What is Optic Neuritis or Retrobulbar Neuritis?
Optic neuropathy is a term generally used to describe any condition that results in damage to the optic nerve. Optic neuritis is alternatively known as retrobulbar neuritis.
Optic neuritis or retrobulbar neuritisis a term used for specific type of optic neuropathy resulting from inflammation or demyelination of the optic nerve, which may suddenly cause reduced vision in the affected eye.
Optic neuritis or retrobulbar neuritiscan occur both in adults or children and may involve either one or both optic nerves.
Epidemiology of Optic Neuritis or Retrobulbar Neuritis
Optic Neuritis or Retrobulbar Neuritis affects typically young adults ranging from 18 to 45 years of age, with an average age of 30 to 35 years. Strong female predominance is seen. The annual incidence is approximately 5/100,000, with a total prevalence estimated to be 115/100,000.
Pathophysiology of Optic Neuritis or Retrobulbar Neuritis
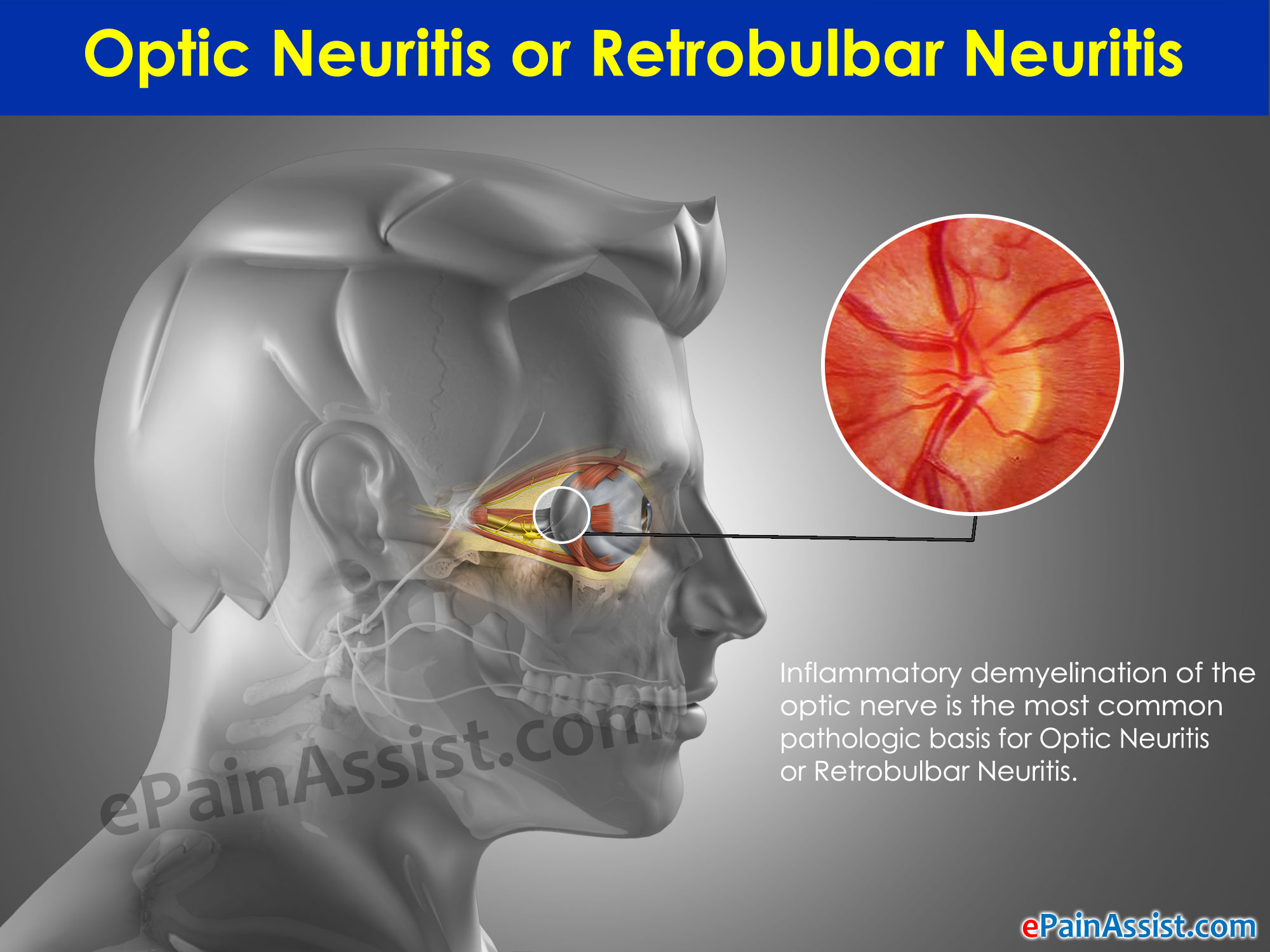
Inflammatory demyelination of the optic nerve is the most common pathologic basis for Optic Neuritis or Retrobulbar Neuritis. The pathology of Optic Neuritis or Retrobulbar Neuritis is similar to acute multiple sclerosis plaques in the brain with perivascular cuffing, myelin breakdown and edema in the myelinated nerve sheaths. Demyelination is preceded by inflammation of the retinal vascular endothelium and sometimes visibly manifest as retinal vein sheathing. Myelin loss exceeds axonal loss.
Causes and Risk Factors of Optic Neuritis or Retrobulbar Neuritis
The basic cause of Optic Neuritis or Retrobulbar Neuritis is often unknown, however, there are many causes of Optic Neuritis or Retrobulbar Neuritis some of which are as follows:
- Cranial arteritis: This means inflammation of the lining of the arteries within the skull. Inflamed cranial arteries can block blood flow to the brain and eyes, which in turn may cause stroke or permanent vision loss. This most likely is seen to occur in adults between 60 to 90 years of age. Cranial arteritis is also known as giant cell arteritis or temporal arteritis.
- Infections: Bacterial infections such as tuberculosis, Lyme disease, cat scratch disease, syphilis and toxoplasmosis, or viral infections such as HIV, hepatitis B, and herpes zoster can cause Optic Neuritis or Retrobulbar Neuritis. Encephalitis, bacterial meningitis and sinusitis, especially in children, may also cause optic nerve damage or Optic Neuritis or Retrobulbar Neuritis.
- Diabetes: Diabetes poses an increased risk of developing optic nerve disorders, including Optic Neuritis or Retrobulbar Neuritis, most likely from decreased blood flow to the optic nerve.
- Drugs: Some drugs have been found to be associated with the development of Optic Neuritis or Retrobulbar Neuritis, Ethambutol or Myambutol and certain antibiotics to name a few.
- Toxins: Toxins like lead, quinine, alcohol, tobacco and arsenic may cause vision loss and other symptoms that may mimic Optic Neuritis or Retrobulbar Neuritis.
- Leber’s Hereditary Optic Neuropathy: This is an inherited form of vision loss from Optic Neuritis or Retrobulbar Neuritis that mostly affects the males in their 20s or 30s.
- Pernicious anemia, Grave’s disease, sarcoidosis, bee stings and vaccinations may lead to optic nerve swelling and cause vision loss.
- Autoimmune diseases such as systemic lupus erythematosus may cause vasculitis or inflammation of blood vessels that nourish the optic nerve leading to loss of vision.
- Though an uncommon cause, radiation therapy to the head may cause Optic Neuritis or Retrobulbar Neuritis.
- Some other causes of Optic Neuritis or Retrobulbar Neuritis include glaucoma, direct trauma to the optic nerve, elevated intracranial pressure, primary and metastatic optic nerve tumors, nutritional deficiencies, intraocular inflammation, and injuries.
Signs and Symptoms of Optic Neuritis or Retrobulbar Neuritis
- The most characteristic findings of Optic Neuritis or Retrobulbar Neuritis include decreased visual acuity, significant change in peripheral vision, decreased perception of brightness, and change in color vision. Disturbance in function of the pupil also known as afferent pupillary defect or APD can be detected if one eye is affected and the other eye is either unaffected or involved to a lesser degree.
- The major symptom of Optic Neuritis or Retrobulbar Neuritis is vision loss, frequently maximal within one or two days and varying from a small area of blurring to complete blindness. Loss of vision develops typically between a day to two weeks and may be worsened by exercise or heat. Vision loss may be permanent in some cases but is usually temporary.
- Most of the people who develop Optic Neuritis or Retrobulbar Neuritis tend to experience eye pain that is worsened by eye movement. Pain usually touches its peak within a week and then goes away within several days.
- Optic Neuritis or Retrobulbar Neuritis may occur in both eyes simultaneously, but it usually affects only one eye. Patients may be unaware of subtle visual loss or changes in the color vision in cases where only one eye is affected until the doctor asks them to close the healthy eye.
Treatment for Optic Neuritis or Retrobulbar Neuritis
It may become easy to treat with appropriate therapy if a definite cause is determined.
- In cases where cause is undetermined or is related to multiple sclerosis, vision often returns to normal within two to 12 weeks without any treatment, but chances are that it may also advance to a state of permanent partial or complete loss of vision.
- Treatment with steroid medications may speed up vision recovery. Although treatment with steroids have little effect on the visual outcome in patients with Optic Neuritis or Retrobulbar Neuritis, patients treated initially with intravenous steroids have about one-half the risk of developing multiple sclerosis in two years compared to untreated patients. In addition, such patients have fewer repeated attacks of Optic Neuritis or Retrobulbar Neuritis than that of untreated patients.
- Ophthalmologists treat patients with Optic Neuritis or Retrobulbar Neuritis with either intravenous followed by oral steroids or no treatment at all. The regimen typically includes three days of intravenous steroids, followed by about 11 days of oral steroids.
- When Optic Neuritis or Retrobulbar Neuritis is associated with multiple sclerosis, immunomodulator or immunosuppressive therapy may be prescribed to reduce the incidence of attacks in future.
Tests to Diagnose Optic Neuritis or Retrobulbar Neuriti
A person with a first episode of Optic Neuritis or Retrobulbar Neuritis is recommended MRI of the brain to look for central nervous system lesions. MRI with gadolinium enhancement may show an enhancing, enlarged optic nerve. MRI may also help in diagnosing multiple sclerosis by demonstrating typical abnormalities in the brain.
- Magnetic Resonance Imaging. (MRI)
- Visual acuity testing.
- Pupillary testing.
- Visual field testing.
- Color vision testing, and visualization of the optic disc by direct and indirect ophthalmoscopy.
- Optic Neuritis: https://www.ncbi.nlm.nih.gov/books/NBK532948/
- Optic Neuritis: https://www.aao.org/eye-health/diseases/optic-neuritis
- Optic Neuritis: A Review: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2749412/
Also Read: