail Infection
- Soaking your affected nails of hands or feet for about 15 to 20 minutes in a liquid mixture containing 1 part vinegar and 2 parts lukewarm water may help with the fungal infection. Rinse well after soaking and gently pat your hands or feet dry.
- Applying Vicks VapoRub on the infected nails can help; however, there is no concrete proof for its effectiveness.
- Always keep your nails trimmed and dry.
- Cut your nails, straight across, especially the toe nails.
- File the thickened areas.
- Dry your hands and feet thoroughly after a bath, especially the areas between the toes.
- Take off your shoes a couple of times during the day and especially after exercise to air your feet.
- Wear the right socks, which can absorb the sweat and moisture.
- Sprinkle some antifungal powder on your feet and inside your shoes.
- Try alternating open-toe shoes with closed-toe shoes.
- Avoid picking or trimming the skin surrounding your nails.
- Always wear rubber gloves when doing the dishes or other work involving water.
- Never, ever walk barefoot in public places such as showers, gym, pools, locker rooms etc.
- Avoid the use of nail polish and artificial nails, as they can trap moisture under them and cause or worsen an already existing fungal infection.
- Get manicure and pedicure done at a reputable salon.
- Always wash your hands after application of medicine or touching an infected nail, as the fungus can spread from one nail to another.
References:
J Drugs Dermatol. 2013 Jul 1;12(7):s96-103.
Onchomycosis: an overview.
Elewski BE1, Rich P, Tosti A, Pariser DM, Scher R, Daniel RC, Gupta AK.
1. Improvement in onychomycosis after initiation of combined antiretroviral therapy.
Moreno-Coutiño G1, Arenas R, Reyes-Terán G.
Int J Dermatol. 2013 Mar;52(3):311-3.
2. Improvement in onychomycosis after initiation of combined antiretroviral therapy.
Moreno-Coutiño G1, Arenas R, Reyes-Terán G.
Int J Dermatol. 2013 Mar;52(3):311-3.
3. Emerging therapeutic agents for onychomycosis.
Piérard GE1, Arrese JE, Quatresooz P, Piérard-Franchimont C.
Expert Opin Investig Drugs. 2007 Feb;16(2):157-67
4. Recent progress on the topical therapy of onychomycosis.
Alley MR1, Baker SJ, Beutner KR, Plattner J.
Expert Opin Emerg Drugs. 2007 Sep;12(3):345-53.
Also Read:
- Athlete’s Foot or Tinea Pedis: Symptoms, Causes, Treatment, Prevention- Cotton Socks
- Onychomycosis: Causes, Symptoms, Treatment, Home Remedies, Prevention, Diagnosis, Signs
- Scalp Conditions that Cause Hair Loss & its Treatment
- Jock Itch: Causes, Symptoms, Treatment, Home Remedies|Is Jock Itch Contagious and How long Does Jock Itch Last?
- Tinea Barbae: Causes, Symptoms, Treatment, Prevention
- What is Tinea Unguium, Know its Causes, Symptoms, Treatment, Prognosis, Pathophysiology, Diagnosis
- Is Dermatophytosis Contagious?|Causes, Symptoms, Treatment, of Dermatophytosis