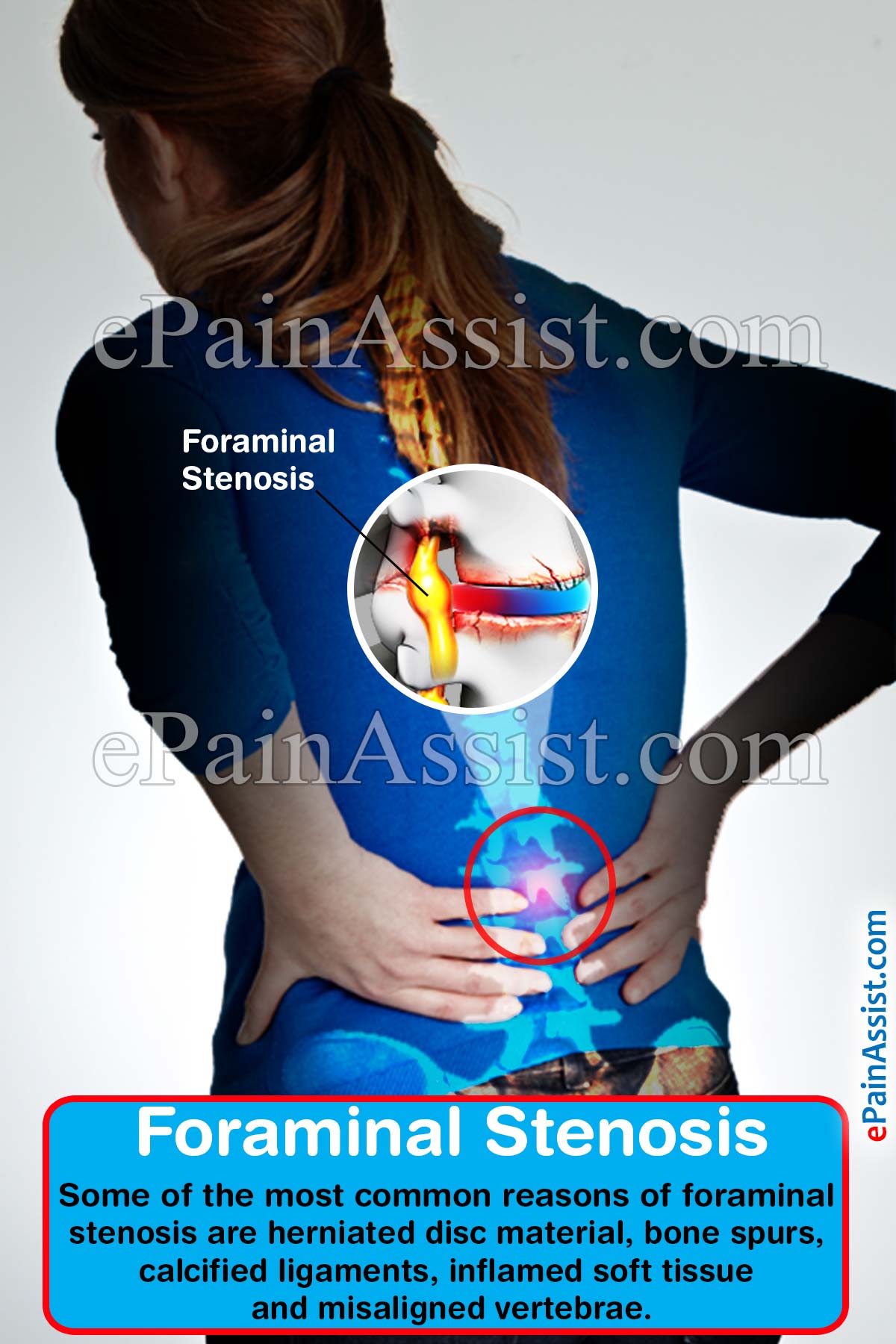
It is narrowing or restriction of openings within the spine called as foramen, which allows the nerve roots to pass to and from the spinal cord. Foramen is the cavity through which spinal nerves pass through as they exit the spine.(1) These apertures or openings are prone to narrowing when there is degeneration of spine and it starts to affect vertebrae, intervertebral discs and other tissues comprising the spine. There is a foramen present at each level of the spine with one on each side. Spinal nerve passes through the foramens at each level. As the foramen is a small area, anything encroaching on that area leads to foraminal stenosis and pinches the nerves. Foraminal stenosis is usually a form of degenerative disease of the spine, which occurs gradually with normal wear of spinal column. Different conditions like arthritic changes of spine, herniated disc, and bulging disc, swelling of soft tissues, and bony growth encroach on foramen and leads to compression of nerve in it. Nerve root compression causes a variety of symptoms like localized pain, pain that radiates along the length of the compressed nerve, tingling, numbness or muscle weakness in the extremities. Mostly foraminal stenosis occurs along with degenerative disease of the spine, but it can be present as a primary problem in some patients. It may cause symptoms at only one level or at many levels if many foramina are involved. Some of the most common reasons of foraminal stenosis are herniated disc material, bone spurs, calcified ligaments, inflamed soft tissue and misaligned vertebrae. In many cases, stenosis can be managed with conservative treatment that is designed to alleviate pressure on the lower back and allow the body to heal. Treatments include rest, physical therapy, using braces, hot or cold compresses, pain medication and corticosteroid injections. If all this fails, then surgery is recommended.
Classification and Types of Foraminal Stenosis
The foramina are openings on each side of vertebrae, which permit passing of nerve root originating from spinal cord. Bilateral narrowing of foramina is narrowing of both foramina. In unilateral only one foramen gets affected. Far-lateral stenosis is narrowing of an area surrounding nerve roots after its exit from foramen. This condition can be as a result of an injury or due to degeneration of spine such as herniated disc, bulging