What is Lactation Mastitis?
Lactation Mastitis is an infection affecting the tissue of the breast resulting pain in the breast, redness, warmth and swelling. Chills and fever may appear as a result of the infection. Breast feeding mothers are those who are commonly affected by this infection and hence the name lactating mastitis.
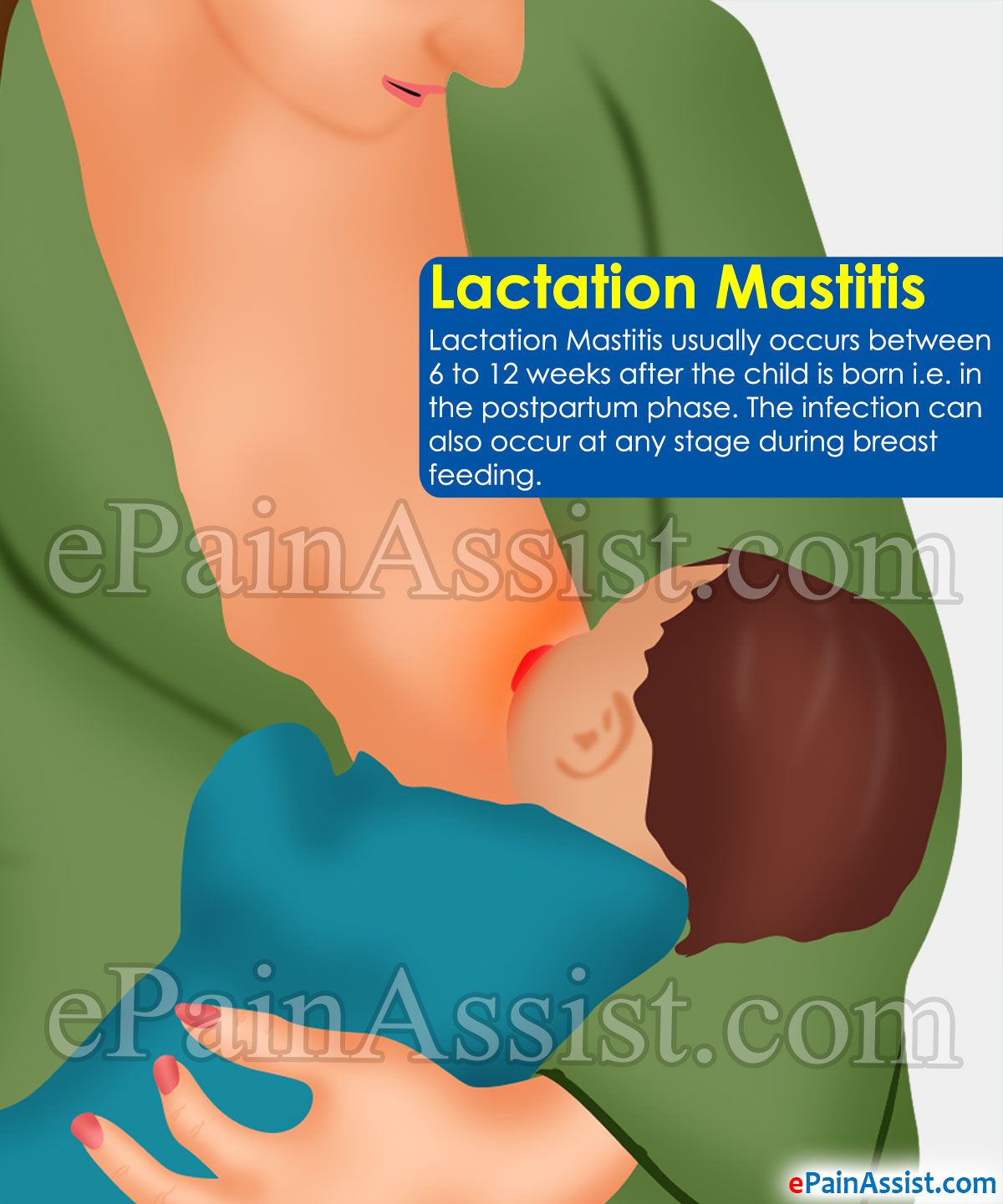
Lactation Mastitis usually occurs between 6 to 12 weeks after the child is born i.e. in the postpartum phase. The infection can also occur at any stage during breast feeding. You will always be demoralized by this condition and as a result it might be so hard for you to take good care of your child. Nevertheless, this condition can also affect women who are not lactating.
