An Overview of Diabetic Retinopathy!
Diabetic Retinopathy refers to retinal changes seen in patients with diabetes mellitus that is our eye undergoes changes in retina (which forms the screen of the eye where image is formed) due to diabetes.
With increase in the life expectancy of diabetics, the incidence of diabetic retinopathy (DR) has also increased. In Western countries, Diabetic Retinopathy is the leading cause of blindness.
For the past decade, there has been a tremendous increase in the number of cases associated with diabetic retinopathy.
Risk Factors of Diabetic Retinopathy
Risk factors associated with occurrence of Diabetic Retinopathy are:
Duration: Duration of diabetes is the most important determining factor for Diabetic Retinopathy. Roughly 50 percent of patients develop Diabetic Retinopathy after 10 years, 70 percent after 20 years and 90 percent after 30 years of onset of diabetes.
Sex: Incidence of Diabetic Retinopathy is higher in females than males (4:3).
Metabolism: Poor metabolic control is less important than duration, but is nevertheless relevant to the development and progression of Diabetic Retinopathy.
Heredity: Diabetic Retinopathy is transmitted as a recessive trait without sex linkage. The effect of heredity is more on the proliferative retinopathy.
Pregnancy: Pregnancy may accelerate the changes of diabetic retinopathy.
Hypertension: Hypertension, when associated, may also accentuate the changes of diabetic retinopathy.
Others: Other risk factors include smoking, obesity, poor lifestyle, unhealthy routine, zero workout and hyperlipidemia.
Pathogenesis of Diabetic Retinopathy
Essentially, diabetic retinopathy is usually seen as a microangiopathy, which means it affects the small vessels of retina and also affects retinal pre-capillary arterioles, capillaries and venules.
Various vascular changes seen in diabetes mellitus include:
- Thickening of capillary basement membrane.
- Capillary endothelial cell damage.
- Changes in red blood cells.
- Loss of capillary pericytes.
These vascular changes cause microvascular occlusion of retinal vessels that leads to the obstruction of the small vessels of the eye. Obstruction of these vessels cause decreased blood flow in eye, which causes retinal ischemia, which can cause various complications due to lack of blood supply. These complications are as follows: capillary leakage, microaneurysms, hemorrhage, retinal edemas, hard exudates, arteriovenous shunts (intraretinal microvascular abnormalities-IRMA) and neovascularization.
Classification of Diabetic Retinopathy
Diabetic retinopathy has been variously classified by different associations of the world.
Presently the most acceptable and followed classification is as follows:
Non-Proliferative Diabetic Retinopathy (NPDR)
- Mild non-proliferative diabetic retinopathy.
- Moderate non-proliferative diabetic retinopathy.
- Severe non-proliferative diabetic retinopathy.
- Very severe non-proliferative diabetic retinopathy.
Proliferative Diabetic Retinopathy (PDR)
Diabetic Maculopathy
Advanced Diabetic Eye Disease (ADED)
Non-Proliferative Diabetic Retinopathy (NPDR)
Ophthalmoscope is a device that is used to look at retina through an ophthalmoscope. The following changes and features of Non-Proliferative Diabetic Retinopathy can be seen:
- Microaneurysms in the macular area of eye are the earliest detectable lesion in case of diabetic retinopathy.
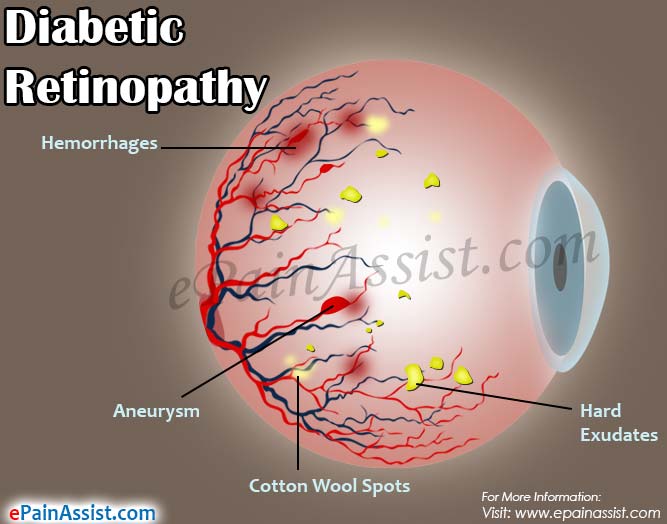
- Retinal hemorrhages, both deep (dot and blot hemorrhages) and superficial hemorrhages (flame-shaped) are seen in diabetic retinopathy.
- Hard exudates, yellowish white and waxy looking patches are arranged in clumps or in circinate pattern can be seen. These are commonly seen and present in the macular area.
- Retinal edema characterized by retinal wall thickening is present in diabetic retinopathy.
- Cotton wool spots are also seen on retina.
- Venous abnormalities like beading, looping and dilatation are commonly present in case of diabetic retinopathy.
- Intraretinal microvascular abnormalities (IRMA) is a common terminology and seen commonly in diabetic retinopathy.
- Dark-blot hemorrhages representing hemorrhagic retinal infarcts (area of retina with lack of blood supply) are seen in eye of the patient with diabetic retinopathy.
Non-Proliferative Diabetic Retinopathy has been further classified on the basis of severity as follows:
Mild Non-Proliferative Diabetic Retinopathy:
- At least one microaneurysm or intraretinal hemorrhage is present.
- Hard/soft exudates may or may not be present.
Moderate Non-Proliferative Diabetic Retinopathy:
- Moderate microaneurysms/intraretinal hemorrhage are present.
- Early mild vascular abnormalities can also be present.
- Hard/soft exudates may or may not be present.
Severe Non-Proliferative Diabetic Retinopathy:
- Full eye of the patient can show severe microaneurysms/intraretinal hemorrhages.
- Half the eye might be filled with venous blood.
- Some intraretinal aneurysms may be present.
Very Severe Non-Proliferative Diabetic Retinopathy:
- Severe microaneurysms/ intraretinal hemorrhages may be seen.
- Venous bleeding can also be seen.
- Some intraretinal aneurysms may be present.
Proliferative Diabetic Retinopathy (PDR)
- Proliferative diabetic retinopathy develops in more than 50 percent of cases after about 25 years of the onset of diabetes. Therefore, it is more common in patients with juvenile onset diabetes or Diabetes Mellitus type 1 or congenital diabetes.
- The hallmark of Proliferative Diabetic Retinopathy is that there is occurrence of neovascularization (formation of new vessels) over the changes of very severe non-proliferative diabetic retinopathy.
- Proliferative diabetic retinopathy is characterized by proliferation of new vessels from the capillaries, in the form of neovascularization at the optic disc (NVD) and/or elsewhere in the fundus of the eye.
- Proliferative diabetic retinopathy is usually along the course of the major temporal retinal vessels. These new vessels may proliferate in retina or spread further.
- Later on condensation of connective tissue around the new vessels results in formation of fibro vascular retinal membrane.
- Vitreous detachment and vitreous hemorrhage may occur in this stage.
On the basis of high risk characteristics (HRCs) described by diabetic retinopathy study (DRS) group, the Proliferative Diabetic Retinopathy can be further classified as below:-
- Proliferative Diabetic Retinopathy (PDR) without High Risk Characters (Early Proliferative Diabetic Retinopathy).
- Proliferative Diabetic Retinopathy (PDR) with High Risks Characters (Advanced Proliferative Diabetic Retinopathy).
Diabetic Maculopathy
Changes in macular region need special mention, due to their effect on vision. These changes may be associated with Non-Proliferative Diabetic Retinopathy (NPDR) or Proliferative Diabetic Retinopathy (PDR). The diabetic edema occurs due to increased permeability of the retinal capillaries and is termed as clinically significant macular edema (CSME) if one of the following three criteria is present on slit-lamp examination with 90D lens:
- Thickening of the retina at fovea of eye.
- Hard exudates are present in retina associated with adjacent retinal thickening.
- Development of a zone of retinal thickening and increase in size.
Classification of Diabetic Maculopathy
Clinically, diabetic maculopathy can be classified into four types:
- Focal Exudative Maculopathy- It is characterized by the following: Microaneurysms, hemorrhages, macular edema and hard exudates, which are usually arranged in a circinate pattern. Fluorescent angiography reveals focal leakage with adequate macular perfusion.
- Diffuse Exudative Maculopathy- It is characterized by diffuse retinal edema, thickening throughout the posterior part of retina, few hard exudates are also present and fluorescent angiography reveals diffuse leakage at the posterior part of retina.
- Ischemic Maculopathy- It occurs due to microvascular blockage. Clinically it is characterized by marked visual loss with microaneurysms, hemorrhages, mild or no macular edema and a few hard exudates are present. Fluorescent angiography shows that pre-capillary arterioles are blocked.
- Mixed Maculopathy- In it combined features of ischemic and exudative maculopathy are present which includes: Marked visual loss with microaneurysms, hemorrhages, mild or no macular edema, a few hard exudates are present, diffuse retinal edema and thickening throughout the posterior part of retina. Fluorescent angiography shows that pre-capillary arterioles are blocked and diffuse leakage at the posterior part of retina is present.
Advanced Diabetic Eye Disease
It is the end result of uncontrolled proliferative diabetic retinopathy. It is marked by complications such as:
- Persistent vitreous hemorrhage.
- Tractional retinal detachment and
- Neovascular glaucoma.
Investigations to Diagnose Diabetic Retinopathy
These include the following tests:
- Urine examination.
- Blood sugar estimation.
- Fundus fluorescent angiography should be carried out to elucidate areas of neovascularization, leakage and capillary non-perfusion.
Management of Diabetic Retinopathy
Screening for Diabetic Retinopathy
It is done to prevent visual loss or blindness occurring from diabetic retinopathy. A periodic follow-up is very important for a timely intervention. The recommendations for periodic fundus examination are as follows:
- Every year, till there is no diabetic retinopathy or there is mild Non-Proliferative Diabetic Retinopathy.
- Every 6 months, in moderate Non-Proliferative Diabetic Retinopathy.
- Every 3 months, in severe Non-Proliferative Diabetic Retinopathy.
- Every 2 months, in Proliferative Diabetic Retinopathy with no high risk characteristic.
Medical Treatment for Diabetic Retinopathy
Besides laser and surgery to the eyes (as indicated and described below), the medical treatment also plays an essential role. Medical treatment for diabetic retinopathy can be discussed as follows:
Control of systemic risk factors is known to influence the occurrence, progression and effect of laser treatment on Diabetic Retinopathy. The systemic risk factors which need attention are as follows:-
- Strict metabolic control of blood sugar.
- Lipid reduction.
- Control of associated anemia.
- Control of associated hypoproteinemia.
Role Of Pharmacological Modulation
Pharmacological inhibition of certain biochemical pathways involved in the pathogenesis of retinal changes in diabetes is being evaluated and this includes:
- Protein Kinase C (PKC) inhibitors.
- Vascular endothelial growth factors (VEGF) inhibitors.
- Aldose reductase and ACE inhibitors.
- Antioxidants, such as vitamin E.
Role of intravitreal steroids in reducing diabetic macular edema is also being stressed recently by following modes of administration:
- Fluocinolone acetonide intravitreal implant.
- Intravitreal injection of triamcinolone (2 to 4 mg).
Photocoagulation Therapy for Diabetic Retinopathy
It remains the mainstay in the treatment of diabetic retinopathy and maculopathy.
Either argon or diode laser can be used. The protocol of laser application is different for macula and rest of the retina as follows: –
Macular Photocoagulation:
Macula is treated by laser only if there is clinically significant macular edema (CSME).
Laser treatment is contraindicated in ischemic diabetic maculopathy Macular photo-coagulation should be considered first i.e., before Pan Retinal Photo Coagulation since the latter may worsen macular edema.
Macular photocoagulation includes two techniques:-
- Focal treatment with argon laser is carried out for all lesions that include microaneurysms, intraretinal aneurysms or short capillary segments.
- Grid treatment. Grid pattern laser burns are applied in the macular area for diffuse diabetic macular edema.
Pan Retinal Photocoagulation (PRP) or Scatter Laser:
It consists of 1200-1600 spots, each 500 μm in size and 0.1 sec. duration. Laser burns are applied 2-3 disc areas from the centre of the macula extending peripherally to the equator of eye. In Pan retinal photo coagulation outer quadrant of retina is first coagulated. Pan retinal photocoagulation produces destruction of ischemic retina. Indications for Pan retinal photo coagulation are:
- Proliferative Diabetic Retinopathy with high risk complications.
- Neovascularization of iris (NVI).
- Severe NPDR associated with: Poor compliance for follow up, before cataract surgery/YAG capsulotomy, renal failure, one-eyed patient and pregnancy.
Surgical Treatment for Diabetic Retinopathy
- It is required in advanced cases of Proliferative Diabetic Retinopathy.
- Pars plana vitrectomy surgery is indicated for dense persistent vitreous hemorrhage, fractional retinal detachment, and epiretinal membranes.
- Associated retinal detachment also needs surgical repair.
Foods to Avoid in Diabetic Retinopathy
Patients are recommended to maintain a proper diet and keep a check on their blood sugar levels. This includes avoidance of high fatty diet and zero intake of food products with high carbohydrates and fat content. Hence the patient should avoid the following food items: junk foods like pizza, burgers etc., ice creams, sugar, aerated drinks, potatoes, chips and other munching snacks, oily food items, high cholesterol containing food items and alcohol.
Recommendations in Diabetic Retinopathy
On the other hand, patient is recommended to increase the intake of various food items which include:
- High fiber diet like salad
- Use low cholesterol oil for cooking
- More usage of green leafy veggies.
- Exercising daily
- Walk after every meal
- Regular checkups are recommended.
Also Read:
