Cholangiocarcinoma, a bile duct cancer, is a rare form of cancer. It is an adenocarcinoma as the initiation of the disease is almost always from the lining of the bile duct. The major function of the bile duct is to carry the bile fluid to the small intestine which then helps in digestion of fats and lipids. The upper part of the bile duct lies in the liver, the middle part is attached to the gall bladder, whereas the lower part enters the initial part of the small intestine known as duodenum. The cancer in the bile duct can start in any of these parts and can spread to the other regions and thus are classified accordingly. Let us have a look at the types, stages and diagnosis of cholangiocarcinoma.
Types and Staging of Cholangiocarcinoma
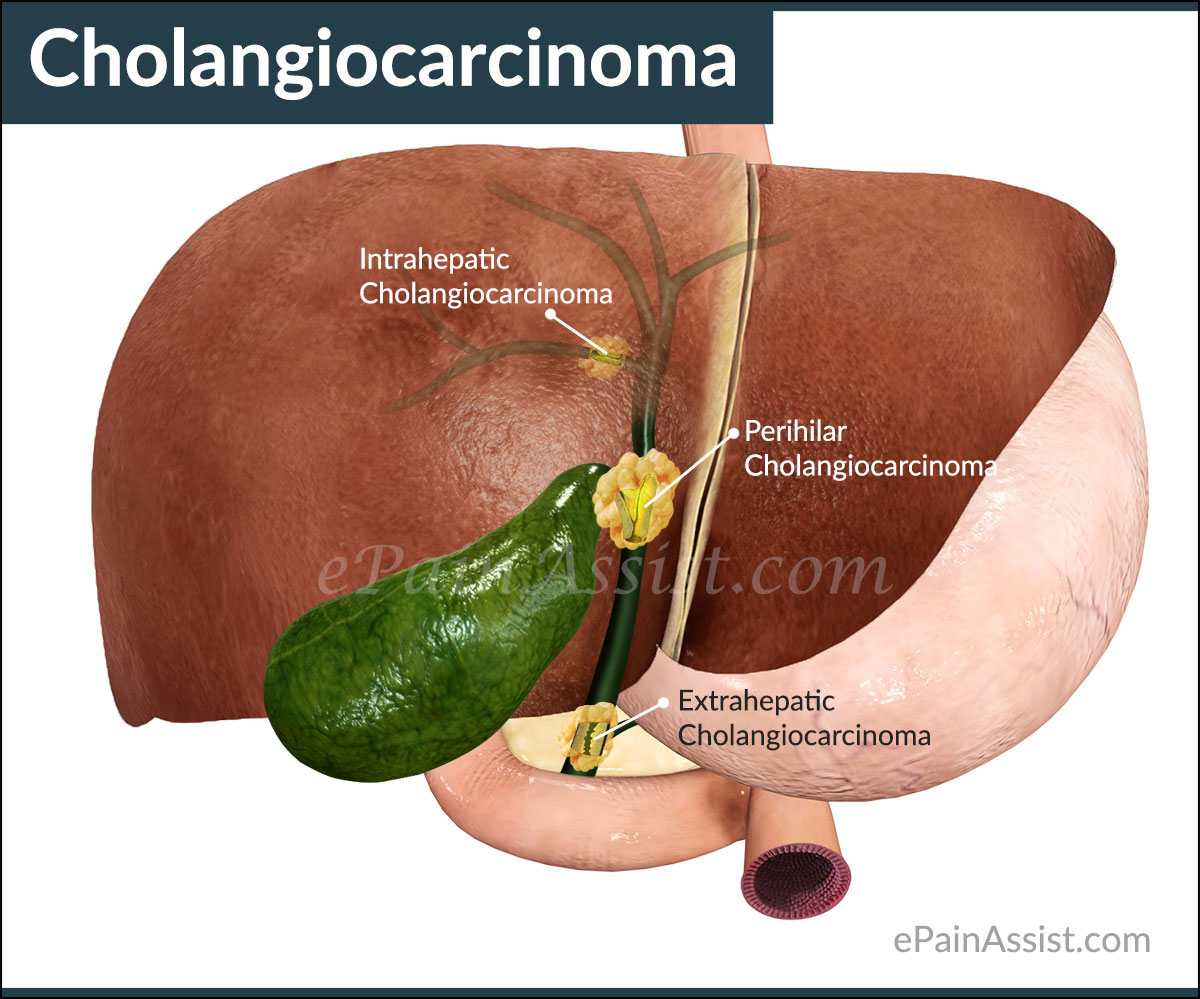
Three most known formations or types of cholangiocarcinoma that affects the bile duct and the liver of patients initially is as follows:
- If the tumor grows in the bile duct within the liver, it’s known as intrahepatic cholangiocarcinoma.
- If the tumor grows in the bile duct but outside and a little far from the liver, it’s known as Extrahepatic cholangiocarcinoma or distal bile duct cancer.
- If the tumor grows on the nodal point where bile duct comes out of the liver, the condition is known as Perihilar cholangiocarcinoma or Hilar bile duct cancer.
Apart from the above three common types of cholangiocarcinoma, there is a fourth condition which normally occurs in the common hepatic duct known as Klatskin tumor.
Understanding the “stage” of cancer is very important for the medical practitioners which help them decide on appropriate treatment. Cancer normally spreads through blood stream or lymphatic system. Staging of cholangiocarcinoma is possible by examining the lymph nodes attached to the biliary system. TNM staging is the most common form of scaling the current status of Cholangiocarcinoma in a patient’s body. TNM stands for Tumor, Node and Metastasis respectively. Here are short descriptions of these really important parameters in different types of Cholangiocarcinoma:
-
Intrahepatic Cholangiocarcinoma or Bile Duct Cancer:
In this type of cancer, the T- stage of cancer may be summarized as follows:
- TX – Tumor cannot be assessed
- T0 – No evidence is found for Primary tumor
- Tis – At this stage the tumor is formed only within the innermost layers of lining on a bile duct.
- T1– One tumor that is formed within the bile duct, but it may have grown deeper into the wall of the duct.
- T2a – The tumor has grown past the wall of the bile duct into the nearest blood vessel.
- T2b – Presence of more than two tumor marks this stage.
- T3 – At this stage two possibilities occur, the tumor may grow into the outer covering of the liver called peritoneum or may grow into any nearby organs just outside the liver like stomach, intestine, abdominal wall or the diaphragm.
- T4 – At this stage the tumor spreads into the liver growing alongside the bile ducts.
N stages of intrahepatic cholangiocarcinoma or intrahepatic bile duct cancer can be narrated as follows:
- NX – Lymph nodes present nearby cannot be assessed
- N0 – It depicts that there are no cancer cells present in the lymphatic nodes.
- N1 – It depicts that there are cancer cells presents in the lymphatic nodes.
M stages of intrahepatic cholangiocarcinoma or intrahepatic bile duct cancer can be narrated as follows:
- MX – Metastases cannot be assessed
- M0 – It depicts that the cancer is not found in tissues and organs situated at a distance from the bile duct.
- M1 – It marks the spread of cancer cells into the other parts of the body at a distance from the bile duct.
-
Perihilar Cholangiocarcinoma or Perihilar Bile Duct Cancer:
In this type of cancer, the T- stage of Perihilar Cholangiocarcinoma or Perihilar Bile Duct Cancer may be summarized as follows:
- TX – The extent of tumor is not possible due to incomplete availability of information.
- T0 – Evidence of primary tumor not found.
- Tis – At this stage, the tumor is only within the inner layers of cells lining the bile duct.
- T1– At this stage, the tumor grows deeper into the walls of the bile duct viz., the muscular or fibrous tissue layer.
- T2a – At this stage, the tumor grows into the fatty tissues present in the bile duct.
- T2b – At this stage, the tumor grows into the liver tissues adjacent to the bile duct.
- T3 – At this stage, the cancer grows into the hepatic artery of the liver.
- T4 – This stage is marked by any of these conditions –
- The tumor grows in one of main blood vessels of the liver like common hepatic artery or portal vein , or
- The cancer spreads in the main blood vessels,
- The cancer spreads on both sides of the liver.
The N stages of Perihilar Cholangiocarcinoma or Perihilar Bile Duct Cancer are narrated here:
- NX – Unable to assess the nearby lymph nodes.
- N0 – This means that there are no cancer cells in the lymphatic nodes.
- N1 – This signifies that there are cancer cells in the nearby lymphatic nodes like the ones nearby to the common bile duct, hepatic artery, portal vein and the cystic ducts.
- N2 – This stage signifies that there are cancer cells in lymph nodes further at a distance from the bile duct.
The M stages of Perihilar Cholangiocarcinoma or Perihilar Bile Duct Cancer can be any of these two:
- M0 – At this stage no sign of cancer cells are detected.
- M1 – At this stage the cancer spreads in other parts of the body at a distance from the bile duct in the main blood vessels like the aorta, vena cava etc.
-
Extrahepatic Cholangiocarcinoma or Distal Bile Duct Cancer
The T stages of Extrahepatic Cholangiocarcinoma or Distal Bile Duct Cancer can be any of the below mentioned stages:
- TX – The extent of tumor is not identifiable.
- T0 – No primary tumor evidence found.
- Tis – At this stage, the tumor grown only on the innermost layer of the bile duct.
- T1 – At this stage, the cancerous tumor has grown on the walls of the bile duct.
- T2 – The tumor grows through the walls of the duct but not in the other nearby structures.
- T3 – At this stage, the tumor reaches into the nearby organs like gallbladder, pancreas, small bowel, duodenum etc.
- T4 – This stage is marked by the cancer having spread to one or both the main blood vessels, the celiac artery and superior mesenteric artery.
The N stages of extrahepatic cholangiocarcinoma or distal bile duct cancer may be any of the following:
- NX – Lymph nodes couldn’t be assessed.
- N0 – This signifies that there are no cancer cells in the lymphatic nodes.
- N1 – This means that cancer has spread to the lymphatic nodes.
The M stages of Extrahepatic Cholangiocarcinoma or Distal Bile Duct Cancer are any of these two:
- M0 – This means that there is no sign of cancer in the tissues and organs at a distance from the bile duct.
- M1 – This depicts that the cancer cells have spread to other parts of the body at a distance from the bile duct.
How is Cholangiocarcinoma Diagnosed?
The following are the most modern form of diagnostic techniques used in detecting this deadly disease of cholangiocarcinoma:
- Tumor Markers to Diagnose Cholangiocarcinoma: The most commonly used markers in this disease are carbohydrate antigen (CA 19-9) and Carcinoembryonic antigen (CEA). CA 19-9 normally possesses a sensitivity of 67%-89% and a specificity of 85%-98% with levels over 100 U/ml. CEA alone is not used to elevate the sensitivity and specificity of cholangiocarcinoma. Studies have shown that 100% sensitivity and specificity are possible when CEA is greater than 5.2 ng/ml used in combination with CA 19-9 greater than 180 U/ml.
- Ultrasonography: The first examination that an oncologist suggests to a suspected patient is an abdominal ultrasonography. Intrahepatic cholangiocarcinoma is generally detectable with ultrasonography, but other types of cholangiocarcinoma like extrahepatic cholangiocarcinoma normally remains undetectable at the primary stages.
- Magnetic Resonance Imaging (MRI): Magnetic resonance cholangiopancreatography or MRCP is an advance form of MRI to diagnose cholangiocarcinoma. MRCP is considered as one of the best choices in the diagnosis of cholangiocarcinoma because of its multi-planar imaging, high contrast resolution, and capability of determining the biliary, parenchymal, and vascular extensions.
- Computed Tomography (CT) Scan: Computed tomography (CT) scan is another form of external imaging system that is capable enough to show the formation of a tumor mass, bile duct wall thickening, bile duct dilatation or formation of intraductal tissues in exophytic, infiltrative, and polypoid cholangiocarcinomas, respectively.
- Cholangeography: In this form of diagnosis of cholangiocarcinoma, fluorescent fluids are used to create contrasting images of bile duct tree to point out abnormalities. There are two types of cholangeography that are done depending upon a patient’s condition, viz. Percutaneous Transhepatic cholangiography (PTC) and Endoscopic Retrograde Cholangiopancreatography (ERCP).
- ERCP: ERCP or Endoscopic retrograde cholangiopancreatography is a modern technique that takes help of endoscopy and fluoroscopy to diagnose and treat certain bile duct cancers. Endoscope is at first pushed in to the stomach and duodenum where through the radiographic contrast the condition of bile duct tree is examined.
- PTC: Percutaneous Transhepatic Cholangiography (PTC) is another technique to diagnose the bile duct obstructions and cancer. In this method, local anesthesia is given in the right side of the abdomen and then a needle is inserted through the skin into the liver. A fluorescent dye is then injected into the bile ducts of the liver wherein x-ray images are taken to diagnose the blockage and abnormality in the ducts. A tissue sample can also be collected for doing a biopsy to analyze malignancy. Pre- and post procedure antibiotics are given to avoid infections and also the patient is kept for overnight observation.
The treatment for cholangiocarcinoma depends on the type and stage of the disease identified from the diagnosis. The earlier the diagnosis of cholangiocarcinoma is made, the better the chances of 5-year survival.
Also Read:
