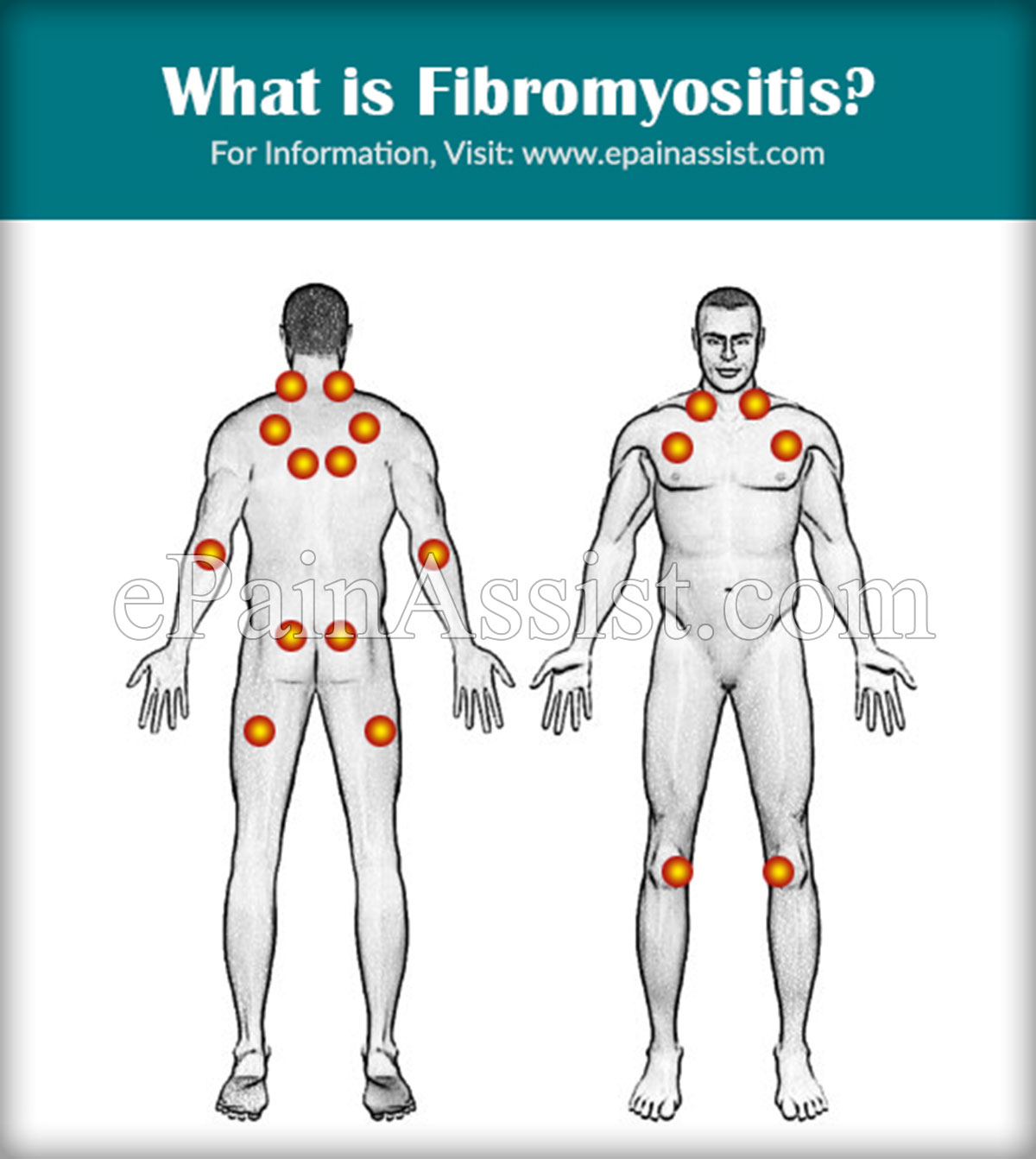
Fibromyositis, a misnomer of fibromyalgia or fibrositis, is a medical condition that is characterized by chronic inflammation and widespread pain in the muscles, muscle sheaths with an overgrowth of the connective tissue. While fibromyositis is a syndrome or a condition, fibromyalgia does not involve inflammation. The International Classification of Diseases (ICD-10) lists fibromyositis as a diagnosable disease under “Diseases of the musculoskeletal system and connective tissue” under the code M79-7, and states that fibromyositis must be classified as a functional somatic syndrome instead of a mental disorder. The condition causes the patients to experience pain in the locations of the body where only a slight amount of pressure can cause pain; such as the neck, shoulders, lower back, elbows, hips, shins and knees. The fibromyositis pain resembles the pain of other diseases such as rheumatoid arthritis; however, the patients suffering from fibromyositis do not exhibit any of the other features of rheumatoid arthritis such as swelling or deformity of joints. While fibromyositis can last for a long period of time, it does not cause any tissue damage; neither does it result in death.
