Lumbar radiculopathy is the nerve irritation caused due to damage to the discs between the vertebrae. Lumbar radiculopathy is more commonly known as sciatica.
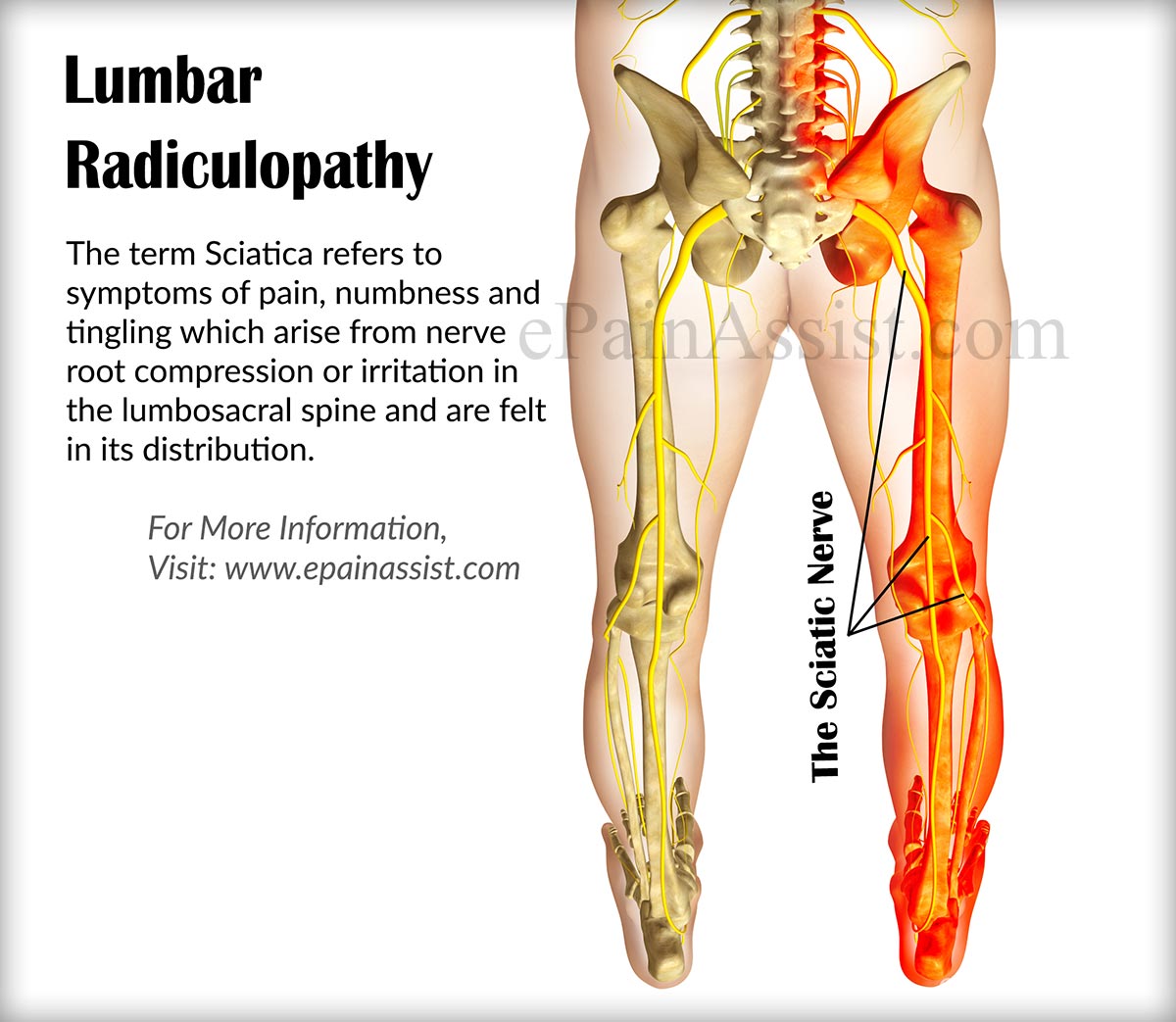
The term Sciatica refers to symptoms of pain, numbness and tingling which arise from nerve root compression or irritation in the lumbosacral spine and are felt in its distribution. Symptoms of sciatica typically extend below the knee, from the buttocks, across the back of the thigh, to the outer calf, and often to the foot and toes.
Epidemiology of Lumbar Radiculopathy or Sciatica
Approximately 3-5% of the population is affected with lumbosacral radiculopathy. Both men and women are affected equally, where men are most commonly affected in their 40s, and women are most commonly affected between ages 50-60. 10-25% of those who have this condition develop symptoms that persist for more than 6 weeks.
Pathophysiology of Lumbar Radiculopathy or Sciatica
- Herniated Intervertebral Disc (Slipped Disc): Lumbosacral nerve root compression due to disc herniation causing sciatica most commonly occurs at L4-L5 and L5-S1 levels. For example, the L5 nerve root passing between the 4th and 5th lumbar vertebrae gets compressed.
- Spondylolisthesis: Vertebra slips forward on the lower vertebrae.
- Spinal Stenosis: This is narrowing of spinal canal. It can be caused by congenital stenosis as well as spondylolisthesis. Lateral recess stenosis and foraminal stenosis tend to cause sciatica. Central spinal stenosis tends to cause spinal claudication which produce paresthesias, calf pains and numbness with ambulation.
- Infection, growth within the spine or injury: Rare causes.
Causes and Risk Factors of Lumbar Radiculopathy or Sciatica
Disc damage occurs due to degeneration or wear and tear of the outer ring of the disc or traumatic injury or both. Due to this, the central softer portion of the disc ruptures and herniates through the outer ring of the disc and abuts the spinal cord or its nerves as they exit the bony spinal column. This abutment of nerves causes lumbar radiculopathy.
Common Risk Factors Include
- Older age.
- Mental stress.
- Jogging.
- Poor job satisfaction.
Signs and Symptoms of Lumbar Radiculopathy or Sciatica
Lumbar radiculopathy symptoms vary depending upon the specific nerve roots affected. The most common symptoms are numbness, tingling, and weakness in the legs. This indicates that the nerve roots along the spinal cord are affected. Sometimes the skin may be supersensitive to touch. If any or all of these symptoms are present, consulting a physician for an accurate diagnosis is recommended.
The most common symptom of lumbar radiculopathy is sciatica. Sciatica pain typically radiates from the back to the buttocks, sometimes all the way to the feet. Sensory symptoms are more common in radiculopathy. When motor sensory symptoms such as muscle weakness are present, it may represent more severe nerve compression.
Treatment of Lumbar Radiculopathy or Sciatica
- Treatment ranges from medical management to surgery depending upon the condition. Medical management includes medications to relieve pain and muscles spasm, epidural injections, physical therapy (heat, ultrasound, massage, electrical stimulation), and rest so as to avoid re-injury.
- Surgery may be necessary if the pain is unrelenting with severe impairment of function, or incontinence. Procedure performed depends on the overall status of the spine, and the age and health of the patient. Procedures include discectomy (excision of herniated disc) with laminotomy (making small hole in bone of lumbar spine surrounding spinal cord), laminectomy (excision of bony wall) by needle technique (percutaneous discectomy), and chemonucleolysis (disc dissolving procedure).
Investigations for Lumbar Radiculopathy or Sciatica
- Electromyogram (EMG) and Nerve Conduction Velocity (NCV).
- Computer Assisted Tomography Scan (CT scan).
- Magnetic Resonance Imaging Scan (MRI).
Also Read:
- Manage Sciatica with 5 Simple Lifestyle Modifications: Proper Posture, Fitness, Nutrition
- Does Sciatica Ever Go Away? How long does Sciatica Pain Last?
- Can Reiki Relieve Sciatica?
- Improving Sciatica Pain With Medications, Exercises And Alternative Treatments
- Yoga for Sciatica: 5 Poses to Ease Sciatica Pain
- Can Sciatica Cause Knee Pain?
Also Watch:
