What is Myofascial Pain Syndrome or Chronic Myofascial Pain?
Myofascial pain syndrome or chronic myofascial pain is a chronic pain disorder characterized by chronic pain caused by multiple trigger points and fascial constrictions.1 In myofascial pain syndrome, compression on sensitive points in the muscles, which are also known as trigger points, cause pain in unrelated parts of the body also known as referred pain. Myofascial pain syndrome or chronic myofascial pain usually occurs after a muscle has been contracted frequently resulting in pain and inflammation in the body’s soft tissues. Myofascial pain primarily affects the fascia i.e. connective tissue that covers the muscles. It may involve either a single muscle or a muscle group.
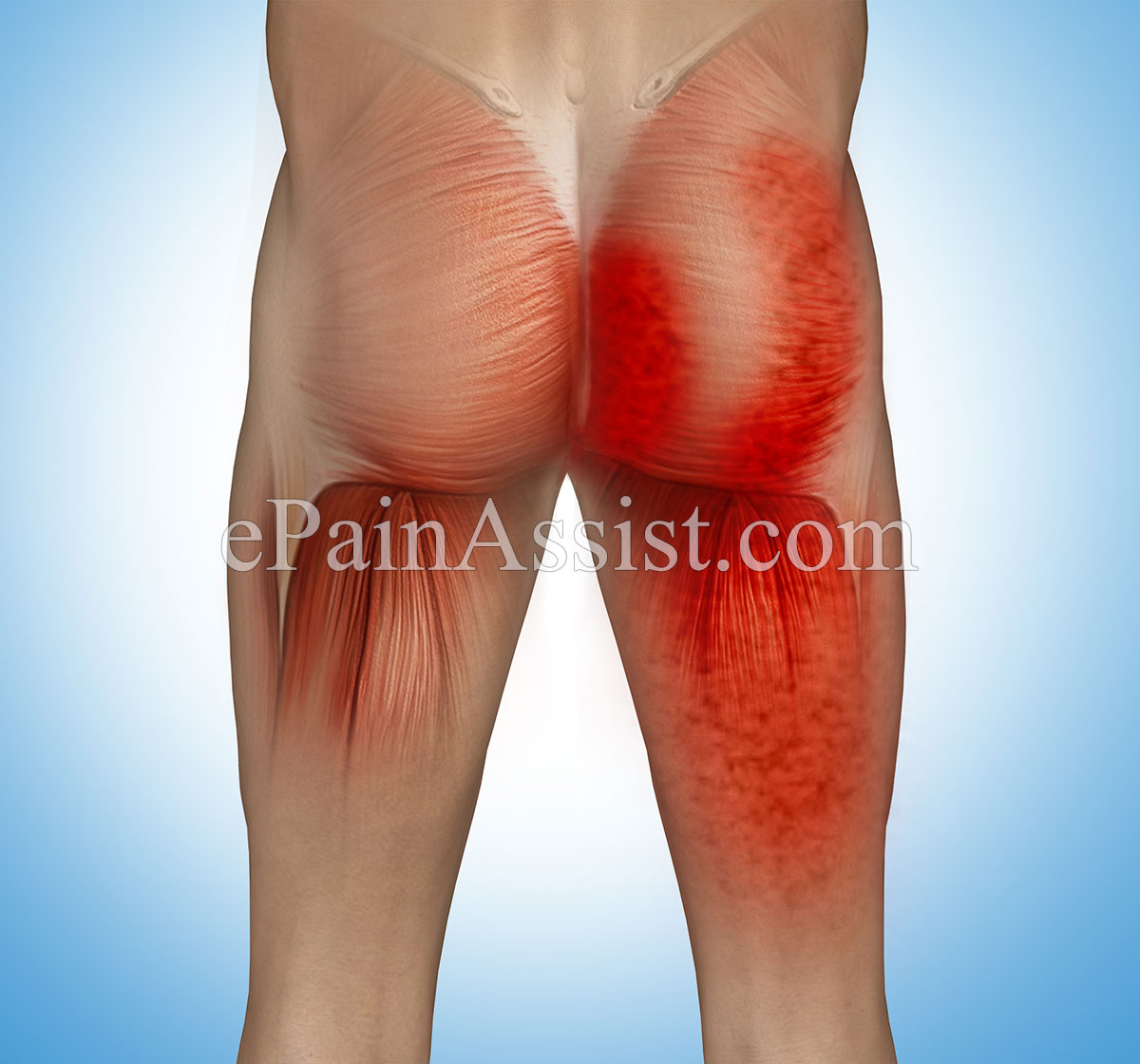
Typical features of a myofascial trigger point are focal point tenderness, pain and hardening of the muscles upon palpation of trigger point, pseudo-weakness of the affected muscle, referred pain, and limited range of motion. The pain or discomfort of myofascial pain syndrome may persist or worsen. Treatment options for Myofascial pain syndrome or chronic myofascial pain include pain medications, trigger point injections, physical therapy and relaxation techniques.
Pathophysiology of Myofascial Pain Syndrome or Chronic Myofascial Pain
There are many changes such as morphological changes, changes in neurotransmitters, neurosensory features, electrophysiological features, and motor impairments occurring in Myofascial pain syndrome or chronic myofascial pain. Morphological changes such as increase in stiffness within the taut band of myofascial trigger points have been found. Changes in neurotransmitters such as increased levels of neuropeptides (substance P or calcitonin gene-related peptide), catecholamines (norepinephrine), and proinflammatory cytokines (tumor necrosis factor alpha, interleukin 1-beta, interleukin 6, and interleukin 8) are present in the active trigger points. Other neurosensory features like referred pain, hypersensitivity to nociceptive stimuli (hyperalgesia) as well as non-nociceptive stimuli (allodynia), mechanical pain sensitivity, sympathetic facilitation of mechanical sensitization, facilitation of local and referred pains, and attenuated cutaneous blood flow responses are also present.
Some studies have discovered spontaneous electrical activity which has been attributed to an increase in miniature endplate potentials and increased acetylcholine release in myofascial trigger points; however, more studies are required to confirm these findings. Motor impairments such as myofascial trigger points may cause changes in normal muscle activation patterns and lead to motor dysfunction.
Types of Myofascial Pain Syndrome or Chronic Myofascial Pain
There Are Two Types Of Myofascial Pain Syndrome or Chronic Myofascial Pain:
Primary Myofascial Pain Syndrome or Primary Chronic Myofascial Pain:
This is not related to other medical conditions or disorders. Usually primary myofascial pain syndromes are the overuse syndromes and are named after the structures affected or for common conditions that produce them. Primary myofascial pain syndromes or primary chronic myofascial pain are myogenic headache (chronic tension-type and mixed tension-type/migraine headache), neck pain, shoulder pain, frozen shoulder, low back pain, piriformis syndrome, knee pain and ankle pain. Headaches are a form of referred pain from the muscles of the neck and shoulders. Postural stresses are the most common causes of neck pain, especially forward head posture and forward rolled shoulders.
Secondary Myofascial Pain Syndrome or Secondary Chronic Myofascial Pain:
This occurs in conjunction with other medical conditions. Secondary myofascial pain syndromes or secondary chronic myofascial pain are chronic cervical whiplash neck pain, temporomandibular joint dysfunction, secondary frozen shoulder/ impingement syndrome, rotator cuff tear, visceral pain syndromes (non-anginal chest pain), hepatic referred pain, renal/ureteral flank pain, structural anatomic variations (scoliosis), pelvic torsions, leg-length inequality, radicular pain, postlaminectomy syndrome, rheumatoid arthritis, osteoarthritis (cervical and lumbar spondylosis), hip or shoulder osteoarthritis, Sjögren’s syndrome, fibromyalgia, acute trauma (fractures), soft-tissue injury, postoperative pain, hypothyroidism, chronic infection (candidiasis, parasitic disease) and Vitamin B12 deficiency.
Causes of Myofascial Pain Syndrome or Chronic Myofascial Pain
Chronic myofascial pain can be caused due to a muscle injury or excessive strain in a particular muscle or muscle group, ligament or tendon. Systemic diseases like connective tissue disease may also cause Myofascial Pain Syndrome or Chronic Myofascial Pain. Other causes such as poor posture and emotional stressors can also contribute to myofascial pain syndrome. Injuries or overuse of muscles can lead to sensitive areas of tight muscle fibers in the muscles. These sensitive areas are known as trigger points and they cause strain and pain throughout the muscle. When this pain continues and increases it is known as myofascial pain syndrome.

Common Causes For Myofascial Pain Syndrome or Chronic Myofascial Pain Are:
- Injury to intervertebral discs.
- General fatigue and ill health.
- Frequent and repetitive motions.
- Medical conditions such as heart attack, stomach irritation etc.
- Lack of physical activity or sedentary lifestyle.
Risk Factors for Myofascial Pain Syndrome or Chronic Myofascial Pain:
- Continuous pressure.
- Muscle injury and weakness.
- Stress and anxiety.
- Muscle tightness. (particularly the piriformis, gluteal or adductor muscles)
- Poor hip joint flexibility.
- Lower back injury.
- Pelvic instability.
- Extreme training.
- Weak biomechanics.
- Insufficient warm up.
- Reduced core stability.
- Muscle inequalities.
Signs and Symptoms of Myofascial Pain Syndrome or Chronic Myofascial Pain
Myofascial pain may occur in isolated parts of the body. Any muscle or fascia can be affected causing a variety of localized symptoms. Typically the muscular pain is steady, aching and deep in nature. Depending on the cause and location of Myofascial Pain Syndrome or Chronic Myofascial Pain, the intensity of the pain can range from mild discomfort to excruciating pain. Knots in the muscles may be visible or may be felt beneath the skin. The symptoms of pain associated with Myofascial Pain Syndrome or Chronic Myofascial Pain may increase with physical activity or stress. Myofascial Pain Syndrome or Chronic Myofascial Pain patients may also suffer from symptoms related to depression, fatigue and behavioral disturbances.
Common Symptoms of Myofascial Pain Syndrome or Chronic Myofascial Pain Are:
- Deep and aching pain in the muscles.
- Increasing pain.
- Local muscle tenderness.
- Difficulty sleeping due to pain.
- Depression.
- Fatigue.3
- Behavioral disturbances.
- Irritability.
Diagnosis of Myofascial Pain Syndrome or Chronic Myofascial Pain
Diagnosis of Myofascial Pain Syndrome or Chronic Myofascial Pain is done by way of physical exam where upon palpating the trigger point causes pain. Four types of trigger points are identified:
- Active trigger point is an area of acute tenderness that typically lies within the skeletal muscle and is associated with local or regional pain.
- Latent trigger point is a dormant (inactive) area that has the capacity to act like a trigger point.
- Secondary trigger point is an extremely irritable spot in a muscle that may become active due to muscular overload in another muscle.
- Satellite myofascial point is also an extremely irritable spot in a muscle that becomes active because the muscle is present in the area of another trigger point.
Lab tests such as hypothyroidism, hypoglycemia, and vitamin deficiencies help in identifying predisposing conditions causing Myofascial Pain Syndrome or Chronic Myofascial Pain.
- Complete blood count (CBC).
- Chemistry profile.
- Erythrocyte sedimentation rate (ESR).
- Levels of vitamins C, B-1, B-6, B-12, and folic acid.
- Thyrotropin level.
- Infrared or liquid crystal thermography.
- Needle electromyography (EMG).
- Ultrasonography.
- X-ray.
- MRI.
Treatment for Myofascial Pain Syndrome or Chronic Myofascial Pain
The Following Are The Treatment Options For Myofascial Pain Syndrome or Chronic Myofascial Pain:
- Massage therapy with trigger-point release techniques is usually effective in providing short-term pain relief from Myofascial Pain Syndrome or Chronic Myofascial Pain.
- Physical therapy involving gentle stretching and exercise is helpful in recovering full range of motion and motor coordination.
- Drugs like anti-depressants (primarily SNRIs), anticonvulsants such as pregabalin (Lyrica), and muscle relaxants (baclofen) and sedatives like clonazepam (Klonopin) are used to treat Myofascial Pain Syndrome or Chronic Myofascial Pain.
- Myofascial release involving gentle fascial manipulation and massage is helpful.
- Posture evaluation and ergonomics can also provide significant relief.
- Movement therapies such as Alexander Technique and Feldenkrais Method can also be helpful in treating Myofascial Pain Syndrome or Chronic Myofascial Pain.
- Trigger point injections.
- Applying heat can help relieve muscle tension and decrease pain.
- Ultrasound uses sound waves to increase blood circulation and warmth, which helps in healing the affected muscles.
- Complementary treatments such as acupuncture also help in alleviating discomfort associated with Myofascial Pain Syndrome or Chronic Myofascial Pain.
- Correction of leg-length discrepancies with a heel lift or the use of dynamic insoles is also helpful.
- Indomethacin phonophoresis.
- Electrical muscle stimulation (EMS) with interferential current (IFC), functional electrical stimulation/electrical nerve stimulation (FES/ENS), or high-frequency transcutaneous electrical nerve stimulation (TENS).
- EMG biofeedback.
- Osteopathic manipulation techniques.
- Consultation with a specialist in physical medicine and rehabilitation may be indicated.
- Dry needling.
- Muscle energy techniques.
- Joint mobilization.
- Neural mobilization.
- Ice or heat treatment.
- Lifestyle changes such as exercising, relaxation techniques like meditating, eating a healthy diet, getting enough sleep etc also help in managing Myofascial Pain Syndrome or Chronic Myofascial Pain.
Prognosis of Myofascial Pain Syndrome (MPS) or Chronic Myofascial Pain (CMP)
Prognosis for Myofascial Pain Syndrome or Chronic Myofascial Pain is usually good if treatment is started in the early stage and if the aggravating factors are eliminated. Treatment becomes more difficult as the disease reaches chronic stage.
Also Read:
