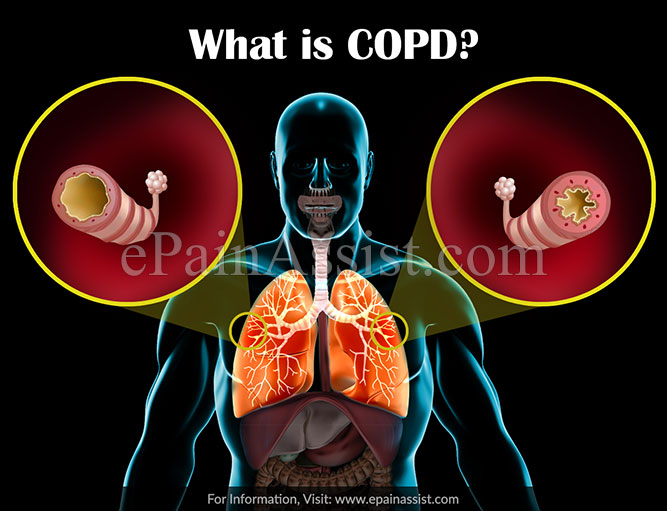
What is COPD?
COPD or Chronic Obstructive Pulmonary Disease is a broad term used to describe chronic conditions and diseases of the lungs. In COPD, patient has progressive and slow obstruction of airflow into the lungs or out of the lungs. COPD or Chronic obstructive pulmonary disease has many causes of which the primary cause is exposure to tobacco smoke and cigarette smoking. Other causes of COPD are air pollution, genetic conditions and infectious diseases.
The prevalence of COPD has increased twice since 1982. COPD is slightly more common in men than women. The symptoms of COPD or Chronic obstructive pulmonary disease which include coughing, shortness of breath etc become obvious slowly which leads to late diagnosis of COPD often after the age of 40 to 50. There are some people though who get diagnosed at a younger age. The symptoms of COPD experienced by the patients consist of chronic bronchitis, asthma and emphysema.
What are the Causes of COPD?
- Exposure to tobacco smoke and cigarette smoking is the primary cause of COPD. Tobacco smoke is responsible for 90% of the risk for development of COPD. Secondhand smoke is also equally responsible for increasing the risk for chronic obstructive pulmonary disease.
- Chronic exposure to air pollution which occurs from burning coal or wood or with industrial air pollutants can also cause COPD or chronic obstructive pulmonary disease.
- Infectious diseases which damage the lung tissue in patients with asthma or hyperactive airways can also lead to COPD.
What are the Risk Factors for COPD?
- Cigarette/tobacco smoking is the biggest risk factor for developing COPD.
- Other risk factors consist of exposure to high levels of air pollution, exposure to secondhand smoke from tobacco and exposure to air pollution associated with coal or wood.
- Patients with chronic bronchitis who have airway hyper-responsiveness are also at increased risk for developing COPD.
- Alpha-1 antitrypsin is a genetic factor and the deficiency of which slightly increases the risk of for emphysema and COPD.
- Intravenous drug use increases the risk of COPD.
- Vesiculitis syndrome increases the risk of COPD.
- Immune deficiency syndromes increase the risk of COPD.
- Connective tissue disorders increases the risk of COPD.
- Genetic problems such as Salla disease increase the risk of COPD.
What are the Signs & Symptoms of COPD?
COPD or Chronic obstructive pulmonary disease is a disease which is slowly progressive; so it is not uncommon to find the initial signs and symptoms a little bit different from the symptoms experienced in the late stages of this disease. Symptoms are the common base upon which the stages of COPD are classified.
Productive cough is the main initial symptom of COPD. The sputum can be colorless or with a white mucus
Shortness of breath or breathlessness (dyspnea) is the most significant symptom of chronic obstructive pulmonary disease. In the initial stages of COPD, dyspnea can occur occasionally with exertion which gradually progresses to breathlessness upon doing simple tasks, such as walking to the bathroom or standing up. In some patients, wheezing can also develop which is a hissing or a whistling sound while breathing.
Other general signs and symptoms of COPD or chronic obstructive pulmonary disease are:
- Cough, (as mentioned above) often with colorless sputum in small amounts.
- Shortness of breath (commonly seen in patients aged 60 and above.
- Acute chest discomfort.
- Wheezing (particularly during exertion).
Serious Symptoms of COPD
As the COPD worsens from mild to moderate, the severity of the symptoms also increases and consists of:
- Rapid breathing (tachypnea).
- Respiratory distress upon doing simple tasks such as climbing up a few stairs.
- Cyanosis, which is bluish discoloration of the skin.
- Wheezing with minimal exertion.
- Peripheral edema, which is the swelling of extremities.
- Use of accessory respiratory muscles.
- Hyperinflation of the lungs.
- Coarse crackles are heard in the lungs with inspiration.
- The expiration (exhalation) is prolonged.
- Diffuse breath sounds are present.
- There is an elevated jugular venous pulse.
What are the Stages of Chronic Obstructive Pulmonary Disease?
There are four stages of COPD. One way to stage COPD or chronic obstructive pulmonary disease is the Global Initiative for Chronic Obstructive Lung Disease program (GOLD) where the staging is based on the results of a pulmonary function test. The staging of chronic obstructive pulmonary disease based on pulmonary function test and more specifically forced expiratory volume in one second are:
- Stage I: In this stage of COPD, the FEV1 is equal or more than 80% of the predicted value.
- Stage II: In this stage of COPD, the FEV1 is about 50% to 79% of the predicted value.
- Stage III: In this stage of COPD, the FEV1 is 30% to 49% of the predicted value.
- Stage IV: In this stage of COPD, the FEV1 is lesser than 30% of predicted value or the FEV1 is lesser than 50% of predicted value along with respiratory failure.
Are There Any Other Medical Conditions/Diseases Which Contribute to COPD?
There are three non-genetic medical problems of lung tissue which contribute to COPD and these are:
- Chronic bronchitis.
- Emphysema.
- Infectious diseases of the lung.
What Types of Doctors Treat COPD?
- COPD or Chronic obstructive pulmonary disease is a chronic or long-term disease which is slowly progressive. Other than a primary care physician, patient also needs to consult a pulmonologist who is a doctor specializing in treatment of lung disease. A pulmonologist will manage and treat COPD symptoms with medications and other treatment methods.
- Other than this, pulmonary rehabilitation specialists also need to be consulted. They will teach the patient breathing exercises and muscle strengthening exercises.
- Nutritional counseling also helps in reducing COPD symptoms.
- Anxiety and depression are other common problems seen in patients with COPD or chronic obstructive pulmonary disease. So it is also beneficial for the patient to consult a psychologist or a psychiatrist to provide treatment for symptoms of anxiety and depression along with counseling for the patient and patient’s family members.
- A surgeon needs to be consulted if the patient needs a lung reduction surgery or a lung transplant surgery or some other lung surgery for severe emphysema.
- An intensivist or a critical care physician is needed in emergency situations of COPD.
How is the Diagnosis of COPD Made?
The initial diagnosis of COPD is made based on the patient’s symptoms, patient’s breathing history, patient’s history of exposure to air pollutants, patient’s history of tobacco smoking or exposure to secondhand smoke and patient’s history of lung disease.
Imaging tests done to diagnose COPD are: Chest X-ray, CT scan of the lungs, Arterial Blood Gas or a pulse oximetry to measure the saturation level of oxygen in blood. Other than this, patient is also referred to a pulmonologist (lung specialist) for assessing their FEV1 level.
What is the Treatment for COPD or Chronic Obstructive Pulmonary Disease?
There are various treatments for chronic obstructive pulmonary disease and the most effective treatment and the best treatment which should be implemented immediately is to stop smoking.
Medical treatments for chronic obstructive pulmonary disease consist of beta-2 agonists and bronchodilators (anti-cholinergic agents), mucolytic agents, steroids and oxygen therapy.
Surgical treatment for chronic obstructive pulmonary disease consists of lung volume reduction surgery, bullectomy and lung transplantation.
Is the Treatment Different for Different Stages of COPD?
Treatment for chronic obstructive pulmonary disease depends on the stage of COPD:
Treatment for Stage I of COPD: Patient needs short-acting bronchodilators.
Treatment for Stage II of COPD: Patient needs short-acting bronchodilator as needed along with long-acting bronchodilators and cardiopulmonary rehabilitation.
Treatment for Stage III of COPD: Patient needs short-acting bronchodilator as required, long-acting bronchodilators with cardiopulmonary rehabilitation along with inhaled glucocorticoids in case of repeated COPD exacerbations.
Treatment for Stage IV of COPD: Stage IV has been termed “end-stage” chronic obstructive pulmonary disease. Patient needs long-acting bronchodilators, inhaled glucocorticoids, cardiopulmonary rehabilitation, long-term oxygen therapy, possible lung volume reduction surgery and even possible lung transplantation.
What are the Medications Used in Treatment of COPD?
Nicotine Replacement Therapy
This is the first line of treatment for smoking cessation. Nicotine replacement therapy helps the patients to quit smoking and using this treatment also decreases the withdrawal symptoms. Nicotine Replacement Therapy comprises of nicotine-containing chewing gum and nicotine patches to be applied on the skin through which the nicotine gets absorbed via the skin. Doing this therapy helps in the nicotine getting gradually withdrawn from the body and helps the patient in successfully quitting smoking.
Oral Medications to Quit Smoking:
- Oral medications, such as varenicline, are also prescribed to help in cessation of smoking. This alternative can also be tried to quit smoking.
- Antidepressants, such as bupropion, help in decreasing the symptoms of nicotine withdrawal.
- There are some medications which are used “off label” to help in quitting smoking. These medications include nortriptyline which is an older type of antidepressant and helps smokers to quit smoking more easily. Clonidine is another off label medicine which can help smokers quit smoking.
Oral Medications/Inhalers for Treating the Symptoms of COPD
- Bronchodilators help in opening the airway tubes and allowing the air to pass more freely in and out of the lungs. For this reason, both short-term (several hours) and long-term (12 or more hours) bronchodilators are prescribed for COPD.
- Some short-term bronchodilators are: albuterol, metaproterenol, pirbuterol and levalbuterol.
- Some long-term bronchodilators are: salmeterol, formoterol, indacaterol and arformoterol.
- Anti-cholinergic bronchodilators are: ipratropium, aclidinium and tiotropium.
- There are other bronchodilators such as theophylline which are used occasionally, but are not recommended as it has unwanted side effects, such as tremors, anxiety, arrhythmias and seizures.
- A combination of drugs using long-acting bronchodilators and steroids are also used for treatment of COPD.
What are the Surgical Treatments for COPD or Chronic Obstructive Pulmonary Disease?
Surgery is not always desirable or possible for many patients suffering from COPD. There are 3 types of surgery done for chronic obstructive pulmonary disease:
Bullectomy: This surgery involves the removal of giant bullae which are the air-filled spaces commonly occurring on the periphery of the lung. These giant bullae occupy lung space usually in patients with emphysema. Giant bullae can occupy more than 32% of the lung tissue which leads to compression of adjacent lung tissue and also restricts ventilation and blood circulation to healthy tissues. By doing bullectomy, the compressed lung tissue which is still functional can expand.
Lung Volume Reduction Surgery: This surgery consists of removing the lung tissue which has been most damaged by tobacco smoking. This usually comprises of 20% to 30% of the lung tissue present in the upper part of each lung. Lung volume reduction surgery is not a frequently done procedure and is done on patients having severe emphysema and marked hyperinflation of the air spaces and airways.
Lung Transplant Surgery: This surgery is done in patients suffering from advanced lung disease. Patients suffering from chronic obstructive pulmonary disease are the largest single category of individuals who undergo lung transplantation. More often, these patients with chronic obstructive pulmonary disease are at COPD stage 3 or 4 with severe symptoms and with lung transplantation they may have an average life expectancy of around two years or less.
What is the Aim of Treatment of COPD?
The aim of treatment and management of chronic obstructive pulmonary disease is:
- Decreasing the airflow limitation.
- Preventing and treating secondary medical complications which can include infection and hypoxemia.
- Reducing the respiratory symptoms and improving the patient’s quality of life.
Does a Patient with COPD Need to be Hospitalized?
The patient needs to be hospitalized if he/she develops acute exacerbation of chronic obstructive pulmonary disease, severe respiratory dysfunction, or if they have other serious respiratory diseases such as acute bronchitis or pneumonia. The main purpose of hospitalization is treating the symptoms of COPD and preventing further deterioration of the condition.
The patient may need to be admitted to ICU (intensive care unit) for invasive or noninvasive mechanical ventilation or hospitalization is needed in case of development of these symptoms: lethargy, confusion, respiratory muscle fatigue, respiratory acidosis and worsening hypoxemia.
What are the Lifestyle Changes Recommended for Patients with COPD?
Smoking Cessation. As mentioned before the, the most effective and preventative therapy for COPD is quitting smoking and avoiding any exposure to tobacco smoke.
Exercises. Exercises for chronic obstructive pulmonary disease should be done. Patients having mild to moderate symptoms of COPD commonly benefit from exercises which help in increasing stamina and creasing the advancement of chronic obstructive pulmonary disease. Yoga is also beneficial in COPD as it helps with breathing muscle control and breathing efficiency.
