One of the rare and fatal diseases that are associated with brain infection is Naegleria infection. It is caused by the amoeba named Naegleria Fowleri, also known as the brain-eating amoeba. Predominantly living in the freshwater lakes, rivers and warm waters of the hot springs, it can get into the body through the nose, when the infected water is forcibly aspirated during swimming or other water sports like diving, skiing etc.
About the Amoeba and the Disease:
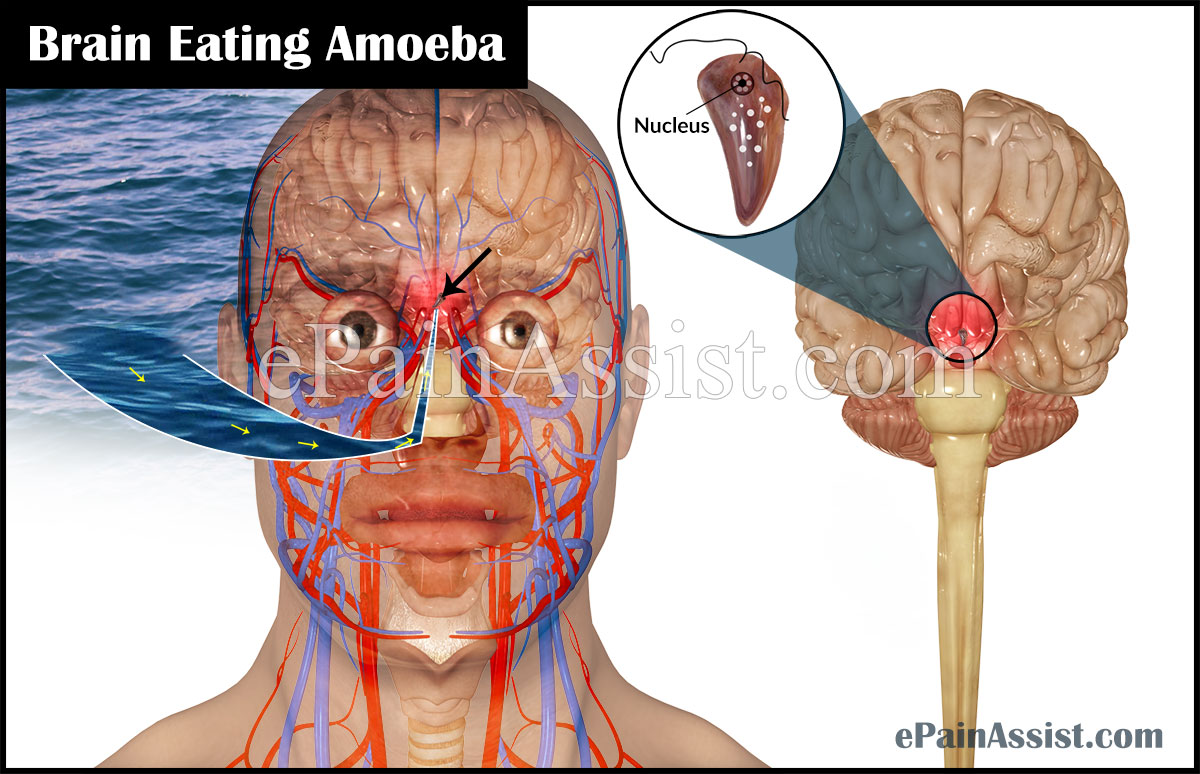
The brain-eating amoeba or Naegleria Fowleri was discovered first in the year 1965. Scientists claim that the evolution of the amoeba has taken place in the United States of America, but it was first identified in Australia. The amoeba gets to the brain through the nasal cavity. However, there is a unique fact associated with this infection that it does not cause infection in every person, who is exposed to it. However, there is no certain justification to this fact.
As the amoeba travels to the brain, it causes PAM or primary amoebic meningoencephalitis. Sometimes, this disease is also called the Naegleriasis, referring to the name of the brain-eating amoeba. Despite being rare, a number of cases of Brain Eating Amoeba or Naegleriasis or PAM are reported in the USA every year. The impacts of the disease are so rapid that it does not give much time to the patient. Hence, despite treatments, in 99% of the cases, the patients die.
When the amoeba gets into the body, rather into the brain, it reproduces by a normal cell division procedure, like any other amoebas. However, since it does not find a suitable atmosphere and favourable condition, it becomes an inactive cyst. When again the conditions are favourable, the cysts transform themselves into trophozoites, which is in fact the feeding form of the amoeba. One study says that the reason why the amoeba eats the brain is that it releases two enzymes that dissolve the brain. According to the reports of the CDC or the Centres for Disease Control and Prevention, only 121 cases of primary amoebic meningoencephalitis or Naegleriasis have been found.
How does the Brain-Eating Amoeba get into the Brain?
The Brain Eating Amoeba or Naegleria Fowleri usually loves warm and moist atmosphere and can survive in temperature as hot as 113 degrees Fahrenheit. It is found in –
- Warm lakes, ponds, and rock pits
- Rivers containing less volumes of water
- Warm, slow-flowing rivers
- Aquariums
- Geothermal water sources
- Thermally polluted water
- Soil and dust, both indoor and outdoor
- Untreated well water, swimming pools and spas
- Mud puddles
- Hot springs.
