Bell’s palsy is a common form of facial paralysis that was named after the Scottish surgeon, Sir Charles Bell. It usually affects the face unilaterally, i.e. one side of the face; however, in extremely rare cases, it may affect both sides of the face. Bell’s palsy is characterised by a sudden episode of facial muscle weakness with loss of sensation over the affected area that worsens over the next 48 hours. It is associated with discomfort and tenderness over the affected side of the face which may extend over the neck and the head. Bell’s palsy arises due to disruption in the normal functioning of the facial nerve (or the 7th cranial nerve) possibly because of damage or trauma to the facial nerves.
The symptoms of Bell’s palsy depend on the extent of damage to the facial nerve involved. Symptoms are noted over the affected side of the face and may include paralysis, drooping of the corner of the mouth, drooping of the eyelids, dryness of mouth, dryness of eye, twitching, muscle weakness, taste impairment, loss of facial expressions, excessive tearing or lacrimation, facial distortion.
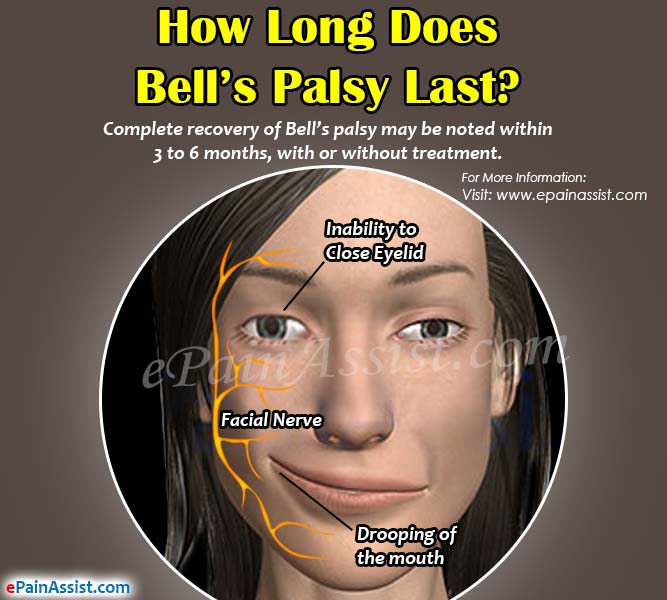
How Long Does Bell’s Palsy Last?
The symptoms of Bell’s palsy usually subside on its own; however, in some cases conventional treatment is required. The prognosis of this condition is generally very good. The extent of recovery and the time required for complete recovery from Bell’s palsy depends on the extent of nerve damage. In most of the cases, the affected individual may notice improvement in symptoms of Bell’s palsy within 2 weeks after initial onset of the symptom. Complete recovery of Bell’s palsy may be noted within 3 to 6 months, with or without treatment. Though in most of the cases, the symptoms disappear after a few months, in some cases the symptoms of Bell’s palsy may linger longer and in certain rare cases, the symptoms may last forever. In other rare cases, reoccurrence of the condition is noted either on the same side of the face or on opposite of the face.
Most of these treatments modalities designed for treating Bell’s palsy includes palliative care and accelerates recovery. These include prescription drugs such as steroids (prednisone), acyclovir, analgesics (acetaminophen, ibuprofen, and aspirin); eye protection; lubricating eye drops; physical therapy; facial massages; acupuncture. Under very rare condition, decompression surgery may be suggested. Cosmetic and reconstructive surgeries may be recommended for management of deformities and for overcoming functional limitations.
What are the Recovery Signs of Bell’s Palsy?
Recovery from Bell’s palsy depends on the extent of nerve damage and it varies from one individual to the other. In most of the cases, recovery begins with reappearance of normal functionality such normalization of taste sensation.
As there is recovery in the affected nerve, there will be improvement in the face as the nerve signals will start communicating with the facial muscles. Some on the facial muscles affected due to Bell’s palsy will recover faster than the others; for example the smile may be still appear lopsided but he or she may regain the ability to close his or her eye. The face will appear more symmetrical when relaxed, as the muscles begin to regain their tonicity. There will be overall improvement in the appearance of the face even though the movement may still be weak. In addition to this, there is improvement in the affected individual’s emotional well-being.
With further strengthening of the facial nerve there are other changes that may take place, which includes; affected eye may appear normal, symmetrical with respect to the unaffected eye and smaller; improvement in drooping of the corner of the mouth, it may seem raised; tightness and stiffness over the affected cheek; improved muscle coordination (synkinesis) and facial expression. As the facial nerve has 5 branches which supply to 5 different areas, each of this area may return back to normal state at different rates.
Also Read:
