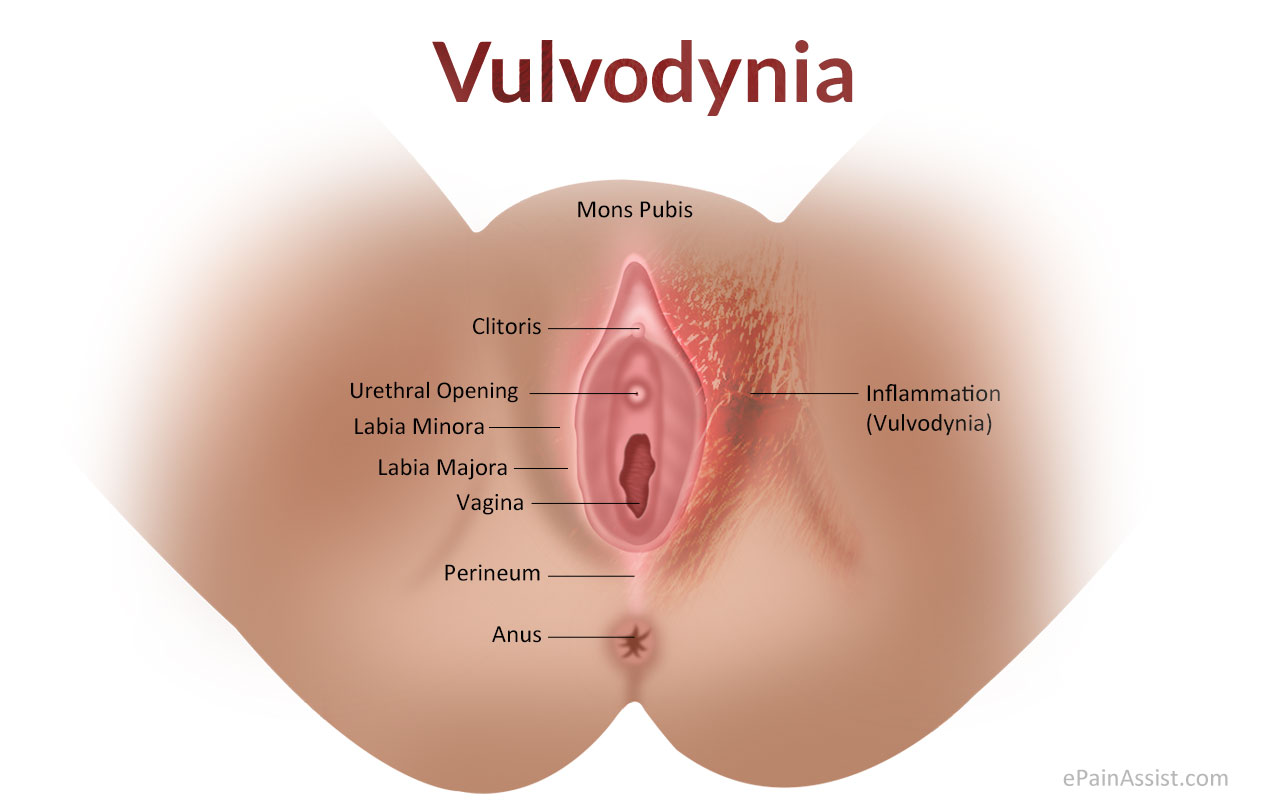
The outer part of female genitalia is termed as vulva. Any sort of inflammation to this area is termed as vulvitis.
Vulvodynia is type of multifactorial chronic pain condition, the origin of which is not yet known, which is characterized by burning of the vulva along with stinging, irritation, and rawness. For females with Vulvodynia, common symptoms include constant pain or burning along with itching of vulva. These symptoms can sometimes be so excruciating that it may cause dyspareunia making sexual intercourse extremely painful. There is practically no tissue damage, discharge, infection, or fungus which means that on examination practically nothing is observed except for chronic inflammation.
When physical examination shows only chronic inflammation in the vestibule, vulvodynia should be suspected. Vulvodynia is a burning, irritation, stinging, or sharp pain that occurs in the vestibule. Such pain can last for short periods of time or be persistent, but vulvodynia is usually defined as lasting at least three months. The symptoms of persistent pain, burning and itching can be so severe that it makes sexual intercourse impossible or at least very difficult. The symptoms of vulvodynia can occur in a small area or may affect the entire vulvar area. Pain can occur before, during, or after sexual activity, when tampons are inserted, or even when wearing underwear or trousers. The pain can also occur for no apparent reason.
Vulvodynia is not associated with sexually transmitted diseases (STDs) or STD risk factors, but affected women often have been treated repeatedly for candidal vulvovaginitis. In the past, it was theorized that the pain of vulvodynia was due to psychological issues. However, recent data indicate that women with vulvodynia are psychologically comparable to women without the disorder and are no more likely to have been abused. Marital satisfaction levels also are similar.
Classification and Types of Vulvodynia
There are two types of Vulvodynia – Vulvar Vestibulitis Syndrome in which there is a painful response upon touch around the vaginal opening and Dysesthetic Vulvodynia in which there is a generalized pain, which is usually unprovoked. Vulvar pain can affect women of any age.
In Vulvar Vestibulitis Syndrome, females experience a sharp stabbing pain on palpation at certain spots at the vaginal opening where major vestibular glands are situated. On examination with an instrument, there is observation of localized point tenderness.
