LEEP stands for Loop Electrocautery Excision Procedure. Prior to jumping into whether LEEP is effective or not, let us first understand what LEEP is and what it is used for.
What is LEEP and What Is It Used For?
LEEP is also known as large loop excision of the transformation zone (LLETZ). In this procedure, a low voltage electric current is passed through a wire loop to heat it and excise dysplastic tissue of the cervix, vagina, or vulva. LEEP can either be used as a diagnostic biopsy procedure or as a treatment for dysplasia. LEEP is rather quite popular because it is simple to perform, is inexpensive and has less risk and side-effects compared to other procedures such as CO2 ablation or cryocautery. The recovery time is also less with LEEP.
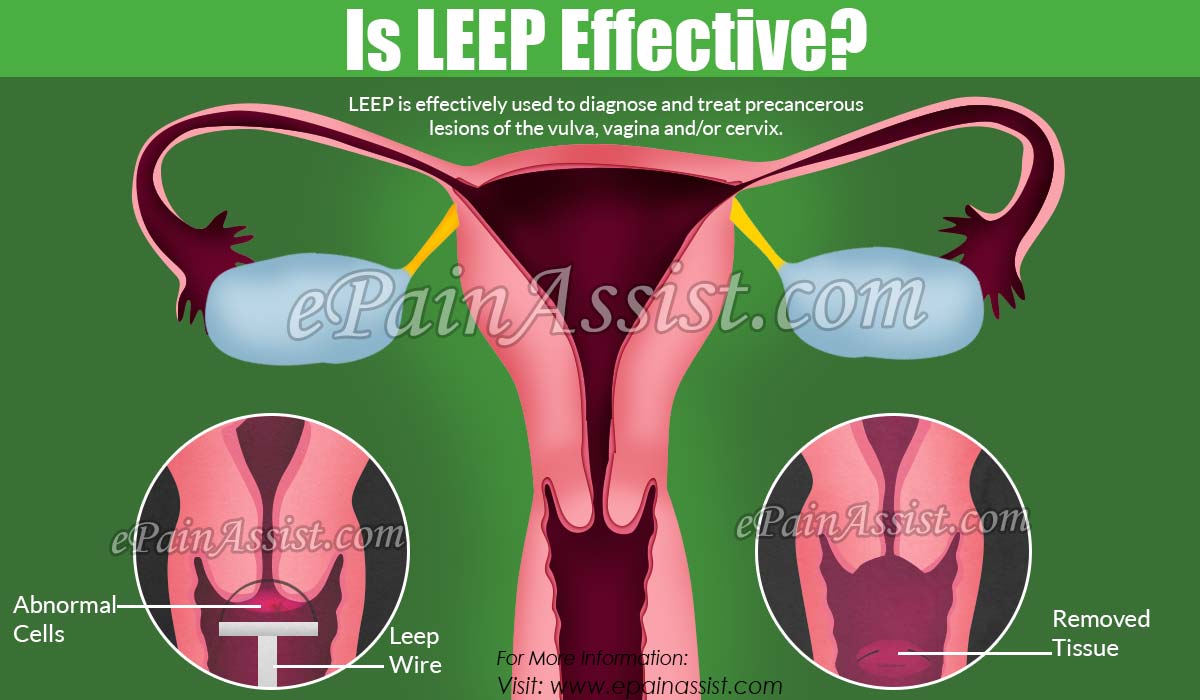
Is LEEP Effective?
LEEP is effectively used to diagnose and treat precancerous lesions of the vulva, vagina and/or cervix. It is mostly used to treat most of the cases of dysplasias, including severe dysplasia and some prudently chosen cases of cervical cancer.
What is a Precancerous Lesion?
A precancerous lesion is a lesion in which the cells are abnormal and have a propensity of developing into cancer over time if left untreated. Precancerous lesions are also known as premalignant lesions. The abnormal cells when viewed under microscope are termed as dysplastic cells and the condition is known as dysplasia. These dysplastic cells can show different levels of abnormality. When only few cells are abnormal it is termed as mild dysplasia, if there are moderate abnormal cells it is termed as moderate dysplasia and if most of the cells are abnormal then it is termed as severe dysplasia.
The cervical dysplasia or premalignancy can be classified into:
Low grade squamous intraepithelial lesion (LSIL): Earlier it was classified as mild dysplasia or cervical intraepithelial neoplasia I (CIN I).
High grade squamous intraepithelial lesion (HSIL): Earlier it was classified under moderate to severe dysplasia. This also includes cervical intraepithelial neoplasia II (CIN II), cervical intraepithelial neoplasia III (CIN III) and carcinoma in situ or adenocarcinoma in situ (AIS).
These precancerous conditions are initially screened with the help of Pap smear and/or HPV (human papilloma virus) and if it is found to be abnormal or HPV testing is positive, then further biopsy is required to confirm the diagnosis. When the diagnosis is confirmed then further treatment is done to prevent progression into cervical cancer.
How is Cervical Dysplasia Treated?
Low grade squamous intraepithelial lesion is usually left untreated and is monitored with yearly Pap smear/HPV screening for resolution. Most of the LSIL resolve over a period of 1 to 2 years. Treatment for high-grade squamous intraepithelial lesion is required and these include excision or destruction of the abnormal cervical cells.
The destruction or ablation procedures include carbon dioxide laser (carbon dioxide laser photoablation), electrocautery and cryotherapy. Ablation procedures are mostly not indicated for severe dysplasias or carcinoma in situ.
The excision or removal procedures are loop electrosurgical excision procedure (LEEP), cold knife conization (CKC) and hysterectomy.
LEEP or CKC are mostly used for the treatment of precancerous cervical dysplasias. However, LEEP is the most popular treatment option as it is simpler, cost-effective procedure which can be done in an outpatient setting under local anesthesia, opposed to cold knife conization that is carried out under general anesthesia. Also LEEP is preferred in women who desire fertility preservation as it has slightly lower risks than cold knife conization. Both the procedures have risk of post-excision bleeding and/or cervical narrowing (stenosis), but are less in LEEP in comparison to CKC. Hysterectomy is the removal of uterus and is reserved for recurrent or persistent cervical dysplasias after the treatment with other treatment procedures. It is usually not the first line of treatment for dysplasias. The final treatment depends on the discretion of doctor.
The efficacy of LEEP has been comparable to CO2 laser, electrocautery, cryotherapy and cold knife conization. It is a highly effective procedure and has become the most popular procedure amongst all the above procedures for cervical dysplasia, given its efficacy, simplicity, cost-effectiveness and lower risks. The dysplasia resolution rate is 90 to 95%, and has recurrence rate of 5 to 10%. It requires regular follow-up screening for cervical cancer prevention.
Also Read:
