What is Spinal Cord Stimulator?
Spinal cord stimulator consists of two devices Epidural Electrode and Neurostimulator (Generator). Epidural electrode is implanted in epidural space and Neurostimulator (generator) is placed under the skin over abdomen or buttocks. Spinal cord electrode is connected internally to generator by a specially designed connecting wire. Spinal Cord Stimulator (Generator) is programed by an external remote.
How Does Spinal Cord Stimulator Relieve Pain?
Neurostimulator sends signal to epidural electrode to stimulate spinal cord and blocks pain impulses going to the pain center in brain.1, 2 Spinal cord stimulator is electrotherapy used for the neuromodulation.1, 2
Watch 3D Video of Placement of Spinal Cord Stimulator To Relieve Back Pain
How Does Spinal Cord Stimulator Block Pain Impulse at Spinal Cord?
The pain impulses pass through a gate (Gate Control Theory) at spinal cord.1, 2 Opening and closing of gate is controlled by neurotransmitters (neurochemicals). Spinal cord stimulator closes the gate by modulating the neurochemicals known as neuromodulation.1, 2
What is Neuromodulation?
Spinal cord stimulator modulates neurotransmitters in spinal cord and also pain controlling gate. The modulation or alterations of forward passage of pain impulse to brain is called neuromodulation.
When was the First Spinal Cord Stimulator Placed in USA?
Dr. Shealy inserted first spinal cord stimulator in human subject in 19671 and Dr. Shimogi published the first scientific paper regarding insertion of spinal cord stimulator in the epidural space.3
Is the Spinal Cord Stimulator Better Now Than in 1967?
Yes, over the last 45 years several Institutions have done research on device and its therapeutic effects on patients. Surgical technique and spinal cord stimulator device has been improved over the last several years.
Is Spinal Cord Stimulator Approved By FDA (Food And Drug Administration)?
Yes, FDA has approved spinal cord stimulator since 1989.
Is Spinal Cord Stimulator Effective in Treating Back Pain in All Segment of the Spinal Cord?
Yes, spinal cord stimulator has been effective in treating several diseases causing upper, middle and lower back pain or backache.4
Which Diseases Causing Upper Back Pain Are Treated With Spinal Cord Stimulator?
Spinal Cord Stimulator Helps Treat The Following Conditions That Can Cause Upper Back Pain Or Backache: 6,7
- Cervical Failed Back Syndrome
- Cervical Radicular Pain
- Cervical Radiculopathy
- Cervical Post-Herpetic Neuralgia
- Cervical Complex Regional Pain Syndrome
- Cervical Peripheral Neuropathy
- Cervical Spasticity5
Which Diseases Causing Middle Back Pain Are Treated With Spinal Cord Stimulator?
Spinal Cord Stimulator Helps Treat The Following Conditions That Can Cause Middle Back Pain or Backache:
- Thoracic Failed Back Syndrome
- Thoracic Intercostal Neuralgia
- Cervical Radiculopathy
- Thoracic Post-Herpetic Neuralgia
- Cervical Complex Regional Pain Syndrome
- Thoracic Arachnoiditis
- Refractory Angina
Which Diseases Causing Lower Back Pain Are Treated With Spinal Cord Stimulator?
Spinal Cord Stimulator Helps Treat The Following Conditions That Can Cause Lower Back Pain or Backache:
- Lumbar Failed Back Syndrome6
- Lumbar Radicular Pain
- Lumbar Radiculopathy
- Lumbar Post-Herpetic Neuralgia
- Lumbar Complex Regional Pain Syndrome
- Lumbar Peripheral Neuropathy
- Peripheral Vascular Disease
- Lumbar Spasticity5
Am I A Candidate for Spinal Cord Stimulator for My Back Pain, I Have Had Multiple Back Surgery (Failed Back Surgery)?
