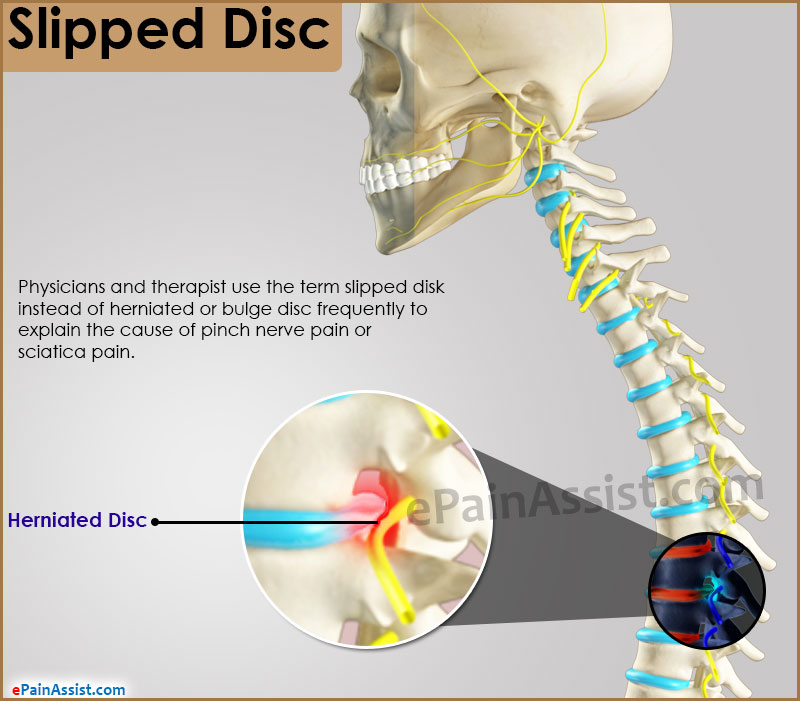
Intervertebral disc lies between upper and lower vertebrae. Disc is immovable and secure in its position between vertebrae and does not slip in any directions. Anatomical changes causing bulge, herniation, protrusion and rupture of the disc are difficult to explain to patient during initial and follow up consultations. Bulged disc, protruded disc or herniated discs are thus explicated in layman’s term as slipped disc. Pain caused by disc anomalies are difficult to explain to general population suffering with pain. Physicians and therapist use the term slipped disc instead of herniated or bulge disc frequently to explain the cause of pinch nerve pain or sciatica pain.
Slipped disc is a generalized term though medically inaccurate and frequently used to describe back and leg pain. Slipped disc is an alternative term used to describe disc bulge, disc protrusion, disc herniation or disc prolapse.
Intervertebral Disc Anatomy
There are 33 vertebrae and 23 discs in vertebral column. There are no disc in sacrum and coccyx. Sacrum and coccyx are lower section of vertebral column. Six discs are located in neck, 12 in middle back and 5 in lower back. Biochemical composition of disc is proteoglycan, collagen and water.
Disc Components
- Nucleus Pulposus (NP)– Jelly like nucleus pulposus lies in the center. Nucleus pulposus is made up of water rich proteoglycans and maintains jelly like consistency. Nucleus pulposus is under heavy pressure because of weight bearing (axial load) in standing and sitting position as well as during activities like flexion, extension and lateral rotation of vertebral column.
- Annulus Fibrosus (AF)– in the periphery tightly covers nucleus pulposus. Annulus fibrosus is tougher than nucleus pulposus because of higher collagen, lower polyglycan and lower water content. Annulus fibrosus prevents escape of soft jelly like content of nucleus pulposus to periphery. The layer of AF is called annulus, because it is made up of 15 to 25 concentric sheets of collagen cartilage.
Disc Function
Intervertebral disc is located between vertebrae. Body weight is transmitted through intervertebral disc. Disc functions as a close hydraulic system to absorb the shock of sudden movement and torque. Central nucleus pulposus is the soft jelly like substance, which functions as hydraulic system to absorb the pressure and volume changes. Pressure and volume changes may occur often during movements and torques. Thus disc is often identified as shock absorber.
Slipped Disc Term Is Commonly Used To Describe Following Disc Injuries
- Disc Bulge or disc protrusion
- Disc herniation or rupture
- Disc fracture or split disc
Disc Bulge or Protrusion of Disc– Term disc bulge or disc protrusion is used to describe out projection of disc or protrusion of disc with intact outer coverings of annulus fibrosus. Nucleus pulposus under pressure bulges or protrudes out from its central position. Nucleus pulposus under pressure pushes annulus fibrosis tissue to periphery causing it to bulge or protrude into foramina or spinal canal. Outer layer of annulus fibrosis is intact in disease of bulge disc and holds the nucleus pulposus from extruding out through its covering. Disc bulge or disc protrusion occurs over period of several months and in most of the cases patient is asymptomatic. Disc bulge is a diagnostic term used to describe anatomical changes in disc as observed in CAT scan or MRI films. Disc bulge may proceed to become herniated disc once annulus fibrosus layer is split. Significantly larger disc bulge or protrusion can cause symptomatic pressure over spinal nerve at foramina or spinal canal.
Disc Herniation or Rupture Disc– Disc herniation is the result of tear or split of annulus fibrosus allowing content of nucleus pulposus to escape outside the outer surface of annulus fibrosus. Herniation is the term used to suggest jelly like nucleus pulposus has passed into space outside its casing of annulus fibrosus. Disc herniation is always symptomatic unlike bulge or protrusion of disc. Nucleus pulposus loses its soft consistency and becomes firm once it is spilled outside annulus fibrosus. Herniated rigid disc occupies space within foramina and spinal canal resulting in space occupying lesion. Herniated disc thus causes severe pain as a result of pressure on one or multiple nerves (pinch nerve) within foramina and spinal canal. Disc herniation most often occurs after whiplash injury or sudden internal pressure changes during torque or movement of vertebral column during lifting or carrying heavy objects. Inflammatory change occurs within traumatized disc and causes secretion of neurotransmitters such as prostaglandin and substance P. Neurotransmitter irritates surrounding nerve and causes severe pain.
Most minor herniation heals within several weeks. Anti-inflammatory medication helps to alleviate pain associated with herniation, protrusion, bulge, or tear of the disc. Symptoms and inflammatory changes caused by bulkier herniated disc may not heal of their own and may require surgical intervention.
Symptoms and Signs of Slipped Disc

1. General Symptoms of Slipped Disc
- Insomnia– secondary to pain.
- Weight loss– result of loss of appetite caused by chronic pain.
- Fever– caused by infection, abscess or discitis.
2. Pain-
- Character- sharp, burning, dull ache and piercing,
- Pain radiate to- arms, hands, leg, feet and buttocks,
- Pain is provoked by – standing, bending, twisting, coughing or sneezing,
- Pain is worst at night.
3. Radiculopathy-1
- Radiculopathy is a condition caused by irritation of sensory nerve. It is presented with symptoms of radicular pain with or without numbness and weakness in extremities. Dermatomal distribution of symptoms depends on level of intervertebral disc causing irritation or pinch of spinal nerve.
- Symptoms are observed in upper or lower extremities following occurrence of slipped disc in neck or lower back.
- Sensory symptoms like tingling and numbness may or may not be associated with pain. Increased pressure or squeeze of spinal nerve within foramina or spinal canal causes increase pinch or squeeze of nerve resulting in sensory distress symptoms like tingling and numbness.
- Muscle weakness and abnormal reflexes indicates irritation of motor nerves when spinal nerve is compressed or pinched. Reflex test of joints in upper and lower extremities are sluggish or absent. Weakness may result in difficulties to straighten sections of arms or legs.
4. Bowel/Bladder Symptoms are observed secondary to spinal stenosis or cauda equina syndrome. Large disc herniation in spinal canal causes spinal stenosis. Large herniated disc puts pressure over spinal nerves or cauda equina in spinal canal causing cauda equina syndrome. Autonomic nerves of bowel and bladder are either irritated or damaged by severe pressure within spinal canal resulting in symptoms such as bladder or bowel incontinence.
5. Paralysis– loss of movement in the arms or legs secondary to spinal cord injury.
Investigations for Slipped Disc
Following investigations are necessary and advised to rule out any differential diagnosis of other spinal diseases causing similar symptoms.
- Blood Tests– Sed rate or CRP is elevated in patients having a history of arthritis or joint or bone inflammation.
- WBC Count– are elevated in patient having history of arthritis, osteomyelitis epidural abscess, etc.
- X-Rays– help in diagnosis of osteoporosis, fracture, foraminal stenosis, degenerative disc disease etc.
- CT Scan– This is essential for diagnosing osteoporosis, fracture, foraminal stenosis, degenerative disc disease, herniated disc, soft tissue injuries etc.
- MRI– This is used quite often for investigating reasons for back pains. It is a reliable study for diagnosis of osteoporosis, fracture, foraminal stenosis, degenerative disc disease, herniated disc. About half of MRIs show bulging discs even when a patient is not having any symptoms and around one fourth of disc ruptures are never found on MRIs.
- Myelogram2– Myelogram is performed quite often and has been a type of a diagnostic test prior to any surgical procedures in past. It is an invasive procedure and is conducted rarely. It is an x-ray study in which a radiopaque dye is injected in the spinal canal. This provides more reliable information in cases of spinal stenosis and foraminal stenosis.
- Ultrasound– Ultrasound gives information regarding blood clots or calcific stones. It is generally used to look for arterial and venous blood clots in lower part of legs.
- EMG– Electromyography studies are performed to look for some sort of damage to nerves as well as to look for radiculopathies.
- Bone Scan– This is done to calculate calcium concentration in bones and is beneficial in diagnosis of bone tumors, compression fractures, osteoporosis etc.
- Bone Densitometry– This is done to look for conditions like osteoporosis.
Treatment for Slipped Disc
Initial treatment of low back pain is based on the assumption that the pain in about 90% of people will go away on its own in about a month.
Medications for Slipped Disc
1. Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- Anti-inflammation– prevents inflammation or decrease inflammatory reaction following disc damage or slipped disc.
- Analgesics– following inflammation of injured disc prostaglandins is secreted by injured tissue. Prostaglandin irritates sensory nerves and causes pain; NSAID antagonizes prostaglandin and prevent transmission of pain impulses. NSAIDS are not effective in treating neuropathic pain.
Most Common NSAIDs are– aspirin, ibuprofen (Motrin, Advil) and naproxen (Aleve).
Risk of Side Effects– complications caused by NSAIDs can be devastating if continued for prolonged period of time.
- Gastrointestinal symptoms- dyspepsia, ulcer, perforation, upper gastrointestinal bleeding.
- Renal toxicity.
- Severe blood loss.
- Myocardial infarction and stroke- NSAIDs with COX2 Inhibitor may increase risk of myocardial infarction and stroke.
2. Tramadol
Also known as Ultram, Ultracet, Ryzolt and Conzip in USA, Ralivia in Canada.
- Analgesic- Used commonly to treat mild to moderate pain.
- Weak mu opioid receptor agonist – Analgesic action is through its effects on mu receptor. Acts as a serotonin releasing agent and norepinephrine reuptake inhibitor. Mu receptor modulation occurs with norepinephrine and serotonin uptake.
- Antagonist with receptors such as NMDA, 5-HT, nicotine acetylcholine and muscarinic acetylcholine receptors.
Naloxone does not reverse analgesic effects of Tramadol.
Physical Dependence and Addiction– with long term use.
Withdrawal Symptoms similar to opioid observed if abruptly discontinued.
Symptoms Following Discontinuation-
- Common symptoms are anxiety, depression, paresthesia, sweating, palpitation, restless leg syndrome, insomnia, vivid dream, tremor and headache.
- Less common symptoms are mood swing, micropsia (object are seen smaller) or macropsia (object are seen larger than real size) are rare but can occur in long-term treatment withdrawal.
- Life threatening withdrawal symptoms such as seizures. Seizure is an atypical withdrawal symptom caused by lower seizure threshold secondary to 5-HT blockade.
Withdrawal symptoms appear in 12 to 24 hours and last several days or weeks.
Potency– Tramadol is less potent than hydrocodone but more effective than codeine.
Metabolite– Primary metabolite O-desmethyltramadol is more potent mu receptor agonist than Tramadol.
Tramadol combined with paracetamol (acetaminophen) provides fast and longer lasting relief that is more effective than either drug alone. This combination therapy has demonstrated efficacy, safety and tolerability for up to two years without the development of tolerance, in the treatment of chronic pain.
3. Opioids for Slipped Disc
- Last Resort– “should be considered only after all other medicinal and nonmedicinal therapies have been exhausted.”
- Widely Used– Chronic pain caused by slipped disc is treated with opioids when all other non-opioid medications failed.
- Benefits– Opioids are beneficial in treating chronic intractable pain. Opioids if used with caution help to maintain near normal indoor and outdoor activities. Opioids are prescribed as a short acting or long acting opioids.
- Tolerance– Continuous opioid treatment for prolonged period of time may result in increased tolerance to dosage. Patient may need increased dosage. Alternatively long acting opioids are prescribed to prevent and overcome tolerance.
- Resistance– Long-term opioid treatment may result in inducing resistance to therapeutic effects of same dosage of narcotics. Resistance can be overcome by alternating short acting opioids with long acting opioids. Alternatively opioid treatment can be discontinued for short period of time or change over to different opioids.
- Addiction– Opioids can cause serious problem such as addiction. Addiction in patients with chronic pain results in continuous use of opioids because of craving for opioids in spite of life threatening side effects. Addiction is also observed in general population when opioids are taken for pleasure and not for pain.
- Pseudoaddiction or Dependence– Pseudoaddiction or dependence to get pain relief is not an addiction and often seen in chronic pain patients. Patients would take more opioids than prescribed dosage to achieve optimum pain relief. Reason for higher consumption is inadequate pain relief with inadequate dosage. Pseudoaddiction is treated with adjustment of dosage and addition of long acting pain medications. Pseudoaddiction may be secondary to resistance and tolerance to opioids.
- Drug Seekers– secure opioid prescriptions from physician by pretending to be a patient suffering with low back pain and sciatica pain caused by slipped disc.
4. Muscle Relaxants
Most commonly used muscle relaxants are Cyclobenzaprine (Flexeril), Soma, Skelaxin and Robaxin.
5. Antidepressants
Treatment using antidepressants were associated with improvements in pain, depression, fatigue, sleep disturbances, and health-related quality of life. Most common antidepressants used are Elavil and Cymbalta.
6. Antiepileptics
FDA has approved Neurontin and Lyrica (pregabalin) as antiepileptic analgesics. Close supervision is necessary to prevent long term use and side effects.
7. Interventional Rx for Slipped Disc
Epidural or caudal cortisone injections.
Biofeedback for Slipped Disc
Electro Acupuncture for Slipped Disc
TENS (Transcutaneous Electrical Nerve Stimulation) – TENS machine delivers small electric pulses into the body through electrodes that are place on the skin. Experts believe TENS encourages the body to produce endorphins, and may possibly block pain signals returning to the brain. Studies on TENS have provided mixed results; some revealed no benefits, while others indicated that it could be helpful for some patients.
Chiropractic Treatment for Slipped Disc
Spinal Manipulation: Osteopathic or chiropractic manipulation appears to be beneficial in people during the first month of symptoms. Studies on this topic have produced conflicting results. The use of manipulation for people with chronic back pain has been studied as well, also with conflicting results. The effectiveness of this treatment remains unknown. Manipulation has not been found to benefit people with nerve root problems. Chiropractor will diagnose by touching (palpitation) and a visual inspection. Chiropractic is known as a direct approach, with a strong focus on the adjustments of the spinal joints. Most good chiropractors will also want to see imaging scan results, as well as blood and urine tests.
Massage Therapy for Slipped Disc
Physical Therapy (Physiotherapy) – The application of heat, ice, ultrasound and electrical stimulation, as well as some muscle-release techniques to the back muscles and soft tissues may help alleviate pain. As the pain subsides the physical therapist may introduce some flexibility and strength exercises for the back and abdominal muscles. Techniques on improving posture may also help. The patient will be encouraged to practice the techniques regularly, even after the pain has gone, to prevent back pain recurrence.
Stretching Exercises for Slipped Disc
- Exercise– Stretching is a group exercise or individual exercise.
- Stretching– Group of muscles are deliberately stretched by extension or flexion of joint. After initial stretching exercise for few weeks, hyperextension, flexion, abduction and adduction of these muscles achieved by joint movements. Goal is to increase flexibility.
- Yoga is an example of therapeutic stretching.
- Swimming and aquatic exercise are also beneficial if water temperature is not too cold or warm. Patients with symptoms of fibromyalgia do not tolerate cold water. Warm water can cause tiredness sooner.
- Tai chi was studied in a small; single blinded randomized controlled trial, resulting in a relative benefit ratio of 2.0 on the Fibromyalgia Impact Questionnaire.
Magnet Therapy for Slipped Disc
Hypothesis– magnet improves blood flow in underlying tissue. Magnetic field is limited in spread and thus does not cause any long-term harm to hemoglobin or any other blood contents.
Alternative Medicine for Slipped Disc
Alternative medicine is an integrative or complimentary medicine to conventional treatment.
Non-responding disease to conventional medicine may respond by changing daily habits of eating, relaxation and stress. Methods are different such as:
- Treatment with herbs
- Spiritual practice
- Healthy eating
- Avoid caffeine
- Practice good sleep
- Adopt cultural traditions
- Homeopathy
- Ayurveda medicine
- Aromatherapy
- Music therapy
- Prayer therapy
- Reflexology
- Massage therapy
- Biofeedback, myofascial trigger point therapy, magnet therapy.
Alternative Medicine is Classified Into These Five Categories, Types, and Lists:
- Alternative Medical systems
- Herbal and Nutritional Medicine
- Mind-Body practices
- Physical Manipulation of the body and spine
- Energy Manipulation Therapies
Surgery for Slipped Disc
Nerve Decompression-4
- Microdiscectomy, percutaneous disc removal.
- Discectomy.
- Laminectomy.
- Spinal Fusion.
Preventive Measures for Slipped Disc
Maintain Decent Postures-
- Sitting: Domestic Chairs- Appropriate, decent lumbar support.
- Automobile Seat– adequate low back support like a small pillow or a rolled over towel.
- Sleeping: Appropriate mattress which is firm. Plywood can also be helpful.
- Lifting– One should not lift objects that are way too heavy. When attempting to lift something, the back should be straight, head looking straight, and lifting should be done with knees. The object should be close to body. One should tighten up stomach muscles so as to keep a balanced back.
Also Read:
- Herniated Disc
- What is Herniated Disc?
- Intervertebral Disc Herniation: Types, Symptoms, Treatment, Diagnosis, Prevention
- Lumbar Disc Herniation: Causes, Symptoms, Treatment-Manual Therapy, PT, Surgery
- Massage Therapy For Disc Herniation or Herniated Disc: Deep Tissue Massage
- What Does A Slipped Disc Feel Like & How to Fix it?
- Predictors of patient-reported recovery from motor or sensory deficits two years after acute symptomatic lumbar disc herniation.
PM R. 2012 Dec;4(12):936-944.e1. doi: 10.1016/j.pmrj.2012.08.023. Epub 2012 Nov 13.
Suri P, Rainville J, Gellhorn A.
Division of Physical Medicine and Rehabilitation, VA Boston Healthcare System, Boston, MA, USA. - Recurrence of radicular pain or back pain after nonsurgical treatment of symptomatic lumbar disc herniation.
Arch Phys Med Rehabil. 2012 Apr;93(4):690-5. doi: 10.1016/j.apmr.2011.11.028.
Suri P, Rainville J, Hunter DJ, Li L, Katz JN.
Veterans Affairs Boston Healthcare System, Boston, MA, USA. - Lumbar discogenic pain, provocation discography, and imaging correlates.
Radiol Clin North Am. 2012 Jul;50(4):681-704. doi: 10.1016/j.rcl.2012.04.013., Maus TP, Aprill CN.
Department of Radiology, Mayo Medical School, Rochester, MN 55905, USA. - Surgical outcome of percutaneous endoscopic interlaminar lumbar discectomy for recurrent disc herniation after open discectomy.
J Spinal Disord Tech. 2012 Jul;25(5):E125-33. doi: 10.1097/BSD.0b013e31825bd111.
Kim CH, Chung CK, Jahng TA, Yang HJ, Son YJ.
Department of Neurosurgery, Seoul National University College of Medicine, Seoul, Korea.