What Is Pseudomembranous Colitis?
Pseudomembranous Colitis is a medical condition in which the colon gets inflamed in association with excessive intake of antibiotics. Pseudomembranous Colitis is also known by the name of Antibiotic-Associated Colitis or C. difficile colitis. The inflammation of the colon is more often than not caused by overgrowth of the bacterium Clostridium Difficile. In some cases, severe forms of Pseudomembranous Colitis can become life-threatening; however this condition can be successfully treated.
What Are The Causes Of Pseudomembranous Colitis?
Pseudomembranous colitis develops when the bacteria present in the colon, normally C. difficile, start releasing toxins thus irritating the colon and causing it to inflame. Under normal circumstances, the harmful bacteria present in the body is kept under control by the healthy bacteria also present in the body, but if an individual takes excessive antibiotics for some form of medical condition or if this balance of harmful and healthy bacteria gets affected causing overgrowth of harmful bacteria then this results in the condition called as Pseudomembranous Colitis. This condition can be caused by any antibiotic but some of the antibiotics usually taken that can cause Pseudomembranous Colitis are:
- Cipro
- Levaquin
- Penicillin
- Cleocin
- Cephalosporins
Even though antibiotics are the medications that most commonly result in development of Pseudomembranous Colitis, there are certain other classes of medications that also have the potential to cause Pseudomembranous Colitis. Individuals undergoing chemotherapy are also prone to develop Pseudomembranous Colitis. Also, individuals with medical conditions like ulcerative colitis or Crohn’s disease are at increased risk for developing this condition.
What Are The Symptoms Of Pseudomembranous Colitis?
Some of The Symptoms of Pseudomembranous Colitis Are:
- Watery diarrhea
- Abdominal pain along with cramping
- Fever
- Mucusy stools
- Nausea
- Dehydration
If an individual experiences the above symptoms within a couple of days of starting an antibiotic then it may be a classic sign of Pseudomembranous Colitis and the individual should seek medical attention to stop taking that antibiotic.
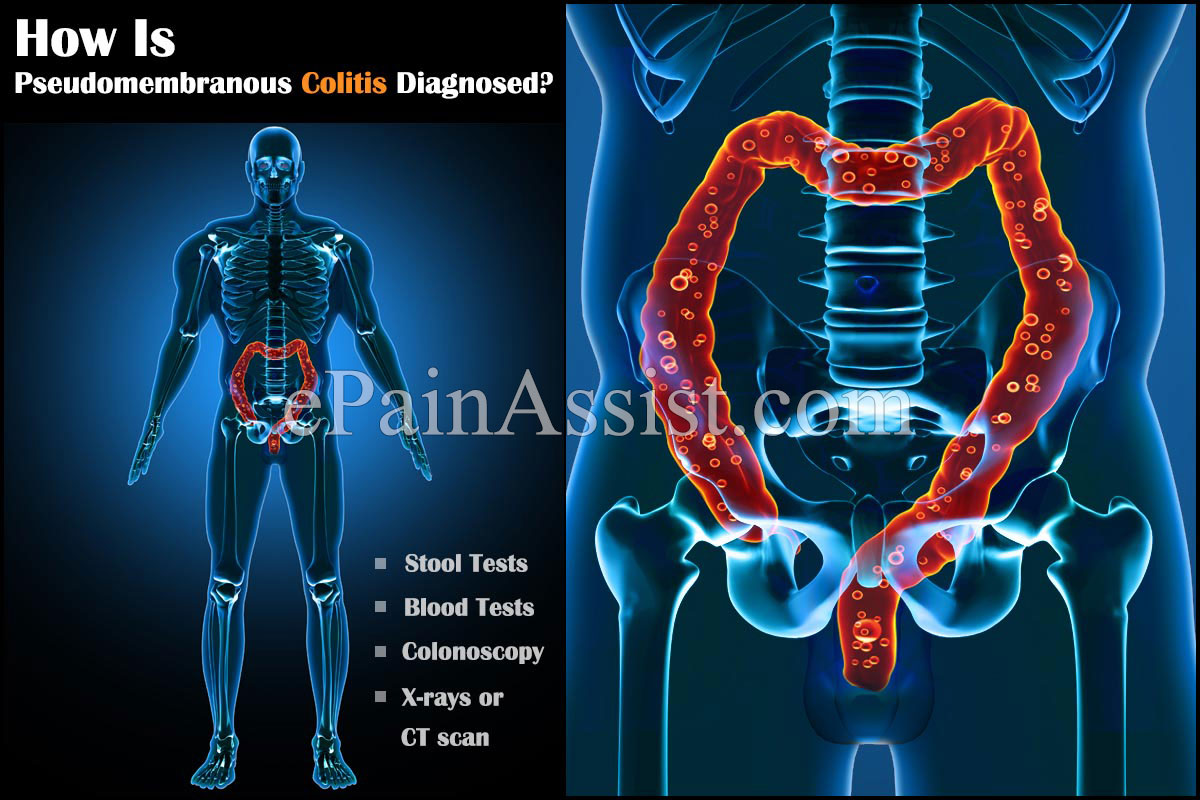
How Is Pseudomembranous Colitis Diagnosed?