Yes, you should consult an Interventional Pain Specialist for spinal cord stimulator for your back pain or backache. You will be scheduled for temporary placement of electrode for trial. Trial period will last for 2 to 3 weeks. The electrode is also known as epidural electrode. One or two epidural electrodes are placed in epidural space depending on pain distribution. Unilateral pain is treated with single spinal cord electrode and bilateral pain is treated with two spinal cord electrode (right and left electrode).
What Does Trial Lead Placement Involve?
Trial electrode is a temporary epidural electrode, which is placed in epidural space for 2 to 3 week. The procedure involves percutaneous placement of epidural electrode through epidural needle. Epidural electrode are placed on right or left side at posterior or back of spinal cord for unilateral (one side) pain. Bilateral pain is treated with two epidural electrodes placed on right and left side in the epidural space.
Why is Trial Lead Placed in Epidural Space?
Spinal cord is tubular in shape and surrounded by a cerebrospinal fluid (CSF). A thick membrane of fibrous tissue called dura encloses CSF and spinal cord. Space outside dura is an epidural space. Epidural space is relatively easy to find without penetrating through dura. Placement of epidural electrode at appropriate level within epidural space is necessary to obtain optimum pain relief.
Is it Safe to Place Spinal Cord Electrode Close to Spinal Cord?
Yes, it is safe and several thousand surgeries have already been performed with least side effects. Thick dura prevents transmission of infection to CSF and spinal cord. Dura and CSF also act as a shock absorber against metallic electrode. CSF also dampens passage of stimulation from stimulator to spinal cord.
How Would I Be Qualified For Permanent Placement of Spinal Cord Stimulator?
You will be considered for placement of permanent epidural electrode and neurostimulator only after a trial of 2 to 3 weeks. Back pain relief of over 50% is expected during the trial period to be qualified for permanent placement of electrode and generator.
What is Dermatomal Distribution of Pain?

Pain spreads along the spinal nerve to neck, arms, chest, abdomen and legs. Example of dermatomal distribution of sciatica pain is as follows. Sciatica pain is felt in feet and lower leg and pain is carried by a L4, L5 and S1 spinal nerve. The dermatomal distribution of this pain is feet, ankle and lower leg and lesions causing irritation of nerve are L4, L5 and S1 spinal nerve. Dermatomal distribution of pain determines the level of spinal cord where pain is generated.

How Would Pain Specialist or Neurosurgeon or Orthopedic Surgeon Determine the Appropriate Level of Spinal Cord to Place Epidural Electrode to Achieve Optimum Pain Relief?
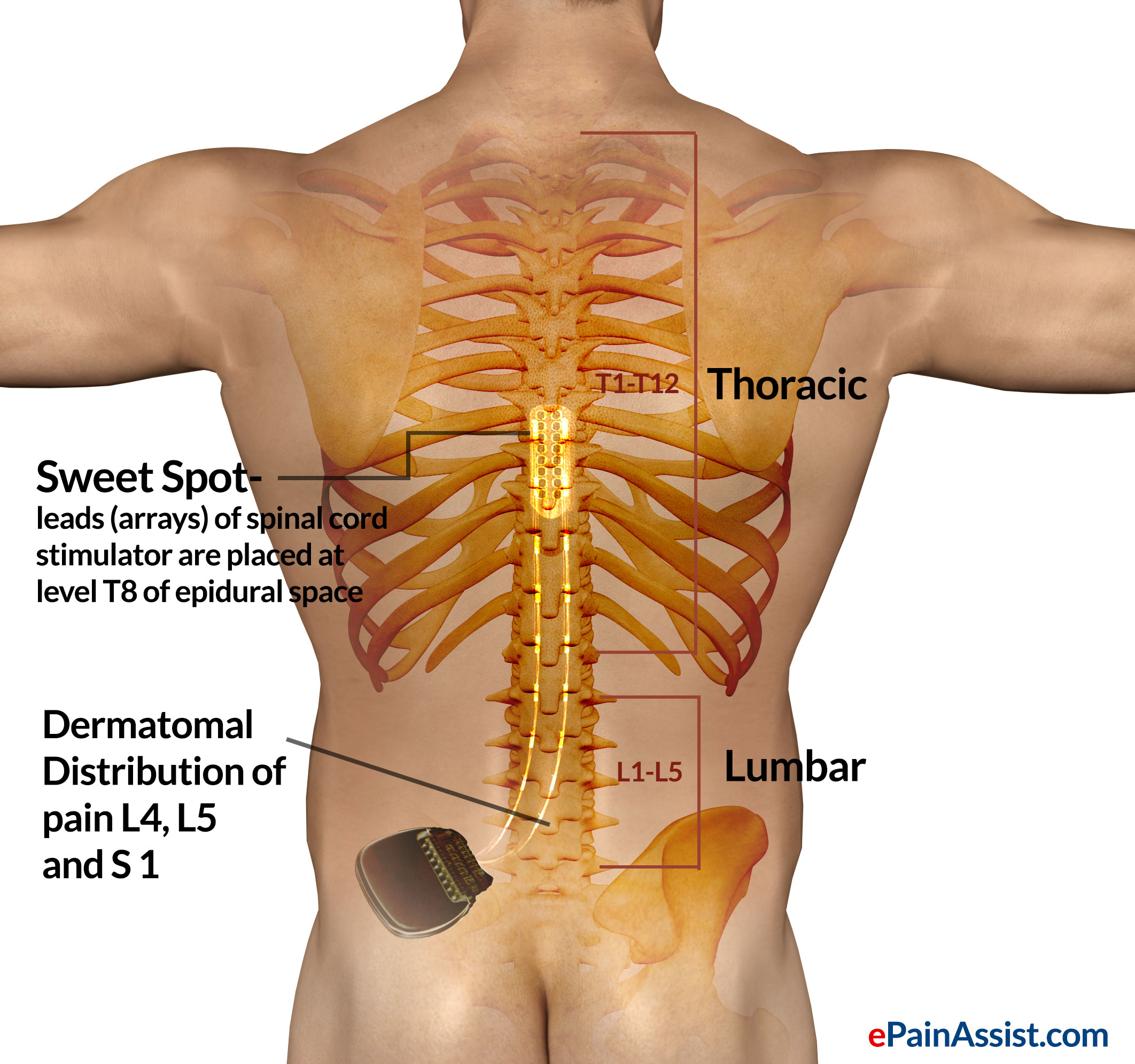
The sweet spot to modulate the pain is often at much higher level than the level of dermatomal pain. Dermatomal spread of pain in leg is caused by irritation of L4, L5 and S1 nerve. Sweet spot for modulation of L4, L5 and S1 dermatomal pain is at thoracic spinal level of T8 to T11. Trial electrode (Trial lead) is placed in epidural space at level of T5 and T6. Surgeon will stimulate the spinal cord to find out the spread of stimulation. Lead will be pulled gently down by few mm until the paresthesia or pleasant tingling stimulation is felt over painful dermatome of leg. Epidural electrode is then anchored to ligaments at the back of the spine once the satisfactory pain relief is accomplished.
What is a Sweet Spot?
The sweet spot is the level of spinal cord when stimulated by epidural electrode causes spread of pleasant tingling stimulation or paresthesia along the dermatome of painful area. Sweet spot is evaluated during trial while selecting appropriate placement of epidural spinal cord stimulator to achieve optimum pain relief.
Why Percutaneous Spinal Cord Stimulator is Preferred Over Paddle Electrode?
Percutaneous electrode is regularly used for trial and in most cases also for permanent electrode placement. Electrode is placed in epidural space through special epidural needle. Surgery is less extensive and placement of electrode does not need laminectomy as in placement of paddle electrode.
What is The Advantage of Paddle Electrode?
Paddle type of electrode is preferred if percutaneous electrode placement fails or patient had multiple back surgery. Paddle electrode rarely changes position in epidural space, unlike percutaneous electrode. Paddle electrode is placed following a partial laminectomy surgical procedure.8

What is Laminectomy?
Lamina is posterior part of the ring of the vertebral bone, which surrounds epidural space. Partial laminectomy is a surgery, which involves removal of small piece of lamina bone. Paddle electrode is flat and wide. Electrode cannot be placed through needle. Paddle electrode needs wider surgical space to place electrode in epidural space.
How is The Trial Spinal Cord Stimulator Programmed?
Trial spinal cord stimulator is programmed at recovery room following surgery. Distal end of the spinal cord stimulator will be connected to external generator or neurostimulator. Trial spinal cord stimulator is programmed using Remote Physician Programmer. There are two types of programmer, Physician Programmer and Patient Programmer.
Why Two Programmers Are Used in Spinal Cord Stimulator?
Physician or technician will use the Physician Programmer for initial programming and for any changes if needed in future. Programmer will choose the combination of leads (arrays) located at proximal end of the spinal cord stimulator (electrode) placed at epidural space. Multiple leads are activated to generate modulating impulses to achieve optimum back pain relief. Patient is discharged home with Patient Remote Programmer.
What Can I Do With Patient Programmer or Patient Remote Programmer?
You will be able to switch the neurostimulator on and off. You will be able to increase or decrease the intensity of spinal cord stimulation to achieve optimum symptoms of tingling spread over painful dermatome (anatomical area).

Describe The Structure of Epidural Electrode?
Epidural Electrodes are of two types percutaneous and paddle type. Percutaneous epidural electrode is thin and tubular used mostly for trial and also permanent use. Paddle epidural electrode is flat and wider, mostly used for permanent use. The electrode consists of arrays of leads on both sides. Each leads are connected to each other. Each electrode may have 4 to 8 leads.
What Are The Configurations of Electrode?
Percutaneous and paddle type epidural electrode host single or paired column of 4 to 8 leads (arrays) at the proximal end. The leads or arrays are connected to distal contact by tiny wires. Distal metallic contacts are located at distal (outer) end of spinal cord stimulator. Distal (outer) end of electrode is threaded in one of the slots of external or internal neurostimulator and locked in with special screws. Electrode is now linked to computer programmer (external or internal neurostimulator).
What is The Function of External or Internal Neurostimulator or Generator?
Neurostimulator is the brain of spinal cord stimulation. Electrical signal from Neurostimulator (generator) is transmitted to distal contact and through tiny wire to proximal leads (arrays). The leads transmits radiofrequency signal passing through CSF to spinal cord. Neurostimulator controls all the leads (arrays) located within proximal end of spinal cord stimulator. Neurostimulator can choose number of leads on one or both side. Neurostimulator can send impulses at various set frequencies, voltage, waveform and duration to electrode. Impulses are programmed at constant current, variable voltage or constant voltage, and variable current settings. Stimulation can be set on or off at desired time.
Can I Change The Combinations And Stimulation Patterns of Leads of Electrode With Patient Control Programming Remote?
No, you cannot change the combination of leads (arrays) that are selected for spinal cord stimulation. The impulses generated by the leads are selected to modulate particular level of spinal cord during programming by experts. Leads can be changes by using Physician Programmer only.
Why External Instead of Internal Neurotransmitter Is Used For Trial?
Trial lasts for 2 to 6 weeks, in most cases 2 to 3 weeks. Trial epidural electrode is removed after 2 to 3 weeks. Internal generator is expensive and battery inside the generator last for over 2 years. Placement of generator is an additional surgery and not recommended for 2 to 3 weeks trial. External generator is used only for trial. External Generator can be used for different patients and works on AA or AAA batteries
What Are The Different Types of Neurostimulator or Generators?
External Neurotransmitter- used only during trial. Equipment is reused after cleaning and external sterilization.
Internal Neurotransmitter- Internal neurotransmitters are classified as follows-
- Implantable Pulse Generator (IPG)- The Internal Implantable Pulse Generator is either rechargeable or disposable. Rechargeable Neurotransmitter can be charged from external contact and replacement may not be needed for over 10 years. Disposable neurotransmitter has a battery, which lasts for 3 to 5 years and once battery is exhausted the IPG needs to be replaced.
- Implantable Radiofrequency (RF) Receiver- RF receiver is implanted under the skin. RF receiver is thin and does not have a battery of it’s own. External neurostimulator is used to transmit RF signals to RF receiver to send signals to epidural electrode.
Which Neurotransmitter is Better RF or IPG?
RF Receiver-
- Advantage- RF receiver is thin and lasts for life of patient. RF receiver lacks battery. Patient feels comfortable holding implanted RF receiver under the skin as compared to IPG.
- Disadvantage- RF receiver receives signal through external pad, which is connected to external neurostimulator. External pad is placed over the skin against the RF receiver. Disadvantage is that pad may slip out of position resulting in interruption of signals to spinal cord. Eventually it may be a nuisance since frequent adjustment is necessary to place pad over the RF receiver.
Intermittent Pulse Generator (IPG Neurotransmitter)
- Advantage- Various sizes are available depending on battery capacity. Ultra IPG is thin and small that is comparable to RF receiver. Daily maintenance is minimum, generator can be put on or off with remote programmer.
- Disadvantage- Replacement of IPG may be necessary after 3 to 5 years depending on daily usage.
What Are The Complications of Spinal Cord Stimulator?
Spinal cord stimulator includes epidural electrode and neurotransmitters.
Complications of Spinal Cord Stimulator Are As Follows-
Epidural Electrode-
- Bleeding In Epidural Space
- Infection
- Dural Puncture and CSF Leak
- Catheter Position Change
- Fracture of Electrode
- Disconnection from Neurotransmission
Neurotransmitter-
- Bleeding Around the Generator
- Infection of Pocket around Generator
- Pulse Generator Rotates Within the Pockets.
Also Read:
- Treatment for Back Pain
- Coping With Back Pain Made Easier With These Home Remedies
- Physical Therapy for Back Pain
- Tips to Cope With Back Pain While Sitting, Standing, Lifting, Driving
- Sleeping Postures To Prevent Back Pain & Neck Pain
- Measures To Alleviate Low Back Pain When Driving Long Distance
- Linderoth, B. and Foreman, R. (1999) “Physiology of spinal cord stimulation: review and update”. Neuromodulation, 3, 150–164.
- Mazak, R., and Wall, P.D. (1965). Pain mechanisms: a new theory. Science, 150:971–979.
- Sealy, C.N., Mortimer, J.T., and Resnick, J. Electrical inhibition of pain by stimulation of the dorsal columns: Preliminary reports. J. Int. Anesth. Res. Soc, 46:489–491, 1967.
- Oakley, J. and Prager, J. (2002). “Spinal cord stimulation: mechanism of action”. Spine, 27, 2574–2583.
- Pinter, MM; Gerstenbrand, F; Dimitrijevic, MR (2000 Sep). “Epidural electrical stimulation of posterior structures of the human lumbosacral cord: 3. Control Of spasticity.”. Spinal cord 38 (9): 524–31.
- North, R.B., Kidd, D.H., and Piantadosi, S. (1995). “Spinal cord stimulation versus reoperation for failed back surgery syndrome: a prospective, randomized study design”. Acta Neurochir. Suppl.,64, 106–108.
- North, R. and Wetzel, T. (2002). “Spinal cord stimulation for chronic pain of spinal origin”. Spine, 22, 2584–2591.
- Barolat, G., Oakley, J., Law, J., et al. (2001). “Epidural spinal cord stimulation with a multiple electrode paddle lead is effective in treating low back pain”. Neuromodulation, 2, 59–66.
