What is a Pressure Ulcer or Bed Sores?
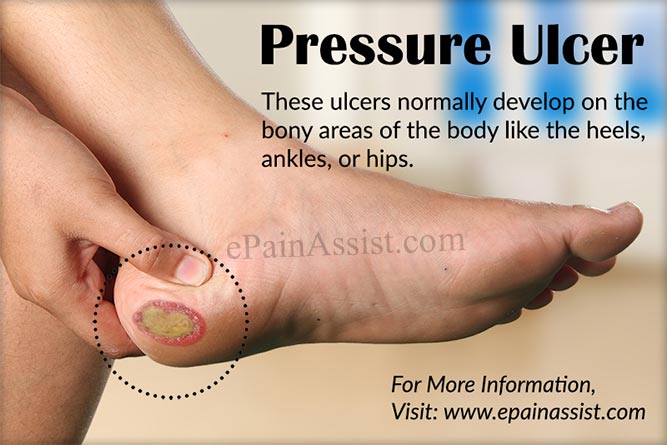
Pressure Ulcer which are also commonly known as Bed Sores is the name given to injuries sustained to the skin and the underlying tissues due to prolonged pressure on the skin. These ulcers normally develop on the bony areas of the body like the heels, ankles, or hips. People who are most at risk for Pressure Ulcers or Bed Sores are those people who do not have the ability to ambulate or change position due to medical conditions or old age and are most of the time confined to the bed. Pressure Ulcers or Bed Sores tend to develop quickly and often at times are very difficult to treat. There are quite a few measures available to treat Pressure Ulcers or Bed Sores or help heal them.
What Causes Pressure Ulcers or Bed Sores?
Pressure Ulcers or Bed Sores are caused due to excess pressure on the skin because of which there is restricted blood flow to the skin and the adjoining tissues. There are also other factors which play a role and predispose an individual to the development of Pressure Ulcers or Bed Sores like immobility for a long time or being confined on the bed for a very long time. Some of the contributing factors for development of Pressure Ulcers or Bed Sores are:
Unrelenting Pressure: In this, the skin and the underlying tissue are trapped between the bone and a solid surface like a bed or a wheelchair. The pressure due to this is much more than the flow of the blood in the capillaries resulting in the blood unable to deliver adequate nutrients to the tissues causing the cells in these regions to get damaged and ultimately die. These areas are such areas which do not have much muscle or fat around them like the spine, hips, elbows etc.
Friction: Friction is also a cause of Pressure Ulcers or Bed Sores. The friction can be caused due to movement or dragging across a surface like when changing positions while being stationary. Sustained friction may cause the skin to get even more fragile and predispose it to injuries.
What Are The Risk Factors for Pressure Ulcers or Bed Sores?
Pressure Ulcers or Bed Sores develop in people who are unable to move from one place to another and are mostly confined to bed or wheelchair. The following are some of the risk factors for Pressure Ulcers or Bed Sores:
- Overall poor health condition
- Paralysis
- Injury making an individual bedridden
- Recovery time postinjury
- Prolonged sedation
- Coma.
Some of the other factors that may predispose an individual to Pressure Ulcers or Bed Sores are:
Age: Due to old age the skin of an individual becomes more sensitive and fragile predisposing them to damage easily.
Lack of Sensation: Injuries to the spinal cord, certain neurological conditions can cause loss of sensory perception. This may cause the patient to not be aware of bedsores or the need to change position.
Weight Loss: Weight loss due to medical condition is also a contributing factor for development of Pressure Ulcers or Bed Sores.
Malnutrition: People who are not able to have enough nourishment are also at risk for development of Pressure Ulcers or Bed Sores.
What Are The Stages and Symptoms of Pressure Ulcers or Bed Sores?
Pressure Ulcers or Bed Sores fall into four stages and the symptoms are dependent on the stage and severity of the condition.
Stage I of Pressure Ulcer or Bed Sore: This is the initial or starting stage of development of Pressure Ulcers or Bed Sores. In this stage of bed sore, there is no skin breakdown. There may be skin discoloration. The area may be tender and painful to touch.