Mothers are often forced by mastitis to wean their babies before the right time. You can breast-feed your baby despite the fact that you are taking mastitis antibiotics.
Causes of Lactation Mastitis
It is a technique to breastfeed properly and poor skills leads to the breast milk being trapped in the breast. This is the main cause of mastitis. Other causes for lactation mastitis are:
- A milk duct being blocked: If a breast is clogged due to failure of a duct to empty completely causes infections as a result of milk backing up.
- If bacteria enter your breast: If the nipple’s skin is broken and a bacterium enters the duct your breast. This can be from the baby or from the surface of your skin. Stagnant breast milk is ground for the bacteria to breed. The milk has antibacterial effects and that usually protect your infants of any infections.
Signs and Symptoms of Lactation Mastitis
Signs and symptoms of lactation mastitis always appear rapidly. This includes:
- Tenderness of breast and warm when touched.
- Feeling sick (malaise)
- The swelling of the breast
- A sensation that is burning or painful in the course of breast-feeding.
- Wedge-shaped pattern of skin redness
- A bad fever of up to 38.3C/101F or more.
At any stage of breast feeding, lactation mastitis can occur. This is despite the fact that it is commonly occasioning during the first few weeks after birth. One breast is usually affected by lactation mastitis.
When to Visit the Physician for Lactation Mastitis?
Symptoms that are like flu will always be there. This is before you notice that some part of your breast is tender and red. It will be good for you to contact a doctor immediately when you realize these signs.
You will probably be tested before any diagnosis by the doctor. This condition is always treated effectively by using antibiotics. If you have a history of lactation mastitis then your doctor can even give the prescription via a phone. You must report to the doctor if the condition does not change after two days of oral administration of the antibiotics. There might be another more serious condition that you might be having.
If I Am Suffering from Lactation Mastitis Should I not Breast Feed?
You are encouraged to continue breast feeding even during the worst inflammation. You will be able to prevent the milk from blocking further the breast duct by continuing to breast feed even if it is painful. Your child needs to be able to get the nutrition they need also. In the course of this process, you will be able to bear this condition further because of relaxation of the reflex and you can now tolerate the paining situation.
You can pump your breast if the baby fails to finish the milk in the breast that is inflamed. You can pump the milk from your breast and feed the baby with it through a bottle. This is when the lactating process proves hard to bear. Your baby is the only individual who can sufficiently pump milk out of your breast. Thus you do not have to rely on the pumping process for effective outcome.
Will the Baby be Affected Because of My Lactation Mastitis?
The supply of milk from the affected breast can be affected adversely but your baby cannot be harmed by the breast milk.
An obstetrician-gynecologist, a nurse practitioner or a doctor will the person you are likely to have your first appointment with. A lactation consultant is another person with you can have an appointment with if you have an issue relating to nursing.
Risk Factors for Lactation Mastitis
The risk factors that accompany lactation mastitis are:
- The process of lactation in the first couple of weeks after giving birth.
- Despite the fact that lactation mastitis can accrue due internal infection which is not a guarantee that the skin cracks, there could be sores that are evident in your skin.
- Carrying heavy luggage, using a tight seat belt, or wearing a tight bra is some of the few examples of the things that might restrict the flow of milk and give such indication of this disease.
- Easily becoming stressed or tired throughout.
- If you have previously suffered from lactation mastitis.
- Insufficient nutrients in your diet.
Tests to Diagnose Lactation Mastitis
Physical examination will determine the diagnosis which the doctor is going to administer for you. The doctor must inquire into the signs of the disease. Issue like fever, breast pain and chills are some of the inquiries the doctor has to be sure of. Another symptom will be the fact that there is going to be a tender area around the nipple that is red and is wedge-shaped.
Breast abscess is another condition that a doctor must ascertain that you do not have. This is another condition that occurs when mastitis is treated late when it has escalated. The history of your lactation might help the doctor to discern the best antibiotics to prescribe for you. This is especially when your condition has become severe.
Mastitis can often be confused with breast cancer. This is a rare inflammatory breast cancer that affects the breast and also causes swellings and redness like mastitis.
Treatment for Lactation Mastitis
The process of treating lactation mastitis often includes:
- Antibiotics. A prescription of 10 to 15day course of antibiotic is recommended for the treatment of lactation mastitis. It can take a short span of only 24 hour of antibiotic usage for you to feel well once again. In order to minimize the risk of lactation mastitis recurring, it is advisable to finish all the prescribed bills.
- Pain relievers. A mild reliever of pain can be recommended by a doctor. Ibuprofen (Motrin IB, Advil and others) and acetaminophen (Tylenol and others) are examples of the mild pain killers.
- You should adjust with you nursing technique. Ensure that your child is able to feed in the right manner and also you must confirm that the milk in your breast is fully emptied. If you need any support your doctor can refer you to a lactating consultant. The physician can also consider to reviews the technique that you apply when breast-feeding.
- You should promote your body to fight the infection by drinking a lot of fluids. This process is known as self-care. You ensure that you continue breast feeding and get enough rest.
It is very important to go back to the doctor if the lactation mastitis has not cleared.
Breast Feeding with Lactation Mastitis
The duration which lactation mastitis can be shortened will depend on your breast feeding technique even after you have started using antibiotics.
In the course of treatment or when you are feeling unwell you should not stop but to continue breast feeding your child. Your child will pump the milk from your breast most effectively than any other mechanism you may opt to use. The digestive system of your baby will destroy any bacteria that might be found in your breast milk.
- Place a warm soft cloth on your breast for approximately 15 minutes prior to breastfeeding your baby. You should do this thrice daily. By massaging the breast that is affected with lactation mastitis,the chances of increasing the flow of milk is surely high.
- You should enable your child to feed on both breasts. It is essential to empty the affected breast. Thus you should always ensure that you start with the ailing breast. If the process of beginning with the affected breast proves to be painful you start with the healthy breast until the milk starts flowing then you switch to the affected breast. Ensure that the baby has completely emptied the lactation mastitis affected breast before switching to the healthy one.
- Sometimes the sore on the nipple is painful and might prevent you from giving the baby to feed on. You should be able to pump out all the milk in it.
- A cracked or sore nipple can be creased with lanolin-based cream like Lansinoh.
- You nursing pads should also be frequently replaced in order to enable for dryness and cleanliness of the breast.
Complications for Lactation Mastitis
Failure to treat lactation mastitis adequately will result in collection of pus/abscess and in turn your breast will thicken and become firm. Immediately you notice evident complication while you are breastfeeding, you should be able to tell your physician about it.
Lifestyle Changes for Lactation Mastitis
It is advisable to continue nursing with lactation mastitis so as to get rid of the infection.
Relieve Your Discomfort of Lactation Mastitis by Adding Few Changes to Your Lifestyle
- If your child is hungry do not hesitate to breast feed.
- Frequent feeding will only be encouraged if you take enough rest with your baby in bed. Rest is therefore encouraged.
- Do not wait always until your breast is clogged with milk so that you start feeding.
- Try to take different positions while breast-feeding.
- You should take fluids in plenty.
- If emptying a portion of your breast proofs hard, shower or apply a warm cloth on that side before you pump the milk.
- A supportive bra should be worn.
Prevention of Lactation Mastitis
Lactation consultant should be able to give you the right direction regarding how you should start your nursing process. This will enable you avoid future lactation mastitis. They will give valuable advice and tips on how to begin breast feeding.
How to Minimize Chances of Being Infected with Lactation Mastitis?
Follow the below tips in order to prevent lactation mastitis
- Emptying milk from the breasts.
- The baby must fully drain the milk from one breast in order to switch to the other.
- The position you feed on should be constantly changed.
- Ensure that your child latches on in the proper manner when feeding.
