What is the Integumentary System?
The integumentary system is a critical system of the body, made up of your skin, hair, nails, glands, and some nerves as well. It is the body’s outer-most layer and acts as your first line of defense. The integumentary system protects you not only against harmful microorganisms, but also from injury and sunlight. The organs and structures of the integumentary system act as the main physical barrier to protect your body from infection, microbes, injury, and sunlight. It also helps regulate the body temperature and lets you feel sensations like hot and cold.
There are many critical roles and functions that the integumentary system carries out in the body, including:(1, 2, 3, 4)
- To protect the body’s internal organs and tissues.
- To protect against invasion by infectious microorganisms and injuries.
- Keeps the body safe from dehydration by helping it retain fluid.
- Protects the body against any abrupt changes in temperature by regulating the body temperature.
- Helps eliminate waste materials.
- Stores fat, water, and vitamin D.
- Synthesizes vitamin D.
- Acts as a receptor for sensations like hot, cold, pain, pressure, and touch.
While the integumentary is a crucial part of the body, it is also susceptible to many diseases, disorders, and even injuries. These can range from being annoying but benign fungal or bacterial infections to severe burns and even skin cancer that can be fatal.
One of the most serious diseases of the integumentary system is skin cancer. Let’s take a look at the connection between the integumentary system and cancer.
The Integumentary System and Cancer
Cancer is an umbrella term used to describe diseases that are caused by abnormal cells in the body that are dividing in an uncontrolled fashion. Most cancers are identified and described by the tissue or organ where it originates. One such common form of cancer is skin cancer. According to estimates by the Skin Cancer Foundation, one in five Americans is likely to experience some form of skin cancer during their lifetime.(5, 6)
The damage and degradation of the ozone layer in the atmosphere along with the increase in exposure to ultraviolet (UV) radiation from the sun has contributed to a sharp increase in the prevalence of skin cancer all over the world. Overexposure to the UV rays from the sun is known to cause damage to the DNA of the skin cells, thus leading to the formation of cancerous lesions throughout the body. Even though a pigment known as melanin present in the topmost layer of the skin offers some protection against DNA damage caused by UV rays, it is often not enough. It has also been observed that cancers often occur on parts of the body that are commonly not exposed to any UV radiation. This suggests that there are many other factors that can cause cancerous lesions to develop.(7)
It is important to remember that all parts of the body work together as parts of a complex machine. The integumentary system plays an important role in assisting other bodily systems in maintaining and carrying out their functions. Since the skin is the largest organ of the body and an integral part of the integumentary system, when you are affected by skin cancer, it impacts all the other parts of the body.
On a general basis, cancers are caused due to a build-up of DNA mutations in the body. These DNA mutations can result in giving rise to certain cell populations that do not die when they should. They then begin a process of uncontrolled multiplication that leads to the formation of tumors.(8, 9) While many tumors remain harmless or benign, some start producing cells that are able to mobilize and produce more tumors in other parts of the body through a process known as metastasis. Cancers are generally characterized by their capability to metastasize.(10, 11, 12)
Types of Skin Cancer
Skin cancer develops when the skin cells start to grow and multiply rapidly in an uncontrolled and unorderly manner. In normal conditions, new skin cells form when the cells grow old and die, or when they get damaged. When this process fails to work as it should, rapid and uncontrolled growth of cells, some of which end up being abnormal cells, takes place. This rapid build-up of cells may be benign or non-cancerous and not a cause of concern, or they may be cancerous. If they are cancerous, they may spread to other parts of the body or nearby tissue if not caught in time and treated. One of the main causes of skin cancer is exposure to UV light from the sun.
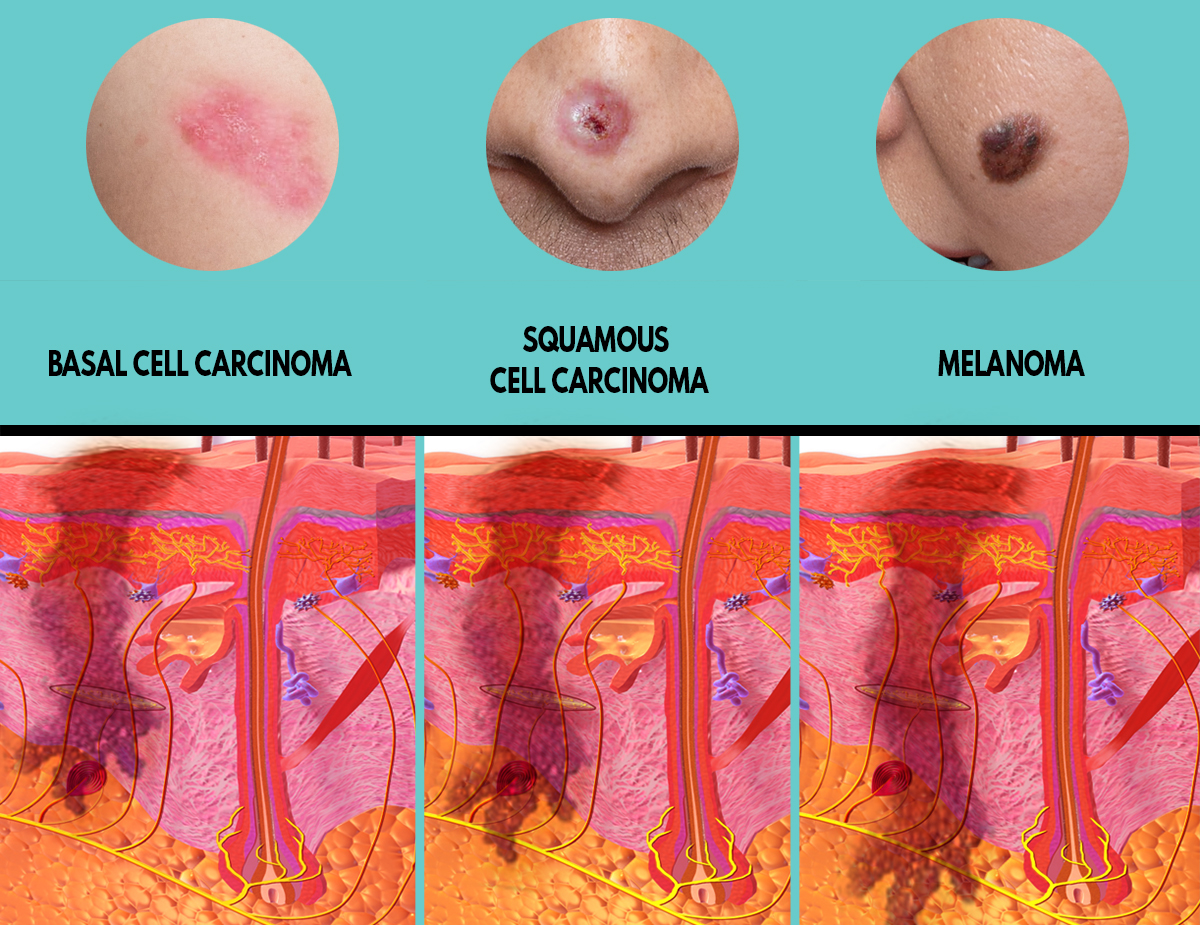
There are three main types of skin cancer that affect the integumentary system. These are:
- Basal cell carcinoma
- Squamous cell carcinoma
- Melanoma
Let’s take a closer look at these three types of skin cancer.
Basal Cell Carcinoma
Basal cell carcinoma is a type of cancer that affects the mitotically active stem cells located in the stratum basale of the epidermis. The stratum basale also called as the stratum germinativum is the deepest layer of the epidermis layer of the skin. It is separated from the second layer of skin (dermis) by a membrane known as the basal lamina.(13, 14, 15) Basal cell carcinomas are sometimes also known as non-melanoma skin cancer.
Basal cell carcinoma is the most common type of all cancers that are diagnosed in the United States and it is mostly found on the head, arms, back, and neck, all parts of the body that are the most vulnerable to long-term sun exposure.(16)
Even though UV rays are the most common cause of basal cell carcinoma, there are many other factors that can cause this type of cancer. For example, exposure to arsenic and radiation can also lead to basal cell carcinoma.
This type of skin cancer typically begins in the stratum basale and tends to spread along this boundary itself. At a certain point, they start to grow and spread towards the surface and eventually become an uneven bump, patch, growth, or may even appear like a scar on the surface of the skin. Basal cell carcinoma commonly appears to be a small, sometimes scaly flat patch or a shiny bump on the skin that tends to grow slowly over time.
While basal cell carcinoma can affect anyone, it is seen to be more common in men and those assigned males at birth. It is also more common in people who are older than 50 years, and people with light eyes and fair skin. It is also interesting to note that people who have had basal cell carcinoma once are at a higher risk for getting another type of non-melanoma skin cancer.
Similar to most other cancers, basal cell carcinomas respond to treatment if they are caught early. Treatment for basal cell carcinoma includes topical ointments, surgery, and freezing or cryosurgery. The most common treatment is surgery to remove all the cancer cells along with some of the healthy tissue around the cells.(17)
Squamous Cell Carcinoma
Squamous cell carcinoma is a type of skin cancer that affects the keratinocytes present in the stratum spinosum. Keratinocytes are the most dominant type of skin cells that make up the epidermis layer. They play an important role in skin repair. Squamous cell carcinoma presents as lesions found on the hands, ears, and the scalp, and it is the second most common form of skin cancer.(18, 19) An interesting fact about squamous cell carcinomas is that this type of cancer also develops in parts of the body where there are mucous membranes present. These are the inner lining of your body cavities and organs. They can be commonly found in your lungs, anus, and mouth.
According to the American Cancer Society, two out of every ten skin cancers are diagnosed as squamous cell carcinomas.(20) While squamous cell carcinoma can affect anyone, you are at a higher risk if you have regular or long-term exposure to the sun or you have suffered from sun damage to your skin at an early age. It is also more common in those who have green or blue eyes, blonde or red hair, or a pale complexion. It tends to affect people who are 65 years or older. While people over the age of 50 are more likely to develop squamous cell carcinoma, but in recent times, the incidence of this type of skin cancer has been increasing in people younger than 50 years as well.
This form of skin cancer is more aggressive than basal cell carcinoma and if not removed on time, these cancerous cells can metastasize. Radiation and surgery are the common forms of treatment for squamous cell carcinoma.(21)
Melanoma
Melanoma is a type of skin cancer that is characterized by the uncontrolled growth of skin cells known as melanocytes. Melanocytes are responsible for producing the pigment melanin in the epidermis layer of your skin. Usually, melanoma starts to develop from a mole. It is known to be the most fatal of all skin cancer since it is not only highly metastatic but also very difficult to detect in the early stages. By the time melanoma is detected, it has already spread to other organs, making it difficult to treat.
Melanomas usually show up as being asymmetrical brown or black patches on the skin with raised surfaces and uneven borders.
Treatment for melanomas involves surgical excision and immunotherapy. If left untreated or caught at an advanced stage, melanomas are likely to spread to other organs beyond the skin. This makes them challenging to treat and often life-threatening.(22, 23)
Diagnosis and Treatment of Skin Cancer
Your dermatologist will first begin the diagnosis process by asking you about any changes in any existing freckles, moles, or new skin spots or growths. They will also examine all your skin, including the scalp, palms of your hands, soles of your feet, ears, between your toes, between your buttocks, and around the genitals as well. If a suspicious-looking skin lesion is found during the physical examination, your doctor will recommend a biopsy. In a biopsy, a small sample of tissue is removed from the affected area and sent for examination by a pathologist. This helps doctors determine if the skin lesion is cancerous or benign, what type of cancer it is, and also discuss your treatment options with you.
Treatment of skin cancer depends on the type and stage of cancer you have. Stages of skin cancer range from stage 0 to stage IV, with the higher numbers denoting a more advanced stage of cancer.
In some cases, even a biopsy is sufficient to remove all the cancerous tissue if the cancer is limited to the skin’s surface and is small. Other skin cancer treatments include:(24, 25)
- Excisional surgery
- Cryotherapy
- Mohs surgery
- Chemotherapy and immunotherapy
- Radiation therapy
- Photodynamic therapy
- Curettage and electrodessication
Conclusion
Skin cancer is the most common type of cancer that affects the integumentary system. Skin cancer also accounts for nearly half of all new cancers in the world. It is most common in people with light-colored skin and those who have a high exposure to the sun’s UV rays. Basal cell carcinoma and squamous cell carcinoma are the two most common types of skin cancer, with the third type of skin cancer being melanoma. If the integumentary system is affected by cancer, it affects many of the crucial functions of the system. If you notice any type of new skin growth or skin lesion or a mole or freckle that suddenly starts to grow or has uneven borders, you should consult a dermatologist at the earliest. Remember that early diagnosis and treatment of skin cancer can increase the chances of successful treatment.
- Mauldin, E.A. and Peters-Kennedy, J., 2016. Integumentary system. Jubb, Kennedy & Palmer’s Pathology of Domestic Animals: Volume 1, p.509.
- Elliott, D.G., 2000. Integumentary system. In The laboratory fish (pp. 271-306). Academic Press.
- Rawles, M.E. and Marshall, A.J., 1960. The integumentary system. Biology and comparative physiology of birds, 1, pp.189-240.
- Lund, C.H. and Kuller, J.M., 2013. Integumentary system. Comprehensive neonatal nursing care, 5, pp.299-333.
- Federman, D.G., Kravetz, J.D. and Kirsner, R.S., 2002. Skin cancer screening by dermatologists: prevalence and barriers. Journal of the American Academy of Dermatology, 46(5), pp.710-714.
- Coups, E.J., Geller, A.C., Weinstock, M.A., Heckman, C.J. and Manne, S.L., 2010. Prevalence and correlates of skin cancer screening among middle-aged and older white adults in the United States. The American journal of medicine, 123(5), pp.439-445.
- Zink, A., 2017. Non-melanoma skin cancer: Pathogenesis, prevalence and prevention. Der Hautarzt; Zeitschrift fur Dermatologie, Venerologie, und verwandte Gebiete, 68(11), pp.919-928.
- MacDonald, I.C., Groom, A.C. and Chambers, A.F., 2002. Cancer spread and micrometastasis development: quantitative approaches for in vivo models. Bioessays, 24(10), pp.885-893.
- MOHS, F.E. and LATHROP, T.G., 1952. Modes of spread of cancer of skin. AMA Archives of Dermatology and Syphilology, 66(4), pp.427-439.
- Chaffer, C.L. and Weinberg, R.A., 2011. A perspective on cancer cell metastasis. science, 331(6024), pp.1559-1564.
- Brooks, S.A., Lomax-Browne, H.J., Carter, T.M., Kinch, C.E. and Hall, D.M., 2010. Molecular interactions in cancer cell metastasis. Acta histochemica, 112(1), pp.3-25.
- Baccelli, I. and Trumpp, A., 2012. The evolving concept of cancer and metastasis stem cells. Journal of Cell Biology, 198(3), pp.281-293.
- Said, J.W., Sassoon, A.F., Shintaku, I.P. and Banks-Schlegel, S., 1984. Involucrin in squamous and basal cell carcinomas of the skin: an immunohistochemical study. Journal of investigative dermatology, 82(5), pp.449-452.
- Bretschko, E., Szeimies, R.M., Landthaler, M. and Lee, G., 1996. Topical 5-aminolevulinic acid for photodynamic therapy of basal cell carcinoma. Evaluation of stratum corneum permeability in vitro. Journal of controlled release, 42(3), pp.203-208.
- Yousef, H., Alhajj, M. and Sharma, S., 2017. Anatomy, skin (integument), epidermis.
- Goldenberg, G., Karagiannis, T., Palmer, J.B., Lotya, J., O’Neill, C., Kisa, R., Herrera, V. and Siegel, D.M., 2016. Incidence and prevalence of basal cell carcinoma (BCC) and locally advanced BCC (LABCC) in a large commercially insured population in the United States: A retrospective cohort study. Journal of the American Academy of Dermatology, 75(5), pp.957-966.
- Berking, C., Hauschild, A., Kölbl, O., Mast, G. and Gutzmer, R., 2014. Basal cell carcinoma—treatments for the commonest skin cancer. Deutsches Ärzteblatt International, 111(22), p.389.
- Marks, R., 1996. Squamous cell carcinoma. The Lancet, 347(9003), pp.735-738.
- Webb, J.L., Burns, R.E., Brown, H.M., LeRoy, B.E. and Kosarek, C.E., 2009. Squamous cell carcinoma. Compendium (Yardley, PA), 31(3), pp.E9-E9.
- Smith, H.O., Tiffany, M.F., Qualls, C.R. and Key, C.R., 2000. The rising incidence of adenocarcinoma relative to squamous cell carcinoma of the uterine cervix in the United States—a 24-year population-based study. Gynecologic oncology, 78(2), pp.97-105.
- Combalia, A. and Carrera, C., 2020. Squamous cell carcinoma: an update on diagnosis and treatment. Dermatology Practical & Conceptual, 10(3).
- Coit, D.G., Andtbacka, R., Bichakjian, C.K., Dilawari, R.A., DiMaio, D., Guild, V., Halpern, A.C., Hodi, F.S., Kashani-Sabet, M., Lange, J.R. and Lind, A., 2009. Melanoma. Journal of the National Comprehensive Cancer Network, 7(3), pp.250-275.
- Houghton, A.N. and Polsky, D., 2002. Focus on melanoma. Cancer cell, 2(4), pp.275-278.
- Simões, M.F., Sousa, J.S. and Pais, A.C., 2015. Skin cancer and new treatment perspectives: A review. Cancer letters, 357(1), pp.8-42.
- Jerant, A.F., Johnson, J.T., Sheridan, C.D. and Caffrey, T.J., 2000. Early detection and treatment of skin cancer. American family physician, 62(2), pp.357-368.
