Chronic muscular intractable pain in otherwise normal healthy individual is often caused by muscle spasm or inflammatory muscular disease. Musculoskeletal pain of severe intensity causes restriction of indoor and outdoor activities. Patient prefers to restrict activities since activities leads to increase pain. Muscle contraction or joint movement provokes severe pain. Patient is desperate to get some pain relief to maintain near normal healthy lifestyle. Trigger point pain is local and; pain is increased with palpation and pressure over painful tender area. “Jump sign” is when patient jumps on palpation because any pressure over tender area (trigger point) causes increase intense pain. “Jump sign” is often seen in fibromyalgia and myofascial pain syndrome. Generalized pain following exercise and sporting activities may exhibit few painful trigger points. Muscular pain following sporting activity subsides after rest of few days and also respond to anti-inflammatory medications. Trigger point injection should not be considered for such acute pain. Chronic trigger point pain not responding to pain medications and physical therapy is considered for trigger point injection treatment.
Trigger point injection is either cortisone injection or dry needling. Dry needle is performed if patient has a history of allergy to cortisone or local anesthetics. Dry injection is just insertion of needle within group of muscle triggering pain. Muscular pain requiring trigger point injection may be spread over arms, legs, chest, neck, lower back or face.
Clinical Examination Prior to Trigger Point Injection
Patient is examined prior to injection treatment. Examination includes history and physical examinations.
History
- History of pain.
- History of medications.
- History of allergies.
- Family History of similar pain and other.
- Past history of similar pain and other illnesses.
- History of needle tolerance.
- Any complication after previous injection treatment.
Examination
- Examination of painful area – Examination is performed to diagnose tender and painful area under the skin called trigger point.
- Examination is also directed to diagnosed
- Tender painful area should be marked carefully at most tender spot.
- Multiple trigger points are treated by injection of maximum six trigger points at each visit. Examination of area of trigger point includes careful analysis of pain, tender knot and tender spasm.
- Most painful spot of tender area is marked as trigger point.
Indications for Trigger Point Injection
- Muscles spasm or knots causing severe localized pain.
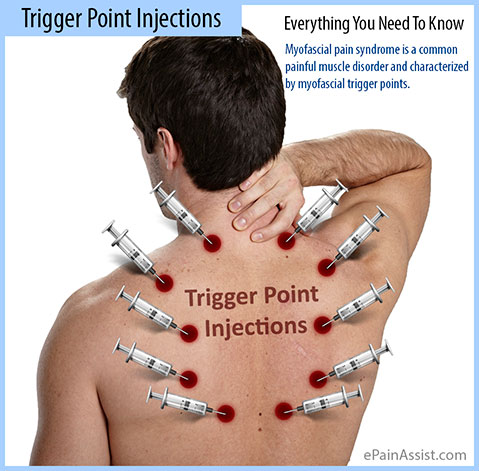
- Myofascial pain syndrome is a common painful muscle disorder and characterized by myofascial trigger points. Myofascial pain syndrome may present with several tender points needing trigger point injections. During each visit maximum six areas of trigger points are treated. Trigger point injection inactivates tender trigger points and relieves severe muscle spasm of surrounding muscles. Pain relief is prompt and helps in continuing physical therapy.
- Fibromyalgia is presented with 11 to 18 painful “jump signs”. Examination may suggest 6 or less focal areas of “jump signs” are extremely tender and painful. These extreme painful areas are considered as trigger point for injection treatment. Severe and generalized pain involving 11 or higher number of painful area cannot be treated by trigger point injection. Widespread pain of severe intensity does not respond to trigger point injection, since local anesthetics and cortisone is injected at restricted volume to prevent side effects and complications. Fibromyalgia patients are suitable for treatment, if severe pain is observed in less than 6 tender spots.
- Tension headache is very painful condition and may present with tender trigger painful area over forehead, side of head, back of head or neck. Injection of tender spots of forehead, temporal, occipital or neck muscles can relieve severe tension headache, which is not responding to medication and manual treatment.
- Sport injury results in inflammatory pain from torn muscles and painful muscle spasm of normal muscles, which are surrounding injured torn muscles. Patient is treated with rest and medications during initial period following injury. After healing patient is often evaluated for physical therapy. Physical therapy sometime is difficult to accomplish, as pain is severe with muscle spam. In similar situations trigger point injection is prefer prior to physical therapy treatment. Effect of injection treatment may last for over 2 weeks and injection can be repeated every 2 weeks until physical therapy treatment is completed.
Contraindications for Trigger Point Injection
- Widespread Muscle Spasm – if pain is generalized and secondary to endocrine disorder then trigger point injection may not relieve generalized pain.
- Fibromyalgia – Fibromyalgia patients with tender and painful area more than 6 are not suitable for injections.
- Local Infection – Trigger points should not be performed in the presence of systemic or local infection.
- Bleeding Disorder – Injection of patient with bleeding disorder or patients on anticoagulation must be done with proper medical evaluation, treatment and monitoring.
- Pregnancy – Avoid cortisone injections in the pregnant patients. Dry needling can be tried and may give pain relief.
- Debilitated Patients – Sick and debilitated patient may not tolerate procedure and may exhibit side effects to cortisone and local anesthetics.
- Allergy to corticosteroid
- Allergy to local anesthetic agents.
- Acute Muscle Trauma– Examination if reveals patient had injury resulting in muscle tear or crush injury, then cortisone injection should not be performed until would is healed or scar tissue has formed. Scarring of torn muscle can cause long-term pain. Such pain can be treated by cortisone injection near or into scar tissue.
