Vitreous degeneration is a condition affecting the eye and is also known as posterior vitreous detachment (PVD). It occurs due to the detachment of the vitreous membrane on the eyeball surface from the retina. This results in various complaints like seeing floaters or spots that affect normal vision. Let us understand about vitreous degeneration, its types, causes, symptoms, treatment and surgery in detail.
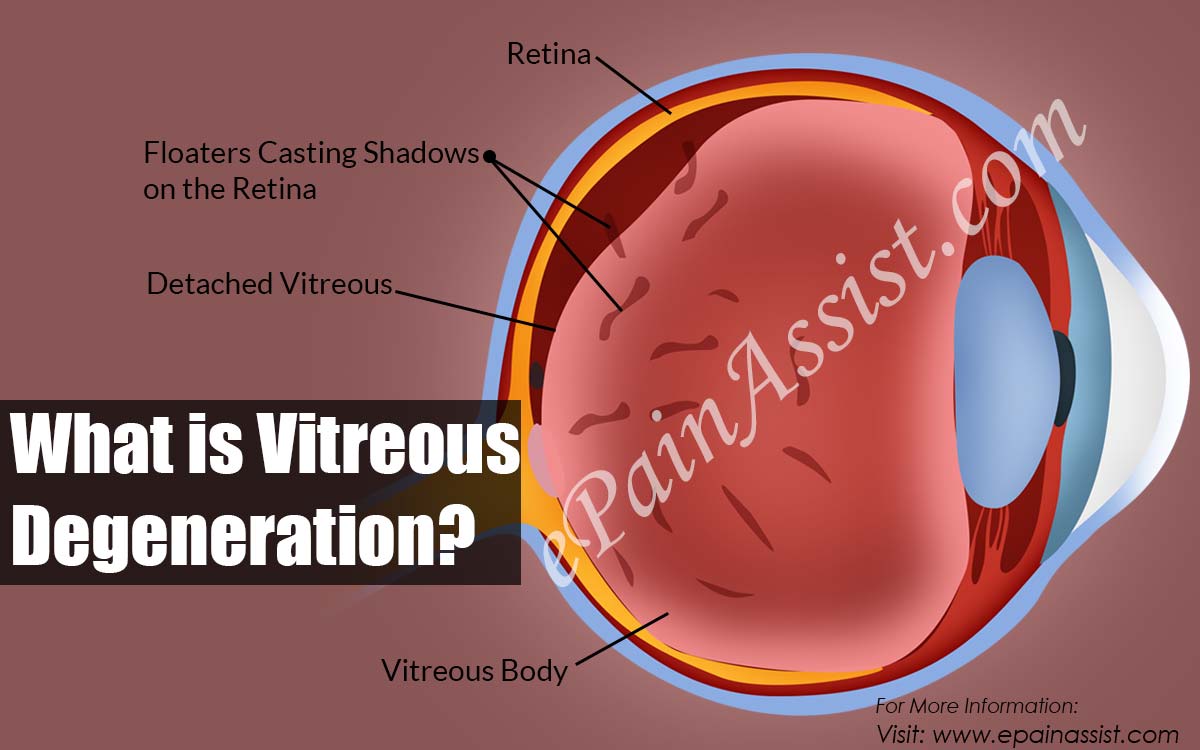
What is Vitreous Degeneration?
The interior chamber of the eye, behind the lens, is filled with a gel like substance known as vitreous that is needed to maintain the round shape of the eye. It also nurtures the eye during the developmental phase. Within vitreous many fibers are entangled and it also remains attached to retina of the eye. Ageing or other disease conditions may cause this vitreous to liquefy and shrink resulting in fibers pull and stress on retina. Subsequently, floaters start to appear, as the commonest symptom of vitreous degeneration.
Healthy vitreous is transparent while degenerative stage causes opacities and clumps in this, resulting in formation of floaters. These floaters may be dark black or grey spots or lines roving with the movement of eye in the field of vision. Patients often complain it as strands of hair, flies, cobwebs, letter C etc. in their vision since floaters formed direct their shadows on retina. In the advanced stage, vitreous separates from retina leaving a mark as round shadow on retina, which is complained as flashes of light by the patients. That is why floaters are generally complained along with flashes of light. Sometimes floaters are not due to degeneration, may be presence of blood or inflammatory debris inside the vitreous look like floaters.
Further, as the stage progresses vitreous totally separates from retina, resulting condition known as posterior vitreous detachment (PVD).
Types of Vitreous Degeneration
According to the presentation of disease some of the common types of vitreous degeneration include,
- Benign Vitreous Floaters or Vitreous Detachment: This type of vitreous degeneration is the starting phase, mainly associated with aging. As age advances, the vitreous become stringy and shrinks. Normally it fills the eye but advancement of age causes its nature to change and when gel shrinks, the condition is known as vitreous detachment. As it often occurs on posterior wall therefore known as posterior vitreous detachment (PVD). It appears as spots, strands, cobwebs or dark shadows etc. The appearance is due to particles and fibers moving in vitreous that emit its shadow on the retinal wall. It has no permanent effect and may persist for weeks to months. It also does not adversely affect the vision though.
- Symptomatic Vitreous Floaters or Vitreous Opacities: In this type of vitreous degeneration, vitreous floaters present with symptoms. There are multiple dark colored floaters present in vitreous gel. It represents the progressive stage of vitreous degeneration with more severe form. As the stage progresses, due to pull on the retina if retina tears which occurs in about 10 % of cases, flashes of lights are also present along with floaters. Further progress of this condition may threaten retinal detachment. Sometimes it is due to other conditions like vitreous hemorrhage or some kind of inflammation. If it is due to other causes, it can happen at any age, even in younger people and is often allied with vision problems.
- Degenerative Vitreous Syndrome/DVS – This type of vitreous degeneration is mostly seen in elders of 50 years or above. It is the persistent form of this disorder that severely affects the vision. Patients often complain about their insufficiency to do their routine work like reading, driving and other skills required to see. Due to lack of clarity in vision and constant struggle for normal vision, the quality of life and emotional status of the patient also gets affected. Few patients complain that they often felt something from behind or side is coming towards them since peripheral vision is also impaired. Blinking of eyes, rubbing or moving head from side to side may relieve the complaints temporarily but again the same inadequate and impaired vision problems arise.
Causes of Vitreous Degeneration
Some of the commonest causes of vitreous degeneration include:
Aging – Advancing again and the related changes is the main cause of vitreous degeneration. Mostly affected patients are 50 years or above, while few cases of 40 years and above had also been reported.
Some risk factors of conditions that fasten the progress of vitreous degeneration include –
- Eye trauma or any inflammation in eyes may quicken the formation of floaters.
- Myopia or near sightedness. Patients of myopia may experience these degenerative changes at an early age.
- Cataract surgery or previously done any laser treatment or surgery of eye may also increase the risk of formation of floaters in some people.
Symptoms of Vitreous Degeneration
- Floaters being the commonest complaint, here are some other symptoms of vitreous degeneration.
- Floaters appear in eye causing spots, strings cobwebs shadows in vision. As time passes either they disappear themselves or settle down at the bottom of the eye.
- Initially, it may be annoying as shadows in vision appear, but after sometime brain learns to ignore it. Blinking of eyes or head movement relieves the condition.
- Increase in the numbers of floaters along with flashes of light and peripheral vision is disturbed in progressive stage of the disease.
- If not treated properly loss of vision may occur.
Vitreous Degeneration and Vision
As discussed earlier, benign form of floaters have no threatening impact on vision. They appear and disappear on their own. When there is sudden increase in the form of multiple floaters in vitreous gel, casting there shadows on retina, patients complain of shadows of spots, strings or cobwebs in their vision. Further advancement in the disease fibers pull hard on the retinal wall, creating a macular hole and retinal detachment. This form threatens the sight and is often described as flashes of light along with shadows of floaters. This needs treatment and if left untreated may lead to permanent vision loss.
Diagnosis of Vitreous Degeneration
Diagnosis of vitreous degeneration depends on the stages of this disease. A comprehensive dilated full eye examination is required in the advanced stages of the disorder.
Treatment of Vitreous Degeneration
Benign form having few floaters need no treatment as possess no threat to the vision. As time passes and the floaters settle down at the bottom of eye by itself. Floaters may last for weeks to months to years. Few cases have been reported where they did not disappear completely. Even then floaters are not accompanied by any vision problem. Therefore no active treatment is required to remove it. Though persistent floaters may annoying effect patient are advised to learn to avoid it since no measure is there to prevent the formation of these floaters.
Progressed state of vitreous degeneration when sudden increase in floaters are observed along with flashes of light in peripheral vision, need full eye examination. Patients are advised not to avoid this situation and immediately undergo full eye examination by an expert. Since leaving macular hole or retinal detachment condition untreated, may lead to severe vision problems or permanent loss of vision. Nearsighted patients need much care since chances of retinal detachment are more common among myopic patients. Treatment of vitreous degeneration in such cases is aimed at reducing floaters and other symptoms and improving the vision problems.
Tear of retina, if detected early, may be treated with the Laser therapy but if condition progresses to retinal detachment surgery is required. There is no simple therapy to remove floaters other than surgery. Surgery is preferred in severe and serious forms like detachment as they too have the risk of complications and side effects.
The Treatment Of Vitreous Degeneration Based On Various Stages Includes:
Floater: Need no treatment
Sudden Increase In Floater: Full eye examination is required. Treatment then depends on severity.
Floaters with Flashes of Light: Comprehensive dilated eye examination should be done by expert. If it suggests early retinal tear, Laser therapy may be beneficial
Retinal Detachment: Surgery – Vitrectomy is advised.
Vitrectomy – Surgery for Vitreous Degeneration
Vitrectomy is the surgery for vitreous degeneration, done to remove the vitreous gel. It is performed by an ophthalmologist who has been trained to intra ocular surgeries.
If there is retinal detachment or blood due to vitreous hemorrhage in vitreous gel that does not clear on its own, vitrectomy is performed. Local or general anesthesia is preferred according to the condition of patient. Vitreous gel is removed from middle of eye using special tools and then repair to the retinal scar, tear or detachment is done. Further, gas bubble or oil bubble is injected inside the eye to press the retinal wall to its original position.
Though surgery is the hope for the patients suffering with retinal tear or detachment, there is a risk of some side effects or complications after operation. These include
- Cataract
- Retinal detachment
- High pressure pain inside eye. Mostly in patients of Glaucoma.
- Hemorrhage
- Inflammation and infection in eyes
To combat these risks some newer technologies has been introduced, for example,
- 360 degree indirect ophthalmoscope laser photocoagulation to the peripheral retina had been introduced that secures retina from the risk of retinal detachment. This is performed few weeks prior to vitrectomy. The suitability and the need for this procedure is decided by the surgeon, based on the condition of the patient.
- Prophylactic retinal detachment laser cerclage to the peripheral retina is another option to minimize the risks.
Post-Surgery Recovery Period for Vitreous Degeneration
Surgery for vitreous degeneration is very much successful and relieves patient thoroughly. Recovery is quick but requires a healing period of few weeks, with proper rest while scars heal and vision improves. After one to two weeks the patient may return to normal activities. Increase in altitude, climbing, adventure sports and travelling should be avoided. Excessive concentration work, watching television, computer work and driving may strain eyes and should be avoided during the initial one or two weeks.
Since after surgery eye may be swollen and sore, pain may be present. Pain controlling medicines prescribed by the doctor should be used. It is necessary to protect the eyes and keep it sanitized and moist during the recovery period. Eye drops and eye packs are advised by experts. Proper follow-ups and regular checkups as advised by ophthalmologist must be attended on time and any abnormal signs or symptoms must be reported immediately.
- American Academy of Ophthalmology. (2021). Posterior Vitreous Detachment. https://www.aao.org/eye-health/diseases/posterior-vitreous-detachment
- American Society of Retina Specialists. (2021). Posterior Vitreous Detachment (PVD). https://www.asrs.org/patients/retinal-diseases/19/posterior-vitreous-detachment-pvd
- Mayo Clinic. (2021). Posterior Vitreous Detachment. https://www.mayoclinic.org/diseases-conditions/retinal-detachment/symptoms-causes/syc-20351344
Also Read:
