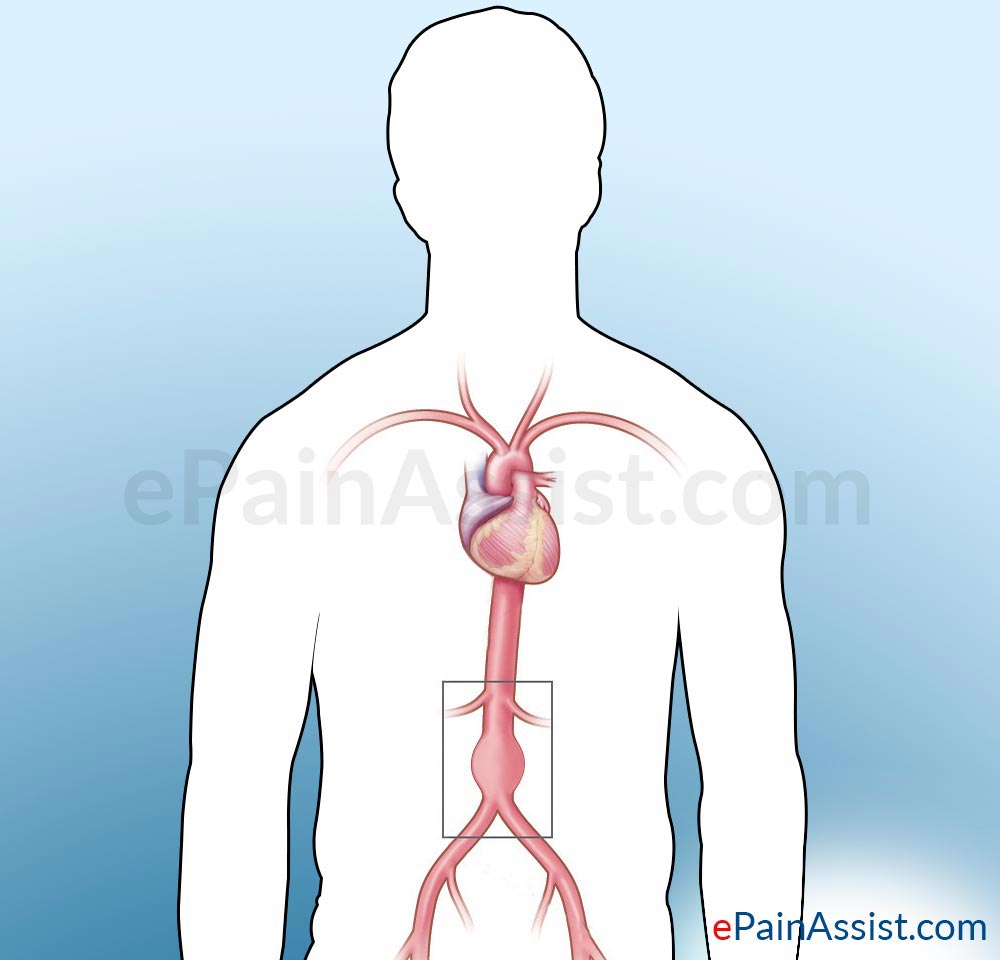
What is Abdominal Aortic Aneurysm?
An abdominal aortic aneurysm is a localized swelling and bulge in the lower part of the aorta due to weakening of the vessel wall. As the blood passes through the weakened portion of the vessel, it dilates or bulges and if this continues, it can rupture, which can be very fatal leading to internal bleeding, organ damage and even death. The aorta is a major blood vessel, which is responsible for supplying blood to the body. As the aorta is the main supplier of blood, a ruptured abdominal aortic aneurysm is a potentially life threatening condition and can cause some serious bleeding. Many of the slow-growing and small abdominal aortic aneurysms do not rupture; however, the fast-growing and large abdominal aortic aneurysms may rupture. Treatment depends on the size and the rate of growth of the aneurysm. Treatment varies from watchful waiting to emergency surgery. Once an abdominal aortic aneurysm is detected, the doctors closely supervise it, so that immediate surgery can be done when and if required. Surgery done on an emergency basis for a ruptured abdominal aneurysm can be quite risky.
Pathophysiology of Abdominal Aortic Aneurysm
The occurrence and expansion of an aneurysm depends on the local hemodynamic factors and factors intrinsic to the arterial segment itself.
The aorta has a relatively low-resistance circuit for circulating blood and the lower extremities have higher arterial resistance. Repeated trauma of a reflected arterial wave on the distal aorta may injure an already weakened aortic wall and lead to aneurysmal degeneration. Systemic hypertension further increases the injury, accelerates the expansion of existing aneurysms, and also contributes to their formation. Aneurysm formation is due to multiple factors affecting the arterial segment and its local environment. Many aneurysms are atherosclerotic in nature. As the aneurysmal dilatation increases, the arterial wall tension also increases and this can result in rupture of the aneurysm. Increase in blood pressure (systemic hypertension) leads to increase in aneurysm size which in turn increases the arterial wall tension and therefore increases the risk of rupture. The vessel wall is supplied by the blood within its lumen although the aorta has vasa vasorum, therefore as the aneurysm develops, the most ischemic portion of the aneurysm is at the distal end, which results in weakening of the vessel wall there and aids in further expansion of the aneurysm. Thus eventually, all aneurysms if left to their natural course rupture without intervention.
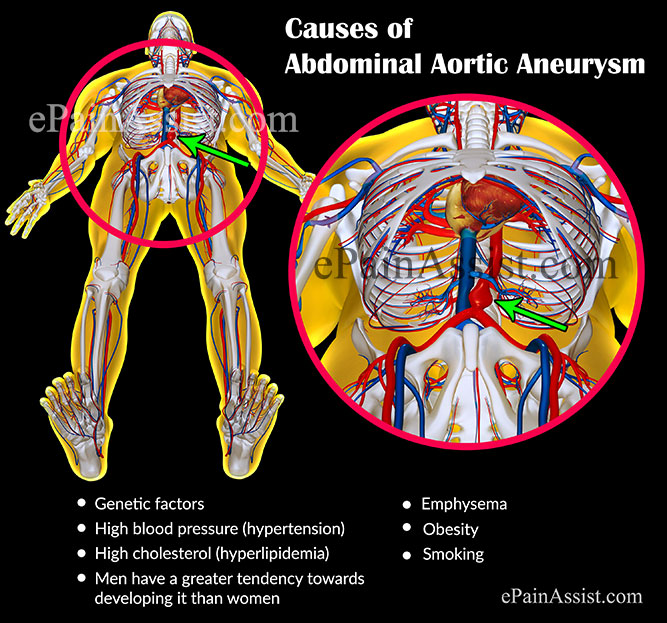
Causes and Risk Factors of Abdominal Aortic Aneurysm
The exact cause of abdominal aortic aneurysm is not known. The Risk Factors Include:
- Genetic factors.
- Emphysema.
- High blood pressure (hypertension).
- High cholesterol (hyperlipidemia).
- Men have a greater tendency towards developing it than women.
- Obesity.
- Smoking.
Although an abdominal aortic aneurysm can develop in anyone, it is more commonly seen in males over 60 years of age and who have one or more risk factors. The larger the aneurysm, the greater the risk of rupturing and bleeding.
Signs and Symptoms of Abdominal Aortic Aneurysm
An Abdominal Aortic Aneurysm (AAA) can be dangerous if it isn’t spotted early on. It can get bigger over time and could burst causing life-threatening bleeding. Screenings are recommended for people who have a family history and in men who are aged 65 and over and have smoked. This is why men are invited for screening to check for an Abdominal Aortic Aneurysm (AAA) when they’re 65.
An aneurysm may develop in any part of the aorta. Aneurysms involving both thoracic and abdominal sections may require complex treatment such as an elephant trunk procedure.
Abdominal Aortic Aneurysm (AAA) doesn’t usually have specific symptoms and is often referred to as a silent killer as they cause no symptoms or problems prior to bursting. It is mostly diagnosed during imaging studies done to diagnose other conditions. Your surgeon may perform an Abdominal Aortic Aneurysm Repair if you have one or more of these conditions:
- The diameter of your aorta exceeds 2 inches.
- You have intense abdominal pain and/or back pain.
- An abnormally prominent abdominal pulsation.
The purpose of the surgery is to prevent the aneurysm from rupturing or bursting.
The Symptoms of Rupture Include:
- Abrupt, severe and constant pain in the abdomen or back.
- The pain may radiate to groin, buttocks or legs.
- Moist skin.
- Dizziness.
- Nausea.
- Vomiting.
- Rapid heart rate.
- Shock.
Tests to Diagnoses Abdominal Aortic Aneurysm
To diagnose your abdominal aortic aneurysm, your doctor will review your medical and family history and perform physical examination. If your doctor suspects that you have abdominal aortic aneurysm, he will order specialized tests mentioned below-
- Abdominal Ultrasounds are most commonly used to diagnose abdominal aortic aneurysm.
- CAT scan with IV contrast is used typically to identify the shape and diameter of the aneurysm.
- MRI is performed to diagnose the size and location of the aneurysm.
The U.S. Preventive Services Task Force recommends that men ages 65 to 75 who have ever smoked should have a one-time screening for abdominal aortic aneurysms using abdominal ultrasound. Men ages 60 and older with a family history of abdominal aortic aneurysms should consider regular screening for the condition.
Diagnosis of Abdominal Aortic Aneurysm Includes:
- Evaluating the pulses in legs.
- A lump (mass) can be felt in the abdomen.
- A pulsating sensation is felt in the abdomen.
- The abdomen feels stiff or rigid.
Abdominal Aortic Aneurysm Which Presents Without Symptoms or Problems Can Be Diagnosed With The Following Tests:
- Chest x-ray.
- Angiogram.
- Computerized tomography (CT) scan of the abdomen.
- Abdominal ultrasound.
- Magnetic resonance imaging (MRI).
Treatment of Abdominal Aortic Aneurysm
Depending on the size of the aneurysm, your doctor will suggest you the treatment.
- For small abdominal aortic aneurysms (ranging about 3cm to 4.4 cm across) annual ultrasounds are recommended to check if it’s growing bigger. You will be asked to follow a healthier lifestyle.
- For medium sized abdominal aortic aneurysms (about 4.5cm to 5.5cm), ultrasounds are recommended every 3 months to check if it’s growing. You will be asked to follow a healthy lifestyle.
- For abdominal aortic aneurysms that are larger than 5.5cm or more, you will be recommended a surgery to stop it getting bigger.
Surgery for Abdominal Aortic Aneurysm
Before The Procedure:
- IV line will be placed
- General anesthesia will be administered
- Breathing tube will be inserted
- Catheter placed in the bladder
The AAA Repair Surgeries Can Be Performed In One of The Below Mentioned Ways:
Open Repair. The traditional operation involves cutting open your abdomen to replace the aneurysm with an artificial piece of artery (a graft). For this surgery, your doctor makes a large incision in the abdomen to expose the aorta. Once the abdomen has been opened, a graft can be used to repair the aneurysm. Open repair remains the standard procedure for an abdominal aortic aneurysm repair. This procedure takes about 4 to 6 hours.
Endovascular Aneurysm Repair (EVAR). This Procedure is Preferred in People Who:
- Have a heart disease
- Are at a higher surgical risk due to age or other factors.
This is a minimally invasive procedure requiring only a small incision in the groin. The surgeon will insert special instruments through a catheter in an artery in the groin and thread them up to the aneurysm. At the aneurysm, your doctor will place the stent and graft to support the aneurysm. This surgery usually takes 2 to 3 hours.
Recovery and Aftercare Following Abdominal Aortic Aneurysm Repair
After the procedure breathing tube will be removed. You will be monitored in the recovery area. IV line will be established. A stomach tube will be inserted. An open surgery requires about 5 to 10 days of hospital stay whereas an endovascular procedure requires 2 to 3 days hospital stay. You will be fully recovered by the end of about 6 to 12 weeks for any kind of activities. The nurses and doctors will try and keep you free of pain by giving painkillers by injection, via the epidural tube in your back, or by a machine that you are able to control yourself by pressing a button. Injection for (deep vein thrombosis) and PE (pulmonary embolus) prophylaxis will be given to you until you are discharged and fully mobile. You can start your exercise, driving, bathing, work etc after a certain amount of time after your surgeon clears you for these.
Complications of Abdominal Aortic Aneurysm Repair Surgery
All surgeries carry risks related to anesthesia, bleeding, infection, and stress on the heart resulting in irregular heart rhythm and heart attack. Additional common problem related to open surgery are development of a hernia or bulge; this occurs in about 10 to 20% of the patients. Sometimes there is alteration in sexual function in men. Less common complications are loss of circulation to the legs or large intestine in immediate postoperative period.
Survival Rate Following Abdominal Aortic Aneurysm Repair Surgery
Survival after repair of ruptured AAA depends on a number of patient factors, such as age and comorbid conditions and the patient’s management within the healthcare system, including accuracy of diagnosis, time from symptoms to surgery, and skill of the surgical team. The age of the patient cannot be changed, and comorbid conditions can be optimized but not eliminated. Studies show that perioperative mortality rate is less in EVAR procedure as compared to open procedure. A study found improvement in short term survival rates of patients who underwent surgery to repair a ruptured AAA. The relative survival rate held at about 87 percent. Patients undergoing elective repair of intact aneurysm face low risk and can expect normal longevity after surgery. The fact that operative treatment is offered to older patients, with more frequent cardiovascular disease, could have resulted in inferior long-term outcomes. Accurately selected elderly patients can have excellent long term survival after surgery.
- “Abdominal Aortic Aneurysm” by Dr. M. Hinchliffe et al., The BMJ. Available at: https://www.bmj.com/content/360/bmj.k851
- “Abdominal Aortic Aneurysm” by Dr. M. Shahin et al., StatPearls. Available at: https://www.ncbi.nlm.nih.gov/books/NBK430789/
- “Abdominal Aortic Aneurysms” by Dr. G. Lawrence et al., American Family Physician. Available at: https://www.aafp.org/afp/2007/1215/p1809.html
- “Abdominal Aortic Aneurysms” by Dr. J. Wanhainen et al., Circulation Research. Available at: https://www.ahajournals.org/doi/10.1161/CIRCRESAHA.117.306590
- “Abdominal Aortic Aneurysm: Pathophysiology, Epidemiology, Prognosis, and Treatment” by Dr. A. Ogawa et al., International Heart Journal. Available at: https://www.jstage.jst.go.jp/article/ihj/57/3/57_17-175/_article
Also Read:
- What is Aneurysm: Causes, Types, Symptoms, Treatment, Survival Rate
- Abdominal Aortic Aneurysm: Pathophysiology, Causes, Risk Factors, Signs, Symptoms, Tests, Treatment
- Thoracic Aortic Aneurysm or Thoracic Aneurysm and Aortic Dissection (TAAD): Causes, Signs, Symptoms, Treatment, Home Remedies