Causes of Hip Joint Osteoarthritis
Hip Joint Inflammation– Osteoarthritis of hip joint is a progressive inflammatory joint disease, which causes degeneration of synovial membrane and joint cartilages.1 Osteoarthritis is a common joint disease which affects 27 million Americans. Most common joints affected are hip, knee, hands, and facet joints. Symptoms such as pain and joint swelling may or may not respond to anti-inflammatory medications. Joint swelling is caused by bony growth of joint edges and synovitis resulting in inflammatory water retention of synovial membrane.
Genetic Disorder– Osteoarthritis is thought to be caused by inherited genetic disorder. A lab study has not shown any solid evidence of chromosomal or genetic abnormalities.
Symptoms and Signs of Hip Joint Osteoarthritis
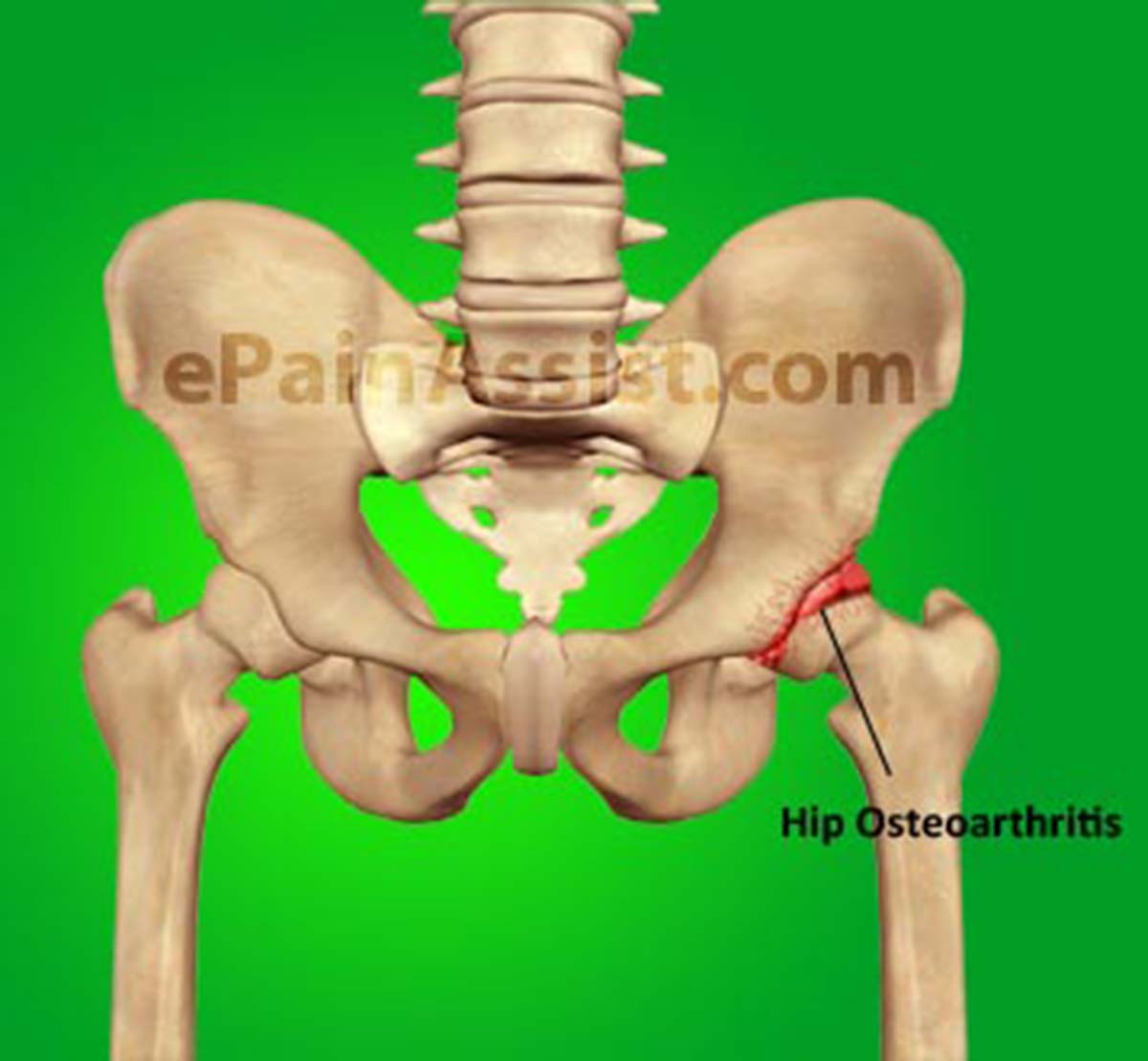
Symptoms of Hip Joint Osteoarthritis
- Sex– Hip Joint Osteoarthritis is common among females than males.1
- Age– Hip Joint Osteoarthritis is most common over age of 40 years.
- Pain– at rest and during activities.
- Joint Stiffness– during active hip joint movement.
- Range of Joint Movements– limited.
- Pain during Change of Position– severe pain observed during change of position like sitting to standing position or getting in and out of car.
- Referred Pain– Pain often felt in buttocks, knee and ankle.
Signs of Hip Joint Osteoarthritis
- Hip Joint:
- Swelling of the joint, or affected joint seems to be larger than normal joint or opposite joint.
- Tenderness on deep pressure over joint.
- Loss of maximum range of joint motion.1
- Stiffness observed during passive hip joint movement.1
- Skin temperature over joint- warmer.
- Muscles of the Affected Limb– loss of muscle mass or muscle atrophy observed.
- Grating or Crackling Sound– heard in the affected limb.
Diagnosis and Investigations for Hip Joint Osteoarthritis
Diagnostic Clinical Findings for Hip Joint Osteoarthritis
- Hip Joint Pain.
- Hip Joint Tenderness.
- Hip Joint Deformity or Swelling.
- Hip Joint Stiffness.
- Hip Joint Crackling or Grating Sound.
Investigation for Hip Joint Osteoarthritis
- X-Ray– Findings are as follows
- Irregular broken cartilage linings.
- Joint space is narrowed.
- Bone spurs around edges of joint.
- MRI– Findings are as follows
- Uneven cartilage linings and surface observed in 3 dimensions.
- Joint space is narrowed.
- Bone spurs around edges of the joint.
- Synovial membrane thickening are seen.
- Blood Examination– Osteoarthritis is not diagnosed with any specific blood test. Most of the blood test performed are to rule out other causes of osteoarthritis like rheumatoid arthritis, psoriatic arthritis, septic arthritis and Wegener’s granuloma.
- ESR (Erythrocyte Sedimentation Rate)– ESR is increased in Osteoarthritis. ESR blood test is used to monitor the progress of hip joint osteoarthritis and prognosis of the hip joint disease. Erythrocyte sedimentation rate (ESR) is increased during active inflammation. ESR is non-specific test. ESR is also elevated in rheumatoid hip joint disease, septic hip joint disease and psoriatic hip joint arthritis.
Blood Test to Rule Out Other Causes of Inflammatory Hip Joint Diseases
- Rheumatoid Factors (RF)– RF is a protein molecule known as antibodies. Blood examination of 70% to 90% of patients suffering with rheumatoid arthritis show presence of RF. RF may also present in patients suffering with autoimmune disorders and no joint pain. Symptoms of Rheumatoid arthritis are less severe in patients with absence of RF antibodies.
- Citrulline Modified Proteins (anti-CCP)– Specific antibodies produced in rheumatoid disease prior to symptoms and during symptoms binds to citrulline. The test is specific and diagnosed even cases which do not show positive rheumatoid factors. Anti-CCP predict severity of Rheumatoid disease (RD) and also subclinical RD.
- ANA Blood Test– ANA is a non specific antibody test, which is often positive as in all autoimmune disease.
- HLA-B27 Genetic Marker– Test is positive in inflammatory joint diseases like Psoriatic hip joint disease, Ankylosing Spondylitis and Reiter’s syndrome.
- Antineutrophil Cytoplasmic Antibodies (ANCA)– ANCA is abnormal antibodies seen in patient with history of hip joint pain caused by Wegener’s granuloma. Blood examination for ANCA level is performed to rule out Wegener’s granuloma as a cause of hip joint pain.
- Serum Cytokines– Cytokins and related protein factors are elevated in early stages of rheumatoid disease. Cytokin factors are used as a marker to diagnose early stage of rheumatoid arthritis.
Joint Fluid Analysis (Arthrocentesis):
- Rule out Gout-Uric acid crystals are observed in gout.
- Septic Arthritis-Bacterial cells, red blood cells and pus cells are observed in septic arthritis.
Treatment for Hip Joint Osteoarthritis
Conservative Treatment for Hip Joint Osteoarthritis
- Rest.
- Exercise, Swimming, and Yoga Therapy.
- Heat or Cold Therapy.
- Cane, Walker or Wheelchair for Ambulation.
- Weight Loss.
Specific Treatment for Hip Joint Osteoarthritis
- Chronic Pain- Due to Hip Joint Osteoarthritis is treated with one of the following medications:
- NSAIDs.
- Opioids– If NSAIDs are ineffective in relieving pain.
- Antidepressant Analgesics– Treats neuropathic pain and pain not responding to opioids.
- Antiepileptic Analgesics– Treats neuropathic pain and pain not responding to opioids.
- Hip Joint Inflammation- Caused by osteoarthritis is treated with following anti-inflammatory medications-
- NSAIDs- Ibuprofen, Naproxen, Daypro, or Celebrex.
- Corticosteroids.
- Muscle Spasm– Muscle relaxants such as Baclofen, Flexeril, Skelaxin, or Robaxin are prescribed with anti-inflammatory medications.
- Physical Therapy- For Hip Joint Osteoarthritis is suggested for:
- Pain.
- Muscle Spasm.
- Joint Stiffness.
- Joint Instability.
- Abnormal Gait.
- Interventional Therapy– Corticosteroid injection of the hip joint
- Surgery For Hip Joint Osteoarthritis:
- Hip Joint Replacement– Head of the femur, neck of the femur and acetabulum is replaced with artificial metal prosthesis.
- Partial Hip Joint Replacement– Head of the femur or neck of the femur or acetabulum is replaced with artificial metal prosthesis.
- Hip Resurfacing– The surface of the head of the femur and acetabulum is replaced and covered with cobalt metal cap.
