Degenerative Disc Disease is a condition where degeneration of the intervertebral discs of the spine occurs. It is a condition which results from wear and tear changes of the discs of the spine and it can occur in any part of the spine.1 Degenerative Disc Disease involving the spine of the neck is called as cervical disc disease. When it involves the mid-back, it’s called thoracic disc disease. When degenerative disc disease involves the lumbar region, it is called lumbar disc disease.
Degenerative Disc Disease can be a very painful condition and can hamper day-to-day activities of people suffering from it. Degenerative Disc Disease is a spinal condition where the discs in the spine have been damaged or have undergone degeneration. It is not really a disease but is a degenerative condition that produces pain from a damaged disc. Degeneration of the discs is a natural part of aging and as the time goes on, all people will exhibit degeneration in their discs, and however, not everyone develops symptoms as Degenerative Disc Disease varies from person to person in its nature and severity.
The spine is designed such that the vertebrae are “stacked” together to provide a flexible support structure. The spine also protects the spinal cord along with its nervous tissue that extends from the brain down to the spinal column from injury. The discs are pads that serve as “cushions” between each vertebral body. These acts as shock absorbers and help in minimizing the impact of movement on the spinal column. The discs are structured with a central softer component (nucleus pulposus). Due to injury or degeneration, this softer component may sometimes rupture or herniate through the surrounding outer ring (annulus fibrosus) and irritate adjacent nervous tissue. Each of the vertebrae is attached by ligaments and they surround each of the discs. As the disc degenerates, the ligaments are injured and produce localized pain in the area.
Types of Degenerative Disc Disease
Based On The Part Of The Spine Affected, The Types Of Degenerative Disc Disease Are As Follows:
Cervical Degenerative Disc Disease
One of the common type of degenerative disc disease is cervical degenerative disc disease. This condition is a common cause of neck pain. It is usually felt as stiff neck. However, many people don’t even know they have cervical degenerative disc disease.2 They may only become aware of this condition when they are being examined for another health problem or during routine checkups. When the nerves in the cervical spine are irritated, it leads to cervical radiculopathy which causes painful burning or tingling sensations in the arms. Wear and tear of cervical discs leads to degeneration of cervical spine. A fall or a twisting injury to the disc space can induce degeneration of the cervical spine. Symptoms of Cervical Degenerative Disc Disease are chronic neck pain, with pain radiating to the head, shoulders, arms and hands, stiff or inflexible neck with numbness, tingling, weakness in the neck, arms, or shoulders along with headaches.
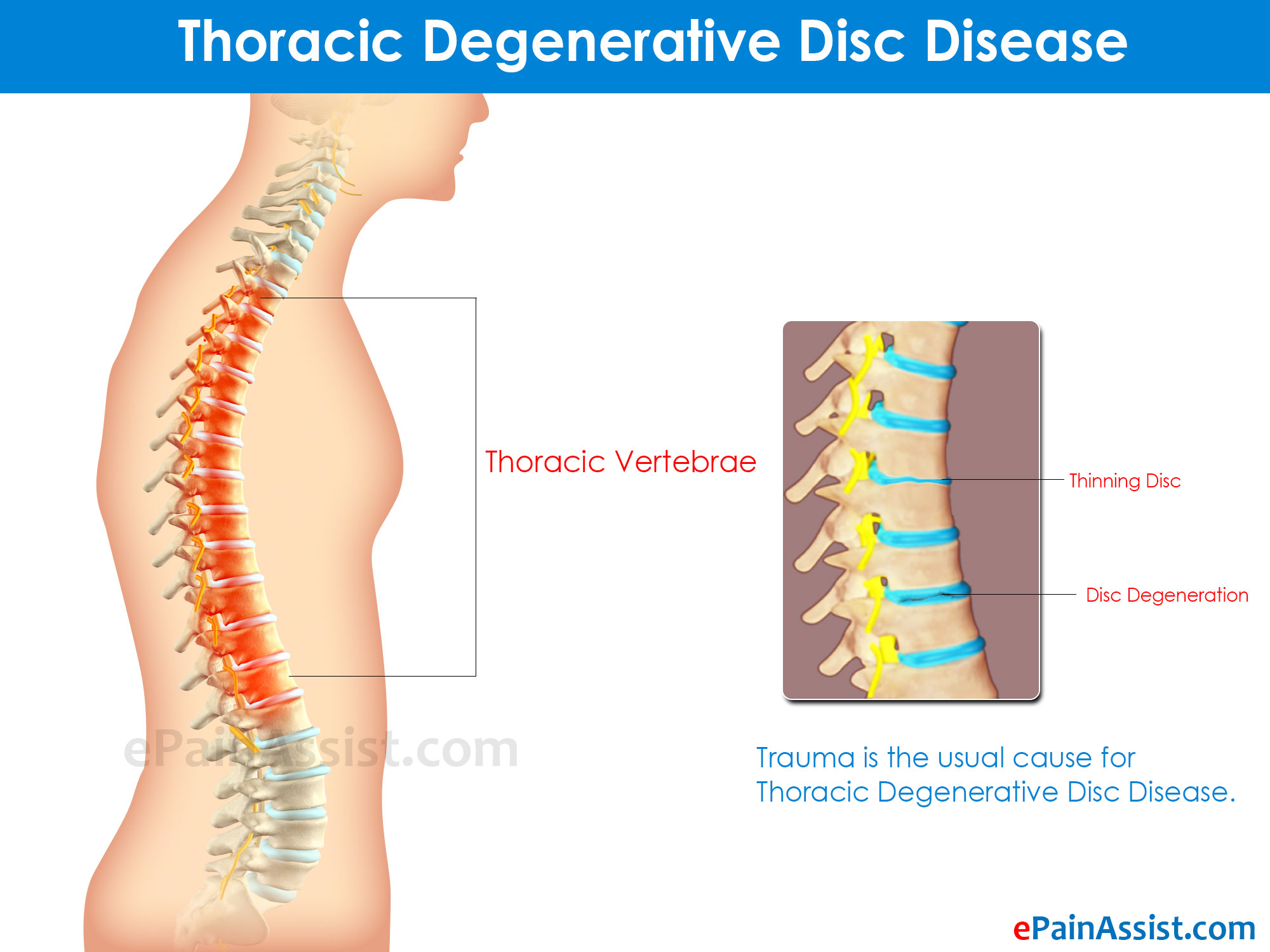
Thoracic Degenerative Disc Disease
Thoracic Spine Degenerative Disc Disease occurs rarely when compared to other parts of the spine. This is because the rib cage stabilizes the thoracic vertebrae, limiting movement and the resultant trauma from frequent flexing and bending. Trauma is the usual cause for this type of Degenerative Disc Disease in thoracic spine. Symptoms are pain when twisting, muscle spasms, slumped posture, bowel or bladder dysfunction. It can be diagnosed by MRI, X-ray, Discogram, CT scan, and Myelogram.
Lumbar Degenerative Disc Disease
This type of degenerative disc disease occurs after a torsional or twisting injury to the lower back; however, wear and tear of the discs in the spine also causes the pain.3 Symptoms of lumbar degenerative disc disease are pain in the lower back sometimes radiating to the hips and legs. Pain that is worse when sitting than standing, walking or even lying down and pain that is exacerbated by movements such as bending, twisting or lifting.
Pathophysiology of Degenerative Disc Disease
Intervertebral disc can be differentiated by annulus fibrosus which is tension-resisting and a nucleus pulposus, which is compression-resisting, formed mainly of proteoglycan. Annulus and nucleus provides mechanical stability to the disc. Degenerative Disc Disease of lumbar spine is quite a serious health hazard and needs to be taken seriously.
The intervertebral disc has three components. These are gelatinous nucleus pulposus, annulus fibrosus, and cartilage endplates. These are present in the superior and inferior portions. Outer annulus fibrosus has abundance of type-I collagen. It is resistant to maximal stress because collagen fibers traverse obliquely between lamellae of annulus in separate directions. The nucleus pulposus is made of proteoglycan as well as water gel, which are joined together lightly by an irregular network of fine type-II collagen as well as Elastin fiber. Aggrecan is name given to the chief proteoglycan of nucleus pulposus. This provides osmotic properties required to endure compression. This disc is termed as the biggest avascular tissues of the body. Vessels present in subchondral bone that adjoin hyaline cartilage in the endplate are responsible for providing nutrition to disc tissues. Glucose as well as oxygen, which are small molecules, passes through endplate as a result of a passive diffusion process. The cells present in disc control numerous materials like cytokines, enzymes, growth factors thus maintaining biological metabolism of discs. Proteoglycan as well as collagen are produced by chondrocytes, the basic structure of disc. A molecule of proteoglycan is made up of protein core that is linked to extended polysaccharide chains, which are named Keratan Sulfate and Chondroitin Sulfate. Every molecule is bound with hyaluronic acid via a link protein. The most abundant proteoglycan in disc is Aggrecan and constitutes approximately 75% of nucleus pulposus with 25% of annulus fibrosus.
The function of normal disc is to retain water within matrix leading to increased viscoelasticity. The Aggrecan generally has greater osmotic pressure due to water that is retained in nucleus pulposus and can inflate collagen framework. Since nucleus pulposus is situated between vertebral endplates and the annulus fibrosus, hence it is not able to expand, but definitely has potential to expand. This is termed turgor of nucleus pulposus. Normal disc tissue is able to support greater load without collapsing because of high concentration of Aggrecan and this load is transferred equally between annulus fibrosus and the vertebral body at time of flexion and extension of spine.
Several factors are responsible for disc degeneration. There can be genetic predilection to it. Polymorphism generally occurs in region of gene responsible for regulating production of MMP-3. It is called promoter region. The 5-A allele carries a risk of progressive degenerative changes of lumbar discs in elderly population than youngsters. Growth factors like Transforming Growth Factor as well as Insulin Like Growth Factor among others facilitate chondrocytes and fibroblasts into producing extra extracellular matrix along with restraining matrix metalloproteinases production. Increase in level of Basic Fibroblast Growth Factor as well as Transforming Growth Factor facilitates repair of debased matrix. As mentioned, the biggest avascular tissue of body is intervertebral disc. The cells present in center of lumbar disc in an adult are somewhere in the region of about 7 mm far from the nearest blood supply. The blood vessels in soft tissues around the periphery of outer annulus and scant penetration of capillaries in its outermost region provide nutrition to cells in the outer annulus. Poor nutrition of disc is also considered to be one of the causes of disc degeneration.
Degenerative disc disease or disc degeneration is also related to age. Declining nutrition, cell senescence, accumulation of degraded matrix products are thought to be other causes; however, no distinct cause has ever been established. The cells in annulus decrease in concentration with age. The cells from disc also degenerate with age and lose their ability to grow. Degeneration is also hastened due to decreased anabolism/increased catabolism of senescent cells. Even though all discs are of same age, the discs in lower lumbar segments are more vulnerable for degenerative changes when compared to upper lumbar segments. This indicates that mechanical loading can also be a major factor other than natural aging process.
Causes and Risk Factors of Degenerative Disc Disease
The main cause for degenerative disc disease is the wear and tear of the discs due to natural aging process in a human being. This gradual deterioration of the discs between the vertebrae is described as degenerative disc disease.
The age-related changes that cause degenerative disc disease are: The loss of fluid in the spinal discs leads to reduced ability of the discs to act as shock absorbers and decreased flexibility. Loss of fluid also leads to thinning of the discs and narrows the distance between the vertebrae. Other changes are the appearance of tiny tears or cracks in the outer layer (annulus or capsule) of the disc. These cracks or tears cause the jellylike material present inside the disc (nucleus) to be forced out through the tears or cracks in the capsule, causing the disc to bulge, break open (rupture), or break into fragments. As the space between the vertebrae gets narrower, there is less padding between them and this decreases the stability of the spine. This leads to the formation of bony growths called as bone spurs (osteophytes). These bone spurs put pressure on the spinal nerve roots or the spinal cord causing pain and affecting the nerve function.

Other causes of degenerative disc disease include trauma or injury to the spine. An injury causes herniated disc and may begin the degeneration process. Degenerative Disc Disease can also be caused due to hereditary factors.
Risk factors for degenerative disc disease include the type of occupation of an individual (e.g. lifting heavy loads), bad lifestyle such as not eating healthy food, not taking enough calcium, smoking cigarettes etc., bad posture and lack of exercise.
Symptoms of Degenerative Disc Disease
Degeneration of the disc tissue makes the disc more susceptible to herniation. Degenerative disc disease may cause pain symptoms in the affected area. As mentioned before, any part of the spine can be affected by disc degeneration.
Symptoms of Cervical Degenerative Disc Disease
When Degenerative Disc Disease affects the spine of the neck, it is called cervical disc disease. Symptoms of cervical degenerative disc disease includes chronic neck pain, with pain radiating to the head, shoulders, arms and hands. Stiff/inflexible neck, numbness, tingling, weakness in the neck, arms, or shoulders along with headaches are other symptoms of cervical degenerative disc disease.
Symptoms of Thoracic Degenerative Disc Disease
When the degenerative disc disease takes place in mid-back, it is referred to as thoracic disc disease. Symptoms of Thoracic Degenerative Disc Disease are pain when twisting, muscle spasms, slumped posture, bowel or bladder dysfunction.
Symptoms of Lumbar Degenerative Disc Disease
Symptoms of Degenerative Disc Disease in the lumbar spine includes chronic low back pain referred to as lumbago or may cause spinal nerve irritation leading to pain radiating down the leg (sciatica). Lumbago also causes symptoms of pain localized to the low back and is common in older people. The low back pain caused due to degenerative disc disease is usually made worse with sitting, because in the sitting position the lumbosacral discs are burdened three times more than while standing. Chronic low back pain may also radiate to hips. There may be pain in the buttocks or thighs during any activity.
Symptoms of lumbar degenerative disc disease also includes tingling or weakness in the knees and legs. The pain is also felt or increases upon any movement such as sitting, bending, lifting, and twisting. Prolonged sitting or standing increases the pain more. Patients usually feel better when they change their positions. The pain especially is at minimum when the patient is lying down, as this relieves stress on the disc space.
Symptoms of lumbar degenerative disc disease also includes pain/discomfort in lower back, stiffness in lower back, burning sensation, tingling and numbness in the buttocks and lower back down to the legs.
Other Common Symptoms of Degenerative Disc Disease
Degenerative Disc Disease also makes the discs more prone to herniation. Degenerative disc disease leading to herniation causes nerve irritation referred to as radiculopathy. When the neck portion is affected, it is called cervical radiculopathy leading to painful burning or tingling sensations in the arms. When the nerves in the back portion are affected, it is called as lumbar radiculopathy. This usually causes “sciatica,” a pain that shoots down towards lower extremities accompanied by numbness and tingling sensation. The pain increases with movement and in more acute cases causes incontinence of the bladder and/or bowels.

Treatment for Degenerative Disc Disease
Most of the time, Degenerative Disc Disease can be successfully treated with conservative treatment consisting of medications to control inflammation and pain with physical therapy and exercise. If the patients have not achieved relief in over six months of conservative treatment and Degenerative Disc Disease is significantly affecting the patient’s ability in performing everyday activities, only then surgery is considered.
Treatment for Cervical Degenerative Disc Disease
Conservative Treatment for Cervical Disc Degeneration:
- Activity modification.
- Exercise helps in relieving stiffness caused by cervical degenerative disc disease.
- Applying ice or heat is an effective treatment to ease the symptoms of cervical degenerative disc disease.
- Non-Steroidal Anti-Inflammatory medications (NSAIDs).
- Analgesics such as acetaminophen.
- Prescription medications like oral steroids, muscle relaxants, or narcotics maybe prescribed to treat cervical degenerative disc disease.
- Physical therapy or chiropractic manipulation can also help treat the symptoms of cervical degenerative disc disease.
- Cervical collar, cervical pillows, or neck traction can be effective in treating the symptoms of cervical degenerative disc disease. All these measures help in stabilizing the neck and improve the alignment of the cervical spine.
Surgical Treatment for Cervical Degenerative Disc Disease:
If the pain caused due to cervical degenerative disc disease is not relieved within six months of non-surgical care, then fusion is recommended to stop the motion of the affected cervical segment of the spine.
Treatment for Thoracic Degenerative Disc Disease
Conservative Treatment for Thoracic Disc Degeneration
- Rest
- Massage is an effective treatment to relieve the symptoms of thoracic degenerative disc disease
- Non-Steroidal Anti-Inflammatory (NSAIDs)
- Prescribed pain relievers
- Physical therapy is also an effective conservative treatment for thoracic degenerative disc disease
- Chiropractic manipulation
- Exercise is the best way to treat thoracic degenerative disc disease
Surgical Treatment Thoracic Degenerative Disc Disease
If the non-surgical methods are not effective in treating symptoms of thoracic degenerative disc disease then a surgical procedure called discectomy is considered as a last resort. This involves removing the disc or the bulged area that is pressing on the neural tissues. Instability results from removing the disc and therefore the bones may need to be fused. This requires bone grafting into the intervertebral space and metal hardware to hold the bones together.
Treatment for Lumbar Degenerative Disc Disease
Conservative Treatment for Lumbar Disc Degeneration:
- Applying heat or ice packs works best for treating the symptoms of lumbar degenerative disc disease
- Exercise
- Non-Steroidal Anti-Inflammatory (NSAIDs) medications
- Pain relievers such as acetaminophen
- Prescription medications like muscle relaxants, oral steroids, and narcotics are effective in treating the symptoms of degenerative disc disease
- Epidural steroid injection provides relief from low back pain by injecting medication directly in to the painful area of the spine to decrease inflammation.
- Chiropractic manipulation
Surgical Treatment for Lumbar Degenerative Disc Disease
If the pain caused due to lumbar degenerative disc disease is severe and continues even after six months of extensive non-surgical care then lumbar spinal fusion surgery is recommended. The most common type of fusion is a one-level fusion at the L5-S1 segment and this does not affect the motions of the back. Whereas a fusion at the L4-L5 segment removes some of the normal motion as this is a major segment of the lower back. Multi-level fusions increase the risks.
Another surgical treatment option for lumbar degenerative disc disease is artificial disc replacement. In this method the disc is replaced instead of fusing the disc space together. Normal growth in the lumbar spine is more maintained in this method of treatment.
Other Surgical Options For The Treatment Of Degenerative Disc Disease Are As Follows:
- Anterior cervical discectomy and fusion
- Micro-discectomy
- Cervical corpectomy
- Dynamic stabilization
- Facetectomy
- Foraminotomy
- Intervertebral disc annuloplasty (IDET)
- Intervertebral disc arthroplasty
- Laminoplasty
- Laminotomy
- Percutaneous disc decompression
- Percutaneous Laser Disc-Decompression (PLDD)
- Spinal decompression
- Spinal laminectomy.
Investigations Done to Diagnose Degenerative Disc Disease
- EMG/Electromyogram.
- NCV/Nerve Conduction Velocity.
- CT scan.
- MRI test.
- Radiographic studies such as x-ray.
- Discography.
Also Read: