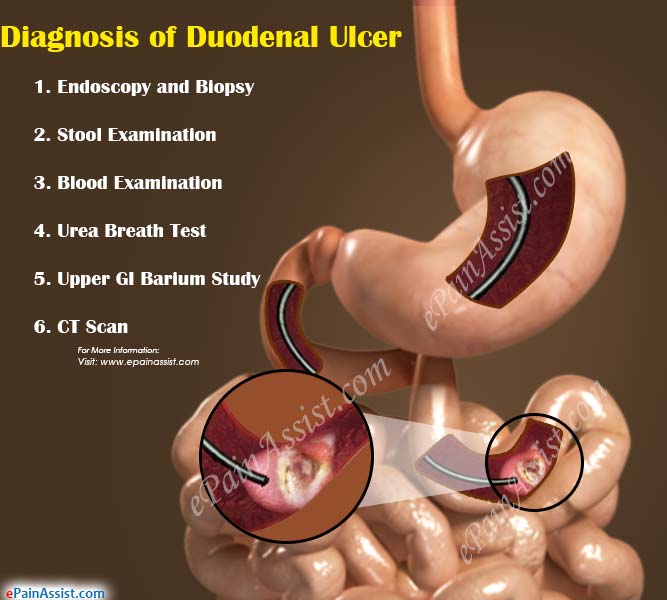
Diagnosis of Duodenal Ulcer
Symptoms caused by duodenal ulcer often are similar to gastric ulcer. The ulcers caused by gastric acidic juice are localized over esophagus, stomach and duodenum and recognized as a peptic ulcer. Duodenal ulcer is the most common ulcer of peptic ulcer. In few cases duodenal ulcer may present with gastric ulcer and in this situation the diagnosis is peptic ulcer. When the ulcer is localized exclusively in duodenum then the disease is diagnosed as duodenal ulcer.
The symptoms of pain are presented differently when individual is suffering with either gastric or duodenal ulcer. The food content when discharged from stomach is acidic in pH and has higher concentration of acidic molecules. The food mixed with gastric juice is treated by digestive enzymes in duodenum. The pH is high during the initial phase of digestion and later the acidic molecule concentration is reduced as the duodenal enzymes neutralizes the gastric juice. The pain is observed at peak after 2 to 3 hours of food intake as the food mixed with acidic stomach juice passes into duodenum. Later the intensity of pain subsides. Patient is often asymptomatic between the hours of severe pain.
What are the Symptoms of Duodenal Ulcer?
Upper Left Side Abdominal Pain Caused By Duodenal Ulcer-
Duodenal ulcer pain is felt on left side of umbilicus unlike gastric ulcer pain, which is felt under the sternum on left side. Character of duodenal ulcer pain is burning pain. The stomach or gastric ulcer pain is at peak when stomach is empty and there is no food content in stomach. The reason gastric acid pain is severe during empty stomach is because of highest acid content of the gastric juice. On the contrary duodenal ulcer pain is at peak and severe after 2 to 3 hours of food intake, when food is acidic, semi digested food and is pushed into duodenum. After 2 to 3 hours the food is pushed into jejunum and small intestine, during this phase patient may not feel any pain or pain intensity is mild. Gastric ulcer pain often become severe after 4 to 5 hours following dinner resulting in interference with sleep.
Bloating Associated With Duodenal Ulcer
Bloating is a feeling of abdominal distension though there may not be any actual intestinal bloating. Bloating is also observed when duodenum and small bowel is distended because of trapped air. Symptom is temporary and often disappears after ingestion of several antacids or antiflatulent pills like simethicone.
Retching Associated with Duodenal Ulcer
Retching is less common with gastric ulcer as compared to duodenal ulcer. The persistent pain in duodenum triggers reverse intestinal movement known as peristalsis. In normal case peristalsis pushes food forward toward next section of bowel. In few cases of duodenal ulcer, the peristalsis become reversed and food is pushed in to stomach. Such a reversed peristalsis in presence of duodenal ulcer causes forceful feeling of nausea.
Hematemesis Caused by Duodenal Ulcer
Hematemesis is a condition, which is observed when blood is found in vomitus or patient is spitting the blood. Hematemesis is often observed in patient suffering with gastric ulcer and very rare in duodenal ulcer. Hematemesis in patient suffering with duodenal ulcer is observed following severe retching resulting in vomiting and blood in vomitus. Hematemesis in absence of retching suggests diagnosis of gastric ulcer.
Melena or Blood in Stool Caused by Duodenal Ulcer
Blood discharged from duodenal ulcer is mixed with stool. The blood in stool is diagnosed as melena with occult blood in stool. Occult blood in very small quantity may not change the color of stool but substantial quantity of blood if mixed with stool then stool looks dark black.
Other Factors That Help in Diagnosis of Duodenal
In addition to the above stated symptoms of duodenal ulcer, following can also help in the diagnosis of duodenal ulcer.
History of Smoking Associated With Duodenal Ulcer
Patient suffering with duodenal ulcer often is chronic smoker. Though diagnosis is not depended on history of smoking but symptoms associated with history smoking signifies the diagnosis of duodenal ulcer.
History of Stress and Anxiety Associated With Duodenal Ulcer
Stress and anxiety causes peptic ulcer and very rarely selective duodenal ulcer. Few cases may suggest individual is suffering with abdominal pain as well as anxiety and stress.
What are the Diagnostic Test for Duodenal Ulcer?
Endoscopy and Biopsy
Duodenoscopy study is performed by using endoscope.1 Endoscope is a long tubular camera, which passed through mouth in to stomach and then duodenum. The eye piece located at opposite end is connected to TV screen. Physician who performs the test is knows as gastroenterologist. Gastroenterologist observes the image of stomach and duodenal mucosa on TV screen, which is magnified several fold. Careful examination of entire mucosa of stomach and duodenum is performed to find the ulcer. Once the ulcer is located in duodenum the piece of border of ulcer is removed as a biopsy for lab study. The tissue biopsy study provides the microscopic changes caused by ulcer and also rules out cancer of mucosa, which is extremely rare.
Stool Examination to Diagnose Duodenal Ulcer
Stool is examined in lab for blood. Presence of blood is not a specific test since blood could be discharged from several inflammatory diseases of small intestine and large colon. The blood in stool with history of pain and finding of endoscopic study signifies the diagnosis of duodenal ulcer.
Blood Examination for Duodenal Ulcer
Blood is tested for Helicobacter Pylori bacteria. The culture of blood serum shows the growth of H. Pylori bacterial colony.
Urea Breath Test
Urea is a waste product secreted by body and discharged in urine. Patient is asked to drink a liquid containing urea. H. Pylori bacteria breaks down the urea to carbon di oxide. Following intake of urea patient is asked to inhale in bag and carbon di oxide content is examined. In patient suffering with H. Pylori carbon di oxide concentration is high in exhaled breath.2
Upper GI Barium Study
Barium study is often avoided. The small ulcer is often difficult to observe in post barium X-Ray. Many centers prefer to perform barium study if patient refuses invasive study such as endoscopy. Patient is asked to swallow barium meal and after 1 to 2 hours once the barium reaches duodenum multiple series of x-ray is performed.3
CT Scan
CT Scan is not of much help in diagnosing duodenal ulcer. CT scan is one of the important diagnostic study to diagnose perforated ulcer. CT scan helps to identify the inflammatory changes of peritoneal tissue and fistula around the duodenum.4
Note: The most important steps in diagnosis of duodenal ulcer is to consult a gastroenterologist. The clinical examination, interpretation of finding of examination and analysis of test results has to be evaluated by expert in the field of diseases of gastroenterology system. Our recommendation is if you suffer with any of similar symptoms then consult gastroenterologist as soon as possible.
Also Read:
- What is Duodenal Ulcer: Risk Factors, Complications, Prevention, Home Remedies
- What Causes Duodenal Ulcer?
- Diet for Duodenal Ulcer Patients
Duodenoscopy in the diagnosis of upper gastrointestinal disease.
Beaudin DJ, DaCosta LR, Prentice RS, Beck IT.
Can Med Assoc J. 1973 Mar 3;108(5):565-9.
https://www.ncbi.nlm.nih.gov/pubmed/?term=Can+Med+Assoc+J.+1973+Mar+3%3B108(5)%3A565-9.+Duodenoscopy+in+the+diagnosis+of+upper+gastrointestinal+disease.+Beaudin+DJ%2C+DaCosta+LR%2C+Prentice+RS%2C+Beck+ITEffect of age on the frequency of active Campylobacter pylori infection diagnosed by the [13C]urea breath test in normal subjects and patients with peptic ulcer disease.
Graham DY1, Klein PD, Opekun AR, Boutton TW.
J Infect Dis. 1988 Apr;157(4):777-80.
https://www.ncbi.nlm.nih.gov/pubmed/3346569Endoscopy and routine and double-contrast barium meal in diagnosis of gastric and duodenal disorders.
Rogers IM, Sokhi GS, Moule B, Joffe SN, Blumgart LH.
Lancet. 1976 Apr 24;1(7965):901-2.
https://www.ncbi.nlm.nih.gov/pubmed/?term=Lancet.+1976+Apr+24%3B1(7965)%3A901-2.+Endoscopy+and+routine+and+double-contrast+barium+meal+in+diagnosis+of+gastric+and+duodenal+disorders.+Rogers+IM%2C+Sokhi+GS%2C+Moule+B%2C+Joffe+SN%2C+Blumgart+LH.Gastrointest Radiol. 1992 Winter;17(1):5-8.
CT in upper gastrointestinal tract perforations secondary to peptic ulcer disease.
Fultz PJ1, Skucas J, Weiss SL.
Gastrointest Radiol. 1992 Winter;17(1):5-8.
https://www.ncbi.nlm.nih.gov/pubmed/1544559