However, simply coming into contact with this amoeba is not a possible cause of the disease. Only when the water is forced into the nose that it affects the person. It enters the brain by migrating through the olfactory nerves. Along with water sports, religious practices and rituals that engage ablutions usually are causes for this amoeba getting into the body and to the brain. Since the nasal cavity has olfactory nerves that help the brain to detect or sense smell, through these nerves it gets to the brain. The olfactory nerves are connected with the front part of the brain that is known as the frontal lobe.
Symptoms of Brain Eating Amoeba or Naegleriasis:
The basic activity or impact of the Brain Eating Amoeba or Naegleria Fowleri is that as it gets into the brain, it considers the brain as its feeding component. As a result, it causes destruction of brain tissue and consequential brain inflammation. The symptoms that are associated with this disease are: –
- Sudden headache
- Nausea and vomiting
- Fever
- Seizures
- Stiff neck
- A change in the sense of smell or taste
- Sensitivity to light
- Blurred vision
- Loss of balance
- Confusion
- Hallucinations
- Sleepiness
- Coma.
Within as less as two days to 15 days, the amoeba eats the brain and the symptoms are seen to grow rapidly. As a result, the infected person dies within a week or to be specific, within 5.3 days from the time of symptom onset.
Diagnosis of Brain Eating Amoeba or Naegleriasis:
PAM or primary amoebic meningoencephalitis, or the Naegleriasis should be suspected in people, especially children, who are exposed to warm freshwater. Those, who are having symptoms of meningitis, should be suspected of this disease. The symptoms are so non-specific that doctors usually mistake it or suspect the symptoms to be signs of common diseases such as bacterial or viral meningitis. Routine and general tests like blood test and MRI scan do not show anything extremely unusual, though a high level of white blood cell, red blood cells and inflammation in the brain can be seen. Even Gram Staining test cannot detect the amoeba. Hence, a wet mount must be done to test the motility of the amoeba under the microscope.
- Spinal tap (lumbar puncture) – This is the only way through which the presence of the Brain Eating Amoeba or Naegleria Fowleri amoeba can be detected. By inserting a needle, a small amount of fluid is collected from between two vertebrae in the lower back. A biopsy test is run to check for the presence of the amoeba under the microscope.
Treatment for Brain Eating Amoeba or Naegleriasis:
As Brain Eating Amoeba or Naegleriasis is one of the rarest of diseases and also difficult to diagnose, very few people survive the disease, even with treatments. However, the treatment procedures for Brain Eating Amoeba are also very limited, offering only a few medicines and drugs. The reason behind this is that as there are very few numbers of cases diagnosed with this disease, and there is no scope to compare the treatment regimens.
Usually an intravenous drug amphotericin B which is used for treating fungal infections is given to a patient with PAM. However, this drug alone cannot manage, control or treat PAM. It must be supported by some other drugs like miltefosine that the CDC or the Centres for Disease Control and Prevention supplies.
The other drugs that are given with amphotericin B include voriconazole (Vfend), rifampin (Rifadin), or the azithromycin (Zithromax, Zmax). Although there are no scientific studies and reports that prove the efficacy of these drugs.
Risk Factor and Prevention of Brain Eating Amoeba or Naegleriasis:
As about 60% of the cases reported for PAM or primary amoebic meningoencephalitis, or the Naegleriasis are children, who are 13 years of age and younger, they are more at risk of getting infected by Brain Eating Amoeba. Moreover, 80% cases are found in males. The only way to prevent this disease is by avoiding diving, water skiing, swimming underwater, and jumping in warm, still waters. Especially during the late summer, it is ideal for the brain-eating amoeba to get into the body through nostrils and hence, staying away from warm water during this time is suggested. Wearing a nose clip is even more useful. It is always advisable that you use distilled or sterile water to clean nose and not regular tap water.
It is also useful to stay protected and clean. As the brain-eating amoeba does not survive in clean water, cleaning the water supply tanks and treat the swimming pool and wells is very important.
- Cope JR, Ratard RC, Hill VR, Sokol T, Causey JJ, Yoder JS, Mirani G, Mull B, Mukerjee KA, Narayanan J, Doucet M, Qvarnstrom Y, Poole CN, Akingbola OA, Ritter JM, Xiong Z, da Silva AJ, Roellig D, Van Dyke R, Stern H, Xiao L, Beach MJ. The first association of a primary amebic meningoencephalitis death with culturable Naegleria fowleri in tap water from a US treated public drinking water system. Clin Infect Dis. 2015 Mar 15;60(6):e36-42. doi: 10.1093/cid/ciu945. PMID: 25391301.
- Yoder JS, Eddy BA, Visvesvara GS, Capewell L, Beach MJ. The epidemiology of primary amoebic meningoencephalitis in the USA, 1962-2008. Epidemiol Infect. 2010 Nov;138(11):1626-33. doi: 10.1017/S095026881000135X. Epub 2010 May 19. PMID: 20482869
- Marciano-Cabral F, Cabral G. Acanthamoeba spp. as agents of disease in humans. Clin Microbiol Rev. 2003 Jan;16(2):273-307. doi: 10.1128/cmr.16.2.273-307.2003. PMID: 12692099.
- Schuster FL. Cultivation of pathogenic and opportunistic free-living amebas. Clin Microbiol Rev. 2002 Apr;15(2):342-54. doi: 10.1128/cmr.15.2.342-354.2002. PMID: 11932229.
- Siddiqui R, Khan NA. Acanthamoeba is an evolutionary ancestor of macrophages: a myth or reality? Exp Parasitol. 2012 Dec;132(4):545-6. doi: 10.1016/j.exppara.2012.10.006. Epub 2012 Oct 24. PMID: 23103557.
