The arteries, veins and capillaries are the blood vessels of our body. The disease of these blood vessels is called Angiopathy. It is caused due to different factors and one of them is diabetes. Diabetes peripheral angiopathy is a serious complication of diabetes.
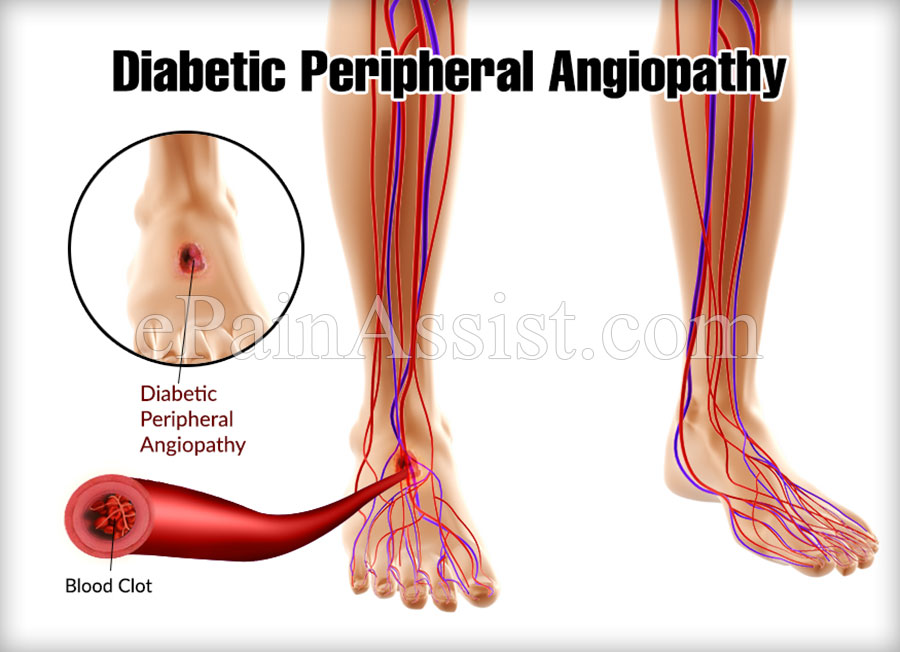
What is Diabetic Peripheral Angiopathy?
When angiopathy occurs as a result of complication of unregulated diabetes, it is termed as Diabetic peripheral angiopathy. It is the most prevalent form of angiopathy. It involves formation of blood clots in blood vessels. Diabetic peripheral angiopathy is of two types: Macroangiopathy and microangiopathy. In macroangiopathy, blood clots are formed in large blood vessels such as the arteries and veins. This causes blockage to the flow of blood. It results in heart attack and stroke. Diabetic peripheral angiopathy affects lower limbs which cause diabetic foot ulcers and has a risk of amputation.
In microangiopathy, blood clots are formed in small blood vessels i.e., the capillaries. The clots make them thick and weak. This obstructs the smooth blood flow throughout the body which impairs supply of nutrients and oxygen. The retina of our eye does not get enough oxygen supply which often develops microangiopathy and causes blindness. This is also known as diabetic retinopathy. Diabetic peripheral angiopathy can also cause damage to the nerve cells and is called peripheral neuropathy. Further, it can also cause renal damage which results in diabetic nephropathy.
Symptoms of Diabetic Peripheral Angiopathy
Diabetic peripheral angiopathy mainly affects the lower limbs. Due to the poor blood supply, the limbs do not get sufficient oxygen and nutrients as a result, they get damaged. This results in leg pain, cramps and muscle pain. In severe cases, the leg pain is difficult to tolerate even when the person is resting. This restricts the movement of the person. Additional symptoms include:
- Lower leg or feet becomes cold and develops numbness for which the person cannot walk properly
- A weak pulse in the leg
- Problem in the skin on the leg
- Legs appear blue in colour
- Wounds on the leg and feet take long time to heal
- Toenails appear thick and opaque.
The final stage is tissue dystrophy where any small bruise leads to formation of unhealed ulcer. It results in gangrene of the foot.
Causes of Diabetic Peripheral Angiopathy
Diabetic peripheral angiopathy is mainly caused due to unregulated diabetes mellitus. The presence of very high glucose levels in diabetes increases the risk of atherosclerosis or plaque formation. Plaque is made of cholesterol and calcium which deposits in the blood vessels and obstructs the flow of blood. Once the blood supply is cut off, the tissues get deprived of nutrients and oxygen which causes their death. This further leads to necrosis and body parts cannot survive. In case of leg and feet necrosis, it has to be amputated.
Diabetic peripheral angiopathy is also caused due to high arterial pressure as seen in smokers, people with excessive alcohol intake and those who work in harmful environments.
Diagnosis of Diabetic Peripheral Angiopathy
Patients who suffer from diabetes mellitus are at a high risk of diabetic peripheral angiopathy. The diagnosis involves:
- A physical examination for a weak pulse and wounds on feet which are slow to heal.
- Both blood and urine samples to be tested for presence of sugar, creatinine, urea and proteins. Determination of lipid profile is also essential.
- Imaging tests such as dopplerography and magnetic resonance angiogram (MRA) to check flow of blood to the limbs, to check the presence of plaques and locate the blockage position.
- Ultrasound of kidneys
- Examination of the eyes
- Electrocardiography, echocardiography, and coronary angiography.
Treatment of Diabetic Peripheral Angiopathy
Proper medications for diabetes and blood pressure are given. Blood sugar levels should be normalized and blood pressure should be within normal limits. Constant monitoring of blood sugar levels is necessary in the management of diabetic peripheral angiopathy.
Medicines that make the blood flow normal and strengthen blood vessels and improve tissue trophism are important in the treatment of diabetic peripheral angiopathy.
When complications develop they are treated as follows:
- Retinopathy is treated with photocoagulation. Further, intravenous administration of parabulbarno or corticosteroid preparations prevents branching of blood vessels.
- In case of renal damage, hemodialysis is advised.
- In case of gangrene, surgery is done where leg amputation takes place.
Prevention of Diabetic Peripheral Angiopathy
When a person is detected to be suffering from diabetes, it is important to regulate the blood glucose levels. Hence prevention of diabetic peripheral angiopathy includes:
- Restricting diet high in sugars and carbohydrates. Instead having diet with moderate amounts of fats and high on proteins is recommended. Taking vitamin supplements and drugs to improve nerve conduction and blood flow is advised.
- One must perform moderate physical exercises to improve blood flow. One should take care that exercises should not result in fatigue since it can cause cardiac arrest, and stroke.
- Regular health check-ups to determine glucose and cholesterol levels are necessary.
- Regular eye check-up to prevent damage to the retina.
- Proper foot care is necessary. People must avoid getting cuts and wounds since they are difficult to heal and can get infected easily.
- Maintaining blood pressure is essential.
Conclusion
Uncontrolled diabetes causes peripheral angiopathy. It is necessary that patients should get diagnosed with this complication and start treatment to control diabetes in time to prevent occurrence of serious consequences.
Also Read:
- Diabetes: Exercise Therapy for Diabetic Neuropathy Pain- Animal Lab Study
- Diabetic Neuropathy: Classification, Types, Causes, Risk Factors, Signs, Symptoms, Treatment
- What Can Cause Diabetes Foot Pain: Treatment, Symptoms, Prevention
- Disability Benefits for Diabetes
- Symptoms & Causes of Peripheral Sensory Neuropathy