Stage II of Pressure Ulcer or Bed Sore: In people suffering from stage 2 of bed sore, the outer layer of the skin gets damaged. There will be formation of a wound which will be pink or red in color. The wound may resemble a blister.
Stage III of Pressure Ulcer or Bed Sore: In this stage of bed sore, the ulcer takes the form of a deep wound. There may also be some fat exposed due to loss of skin. Right at the bottom of the wound there may be some dead tissue seen.
Stage IV of Pressure Ulcer or Bed Sore: In stage IV of Bed Sore, there is tremendous amount of skin loss. The ulcer wound may be deep enough to expose the bone or muscles. The bottom of the wound will contain dead tissue.
How Are Pressure Ulcers or Bed Sores Diagnosed?
For evaluating a Pressure Ulcer or Bed Sore, the treating physician will look into the following:
- The size of the pressure ulcer or bed sore and its depth
- Look for any areas of bleeding, drainage of any fluids, or signs of any infection.
- Check for any foul odor indicating an infection of the dead tissue
- Look for any other areas where Pressure Ulcer may be developing.
The physician will then ask the following questions to confirm the diagnosis of Pressure Ulcer or Bed Sore.
- When did the Bed Sore appear first?
- Whether the Bed Sore is painful or not?
- Is there any prior history of Pressure Ulcers or Bed Sores?
- Does the patient change positions frequently while in bed or wheelchair?
Apart from this the physician will order the following tests:
- Blood test to look at the status of the health
- Tissue cultures to look for any signs of viral or bacteria infection
How Are Pressure Ulcers or Bed Sores Treated?
When it comes to treatment of Pressure Ulcers or Bed Sores, Stage I and II ulcers are mild and can be treated within a few weeks with appropriate wound care and other conservative measures. Stage III and IV ulcers are more difficult to treat.
Some of the ways to treat Pressure Ulcers or Bed Sores are:
Decreasing Pressure: Some of the ways to decrease pressure on the skin are:
Repositioning the Body in Bed or Wheel Chair to Treat and/or Prevent Pressure Ulcer or Bed Sore: Frequently changing positions is one of the ways to reduce pressure on the skin. If the patient is wheelchair bound it will be helpful to reposition the weight every 10 minutes or so. If the patient is unable to do this, then the caregiver needs to do it. For patients who are bedbound then changing positions every couple of hours is beneficial to take care of the Pressure Ulcers or Bed Sores or to prevent it.
Adequate Surfaces: it is beneficial to use surfaces which are soft and help in decreasing pressure on the skin. For wheelchair patients, a cushion can be used. For a bed bound patient, using water bed is recommended to treat and or prevent pressure ulcer or bed sores from forming.
Wound Care for Pressure Ulcer or Bed Sores: The next step towards treating Pressure Ulcers or Bed Sores is taking care of the wounds. This involves thorough cleaning of the wounds so as to avoid infection from developing. For stage I and II pressure ulcers or bed sores, just cleaning the area with soap and water is enough. Open sores can be cleaned with saline solution every time there is a change of dressing. Dressing is also an important aspect of wound healing as it promotes faster healing.
Removing Damaged Tissue: This is the next step for treatment of Pressure Ulcers or Bed Sores. This is essential so that the wound heal quickly and there is no risk of an infection due to dead or damaged tissue. This can be done surgically by removing the tissue altogether.
Some of the other ways of treating Pressure Ulcers or Bed Sores are:
Pain Medications for Pressure Ulcer or Bed Sores: Pain medications like Advil or Aleve can be used for painful sores. Topical pain medications are also helpful in reliving pain and can be applied during dressing changes.
Antibiotics: Infection related to Pressure Ulcers or Bed Sores which are not responding to other interventions can be treated with antibiotics.
Balanced Diet: A healthy and balanced diet is important to promote faster healing of Pressure Ulcer and Bed Sore.
Surgery: In some cases if no treatment is effective in treating Pressure Ulcers or Bed Sores then surgery is a way to treat Pressure Ulcers or Bed Sores. The aim of the surgery is to improve the appearance of the sore and treating infection. Surgery is done depending on the location of the wound and severity of the Pressure Ulcers or Bed Sores.