disc etc. in association with normal aging. Foraminal narrowing gets symptomatic if restricted space gives rise to compression of nerves resulting in symptoms like pain, numbness, tingling, weakness etc. Foraminal narrowing has the potential of occurring in any level in the spine, but most common are cervical and lumbar region. Due to stability of thoracic region, the spine in that region is protected against degeneration due to aging process but in the case of neck/lower back, there is continuous stress on it due to movement as well as supporting weight of body resulting in degeneration.
Types of Foraminal Stenosis
There Are 3 Types Of Foraminal Stenosis Depending On Its Location
- Foraminal Narrowing In The Cervical Region: Affects head, shoulder, upper portion of back, upper extremities.(2)
- Foraminal Narrowing In The Thoracic Region: Affects ribcage, shoulders, and internal organs.
- Foraminal Narrowing In The Lumbar Region: Affects lower back, lower extremities, buttocks.(2)
Cervical Foraminal Narrowing: This causes pain slowly as the time goes on. In its early stages, there occasionally may be discomfort usually associated with a particular activity such as riding a bicycle or sitting at a desk for a long period of time. It may be mistaken for a muscle strain in the areas of the neck or upper back. Foraminal narrowing or stenosis is the narrowing or restriction of the space from where nerve roots exit the spinal cord. The foramina are openings on either side of vertebrae through, which nerve roots branches off spinal cord. Injury may cause narrowing of these apertures, but this narrowing is mostly caused by years of wear and tear borne by the spine. As the spine ages, it becomes more susceptible to inflammation or deterioration. Joints become enlarged and intervertebral discs may lose their elasticity and begin to bulge or herniate. Usually this degeneration may not always be a cause for concern. If a nerve root becomes compressed because of foraminal narrowing, it produces debilitating pain, tingling, numbness, or muscle weakness. When the foramina within the cervical region become restricted, it produces symptoms in the neck, upper back, shoulders, arms, hands and fingers. Treatment consists of using pain medication, exercise, corticosteroid injections or other conservative methods. If the conservative methods have been ineffective then the doctor may recommend surgery.
Thoracic Foraminal Stenosis: The symptoms of thoracic foraminal stenosis are similar to thoracic spinal stenosis. The difference being that in thoracic foraminal stenosis there is narrowing of one or more vertebral foramen. Usually age is the cause of this stenosis due to disc bulging or herniation. Thoracic foraminal stenosis may be congenital or degenerative, the latter being the more common cause of this condition. As degeneration increases, pain also increases either during or after activity or with prolonged periods of standing. In patients who are suffering from congenital thoracic foraminal stenosis, a minor injury may accelerate the symptoms as the canal is already narrowed and compression occurs easily. Treatment consists of anti-inflammatory and over the counter medications and physical therapy. Cortisone injections also provide relief although there is a limit as to how many injections a patient can have over a specific duration of time. If there is no relief from the traditional or conventional treatments then surgery may be recommended. The most common procedure is a laminectomy or spinal fusion. The main aim of these procedures is to offer relief from the pressure and compression in the spinal canal. Minimally invasive surgery is also an option that should be explored, as they have quick recovery time in addition to a small incision, thus resulting in minimal scars and tissue formation.
Lumbar Foraminal Stenosis: Foraminal narrowing of the lumbar spine is a gradual, degenerative process that results in lower back pain and neuropathic symptoms like sciatica. Foraminal stenosis may go completely undetected if the passages do not narrow to the point that they constrict the nerves and cause symptoms. Treatment depends on the source and severity of the stenosis, but conservative and nonsurgical treatments often provide sufficient pain relief. If lower back pain does not abate with conservative methods then surgery is recommended.
Pathophysiology of Foraminal Stenosis
When osteophytes are formed anteriorly or posteriorly, this leads to physiological stress. Posteriorly, it constricts the intraspinal diameter and causes lateral stenosis and impingement of the spinal cord. As the human body ages, the discs dehydrate and lose their moisture causing compression and bulging leading to tilting, slippage or rotation of vertebral bodies. These compressed discs result in shortening of the spinal column, which causes the ligamentum flavum to buckle inward and compress the nerve roots producing symptoms like pain, numbness, tingling and muscle weakness. Almost all the individuals in their seventies have some degree of spinal stenosis on imaging studies, but only a small portion of them produce true symptoms of central and/or foraminal stenosis. Usually, patients with lumbar spinal stenosis have chronic pain in the back, buttocks, and/or legs that slowly worsens over time. Standing or walking upright may cause increase in the symptoms like achy pain, tightness, heaviness, and a sense of weakness in the buttocks and/or legs. These symptoms are usually relieved by sitting down or leaning forward as this increases the space around the nerves. Some patients also find it easier to walk while leaning forward on a shopping cart as this position creates more space in the spinal canal and relieves some of the pressure on the nerves. It is important to rule out any underlying vascular problems in a patient before proceeding further.
Causes And Risk Factors of Foraminal Stenosis
Foraminal stenosis may not always result in nerve compression. Many patients with degenerative spine conditions causing foraminal stenosis remain asymptomatic or experience only mild discomfort. It is almost impossible to predict whether a specific spine condition will or will not lead to nerve compression, because no two patients are alike. Still, it is generally understood that foraminal narrowing increases the risk of nerve compression.
The Conditions Causing Foraminal Stenosis Include
- Herniated disc.
- Bulging disc.
- Spondylolisthesis (vertebral slippage).
- Osteophytes (bone spurs).
- Ligament thickening.
- Osteoarthritis.
- Degenerative disc disease.
- Aging.
- Weight gain.
- Repetitive stress placed on the back or neck.
- Traumatic injury.
- Excessive alcohol and tobacco use.
- Genetics.
These conditions are usually related to the aging process. Osteoarthritis and degenerative disc disease is more common in older people which is why that age group is more vulnerable to foraminal stenosis. One or more of these factors may contribute to the constriction of foraminal canal because of spinal degeneration. Symptoms of foraminal stenosis may range in severity and can affect the upper or lower body, depending on the location of the compressed nerve root whether it is in the neck or lower back. Symptoms include sharp, shooting pain, numbness, tingling, and weakness in the arms or legs.
Risk factors include obesity, smoking, sedentary lifestyles, occupations that require constant sitting, standing, driving, bending, lifting, and twisting and regular participation in high-impact sports.
Signs And Symptoms of Foraminal Stenosis
As the narrowing (stenosis) of the foramen compresses and pinches a nerve, the majority symptoms are related to the nerve that is affected. This varies depending on which foramen is involved. Each foramen consists of one nerve which goes to specific parts of the body. A left-sided foramen contains a nerve which only goes to the left side of the body and therefore, the symptoms will always be on the side of the stenosis. It may affect both sensory and motor function in the area that the nerve normally goes to. Foramen disease in the lumbar region leads to symptoms in the legs. Cervical foraminal stenosis will lead to symptoms in the arms. The pinched nerve leads to basically two classes of symptoms. Firstly, sensory symptoms including pain in the distribution of that nerve as well as numbness, tingling and other sensory abnormalities. Secondly, motor symptoms including weakness, abnormal reflexes and even paralysis in acute cases. The weakness or paralysis is one sided, unless the foramina of both sides are affected, and it is limited to the muscles that are controlled by the affected nerve. Common symptoms of foraminal stenosis are numbness, weakness and sensations of burning, tingling, and pins and needles in the affected extremity.

Treatment of Foraminal Stenosis
In most cases, the symptoms from foraminal stenosis can be managed using a combination of conservative treatment methods. These methods include rest, exercise, stretching, analgesics and anti-inflammatories, as well as corticosteroid injections. Surgery becomes an option only when conservative treatment fails to provide relief. Initially patients are recommended to undergo a period of conservative therapy with rest, physical therapy, braces and/or anti-inflammatory medications and in some patients this is enough to provide relief from the pressure on the nerve and for the symptoms to improve. Other treatment options are spinal injections which help in decreasing the inflammation in the area.
Medications For Foraminal Stenosis Include As Follows:
- Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, aspirin, and naproxen. These help in reducing inflammation and are effective in treating mild to moderate pain.
- Opioid pain medications are stronger, narcotic drugs such as oxycodone, codeine and morphine. These are prescribed to treat moderate to severe pain, however, these drugs are highly addictive so it’s important to use these drugs with caution.
- Epidural steroid injections involve a combination of steroids and anesthetic that is injected directly near the affected nerve root. The steroids help in reducing inflammation and the anesthetic helps in the nerve pain.
- Anti-depressants and anti-seizure drugs are more commonly used in foraminal stenosis treatment because they are helpful in blocking pain signals.
Surgery For Foraminal Stenosis
If all this fails and if the symptoms are severe then some patients will be offered surgical treatment. The procedure generally used to specifically address foraminal stenosis is called a foraminotomy. This procedure opens up the foramen so that the nerve within has more space and is not compressed. Foraminal stenosis surgery typically involves decompressing the affected nerve root and can be performed as an open spine surgery or as an endoscopic procedure. Open spine surgery is a highly invasive operation and may or may not involve a spinal fusion. Complete healing can take up to a year and there is a risk that the foraminal stenosis will worsen.
The Minimally Invasive Alternative For Foraminal Stenosis
An endoscopic foraminal stenosis surgery is considered a minimally invasive approach to the surgery. These procedures usually are performed on an outpatient basis with no hospital stay. Recovery is far less difficult than an open spine surgery.
Investigations for Foraminal Stenosis
- Complete physical and neurological examination.
- X-rays help in ruling out tumors, injuries and other abnormalities.
- MRI (Magnetic Resonance Imaging) is helpful in evaluating the damage or disease in the soft tissues, discs and ligaments with other pathologies of the spine.
- CT Scan (Computerized Tomography) helps in evaluating the shape and size of the nearby structures of the spinal canal.
- Myelogram is a procedure in which an opaque dye is injected into the spinal column. This is the followed by an MRI or CT scan.
- Bone scan can detect fractures, tumors, infections, and arthritis.
Also Read:
