What is Abdominal Angina?
Abdominal angina is a condition where an individual feels pain in the abdomen after having a meal. This is caused due to inadequate blood supply, which cannot meet the demands of the mesenteric visceral. This condition is named as “angina” in relation to angina pectoris because of the similarity in the symptoms where angina pectoris is caused by coronary artery obstruction. The similarity between abdominal angina and angina pectoris is that in both these conditions the pain is caused due to insufficient blood supply. Otherwise both these conditions are completely different.
Atherosclerosis or narrowed blood vessels commonly cause abdominal angina, where there is a buildup of plaque resulting in narrowed blood vessels and deficient blood supply. Cigarette smokers are at a higher risk for developing this condition. Abdominal angina is not a very common condition and women suffer more from this condition than men. Abdominal angina is also known as intestinal angina.
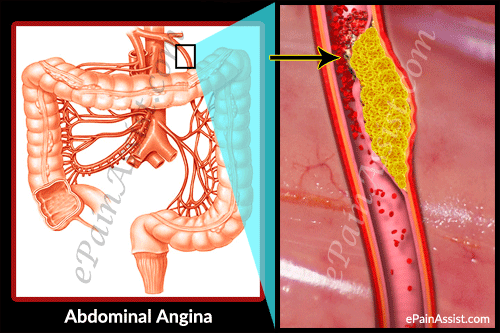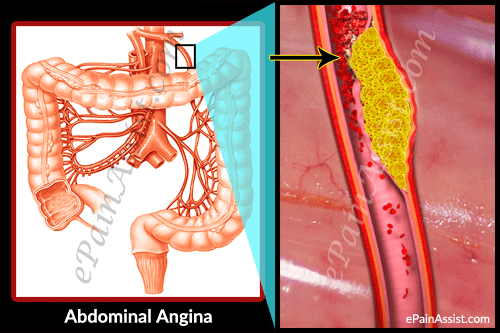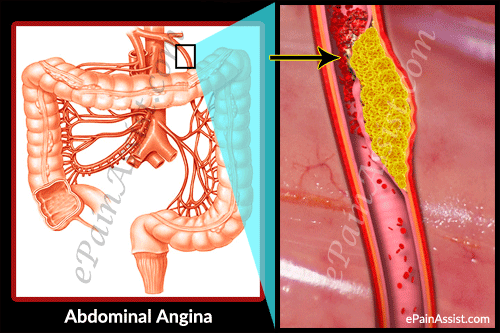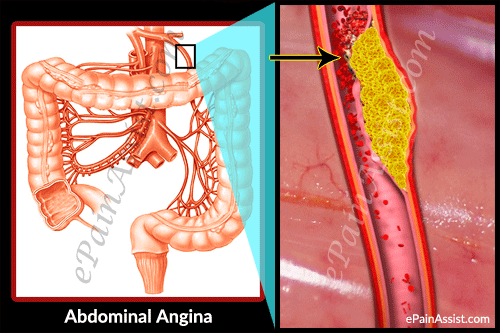
Causes and Pathophysiology of Abdominal Angina
The pathophysiology of abdominal angina resembles angina pectoris and intermittent claudication. Abdominal angina is commonly caused by atherosclerotic vascular disease, where there is obstruction in the ostia and few centimeters from the origin of the mesenteric vessels. This condition can occur with carcinoid, aortic coarctation and antiphospholipid syndrome. Smokers are at a higher risk for developing this condition so smoking is a big risk factor. Women are more prone to develop this condition than men. Abdominal angina is commonly seen in individuals aged above 60 years.
Abdominal Angina Symptoms:
- Abdominal angina symptoms may include severe and crippling pain in the mid-epigastric or central abdominal region occurring within 10 to 15 minutes after consuming a meal.
- Cramping is felt in the abdomen, especially in the mid-region.
- Nausea and vomiting.
- Patient may feel anxious.
- Patient may be constipated or may have diarrhea.
- The pain may continue for many hours as the digestive system is exerted, due to decreased blood supply, in order to digest the food.
- Upon palpation, the abdomen often feels hollow and soft.
- Patients may also experience weight loss, as they eat less to avoid pain which occurs after consuming a meal. They tend to develop an aversion to food.
- There are signs of peripheral vascular disease, especially aortoiliac occlusive disease.

Treatment of Abdominal Angina
Treatment for abdominal angina depends on the cause, the affected region and the amount of tissue damage.
- If the cause is colonic ischemia, antibiotics are given to control or prevent infections that have resulted from abdominal angina.
- If the cause of abdominal angina is heart failure, hyperlipidemia, dysrhythmia or hypertension, then medications are given accordingly and the patient is advised on diet and exercise.
- It is recommended that patient consume frequent, small meals so the load on the digestive system is lessened.
- Surgery is required depending on the degree of arterial occlusion and tissue damage. If there is necrosis, then the tissue needs to be removed via surgery. In case of severe occlusion or blockage, the affected artery is bypassed to restore perfusion.
- If the cause is acute mesenteric artery ischemia, then surgery is done where the obstructed vessel is bypassed or the obstruction is removed.
- Medications such as vasodilators and anticoagulants are often given with surgery to help with recovery process.
- Surgery is also done if the cause is chronic mesenteric artery ischemia.
- If the patient is not able to tolerate an open surgical procedure, then endovascular mesenteric revascularization can be done.
- Stents are often used to ease the obstruction instead of bypassing the affected vessel.
- If ischemia has occurred as a result of mesenteric venous thrombosis, then surgery is not necessary. The patient is started on anticoagulants for about 3 to 6 months in order to prevent the formation of new clots. Surgery is done only if there is any damage to the mesenteric tissues.
- Catheterization/angioplasty can also be done to widen the narrowed blood vessels. Open surgeries are also done, though rarely.
- Percutaneous transluminal angioplasty (PTA) can be done in some patients.
- Patient is advised on the right diet, i.e. eating healthy food, so as to regain the lost weight. Healthy eating also prevents the cholesterol levels from rising.
- If the patient is a smoker, then quitting the smoking is highly recommended.
- StatPearls. (2022). Chronic Mesenteric Ischemia. https://www.ncbi.nlm.nih.gov/books/NBK459339/

