Pericarditis is the inflammation of one or all layers of pericardium. The different layers of pericardium are parietal (outer layer), middle fluid layer (prevents friction between the outer and the inner layer), and visceral (inner layer) pericardium. Pericardium surrounds the heart and holds it into place when in motion. Infection, heart attack, trauma, heart surgery, cancer, radiation, autoimmune disease, and certain drugs can cause it.
Pericarditis Symptoms
Pericarditis mostly causes sharp chest pain and can cause dull chest pain that might radiate from the middle of the chest to the neck/back area. The chest pain worsens on lying down, swallowing or coughing, but is relieved on sitting erect. Other symptoms include shortness of breath, increased heart rate, painful breathing, difficulty swallowing, fatigue, fever, chills, and malaise. Men, between the ages of 20 to 50 years, are at a greater risk of developing pericarditis and around 20 to 30% may have a recurrence of pericarditis.
Diagnosis and Treatment
The diagnosis of pericarditis is done after evaluating medical history, examining the patient for signs and blood test. Imaging such as chest X-ray, electrocardiogram, echocardiogram, or CT heart can also be done to look at the heart and tissue layer. The treatment of pericarditis includes NSAIDs such as ibuprofen and naproxen for pain and inflammation, steroids for severe inflammation, antibiotics for bacterial infection and colchicine for repetitive and prolonged symptoms of pericarditis.
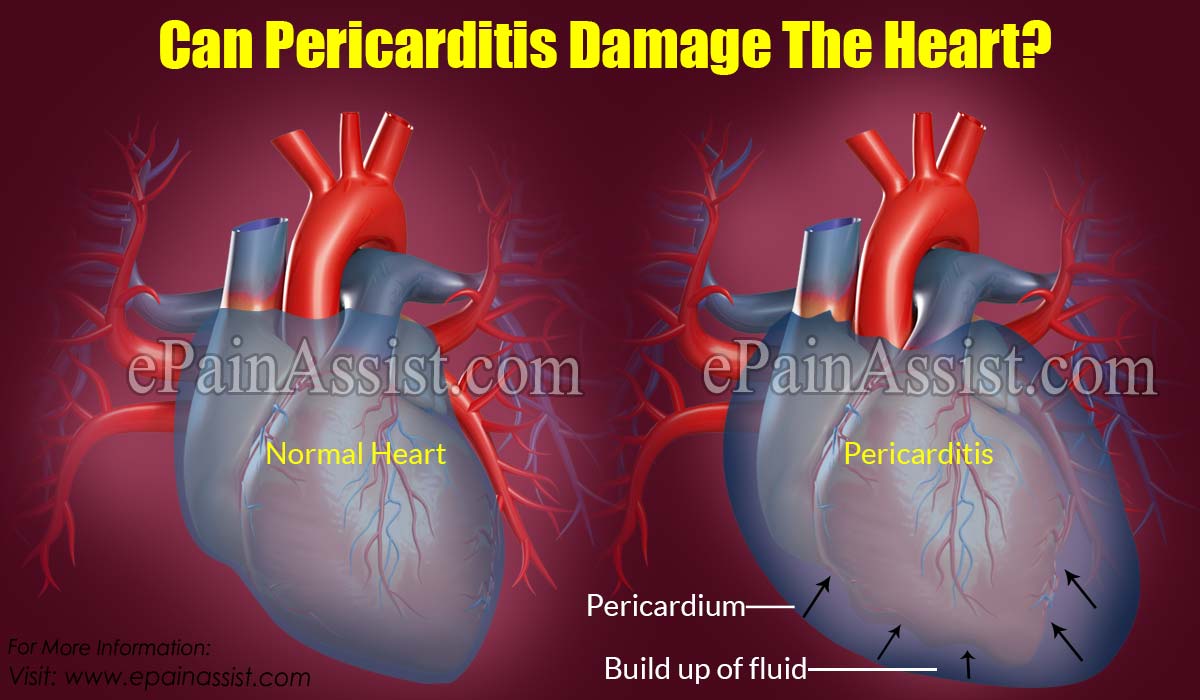
Can Pericarditis Damage The Heart?
If pericarditis is left untreated then it necessarily does not damage the heart, but may lead to certain complications such as cardiac tamponade and constrictive pericarditis.
Cardiac tamponade is the accumulation of large amounts of fluid inside the pericardial sac that affects the heart causing decreased blood pressure and alteration of heart function. Cardiac tamponade requires immediate drainage of fluid known as pericardiocentesis and if fluid is not drained from the pericardial sac then the patient might show signs of shock, hypotension or even congestive heart failure.
Untreated pericarditis could also lead to constrictive pericarditis. It is a chronic inflammation of pericardium that leads to scarring and thickening of the pericardium. The elasticity of the pericardium is lost, which makes it rigid and difficult for the heart to function properly. The symptoms of constrictive pericarditis include difficulty breathing, shortness of breath, fatigue, swelling of extremities, chest pain, low-grade fever, unexplained weight gain, and irregular heartbeat (atrial fibrillation).
Causes and Risk Factors of Constrictive Pericarditis
Constrictive pericarditis is idiopathic in nature. The other possible causes may include heart surgery, tuberculosis, radiation therapy to the chest, viral/bacterial infection. Constrictive pericarditis is caused due to rigidity of the pericardium due to which it is unable to expand properly, which prevents the heart chambers from filling up with blood completely that might lead to heart failure symptoms.
Constrictive pericarditis is an extremely rare condition in adults as well as in children, but people who are not treated for pericarditis are at a greater risk of developing constrictive pericarditis. Other risk factors include autoimmune disease (lupus and rheumatoid arthritis), trauma to heart, and certain medications.
Diagnosis and Treatment of Constrictive Pericarditis
Constrictive pericarditis is difficult to diagnose as it is most often confused with other heart conditions such as cardiac tamponade or restrictive cardiomyopathy and is often misdiagnosed. Imaging such as chest X-ray, MRI, CT scan, cardiac catheterization, electrocardiogram, and echocardiogram may be done for further diagnosis of constrictive pericarditis.
The treatment of constrictive pericarditis is focused on improving heart function and to relieve signs and symptoms. Diuretics may be used to remove fluid buildup in the extremities, pain medication for pain relief, antiinflammatories for the reduction of inflammation, use of colchicines and/or steroids. The patient is also advised to rest and reduce the intake of salt in his/her diet. If symptoms do not improve with medications then the last resort is pericardiectomy, which is the removal of the scarred portion of the pericardium. The patient does lead a healthy life after proper treatment of constrictive pericarditis, but it is best to prevent this complication and be treated for pericarditis to avoid progression to constrictive pericarditis.
Also Read:
