According to the medical Dictionary, the word ‘ectomy’ means surgically removing a body part or an anatomical structure. The abdomen is the place where the maximum number of varied surgeries could be performed as there are various organs included in the digestive system. Each organ has its own set of surgeries. Hepatectomy is one such surgery performed on the liver to surgically push out tumors from this vital organ. Splenectomy, on the other hand is a surgical process which helps in removing the Spleen either partly or totally.
Hepatectomy – The How’s and Why’s
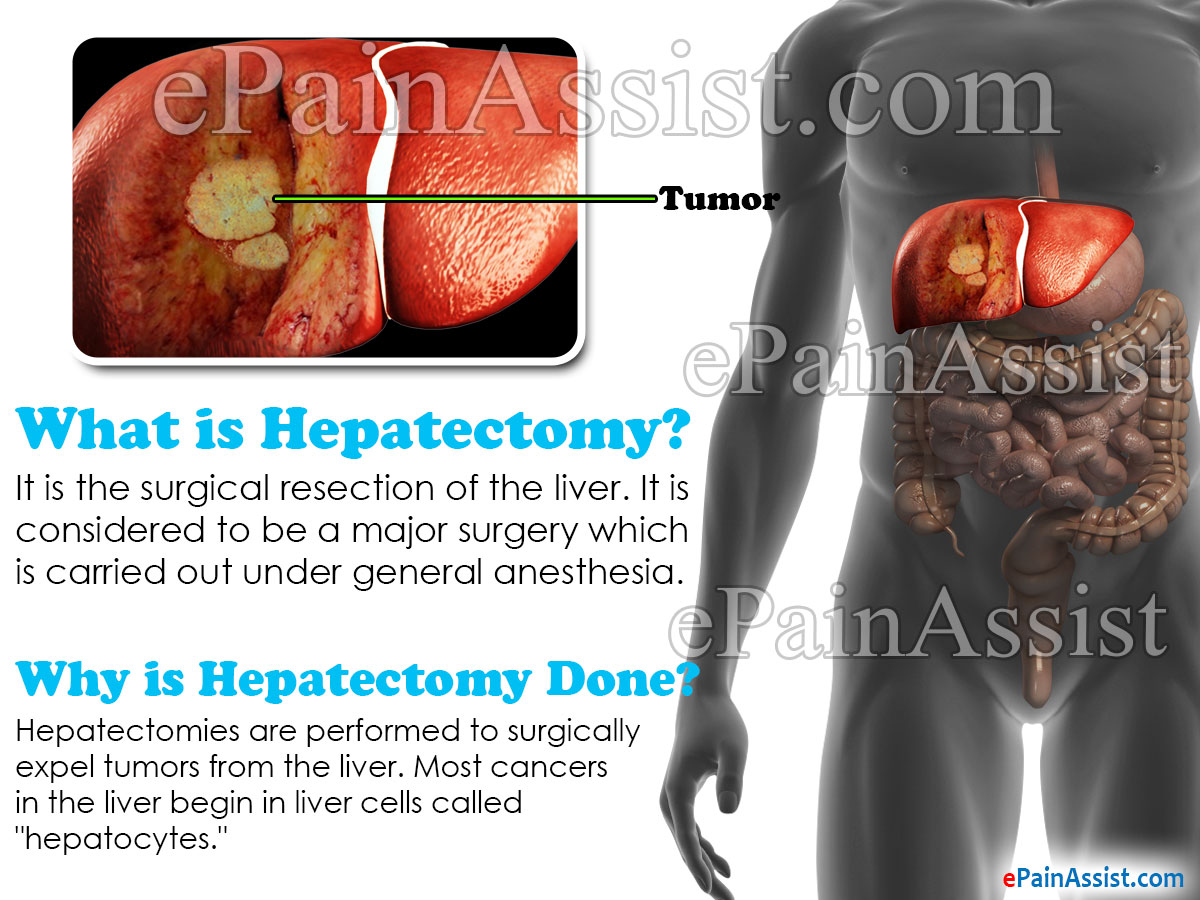
What is Hepatectomy?
Hepatectomy is the surgical resection of the liver. It is considered to be a major surgery which is carried out under general anesthesia.
The period of hepatic surgery started with a left lateral hepatic lobectomy performed effectively in Germany by Langenbuch in the year 1887. From that point forward, hepatectomy has been generally performed for the treatment of different liver illnesses for example, benign tumors and malignant tumors, calculi in the intrahepatic channels, hydatid infection, and abscesses. Liver operations are extremely challenging in light of its interesting anatomic structure and also due to its crucial functions. Regardless of specialized advances and surgeons with high experience of liver resection in different centres, it is still troubled by moderately high rates of postoperative deaths (0.24%-9.7%) and morbidity (4.09%-47.7%).
Why is Hepatectomy Done?
Hepatectomies are performed to surgically expel tumors from the liver. Most cancers in the liver begin in liver cells called “hepatocytes.” The subsequent tumor is called hepatocellular carcinoma or malignant hepatoma. The sort of growth that can be uprooted by hepatectomy is known as a limited resectable (removable) liver disease. This disease is confirmed when there is a confirmation that it has not spread to the close-by lymph nodes or to some other parts of the body. Diagnostic tests additionally demonstrate that the liver is functioning admirably. As a major aspect of a multidisciplinary approach, the methodology can offer a possibility of long haul reduction of problems to patients generally ensured of having a poor result otherwise.
How is Hepatectomy Done?
A hepatectomy is viewed as a noteworthy surgery done under general anesthesia. It all depends as to how big the tumor is and what portion of the liver has to be removed that has been affected by cancer. In Hepatectomy, the operating surgeon may remove a part of the liver or may be the entire liver lobe or the bigger portion of liver, depending on the area affected by the disease. It is seen that the surgeon often leaves a healthy part of liver tissues to carry on the function of the liver. Sometimes the surgeon also informs that the patient can even undergo liver transplantation. In this, the patient’s entire liver is removed from the body and replaced with a healthy liver from the donor. This is only possible if cancer has not affected the other parts of the body. It is very essential to keep the patient under observation before the transplantation is done.
In Hepatectomy, the patient’s abdomen is opened by making an incision up to the bottom of the rib cage. The main task is to free the liver by cutting the fibers over the liver and removing the segments without rupturing the blood vessels. There are two techniques that can be used here:
- First, by making a superficial burn with electric lancet on liver marking the junction affected and then removing it by cutting the section.
- Second technique is to identify the large vessel that need to be removed by operating at the vein level first and clamp the vessels required to be removed.
The Pringle process is typically performed amid a hepatectomy to minimize loss of blood – however this can prompt damage in the liver because of Ischemia or hypoxia/apoxia.
What are the Post Hepatectomy Complications?
Bleeding is the most dreaded complication that can arise and initiate the urgency for immediate reoperation. Biliary fistula is likewise a conceivable complexity, yet one more agreeable to nonsurgical administration. Aspiratory complexities, for example, atelectasis and pleural radiation are typical, and perilous in patients with hidden lung ailments. Contamination is moderately rare.
Liver disappointment represents a noteworthy peril to patients with basic hepatic illness; this is a noteworthy obstacle in the surgical resection of hepatocellular carcinoma in patients with cirrhosis. It is additionally an issue, to a lesser degree, in patients with past hepatectomies (e.g. repeated resections for relapsed colorectal malignancy metastases).
Splenectomy: The How’s and Why’s
What is Splenectomy?
Splenectomy is a surgical technique to remove spleen. Spleen is a small delicate organ situated just under the left rib above the stomach. It is also one of the important organs of the body which functions as a defense system. The spleen contains white blood cells which can destroy bacteria in the body and help to fight infections when the person is sick. The main function of the spleen is to produce red blood cells and store blood that is not needed and also remove the old cells from the circulatory system. Splenectomy is most regularly performed utilizing a minor camcorder and exceptional surgical devices.
Why is Splenectomy Done?
Splenectomy is utilized to treat a wide assortment of illnesses and conditions. The most well-known explanation behind splenectomy is to treat a ruptured spleen, regularly created by stomach injury. Some of the other reasons are as follows:
- Burst spleen: On the off chance that your spleen breaks because of serious injury to the abdomen or in view of an augmented spleen (splenomegaly), the outcome may be life-threatening, internal bleeding. Splenectomy is performed immediately to treat the condition.
- Developed spleen: A spleen may be evacuated to facilitate the side effects of an augmented spleen, which incorporate agony and feelings of bloating/ fullness.
- Blood issue: Blood issue that may be treated with splenectomy incorporate idiopathic polycythemia vera, thrombocytopenic purpura, sickle-cell anemia and thalassemia. Be that as it may, splenectomy is only performed when different medications have failed to lessen the indications of these issues.
- Infection: Chronic infection and along with accumulation of pus secretions in and around the spleen are indications of having a splenectomy done.
- Cancer: Cancer’s like Hodgkin’s lymphoma, non-hodgkin’s lymphoma, hairy-cell leukemia and chronic lymphocytic leukemia needs the splenectomy surgery to be done as a treatment plan.
- Tumor: For the removal of non-cancerous tumors or cysts splenectomy might be required, if they are huge in size or if they are non-removal completely until the spleen is removed.
How is Splenectomy Done?
Splenectomy is done under general anesthesia. There are two approaches to perform a splenectomy: laparoscopic surgery and open surgery.
- Laparoscopic Splenectomy: This is done utilizing an instrument called a laparoscope which contains a light and a camera on the end. The specialist makes three or four little cuts in the guts, and embeds the laparoscope through one of them. This permits the specialist to investigate the stomach territory and find the spleen. Distinctive restorative instruments are gone through alternate openings. One of them is utilized to convey carbon dioxide gas into the stomach zone, which pushes close-by organs off the beaten path and gives specialist more space to work. The specialist separates the spleen from encompassing structures and the blood vessels, and afterward uproots it through the big surgical opening. The surgical openings are shut utilizing join or sutures.
- Open Surgeries: These are done mainly in cases where there is a trauma caused to the spleen or in cases of enlarged spleen.
Complications of Splenectomy
Spleen plays an important role in the body that enables to fight off the bacteria, hence without the spleen you can easily get affected or develop dangerous infections like Pneumonia, Streptococcus, and Meningitis etc. Therefore it is very important that the patient before undergoing the surgery of splenectomy, must be given vaccinations to cover these bacteria just two weeks in advance or after the surgery. Injury to nearby organs is a possible complication.
Precautions Post Hepatectomy and Splenectomy
Hepatectomy: Basic post-hepatectomy inconveniences incorporate fever, drain, bile spillage, liver disappointment, pleural emission, and subphrenic infections. The doctors frequently ask for blood tests and also other tests for specific organs to diagnose further health issues.
Splenectomy: Children, who have their spleen operated, frequently need to take anti-infection agents to keep them from having infections. Grown-ups more often than not needn’t bother with every day anti-infection agents, unless there are chances of complications.
Performing Hepatectomy and Splenectomy helps people keep safe from the dangers like liver and spleen cancer, which not only affect the human body but it may be dangerous for various health disease and sometimes life.