Some of the tests done in order to diagnose Pseudomembranous Colitis are:
- Stool Tests: Testing the stool can help determine presence of excess C. difficile in the body.
- Blood Tests: This will show elevated levels of white blood cells which is also a sign of Pseudomembranous colitis.
- Colonoscopy: This is a procedure in which a tube with a minute camera is inserted inside the colon through the rectum to look at the internal structures of colon. This examination can definitively determine presence of inflammation in any part of the colon.
- Imaging Studies: Imaging studies like abdominal x-rays or a CT scan of the abdomen can also be done in severe cases to look for other complications.
What Are The Treatments For Pseudomembranous Colitis?
The treatment for Pseudomembranous Colitis starts with stopping the antibiotic which started the symptoms in the first place. In most cases, this is enough in controlling the symptoms and resolving the condition. If the symptoms are still not appropriately controlled, the physician may recommend switching to a different antibiotic, which has properties to fight effectively against C. difficile. It may sound unusual to treat a medical condition caused by antibiotic to treat with another antibiotic but switching to an antibiotic which can destroy C. difficile will allow healthy bacteria to grow back and restore balance between harmful and healthy bacteria. These antibiotics are either given orally or intravenously in a hospital setting depending on the severity of the symptoms. Once treatment kicks in, the symptoms start to resolve within a few days.
In case of Pseudomembranous Colitis recurs post-treatment then the following options are available for treatment:
- Further Administration of Antibiotics: The physician may prescribe another round of antibiotic to treat the condition
- Surgery: A surgical procedure may be done in individuals who end up having rupture of the colon or a medical condition called peritonitis. The surgical portion involves removing part of the diseased colon.
- Fecal Replacement Therapy: In this form of therapy healthy stool from a member of the family of the affected individual is inserted on the colon of the patient. This healthy stool then facilitates growth of healthy bacteria in the colon thus restoring balance between healthy and harmful bacteria thus treating the condition.
- Mayo Clinic Staff. (2019). Clostridium difficile infection. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/c-difficile/symptoms-causes/syc-20351691
- Haines, C. F., & Sears, C. L. (2014). The epidemiology of Clostridium difficile‐associated disease. Clinics in Colon and Rectal Surgery, 27(03), 231-236.
- Leffler, D. A., & Lamont, J. T. (2015). Clostridium difficile infection. New England Journal of Medicine, 372(16), 1539-1548.
- Gerding, D. N., Johnson, S., Peterson, L. R., Mulligan, M. E., & Silva Jr, J. (1995). Clostridium difficile–associated diarrhea and colitis. Infection Control & Hospital Epidemiology, 16(09), 459-477.
- McFarland, L. V., Surawicz, C. M., Stamm, W. E., & Elmer, G. W. (1990). Risk factors for Clostridium difficile carriage and C. difficile–associated diarrhea in a cohort of hospitalized patients. Journal of Infectious Diseases, 162(3), 678-684.
- Guh, A. Y., Kutty, P. K., & CDC Prevention Epicenter Program. (2018). Clostridioides difficile infection. Annals of Internal Medicine, 169(7), ITC49-ITC64.
- Dubberke, E. R., & Olsen, M. A. (2012). Burden of Clostridium difficile on the healthcare system. Clinical Infectious Diseases, 55(suppl_2), S88-S92.
- Johnson, S. (2017). Clostridium difficile infection: update on epidemiology, risk factors, and therapeutic options. Current Infectious Disease Reports, 19(1), 1-9.
- Freeman, J., Bauer, M. P., Baines, S. D., Corver, J., Fawley, W. N., Goorhuis, B., … & Wilcox, M. H. (2010). The changing epidemiology of Clostridium difficile infections. Clinical Microbiology Reviews, 23(3), 529-549.