Causes of Fibromyositis
The cause of fibromyositis is unknown; however, possible causes might be genetic, derived from infections or influenced from the environment. Some of the possible causes are listed below:
- Stress related disorders.
- Poor lifestyle.
- Obesity.
- Lack of physical activity.
- Psychological trauma.
- An imbalance in the brain chemicals.
Until recently, this was thought to be a psychological disorder. Research continues to find out the cause of fibromyositis.
Signs and Symptoms of Fibromyositis
The individual suffering from Fibromyositis feels tired to a degree that his or her daily activities are hampered. The most common symptoms of fibromyositis are listed below:
- Chronic headache, fatigue, dizziness.
- Sleeping difficulties.
- Cognitive problems.
- Memory problems.
- Depression, anxiety and post-traumatic stress disorder.
- Sensitivity to sensory stimuli such as noise, odor, and light.
- Sudden, painful muscle spasms that worsen with activity or exercise.
- Stiffness and weakness.
- Painful muscle areas.
- Nodules or localized areas that are tender to touch.
- Sometimes problems in urinating and irritable bowel syndrome.
Epidemiology of Fibromyositis
Fibromyositis patients are a very heterogeneous population, and it is likely that different subgroups will display different levels of disability. The ‘Multidimensional Pain Inventory’ (Kerns et al. 1985) has been used to classify fibromyositis patients into three groups: Dysfunctional, Interpersonally distressed or Adaptive copers. The dysfunctional and interpersonally distressed groups have higher levels of disability. Observed physical function (cervical spine mobility) is positively correlated with patient’s perceived disability in the adaptive copers group, but not in the other two groups (Turk et al. 1996).
Fibromyositis is estimated to affect 2 to 8% of the total population. It usually occurs in adults between the ages 30 and 60, and more frequently in women than in men (ratio of 5:1). Sometimes, it may not be diagnosed in up to 75% of the affected people. Rarely, 1 out of 6 people with fibromyositis are under 18.
Risk Factors for Fibromyositis
The following are the risk factors which can either contribute or increase the intensity of the disorder:
- Stress.
- Sleep disturbances.
- Muscle injury.
- Exposure to dampness and cold.
- Viral infections.
- Poor nutrition.
- Fatigue.
- Overwork.
Diagnosis of Fibromyositis
There is no particular diagnosis for fibromyositis. In order for a patient to be diagnosed with this condition, he or she must have a history of 3 or more months of widespread pain and must have pain or tenderness in a minimum of 11 of 18 tender points.
The problems that physicians encounter in diagnosing the chronic pain in patients are largely related to four issues:
- Pain is a purely subjective perception, which is usually interpreted in an emotional context.
- Chronic pain is not fully understood with regards to the classical model of disease, which equates the pathogenesis with tissue damage or dysfunction.
- Many people who are not sick also have persistent pain, but are not disabled.
- Apparent impairment due to pain is an outcome of a complex interplay between education, past experiences, income level, motivation, psychological distress, fatigue, personal value systems, work related self-esteem, ethno-cultural background, and the availability of financial compensation.
Treatment for Fibromyositis
- General Treatment for Fibromyositis: The general treatment for fibromyositis includes the following-
- Lab blood studies to measure inflammation and tests to rule out rheumatoid arthritis or polymyalgia. There is no such specific test for fibromyositis.
- Heat relieves pain. Hot showers, electric lamps, heating pads may help relieve the pain.
- Gently massage the painful areas.
- Eliminating stress in daily life.
- Learning relaxation techniques.
- Biofeedback is helpful for some patients who use it to relax contracted muscles.
- Eating a healthy diet.
- Physical therapy or chiropractics therapy can help in reducing the fibromyositis pain.
- Medications for Fibromyositis:
- For minor discomfort, over-the-counter medications such as aspirin, acetaminophen, or ibuprofen can be used.
- Cortisone injections into “trigger areas” or non-steroidal anti-inflammatory drugs can be used to reduce the Fibromyositis pain.
- Antidepressants, anti-seizure medicines or opioids in low dosages and for shorter periods can be used under prescription.
- Emotional support and education needs to be provided for patients suffering from fibromyositis as due to the tremendous pain they often feel depressed.
Prognosis of Fibromyositis
The pain of fibromyositis is pervasive and persistent. Most of the people with this condition complain that their symptoms do not improve over time. However, the disorder doesn’t get worse and isn’t fatal. The symptoms better over time for adults and it is reported that children recover after 2 to 3 years, if at all they are affected. Reports suggest that there is spontaneous recovery in some people. Others may have flare-ups and remission indefinitely. The disease is uncomfortable, but not life-threatening. The symptoms can be relieved with treatment.
Prevention of Fibromyositis
Continuous activity is required to avoid any kind of pains, stretching may be helpful. General conditioning exercises are also helpful for Fibromyositis.
Lifestyle Modifications for Fibromyositis
Chronic pain perpetually produces an existential crisis as it changes a person’s perception of “self”. This generally results in varying degrees of anxiety, depression and anger with loss of self-esteem, reduced self-efficacy and functional decline. Employment helps in fulfilling one’s obligations to family and society, maintaining self-esteem and in achieving financial security.
Patients with Fibromyositis should be encouraged to continue with productive employment based on two major strategies, namely (1) optimal management of fibromyositis symptomatology, and (2) a willingness to intercede in issues relating to job and workplace modifications (Liedberg and Henriksson 2002). The optimal management of fibromyositis symptomatology needs to be based on a multimodal approach to management (Bennett 2002).
This also involves attention to the following issues: Fibromyositis patient education, pain, fatigue, sleep, psychological distress, deconditioning and attention to commonly associated disorders (e.g. irritable bowel syndrome). A readiness on the part of physicians to act in an administrative role in making recommendations to employers is an essential component of minimizing disability in fibromyositis patients. In majority of cases, a careful evaluation of work place by an occupational therapist is an invaluable tool for making appropriate ergonomic changes. Health care provider’s unwillingness to act on a patient’s behalf often results in a downhill spiral of increasing work place stress, depressive symptoms, and sense of victimization by people with fibromyositis. Thus, the prevention of disability in people with fibromyositis ultimately depends on both the expert management of their symptoms, and a willingness to act pro-actively on their behalf in securing appropriate work place modifications. If a patients’ work efficiency and productivity declines progressively over the years of continued observation, then the physician should recommend the patient seek disability and be prepared to help administratively in this process.
Conclusion
Fibromyositis, although not a life-threatening condition, is a painful condition to go through. The management of the condition must be holistic in nature with simple home remedies, medications, and lifestyle modifications. Since the pain is debilitating at times, many times the patients need emotional support or counseling services as well. With a conservative approach the condition can be managed and the patient can live an active and productive life.
Also Read:
