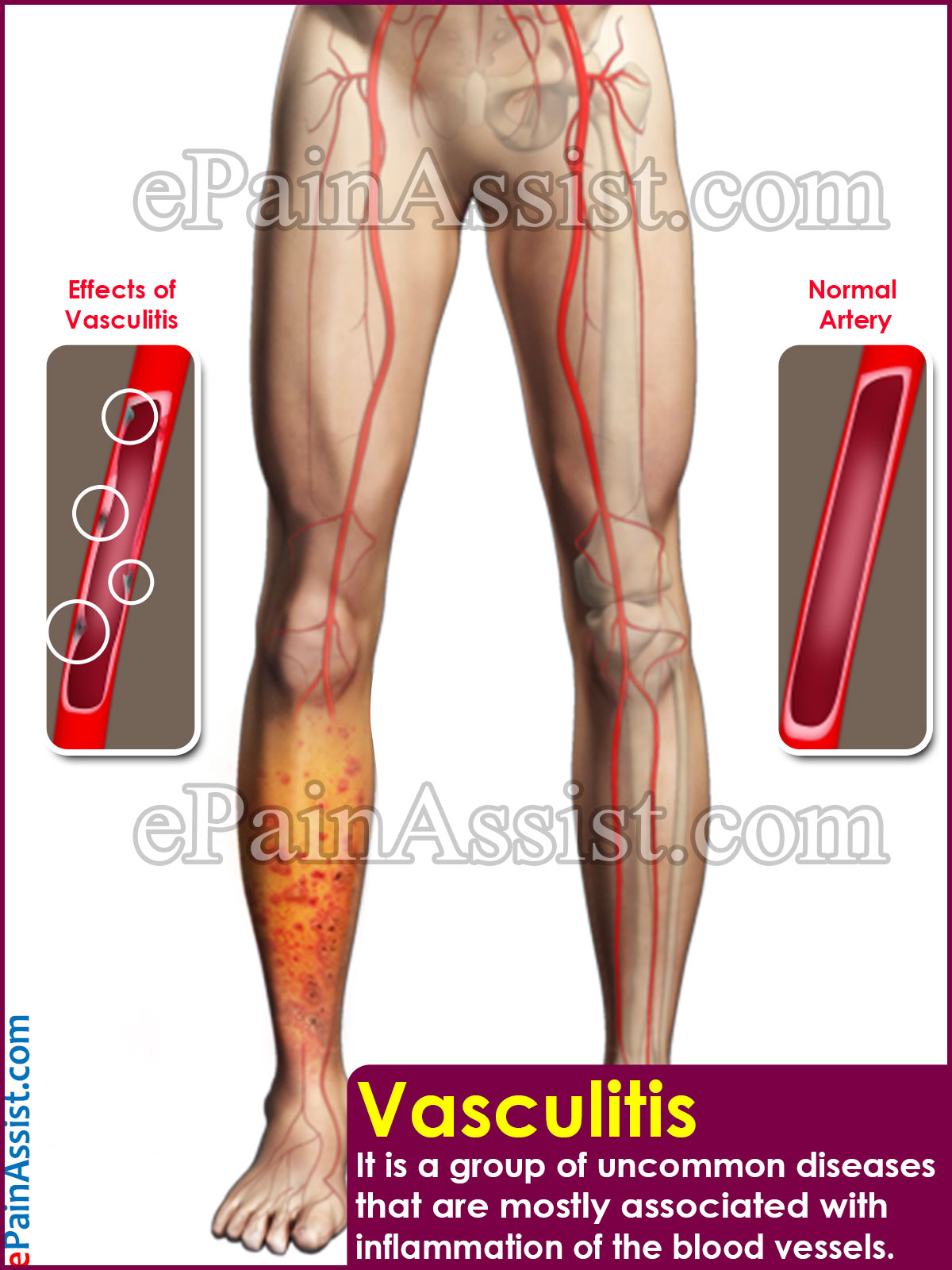
Vasculitis is a group of uncommon diseases that are mostly associated with inflammation of the blood vessels. There are various blood vessels throughout the body. When they come out of the heart, the main blood vessel is called the aorta. This aorta breaks and divides into several arteries to reach the different body parts and internal organs. As the arteries reach the organs to supply blood, they get divided into even smaller arterioles and capillaries. The task is to supply the body parts and organs with oxygen rich blood. Once this task is completed, the blood vessels again get together to form veins and collect the oxygen-depleted blood from the tissues and reach the lungs to collect more oxygen. This oxygen rich blood is then sent to the heart to pump again through the arteries. This entire process runs like a constant and continuous cycle. When the walls of these blood vessels get damaged and inflamed, it is known as Vasculitis.
Definition of Vasculitis:
Vasculitis is a group of uncommon diseases in which the blood vessels, especially the walls get damaged and inflamed.
In Vasculitis, the walls of the blood vessels are either thickened or narrowed or even face scarring. This restricts the blood flow, causing damage to tissues and different organs.
Signs and Symptoms of Vasculitis:
The signs and symptoms of Vasculitis are mostly associated with decreased blood flow to different body organs. They vary to a great extent depending on the organ that is affected or the blood vessels around the organ that are affected as well as the severity of the disease. The general signs and symptoms are –

- Loss of pulse
- Fever
- Night sweats
- Nerve problems
- Headache
- Weight loss
- Rash
- Fatigue
- Aches and pains.
Different Types of Vasculitis:
As already stated, Vasculitis is a group of conditions in which the blood vessels and their walls get damaged. There are different types of Vasculitis and they all have their own signs and symptoms associated with the cause and type of Vasculitis. The common types are –
- Behcet’s Syndrome: This occurs generally in people, who are in their mid 20s and 30s. It causes damage to arteries and veins. The symptoms are eye inflammation, genital ulcers, acne like lesions etc.
- Cryoglobulinemia: Caused by abnormal proteins in the blood and hepatitis C infections, in this condition, numbness and a tingling sensation, along with rash, weakness and joint pain is seen to occur.
- Buerger’s disease: When the blood vessels of your hands and feet are inflamed with blood clots in them, causing ulcers on your fingers and toes as well as pain in arms, hands, feet and legs, it is known as Buerger’s disease.
- Churg-Strauss syndrome: It is also known as Eosinophilic granulomatosis with polyangiitis and is a very rare condition. The kidneys, lungs and nerves are affected in this disease, causing nerve pain, asthma and sinus problems.
- Wegener’s granulomatosis: When the blood vessels of sinuses, nose, lungs, throat and kidneys are affected causing nasal stiffness, nosebleeds and sinus infections, it is known as Wegener’s granulomatosis. Lumps called granulomas are developed by the affected tissue.
- Giant cell arteritis: In this condition, the arteries in the head are mostly affected in people, who are more than 50 years of age. Headaches, blurred or double vision, jaw pain, scalp tenderness and blindness are common symptoms.
- Hypersensitivity vasculitis: In this condition, red spots are seen on the skin around the legs.
- Polyarteritis nodosa: When Vasculitis is associated with hepatitis B infections and causes rash, abdominal pain, muscle and joint pain, kidney problems and high blood pressure, it is polyarteritis nodosa.
- Henoch-Schonlein purpura: Inflammation of the capillaries is known as this condition. Occurring mostly in children, the symptoms include joint pain, blood in the urine, abdominal pain and rash on our buttocks and lower legs.
- Takayasu’s arteritis: When Vasculitis occurs in aorta, it is called by this name. The signs and symptoms include headaches, loss of pulse, numbness of the limbs, high blood pressure and visual changes.
Causes of Vasculitis:
The exact cause of Vasculitis or rather group of diseases is not clearly known. Genetic makeup, however, is often held responsible for Vasculitis. There is often another condition held responsible for this disease and it is when the immune system mistakenly attacks the blood vessel cells. The other common causes of Vasculitis are –
- Blood cancer
- Reaction to certain drugs like amphetamine, anthrax vaccines and cocaine
- Hepatitis B and hepatitis C infections
- Rheumatoid arthritis, lupus and scleroderma and other immune system diseases.
Complications of Vasculitis:
Vasculitis is a condition that can be very serious if not treated on time or properly. Apart from the general symptoms that one will get depending on the type of Vasculitis, the other complications may include –
- Difficulty of the blood to get through the blood vessels. This difficulty will vary from case to case, depending on the thickness of the wall of the blood vessels.
- Sometimes, the blood fails to get through the blood vessels as the space is completely closed off due to thickened walls of the blood vessels.
- When the wall of the blood vessels are so weak and thin that it bulges as a result of stretching. This stretching and bulging is called aneurysm. It is a serious condition that can cause serious and severe conditions like internal bleeding. At times, the internal bleeding becomes so dangerous that it can even cause death.
- The symptomatic damage can include severe problems like vision loss.
- If Vasculitis is severe and blood is not supplied to the body organs, it can cause organ damage.
Diagnosis of Vasculitis:
General body fluid tests and blood tests done in the laboratory can indicate the inflammation in the body. The level of C-reactive protein can be checked by a blood test. Anti-neutrophil cytoplasmic antibodies test can also diagnose Vasculitis. X-rays, computerized tomography (CT), ultrasound, positron emission tomography (PET) and magnetic resonance imaging (MRI) etc. are non-invasive imaging techniques which helps the doctor to diagnose the affected blood vessels and also to check the progress of the treatment. Sometimes, angiography and biopsy are also done to diagnose Vasculitis by collecting a tissue sample from the affected area.
Treatment of Vasculitis:
Depending on the severity of illness and the involved organs, the doctor determines the treatment procedure for Vasculitis. The diagnosis plays a very important role in determining the cause of Vasculitis and the line of treatment. When Vasculitis is the result of an allergic infection, no treatment is required and the condition disappears as the allergy is treated or gone away. On the other hand, when Vasculitis involves critical organs like brain, lungs and kidneys, timely and aggressive treatment are needed.
Usually, medicines that are related to cortisone, like prednisone or methylprednisolone (Medrol) etc. corticosteroid drugs are prescribed to treat vasculitis. These drugs are used to reduce the inflammation of the blood vessels. Sometimes, methotrexate (Trexall, Rheumatrex), azathioprine (Azasan, Imuran) and cyclophosphamide etc. immune suppressant drugs are prescribed to reduce the inflammation of the blood vessels. When the patient suffering from Vasculitis is unresponsive to corticosteroid drugs, then only these immune suppressant drugs are prescribed, since these have severe side effects.
Chemotherapy drugs are also prescribed at times to the patients suffering from Vasculitis. The purpose is to suppress the abnormal immune response that is the cause of the blood vessel inflammation. However, in these cases, the dose of the chemotherapy drugs is lesser than a cancer patient.
Coping with Vasculitis:
There was a time in the past decades, when the patients with Vasculitis survived only for a few weeks or months. However, with advancement of treatment procedures, the patients can nowadays lead a normal life span. For this, a prompt diagnosis and proper as well as aggressive treatment for Vasculitis is a must. To make sure that the side effects are not too severe and that the medications do not leave their harmful effects behind, regular follow-ups are must. Once Vasculitis is treated, the medications can well be withdrawn with the hope that the remission will last long. However, there is no guarantee that the doctor can predict about the remission time. Hence, regular check-ups are a must.
Vasculitis is not a deadly condition if treated on the very early stage. However, at times and in some of the types of Vasculitis, severe problems may occur if not treated well. Hence, diagnosis on the very first place and proper treatment is a must.