Precautions for Trigger Point Injection

- Diabetes Mellitus – Patient with insulin resistant unstable diabetes with moderate to severe hyperglycemia may not respond to anti-diabetic medications. Unstable diabetic patient after cortisone injection may reveal extremely high blood sugar level. Level of blood sugar may not respond to I.V. insulin. Patient may develop diabetic ketoacidosis. In contrast patient with history of mild hyperglycemia can be treated cortisone injection. Cortisone will caused increased level of blood sugar. Such hyperglycemia can be treated with insulin or oral anti-diabetic medication after procedure if necessary.
- Corticosteroid Treatment – If patient is receiving corticosteroid treatment then it is better to avoid trigger point injection with cortisone.
- Fear of Needles – If patient has fear of needles all precautions should be taken to observed and treats conditions like vasovagal shock or hysterical behavior.
Complications and Side Effects of Trigger Point Injection
- Nerve Injury – anytime needle is inserted in the muscle or viscera there is a possibility of nerve injury. Nerve injury is not common. Experience physician, anatomical knowledge and use of monitoring equipment such as X-ray and ultrasound has eliminated nerve injury
- Bleeding – Tear of veins or capillaries can cause bleeding. Bleeding can be significant if patient has bleeding disorder. Trigger point injections are done within subcutaneous tissue and muscles. Life threatening bleeding is impossible or rare unless needle is place too deep into viscera or major blood vessels.
- Infection – needle placement is invasive procedure. Sterile equipment and clean surface of skin can avoid skin, subcutaneous or intramuscular infection. Infection can come through injecting liquid preparation such as cortisone and local anesthetics.
Mechanism of Action
Several mechanisms are speculated to explain the inactivation of trigger points by injection
- Disruption of abnormal muscle fibers.
- Disruption of nerve endings that make up the sensory and motor aspects of the feedback loop, which may be responsible for trigger point activity.
- Needling may cause a local release of intracellular potassium, which triggers depolarization of nerve and thus disrupt nerve conduction.
- Injected fluid may dilute any nerve-sensitizing substances like neurotransmitters. Neurotransmitter induces pain sensation at pain receptors causing conduction of pain impulses to spinal cord. Dilution of neurotransmitters inactivates triggering of nerve impulses resulting in blocking of neural feedback mechanisms.
- Procaine has a local vasodilatation effect that increases circulation at the trigger point. Increase flow of blood causes efficient removal of local metabolites and increasing local energy supply.
- Further, a local anesthetic may interrupt feedback mechanisms between the trigger point and the central nervous system, limiting high frequency discharges transmitted by the nerve.
- Depending on the anesthetic, focal necrosis may destroy the trigger point.
Alternative Treatment Option For Trigger Point Injection
Trigger point injection is invasive procedure and can cause complications such as nerve injury, infection or bleeding. Alternative treatment that could be tried before trigger point injections are as follows-
- Medications – NSAIDs, Neurontin, Lyrica, Cymbalta and Tramadol.
- Massage therapy.
- Physical therapy.
- Spray and stretching.
- Ultrasound.
- Heat treatment – heating pad or infra red light treatment.
- Manipulative therapy such chiropractic or osteopathic treatment.
Trigger Point Injection Procedure
Procedure is performed either at doctor’s office or surgical facilities. Most of the trigger point injections are performed after localizing most painful area (trigger point). Some procedure may need X-ray or ultrasound to guide placement needle. Clean environment, sterilized instruments and sterilized supply must be used to prevent systemic and contact infection. Skin condition should be checked prior to scheduling patient for procedure. Procedure is postponed if patient is having skin rash, bruises skin infection or and systemic infection. Skin should be shaved if necessary prior to procedure. Skin is prepped to remove bacteria, dirt and skin oil. Skin is prep by using chloroprep or duraprep according to recommendation and guidelines set by manufacturer.
Synthetic corticosteroid is injected close to inflame tissue causing trigger point. Appropriate amount of synthetic cortisone mix with local anesthetic such as lidocaine or bupivacaine is injected. Patient is observed in recovery room for any post surgery complication before discharged home.
Cortisone Injection (Wet Needling)
- Needle inserted into trigger point, local anesthesia and corticosteroids
- Several sites up to 6 rigger points are treated as same visit
Dry Needling
- Pain from myofascial trigger points is often treated by needling, with or without injection,
- Although evidence is inconclusive on whether this is effective.
- Several published studies are suggesting direct dry needling was superior to no intervention or no treatment.
Trigger Point Injection Frequency
How many procedures can be done in one calendar month or year? Dry needling can be done as frequently as acupuncture like 2 to 3 times a week for 4 to 6 weeks. Wet needling or corticosteroid injection is repeated every 2 to 3 weeks at one location for initial 6 weeks. Following initial 6-week procedure, it is repeated every 2 months or longer. American Society of Pain Medicine, ASIPP and ASA have described guidelines, which are not specific to disease or number of trigger point. Repetition of procedure depends on pain relief and side effects to cortisone and local anesthetics.
Duration of Pain Relief From Trigger Point Injection
Pain relief may last more than 2 weeks. There is very few research done and published suggesting Outcome of Trigger Point Injection Treatment. Patient would decide to continue treatment after experience of pain relief and duration of pain relief. Patient should discontinue treatment if there are side effects or treatment is not beneficial. Most of the patient suffering with severe intractable pain resulting devastating lifestyle would prefer to have some or any pain relief. Patient would prefer to have injection treatment frequently if there is none side effects and benefits of pain relief over 50%.
Also Read: