Lung atelectasis is also an impediment that could occur due to other issues affecting the respiratory system such as cystic fibrosis, foreign objects breathed into the lungs, tumors in the lung, immune weakness in the respiratory system and injuries to the chest.
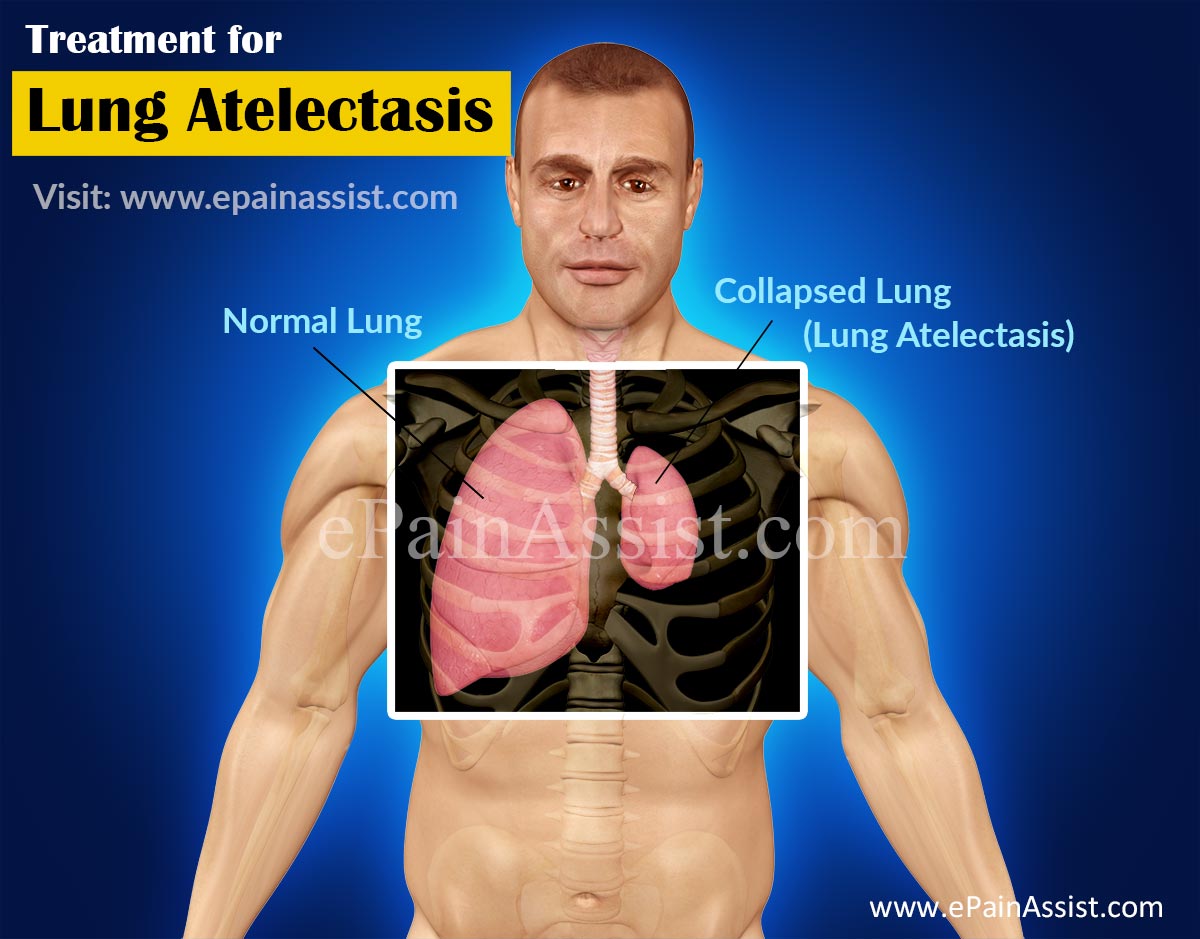
It does not always involve the same amount of lung tissue and the amount varies depending on the source of lung atelectasis. The condition can result in breathing difficulties and reduced oxygen in the lungs especially where lung disease already exists. Treatment is administered based on the origin of the condition and the degree of collapse.
In this article you will learn about the treatment for lung atelectasis, home remedies, prognosis/outlook, lifestyle changes, yoga for lung atelectasis, recovery period and healing time for lung atelectasis.
Treatment for Lung Atelectasis
Treatment for lung atelectasis is dependent on its cause. Where lung atelectasis affects only a small portion of the lung, treatment may not be necessary and the infection could heal on its own. Where the cause is a tumor, treatment may involve its removal or shrinkage through chemotherapy, surgery or radiotherapy. It is important to note that lung atelectasis is not a disease by itself but rather a sign of disease.
Nursing measures to manage the condition of lung atelectasis include frequent turning and early mobilization and strategies to expand the lungs and manage secretions. Voluntary breathing maneuvers at least every 2 hours help in preventing and treating the condition. Secretion management method includes directed cough, and aerosol nebulizer treatments which is then followed by chest physical therapy (PT) and bronchoscopy. Use of voluntary deep breathing enhances lung expansion.
-
Chest Physiotherapy Treatment for Lung Atelectasis
Chest physiotherapy for lung atelectasis is designed to improve respiratory efficiency by promoting expansion of the lungs, strengthening respiratory muscles and eliminating lung secretions. It is designed to help patients breathe more freely after surgery. These techniques of chest physiotherapy for lung atelectasis include:
- Relaxed positioning, turning in bed, such that the head is positioned lower than the chest to make it easier for mucus to drain out.
- Deep breathing exercises, chest percussion and vibration.
- Chest physiotherapy for effective coughing in lung atelectasis.
- Chest physiotherapy for loosening mucus from the affected area by clapping on the chest for lung atelectasis as well as the use of devices to manually clear the mucus.
- Patients can use supplemental oxygen to make breathing easier to remove shortness of breath.
-
Physical Therapy (PT) for Treating Lung Atelectasis
Physical therapy (PT) for lung atelectasis involves use of different methods to remove mucous from the lung. The patient is positioned in a way that gravity assists in removing the secretions from the body. The patient lies on the side of the collapsed lung to encourage drainage.
-
Respiratory Therapy for Treating Lung Atelectasis
Respiratory therapy for lung atelectasis may include one or all of the following:
- Use of breathing treatments or masks to open up the airways is the primary respiratory therapy for lung atelectasis.
- Removal of secretions by suctioning is another respiratory therapy for lung atelectasis.
- Use of a ventilator to assist in breathing where the patient cannot breathe properly without assistance.
- Use of a breathing device to help the patient achieve maximal ventilation.
-
Medications for Treating Lung Atelectasis
The medications given to treat lung atelectasis may include:
Medicines for lung atelectasis that clear up the airways.
- Medicines for lung atelectasis that are given to cure the disease that caused the collapse.
- Antibiotic drugs for lung atelectasis to clear up the infection.
- Drugs such as inhalers to keep asthma under control.
- Oxygen supply to help with breathing.
- Drugs that control heart disease.
-
Bronchoscopy for Treating Lung Atelectasis
Bronchoscopy technique can be used for lung atelectasis to eliminate the foreign bodies and mucus that blocks the air passage.
-
Surgical or Other Procedures to Treat Lung Atelectasis
Specialists might suggest opting for suctioning mucus or bronchoscopy for cleaning of the obstructed airways. In bronchoscopy for treating lung atelectasis, an elastic tube is sent down the throat of the patient to clear the air passage. If the patient is too weak to cough or has low levels of oxygen then the air pressure is increased to clear the air ways.
Home Remedies for Lung Atelectasis
Lung atelectasis cannot be treated at home. Rehydrating by taking at least 2 liters of water and other fluids daily may help with removing the lung secretions by thinning them. There are some ways through which the risk of lung atelectasis can be reduced. They are:
- Breathing deeply after surgery to clear the airways is a remedy for lung atelectasis.
- Frequently changing the position of a bedridden person can be a good remedy for victims of lung atelectasis.
- Avoiding smoking as it increases mucous production at the same time damaging the cilia which are found in the bronchial tubes lining making it hard to remove mucous from the airways.
- Keeping nuts away from children under 3 years or those who do not have molars for chewing.
Coping with Lung Atelectasis
Lung atelectasis, especially the severe form is not an easy condition to live with. In order to make it through, it is important to keenly follow the advice given by the doctor and obtain as much information about lung atelectasis as possible. The doctor may recommend different things, for example, the use of an incentive spirometry hourly to help the lungs expand or visit a respiratory therapist in order to free the lungs from phlegm. One should stay constantly hydrated and avoid too much use of painkillers to avoid interference with breathing in order to properly cope with lung atelectasis
Outlook/Prognosis for Lung Atelectasis
How the condition of lung atelectasis progresses is a factor of its cause. In adults, it usually does not last long as the air sacs easily refill with air once the cause has been treated. If it lasts for long, the lungs may be unable to clear mucous and thus result in infections such as pneumonia.
In most instances, lung atelectasis is non-life threatening. It can, however, affect a large portion of the lungs in a baby or someone with an existing lung disease and in such an instance, death can occur if treatment is not administered quickly on time.
Lifestyle Changes for Lung Atelectasis
The following are the lifestyle changes recommended for the sufferers of lung atelectasis:
- Maintenance of good hygiene through washing of hands with ordinary soap before eating and on returning home is important lifestyle to adapt for patients of lung atelectasis. Antibacterial soaps do not give a lot of protection especially where viruses are concerned.
- Another important lifestyle change is to maintain a healthy weight through healthy eating.
- Quitting smoking is a major recommended lifestyle change for lung atelectasis. Smoking highly contributes to lung disease and breaking this habit could go a long way in preventing lung atelectasis.
Yoga for Lung Atelectasis
Certain yoga poses or asanas and kriyas are designed to strengthen the lungs and thus should be used only after full recovery and not during treatment. The following are some of the yoga kriyas and asanas for lung atelectasis:
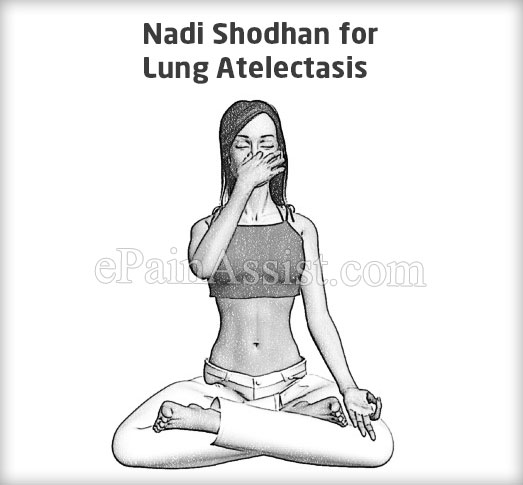
- Nadi Shodhan is a balancing kriya for lung atelectasis in which alternate nostril breathing is practiced by opening and closing the nostrils with fingers and thumb of the right hand. It helps a lot with healing many respiratory and circulatory issues.
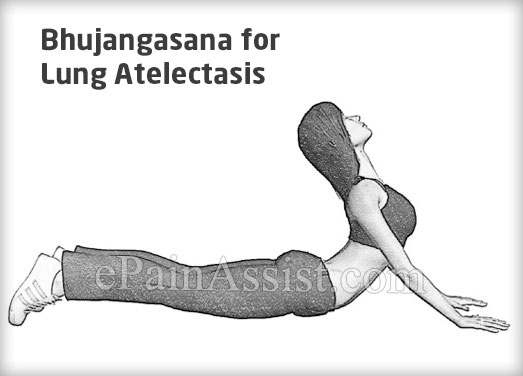
- Bhujangasana which is also known as cobra pose for lung atelectasis is a posture that provides a strong backward bend, so lift your chest, pull down and away with your shoulders, and arch your upper back as much as you can to get the greatest stretch possible. It improves blood circulation and can help people with lung problems.
- Ardhamatsyendrasana which is also known as sitting half spinal twist yoga pose for lung atelectasis helps the chest open up and helps the lungs receive more oxygen thus reducing the chance of being restricted by lung problems.

- Pavanamuktasana alsoknown as wind relieving yoga pose for lung atelectasis is a move that helps massage the abdomen and relieve gas and thus is good for asthmatic people.

- Setubandhasana alsoknown as Bridge yoga pose for lung atelectasis is a very effective move for asthmatic patients. It helps improve digestion by opening up the chest and lungs. It also lowers thyroid issues.

- Adho mukha svanasana also known as Downward-facing dog yoga pose for lung atelectasis is a move that is recommended for asthmatic people as well as people with sinusitis. It calms the mind and takes away stress.

- Badhakonasana whose alternative name is Butterfly yoga pose for lung atelectasis helps improve blood circulation, takes away fatigue and relieves lung atelectasis patients.

- Poorvottanasana alsoknown as upward plank pose for lung atelectasis adds strength to the arms, wrists, back and spine, it also stimulates the thyroid gland and makes improvements to the respiratory system.

- Shavasana also known as Corpse pose is a meditative move and helps remove anxiety and pressure resulting in a relaxed body and mind. This makes it easy to manage asthma.

It is important to gain yoga skills from a professional and then practice at home daily. There is need to consult a doctor first before taking up the yoga classes to determine if one is ready.
Recovery Period/Healing Time for Lung Atelectasis
Recovery period or healing time for lung atelectasis varies based on the underlying cause as well as the extent of the lung atelectasis. Once the underlying cause has been dealt with, the recovery time does not take long.
Prevention of Lung Atelectasis
Prevention of lung atelectasis is better than curing it. For children, it is important to keep them away from small objects as blockage is the biggest cause of lung atelectasis for this group.
In adults, lung atelectasis usually follows a surgery thus it is important to learn ways of reducing the risks if scheduled for surgery by consulting a doctor.
Also Read:
