Chronic liver diseases produce, independently of their etiology, a progressive accumulation of collagen fiber in the hepatic parenchyma. The appearance of regeneration nodules alters the hepatic architecture and produces an increase in the portal pressure. The significant increase in body pressure is the cause of the appearance of esophageal varices and ascites, which worsens the prognosis of the disease.
The quantification of hepatic fibrosis has been done, for years, by histological analysis of a small sample of liver tissue (obtained percutaneously or transjugularly). However, the reliability of the biopsy for fibrosis is limited. The sample of liver tissue represents only a part of 50,000 parts of the liver, the distribution of the fiber can be heterogeneous, but it is worth mentioning that correct process of the sample and an observer for its identification are required.
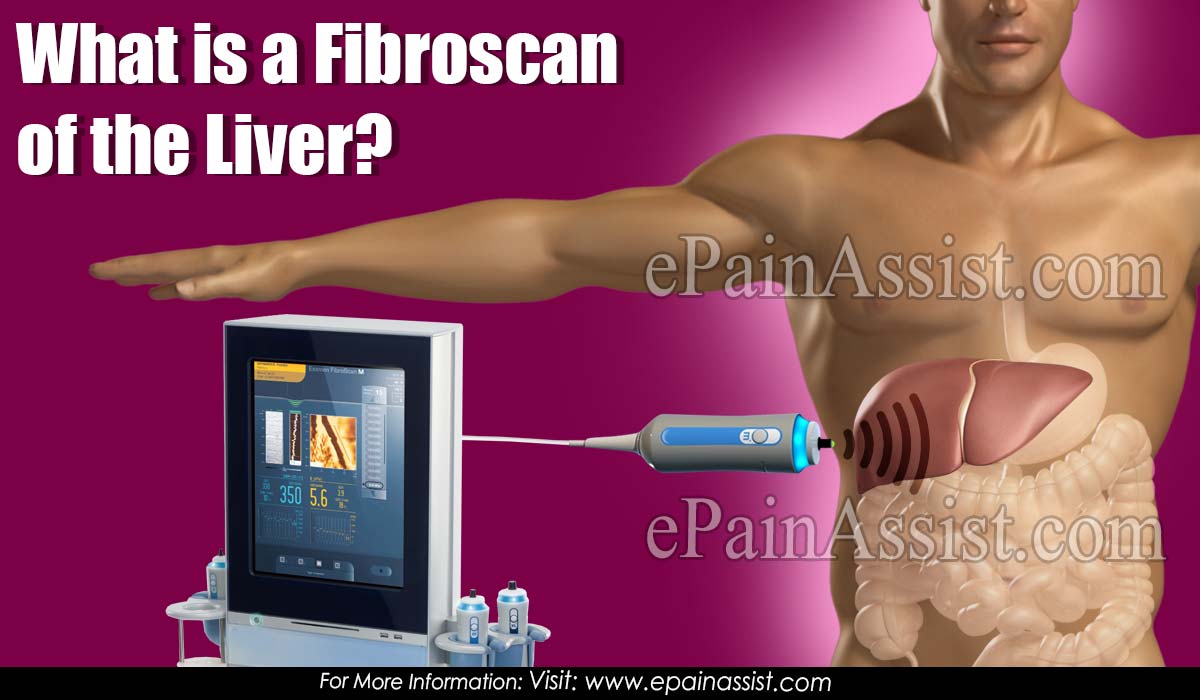
What is a Fibroscan of the Liver?
The limitations of the biopsy and the periodic evaluation of the patient have prompted the search for non-invasive alternatives to assess the degree of liver fibrosis. In recent years, a large number of serological markers have been identified that are directly or indirectly involved in the process of liver fibrosis. Specific programs have been developed to increase the reliability of detection of liver fibrosis with the use of existing radiological techniques. However, the most important advance has been obtained with the appearance of transitional elastography (TE) or Fibroscan® (FS).
This procedure is also known as “one-dimensional pulse elastography” and is based on the measurement of the stiffness or elasticity of a tissue; it uses a mechanical pulse of vibration and an ultrasound wave. First, the mechanical pulse that produces an elastic wave that is transmitted through the tissue is emitted. Second, the ultrasonic wave, which follows the mechanical wave, measures the speed of propagation of the elastic wave inside the tissue. The speed of propagation of the elastic wave is proportional to the rigidity of the tissue (the harder the tissue the faster the wave propagates). The result is expressed in units of kilopascal (kPa)
About the Technique
The marketed method used by TE to measure the rigidity of the liver is called Fibroscan® (FS). The FS is formed by a transmitting and receiving probe and a computer that processes the information and generates an image of the elastic wave and the value of the hepatic rigidity in kPa. The probe contains a vibrating mechanism that produces the mechanical wave and a transducer that produces the ultrasound wave. The exploration begins with the fasting patient, in the supine position and with the right arm behind the head. The probe is applied on the hepatic silhouette, between the ribs, in the right mid-axillary line and perpendicular to the plane of the skin. The scanner must maintain the position of the probe (with the minimum possible movement) and press the button to obtain 10 valid determinations. The mechanical wave produces a vibration of medium amplitude and low frequency (50 Hz) that propagates up to 65 mm of the cutaneous surface and the volume of hepatic parenchyma evaluated is 100 times higher than that of the biopsy.
An image of the elastic wave in 2 dimensions is generated on the computer screen and its morphology can facilitate obtaining valid records. 10 valid determinations must be made (the computer will determine if the measurement is valid or should be repeated). In addition to the image, the screen will show 3 values that must be taken into account: the ratio or ratio between the number of valid measurements and the total number of measurements, the interquartile range or variation of the total valid measurements with respect to its median value and the final stiffness or median value of the 10 valid determinations (expressed in kPa).
Conclusion
The exploration with Fibroscan is fast (5 minutes), simple and its detection range is wide, between 2.5 and 75 kPa. Non-medical personnel (preferably a nurse) can perform the exploration after completing a short learning (50 to 100 scans), but the interpretation of the results should be done by a doctor with extensive knowledge about the characteristics and limitations of the technique.
Also Read:
- Liver Disease In Pregnancy: Definition, Causes, Types, Diagnosis, Symptoms, Signs, Treatment, Factors To Consider In Pregnancy
- Liver Damage or Liver Failure: Causes, Signs, Symptoms, Prevention
- Types of Liver Infection: Viral and Non-Viral Liver Infection
- 11 Signs & Symptoms of Liver Damage
- How Long Can You Live With Liver Cirrhosis?
- What Does Liver Pain Feel Like & What Can You Do About A Liver Pain?
- Why is Liver Function Test Done & What Does its Value (High, Low) Indicate?
- How Do You Know If Your Liver Is Failing?
