Rheumatoid arthritis is an autoimmune inflammatory disease that affects synovial membrane of major and minor joints. Rheumatoid arthritis is not a genetic or abnormal chromosomal disorder. The autoimmune dysfunction may be triggered after viral, bacterial or parasite infection in few individuals carrying certain gene types like PTPN22 and PAD14. Several epidemiological studies have indicated links between herpes virus infection and rheumatoid arthritis.
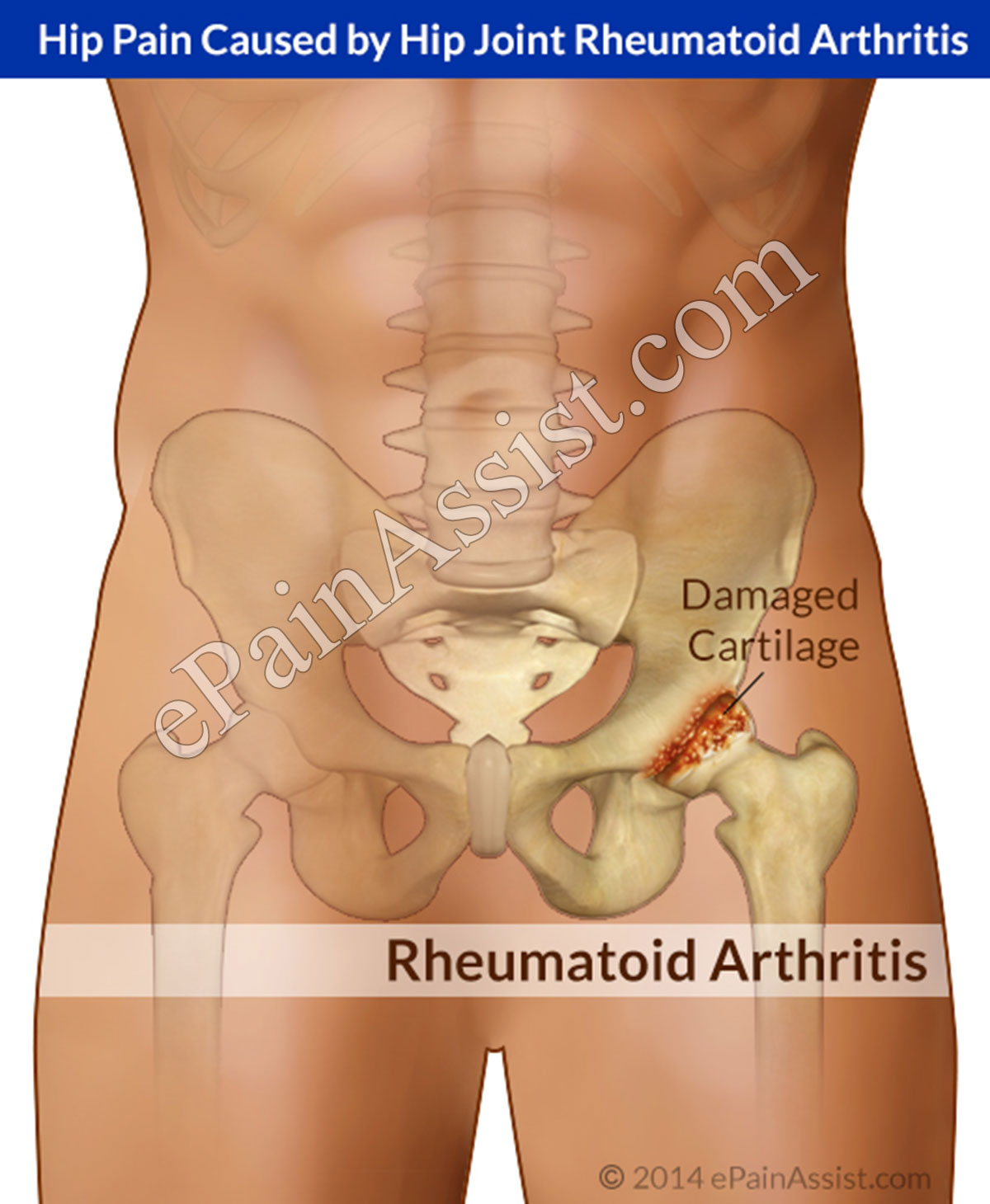
Causes of Hip Joint Rheumatoid Arthritis
- Hip Joint Inflammation– Inflammation of synovium causes swelling or edema of the synovial membrane, hypertrophy of synovial fibrous tissue, and excess secretion of synovial fluid within the joint.
- Cartilage Damage– Later stage continuation of inflammation causes destruction of articular cartilage within the joint.
- Vitamin D Deficiency– Several studies has suggested link between vitamin D deficiency and occurrence of rheumatoid arthritis.
- Smoking– Rheumatoid arthritis is more common among smokers than non-smokers. Rheumatoid arthritis is 3 times more common in patients with history of smoking than non-smoking.1
Symptoms and Signs of Hip Joint Rheumatoid Arthritis
Symptoms of Hip Joint Rheumatoid Arthritis
- Sex– More common in female than male (F/M: 2/1)
- Age– Middle age
- Pain– Hip joint pain is observed at rest and with activities, pain is at time extremely severe lasting few hours and followed by less severe pain
- Morning Aches– Joint pain is worse in the morning at rest and with activities,
- Swollen Hip Joint
- Weight Loss- History of weight loss
- Fatigue– History of fatigue and tiredness
- Fever– History of on and off fever
Signs of Hip Joint Rheumatoid Arthritis
- Tender hip joint on examination.
- Warm skin over hip joint.
- Swollen Hip Joints.
- Hip Joint Stiffness mostly observed in the morning.
- Nodules known as rheumatoid nodule observed under skin mostly over arms.
- Smaller joints like fingers and hands are affected during earlier stages.
- Associated Joint Deformity observed in hand and feet.
Diagnosis and Investigations for Hip Joint Rheumatoid Arthritis
Diagnostic Clinical Findings for Hip Joint Rheumatoid Arthritis
- Hip Joint Pain.
- Joint Deformity– Seen in hand, finger and feet.
- Hip Joint Tenderness– Deep pressure over the hip joint either on lateral side or over the groin triggers severe pain and joint stiffness.
- Hip Joint Swelling– Observed with fluctuating soft consistency secondary to synovial fluid accumulations in joint.
- Hip Joint Stiffness– Mostly observed early morning and results in difficulties getting out of the bed.
- Hip Joint Dislocation– Occasionally few cases may be associated with hip joint dislocation.
Investigations for Hip Joint Rheumatoid Arthritis
- X-Ray– Findings are as follows-
- Joint effusion and joint space may be filled with synovial fluid.
- Joint space is narrowed.
- Dislocated joints in hands and feet causing joint deformity.
- MRI– Findings are as follows-
- Uneven cartilage linings and surface observed in 3 dimensions.
- Joint space filled with synovial fluid.
- Joint subluxation or dislocation in hand and feet, rarely hip joint dislocation is associated with advanced rheumatoid arthritis.
- Bone spurs around edges of the joint.
- Synovial membrane thickening are seen
Blood Examination
Specific Blood Examination to Diagnose RF
- Rheumatoid Factors (RF)– RF is a protein molecule known as antibodies. Blood examination of 70% to 90% of patients suffering with rheumatoid arthritis show presence of RF. RF may also present in patients suffering with autoimmune disorders and no joint pain. Symptoms of Rheumatoid arthritis are less severe in patients with absence of RF antibodies.
- Citrulline Modified Proteins (Anti-CCP) – specific antibodies produced in rheumatoid disease prior to symptoms and during symptoms binds to citrulline. The test is specific and diagnoses even cases which do not show positive rheumatoid factors. Anti-CCP predicts severity of rheumatoid disease (RD) and also subclinical RD.
- Serum Cytokines– Cytokins and related protein factors are elevated in early stages of rheumatoid disease. Cytokine factors are used as a marker to diagnose early stage of rheumatoid arthritis.
- ESR-ESR is increased in Rheumatoid Disease. ESR and Anti-CCP test are used to monitor the disease and prognosis. Erythrocyte sedimentation rate (ESR) is increased during active inflammation. ESR is non-specific test and used to diagnose inflammatory joint disease and prognosis of the disease. ESR is elevated in rheumatoid hip joint disease, osteoarthritis of hip joint and psoriatic hip joint arthritis.
Non-Specific Blood Test to Rule Out Other Inflammatory Hip Joint Diseases
- ANA blood test– ANA is a non-specific antibody test, which is often positive as in all autoimmune disease.
- HLA-B27 Genetic Marker– Test is positive in inflammatory joint diseases like Psoriatic hip joint disease, Ankylosing Spondylitis and Reiter’s syndrome.
- Antineutrophil Cytoplasmic Antibodies (ANCA) – ANCA is an abnormal antibody seen in-patient with history of hip joint pain caused by Wegener’s granuloma. Blood examination for ANCA level is performed to rule out Wegener’s granuloma as a cause of hip joint pain.
Joint Fluid Analysis (Arthrocentesis)-
- Rule-out Gout- uric acid crystals are observed in gout,
- Septic Arthritis- bacterial cells, red blood cells and pus cells are observed in septic arthritis.
Treatment for Hip Joint Rheumatoid Arthritis
Conservative Treatment for Hip Joint Rheumatoid Arthritis
- Rest.
- Heat or cold therapy.
- Assistive devices- Cane, walker or wheelchair.
- Weight loss.
- Exercise or Yoga therapy.
Specific Treatment for Hip Joint Rheumatoid Arthritis
For Pain in Hip Due To Rheumatoid Arthritis
- NSAIDs.
- Opioids- indicated if NSAIDs are not effective to relieve hip pain.
- Antidepressant Analgesics– Indicated to treat neuropathic pain and pain not responding to opioids.
- Antiepileptic Analgesics– Treats neuropathic pain and pain not responding to opioids.
For Hip Joint Inflammation Due To Rheumatoid Arthritis-
- Anti-inflammatory Medications– NSAIDs, Corticosteroids tablets or injection.
Advanced Treatment For Severe Hip Joint Rheumatoid Arthritis
- Disease-Modifying Anti-Rheumatic Drugs (DMARDs)– DMARDs are used to slow the progress of the disease. DMARD prevents permanent damage of the synovial membrane of the joint and ligaments. Following medications are often used as DMARDs.
- Methotrexate (Trexall)
- Leflunomide (Arava)
- Hdroxychloroquine (Plaquenil)
- Sulfasalazine (Azulfidine)
- Immunosuppressant for Hip Rheumatoid Arthritis– Rheumatoid disease is associated with exaggerated immune activities. Following medications are used to suppress hyperactivities of immune system-
- Azathioprine (Imuran, Azasan)
- Cyclosporine (Neoral, Sandimmune, Gengraf)
- TNF- Alpha Inhibitors for Hip Joint Rheumatoid Arthritis Relief– Rheumatoid arthritis causes increase secretion of Tumor Necrosis Factor-Alpha (TNF-alpha) within hip joint. TNF-alpha triggers inflammation. Inflammation induced by TNF-alpha factor causes pain, joint stiffness and joint swelling. Medications known as TNF-alpha inhibitors reduces production of TNF-alpha factor and provides symptomatic relief from pain, joint swelling and joint stiffness. Following medications are used to inhibit secretions of TNF- alpha factors.
- Etanercept (Enbrel)
- Infliximab (Remicade)
- Adalimumab (Humira)
- Golimumab (Simponi)
- Certolizumab (Cimzia)
- Vitamin D Deficiency– Vitamin D pills or injection
- Muscle Spasm– Muscle spasm is treated with muscle relaxants. Following muscle relaxants are often used-
- Baclofen
- Flexeril
- Skelaxin
- Robaxin
Physical Therapy for Hip Joint Rheumatoid Arthritis
PT Is Indicated For Following Clinical Manifestations-
- Hip Pain
- Muscle Spasm
- Hip Joint Stiffness
- Hip Joint Instability
- Abnormal Gait
Interventional Therapy for Hip Joint Rheumatoid Arthritis
Corticosteroid injection of the hip joint.
Surgery for Hip Joint Rheumatoid Arthritis
- Hip Joint Replacement– Head of the femur, neck of the femur and acetabulum is replaced with artificial metal prosthesis.
- Partial Hip Joint Replacement– Head of the femur or neck of the femur or acetabulum is replaced with artificial metal prosthesis.
- Hip Resurfacing- The surface of the head of the femur and acetabulum is replaced and covered with cobalt metal cap.
Also Read:
- Hip Sprain: Causes, Symptoms, Treatment, Exercises
- Post Traumatic Osteoarthritis of the Hip Joint: Causes, Signs, Treatment, Exercises
- Q&A: Hip Joint Pain Treatment Approach and Options–Everything You Need To Know
- Hip Joint Septic Arthritis: Causes, Symptoms, Treatment, PT, Surgery
- Hip Joint Psoriatic Arthritis: Causes, Symptoms, Treatment, PT, Surgery
- Enthesopathy of Hip: Causes, Symptoms, Treatment
- Predicting the Risk of Rheumatoid Arthritis and Its Age of Onset through Modelling Genetic Risk Variants with Smoking.
Scott IC, Seegobin SD, Steer S, Tan R, Forabosco P, Hinks A, Eyre S, Morgan AW, Wilson AG, Hocking LJ, Wordsworth P, Barton A, Worthington J, Cope AP, Lewis CM.PLoS Genet. 2013 Sep;9(9):e1003808. doi: 10.1371/journal.pgen.1003808.Academic Department of Rheumatology, Centre for Molecular and Cellular Biology of Inflammation, King’s College London, London, United Kingdom ; Department of Medical and Molecular Genetics, King’s College London, London, United Kingdom.
- Autoimmunity in rheumatoid arthritis: different antigens–common principles.
Trouw LA, Huizinga TW, Toes RE.Ann Rheum Dis. 2013 Apr;72 Suppl 2:ii132-6. doi: 10.1136/annrheumdis-2012-202349. Epub 2012 Dec 19.Department of Rheumatology, Leiden University Medical Center, Leiden, the Netherlands.
