The Noonan syndrome is a rare disease of genetic origin characterized by a particular aspect of facial features, congenital heart defects, and short stature. Sometimes there is an intellectual disability (mild) as well as manifested with a delay in language acquisition. (1)
Noonan syndrome is a congenital genetic disorder that occurs in men and women (no gender preference). Earlier this name was used when people talked about the male form of Turner syndrome, but now it is known that they are two very different genetic abnormalities. The most common consequences of this syndrome are heart malformations, small size, learning problems, chest indentation, poor blood clotting, cryptorchidism, and facial deformities. The syndrome is named after Dr. Jackie Noonan. (2)
This syndrome results from a disruption of the intracellular signaling pathway RAS/MAPK and consequently a disruption of the cells of the body and the process of growth of new blood vessels (angiogenesis). In 40 to 50% of cases, Noonan syndrome is due to a mutation of the gene called PTPN11 located on chromosome 12. This gene allows the manufacture of protein tyrosine phosphatase SHP-2, which is present in large quantities in the human body. It plays a role in the regulation of information exchanged between cells and intervenes in many functions of the body.
How Dangerous Is Noonan Syndrome?
Manifestation and severity of Noonan syndrome are highly varied. But in most individuals, the disease prognosis can be effectively managed and the patients can expect a normal life expectancy. The disease can become dangerous in some individuals with cardiovascular complications and the development of malignant tumors or leukemia. (4)
Common cardiac defects include:
- Atrial communication
- Hypertrophic cardiomyopathy
- Interauricular communication
- Pulmonary Stenosis
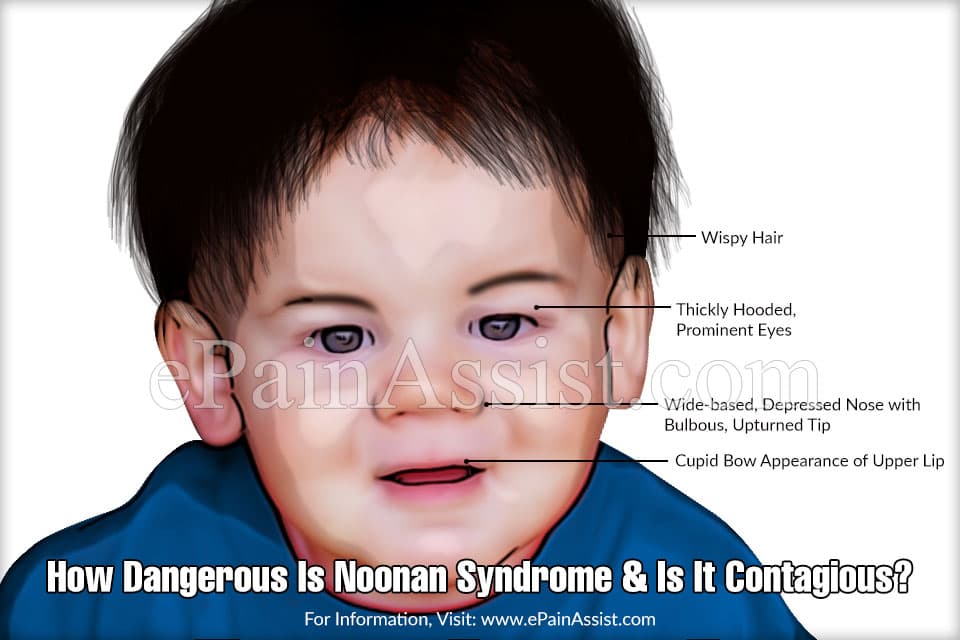
Common facial abnormalities include:
- An abnormal amount of freckles
- Abnormal position and shape of the ears
- A webbed neck
- Big eyes
- Flat nose bridge
- Hypertelorism
- Ptosis
About 1 in 1000 to 1 in 2500 children are born with this syndrome. It is one of the most common genetic syndromes in which a cardiac malformation is a feature. Individuals with Down syndrome also have a higher risk of developing this disorder. It is also true that the severity of the symptoms can be extremely varied in people with Noonan syndrome. Because of this, it is possible that the syndrome remains undetected for long and being discovered only after years by specialized physicians. (4)
Is Noonan Syndrome Contagious?
It is a hereditary disorder affected by a gene mutation. However, the non-hereditary onset of the disease can also be seen (though less abundant) in less than 1% of the children (whole general population). Children whose parents have the disease are at a 50% chance of acquiring the disease in their lifetime. However, the disease is not due to an infection and thus cannot be contagious (cannot be transferred from one patient to another other than from parents to offspring).
Noonan syndrome is not common. Someone is born with this condition in most cases and sometimes develop it after birth through genetic mutation of specific genes. So, there is a multitude of disorders that doctors have to focus on, such as heart disease, pulmonary artery abnormality, and deformities in the face. (3)
The characteristic manifestations of Noonan syndrome are (facial features, heart problems, small size, etc.) Theoretical makes it easy to diagnose. In practice, it is sometimes very difficult to assert the diagnosis as the manifestations are variable and subtle for the non-specialists. Confirmation is possible in almost 50% of cases by a simple blood test. It makes it possible to carry out a genetic test highlighting the mutation of the PTPN11 gene or the K-RAS gene. Nevertheless, in almost half of the cases, please diagnosis cannot be confirmed coma and remains clearly clinical. It is hoped that progress in Genetics will in the near future to confirm the diagnosis in the majority of cases. It must be emphasized that the genetic diagnosis of Noonan syndrome is very complex.
Noonan Syndrome Treatment
Each case is treated differently. A distortion of congenital heart disease can be surgically corrected. The scrotum can be surgically updated. Sometimes growth hormones are prescribed to address slow growth, short stature or abnormalities in growth. Learning disabilities can be accommodated in special education. Due to the diversity of symptoms and the varying severity of the disease among different individuals, there is no definite method of treatment. (5)
- Romano AA, Allanson JE, Dahlgren J, et al. Noonan syndrome: clinical features, diagnosis, and management guidelines. Pediatrics. 2010;126(4):746-759.
- Roberts AE, Allanson JE, Tartaglia M, Gelb BD. Noonan syndrome. The Lancet. 2013;381(9863):333-342.
- Noonan JA. Noonan syndrome. Health Care for People with Intellectual and Developmental Disabilities across the Lifespan: Springer; 2016:827-832.
- Hemmati P, Dearani JA, Daly RC, et al. Early outcomes of cardiac surgery in patients with noonan syndrome. Paper presented at: Seminars in thoracic and cardiovascular surgery2019.
- Kruszka P, Porras AR, Addissie YA, et al. Noonan syndrome in diverse populations. American Journal of Medical Genetics Part A. 2017;173(9):2323-2334.
Also Read:
- Can You Detect Noonan Syndrome Before Birth & Is It More Common In Males Or Females?
- Is Noonan Syndrome Recessive Or Dominant?
- Is Noonan Syndrome A Serious Condition & Can It Be Reversed?
- Lifestyle Changes For Noonan Syndrome
- What Is The Prognosis For Noonan Syndrome?
- What To Eat & Avoid When You Have Noonan Syndrome?
