A pneumothorax is described as an abnormal collection of air in the pleural cavity. Pleural cavity is the space between the lung and the chest wall. It is a small space usually filled with a serous fluid. It is usually not possible for the air to enter this space. But, in case of a trauma or injury to the chest, this space may get filled with air, which results in pneumothorax.
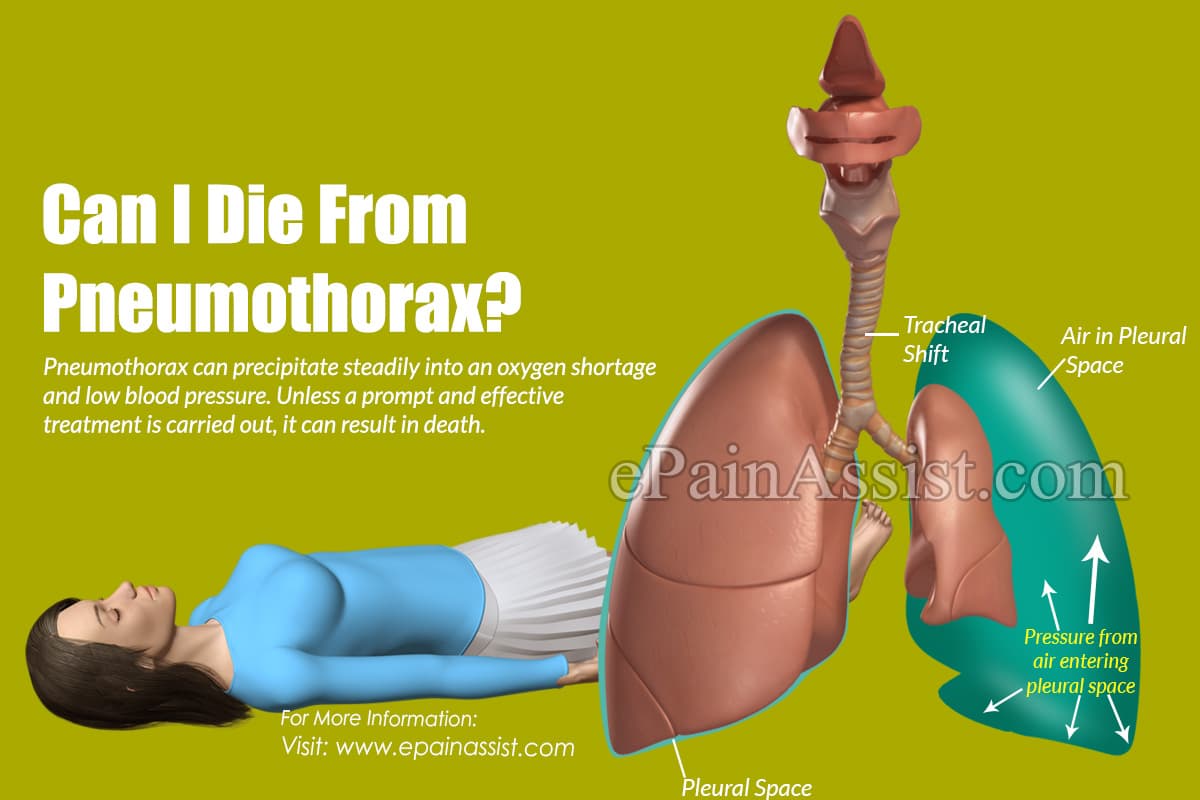
Can I Die From Pneumothorax?
Pneumothorax can precipitate steadily into an oxygen shortage and low blood pressure. Unless a prompt and effective treatment is carried out, it can result in death.
If a pneumothorax is of such a degree that it is responsible for the collapse of one or both lungs, it is a reason to worry. If both lungs collapse, it can be fatal as one will not be able to breathe at all.
There are different classifications for pneumothorax. One of the most widely seen classifies pneumothorax as traumatic and non-traumatic.
Traumatic one, according to the name, is formed as a result of some trauma caused to the chest or to the lungs. An example is a stab wound or a gunshot wound.
The non-traumatic one is again classified into further two types- primary and secondary. As there is no apparent reason for their formation, they are also known as spontaneous pneumothorax. This is why they are called as primary spontaneous pneumothorax (PSP) and secondary spontaneous pneumothorax (SSP).
The primary spontaneous pneumothorax (PSP) is seen without any presence of a lung disease, or without any obvious reason. The secondary spontaneous pneumothorax (SSP) is seen in the presence of an already existing, underlying lung disease, like COPD, asthma etc. Smoking also increases the risk of a pneumothorax.
Pneumothorax may also occur as a complication of a medical procedure, like mechanical ventilation or resuscitation.
Signs and Symptoms Seen In A Pneumothorax
Primary spontaneous Pneumothorax- as mentioned above, there is no underlying lung disease in such cases and the pneumothorax appears spontaneously. This type usually does not cause severe symptoms. A degree of mild breathlessness and chest pain are usually present. Many people suffering from PSP do not even know it, as there are no severe symptoms as such and hence it might be too late by the time they actually consult a physician and start the treatment. These are most commonly seen to be occurring due to changes in atmospheric pressure.
Secondary spontaneous pneumothorax- as there is a significant underlying cause for the SSPs to occur; they tend to be more severe in nature compared to the PSPs. This happens because the unaffected lung fails to compensate for the affected lung. Usually hypoxemia (reduced blood-oxygen) is observed. This can present in the form of cyanosis, which is a blue discoloration of lips and skin. Hypercapnia (increased blood-carbon dioxide) can be seen in some cases, which can even lead to coma. If a person with a history of any significant lung disease suddenly presents with breathlessness, this fact is to be immediately brought to the notice of the physician.
There is another type called as tension pneumothorax. When any of the above types of pneumothorax results in a significant damage to the lungs, thereby causing an impaired respiration and blood circulation, or one of these, it is known as tension pneumothorax. This can be seen in many other clinical conditions like patients with a lung disease, resuscitation, mechanical ventilation etc.
The persons with tension pneumothorax usually present with chest pain, respiration impairment and many times tachycardia (increased heart rate) and tachypnea (increased breathing rate). Low oxygen levels and low blood pressure can be seen. Also, the x-ray may reveal deviation of trachea away from the affected part of the chest.
A small spontaneous pneumothorax, especially if there is no underlying disease, can be left alone to subside on its own. However, a tension pneumothorax especially is to be considered seriously.
Also Read:
- What Is a Collapsed Lung or Pneumothorax: Causes, Symptoms, Signs, Types
- What is Pneumothorax in Infants, Know its Causes, Symptoms, Treatment
- How Long Does It Take To Recover From A Pneumothorax?
- How Do You Fix A Pneumothorax?
- What Are The Different Types Of Pneumothorax?
- What Is Closed Pneumothorax?
- Does Pneumothorax Hurt?