Dysesthetic Vulvodynia in comparison with Vulvar Vestibulitis Syndrome is much less common. In this, the pain is in the form of a spontaneous burning sensation, at times all over the vulva and even down legs. Since it is often associated with menopause, hence there may be a hormonal component to it.
Epidemiology Of Vulvodynia
It is estimated that around 28 to 30% of the U.S. female population suffers from this condition at some point in their lifetime. Specifically, national telephone surveys assessed prevalence of vulvar symptoms in an ambulatory care setting (4%) and the general population (9.9% lifetime, 3.8% current), respectively. These studies also identified associations between vulvar symptoms and other chronic conditions, with a history of chronic vulvovaginal infections and depression as the strongest predictors of vulvar pain. A case-control survey of women with a confirmed diagnosis of vulvodynia yielded similar results. A comparison of symptomatic and diagnosed women illustrates commonalities in health history, pain characteristics, and impact of pain on lifestyle, indicating that the symptomatic population identified from the general population is a good representation of women who may suffer from vulvodynia. Multivariate models demonstrate that the strongest predictors of a diagnosis based upon symptoms are a combination of physical and psychological factors, including pain with speculum insertion, abstaining from intercourse, and fearing intercourse because of vulvar pain. It is anticipated that these findings will serve as a basis for developing a screening tool that identifies women who experience chronic vulvar pain that may be indicative of vulvodynia. When considered together, these three survey studies further the understanding of the prevalence of chronic vulvar symptoms and provide insight regarding predictors of both symptoms and a diagnosis of vulvodynia in the general population.
Pathophysiology of Vulvodynia
The pathophysiology of vulvodynia may relate to soft tissue irritation. Under such circumstances, the body activates a number of defenses. The tissue becomes inflamed to prevent further contact. New nerve endings grow and become hypersensitive so they can detect further contact and withdraw. Blood vessels in the area constrict to prevent possible infection from spreading. Finally, muscles produce spasms in the pelvic floor that reduce blood flow and produce further inflammation.
Etiology And Risk Factors Of Vulvodynia
Vulvodynia is a pathological condition which has numerous and ill-defined antecedents. Very little is known about the biological processes which lead to the development of Vulvodynia along with its long-term sequelae. The factors which prompts an individual to seek care and the diagnostic criteria by which a physician formulates treatment or therapy is not constant. Affected patients commonly experience pain with sexual intercourse, constant vulvar irritation along with burning and pain. There may also be symptoms associated with urinary and GI tracts. Additionally, diagnostic criteria which define categories and subsets of Vulvodynia are neither adequately defined nor utilized on a consistent basis by physicians. While the true occurrence of Vulvodynia still remains not known, there are several common diagnostic subsets that are recognized to include
- Vulvar Vestibulitis.
- Dysesthetic Vulvodynia.
- Vulvar dermatitis.
Vulvar Vestibulitis which is thought to be the most common subtype has been observed in approximately 15% of people in some studies. While histologic studies indicate a chronic inflammatory reaction, the exact cause of this inflammation as well as its significance remains unclear. It has also been proposed in some studies the role which a pelvic floor dysfunction plays in acting as a catalyst for development of vulvar pain syndromes, Dysesthethic Vulvodynia to be precise but its exact impact is still uncertain. The studies also make a comment on the effect of neurophysiological parameters as a potential association which should be taken into account.
Signs and Symptoms of Vulvodynia
10 – 16% of women have complained of vulvar pain lasting three months or more. Vulvar pain can affect women of any age. This pain might be secondary to yeast or herpes infections, traumatic incidents like sexual assaults, pathological conditions like Behcet or Crohn’s disease, precancerous conditions, irritants like soaps, and skin abnormalities like dermatitis and psoriasis.
It is said that among the many theories about what causes vulvodynia, the most likely is a response to tissue abnormality, possibly caused by infection, irritation, or trauma long after it’s been resolved.
Symptoms vary greatly among patients and may be localized or diffuse, superficial or deep, and constant or intermittent. Pathologic findings are limited to vulvar erythema, and the diagnosis is one of exclusion.
Treatment of Vulvodynia
Surgery has been reported to be a successful intervention for selected cases of vulvar vestibulitis, and is reserved for women with severe and long-standing symptoms. However, optimum surgical management is still undetermined and very few well-designed, long-term studies document the outcome of surgical procedures. In addition, pharmacological and behavioral therapies would benefit from treatment standardization and prospective clinical studies.
Despite treatments with surgery, pharmaceutical therapies, psychological treatments, physical therapy, and pain management therapy like biofeedback and behavioral modification, still there is no consensus as to which procedure or procedures gives the maximum amount of benefit with patient satisfaction to an affected individual. A combination of therapies is frequently utilized and, while there are several options available for the treatment of vulvodynia, most of the literature supports the conclusion that cures for vulvodynia are uncommon and a specific inciting cause can be diagnosed in a relatively small percentage of patients. Consideration of these factors must be an integral part of the management of patients with vulvodynia and this underscores the need to examine this condition in a multidisciplinary context.
Prognosis for Vulvodynia
The natural history of vulvodynia is not clear. Many women complain of this disorder for years, and it traditionally has been considered chronic. However, recent data suggest that approximately one half of women who report that they have had prolonged vulvar pain no longer have symptoms of vulvodynia. Hence, it is reasonable to think that symptoms in a substantial proportion of women with this disorder may abate. The prognosis for women who receive appropriate treatment is quite good. A follow-up study of 104 women seen in two referral clinics at a university suggests that most women with vulvodynia experience substantial improvement with medical treatment.