Complementary/Home Treatment for COPD
There are various over-the-counter (OTC) foods and supplements which are thought to help in reducing symptoms of COPD; however, patients with COPD should discuss with their doctor before starting any of these supplements or home remedies as such type of treatments can interfere with their ongoing therapy. Dietary and supplementary treatment for COPD includes:
- Intake of Omega-3 fatty acids helps in decreasing inflammation. Omega-3 fatty acids can be taken in the form of supplements and is also found in foods such as herring, salmon, sardines, mackerel, canola oil and soybeans.
- Vitamin E helps in improving the function of the lungs.
- Antioxidants intake should be increased as it helps in fighting inflammation. Antioxidants are found in abundance in foods such as tomatoes, kale, green tea, broccoli and red grapes.
- Acupuncture is also said to benefit in reduction of symptoms of COPD.
- Relaxation therapy, breathing techniques and meditation also help in COPD.
Supplemental Therapies to Treat the Complications & Symptoms of COPD
Supplementary therapies for COPD include antibiotics to reduce pathogen damage to lung tissue, mucolytic agents and oxygenation therapies; all these help in reducing the symptoms of COPD. Many patients benefit from oxygen therapy where it increases their life expectancy and improves their quality of life. Oxygen therapy also helps with exercise endurance.
Can Chronic Obstructive Pulmonary Disease be Prevented?
Preventive measures for COPD include:
- Chronic obstructive pulmonary disease can be easily prevented by abstaining from tobacco products. However, COPD developing as a result of genetic problems cannot be prevented.
- Avoiding exposure to lung irritants like air pollutants.
- Avoiding coal, oil, and wood -burning fumes.
- Getting the recommended vaccines to avoid infections, such as flu, helps in reducing the lung damage and the symptoms of COPD which accompany lung damage.
What is the Prognosis & Life Expectancy of Chronic Obstructive Pulmonary Disease?
- Patients with mild chronic obstructive pulmonary disease have a good prognosis and they can have a relatively normal life expectancy. However the prognosis of chronic obstructive pulmonary disease decreases if the severity of COPD staging increases.
- The average life expectancy of a patient with chronic obstructive pulmonary disease who undergoes a lung transplant is around 5 years.
- Patients suffering from COPD and who are admitted to ICU have an estimated mortality rate of about 25%. This is more than twice for patients who are above the age of 65.
- Patients suffering from COPD and who continue to smoke will face a rapid decline in FEV1. These patients who develop right-sided heart failure and severe hypoxemia with decreased ability to perform daily functions will have a poor prognosis.
Brief Summary Points About Chronic Obstructive Pulmonary Disease
- Chronic Obstructive Pulmonary Disease (COPD) is a medical term used to describe chronic diseases and conditions of the lungs.
- Chronic bronchitis, emphysema, asthma, and infectious diseases can contribute to the development of chronic obstructive pulmonary disease.
- Symptoms of chronic obstructive pulmonary disease consist of cough, shortness of breath, chest discomfort, wheezing. Serious symptoms of COPD consist of: respiratory distress, cyanosis, tachypnea, peripheral edema, use of accessory respiratory muscles, chronic wheezing, hyperinflation, abnormal lung sounds, elevated jugular venous pulse, prolonged expiration and cyanosis.
- There are 4 stages of chronic obstructive pulmonary disease. Increase in the stage number means that the COPD is becoming progressively worse. COPD stage IV is also referred to as “end stage” chronic obstructive pulmonary disease.
- Doctors who treat COPD comprise of primary care physician, pulmonologist and lung surgeons. Other professionals include pulmonary rehabilitation specialists and mental health specialists.
- The diagnosis of COPD is made by taking the patient’s history of exposure to irritants and patient’s breathing history. Depending on the patient’s FEV1 level, a pulmonologist will determine the stage of COPD.
- Except for genetic form of COPD, this disease can be easily prevented by avoiding cigarette smoke / toxic fumes.
- Medical treatment for COPD includes medications to help quit smoking, anticholinergics, bronchodilators, enzyme inhibitors and steroids.
- Other supplemental therapies for COPD include antibiotics, oxygen therapy, mucolytic agents, yoga and endurance exercises.
- Patients should consult their doctor before undertaking other complementary treatment or home remedies.
- Surgery for COPD includes bullectomy, lung volume reduction surgery or lung transplant surgery.
- The prognosis and life expectancy for patients with COPD depends on the stage of the disease. The prognosis worsens as the COPD stage increases.
Also Read:
