Ocular hypertension is a medical term used to define a condition characterized by elevated eye pressure i.e. intraocular pressure. Intraocular pressure is the pressure of the fluid present inside the eye. It is measured using a tonometer that is calibrated to measure the eye pressure in millimeters of mercury (mmHg). Eye pressure ranges between 10 – 21 mm Hg under normal circumstances. In ocular hypertension, the eye pressure is above 21mm Hg.
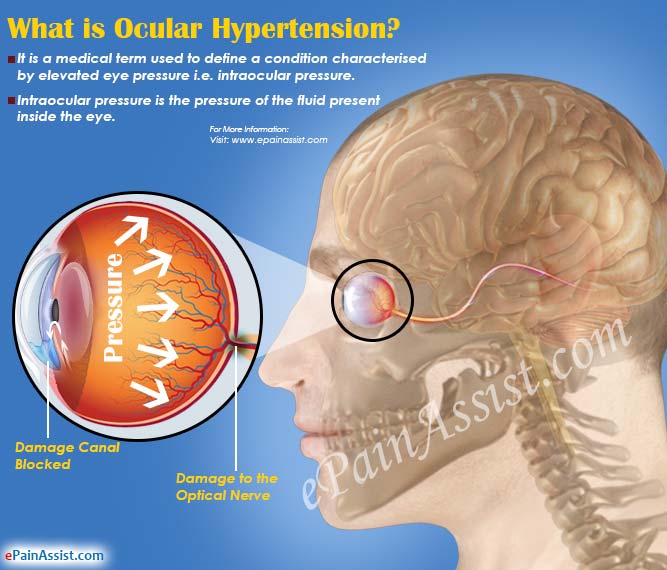
What is Ocular Hypertension?
Elevated ocular pressure is generally noted in presence of ophthalmic issues and glaucoma. However, if the pressure appears elevated in the absence of eye disorders, it is termed as ocular hypertension. Individuals diagnosed with ocular hypertension are categorized as a “glaucoma suspect” and have to be monitored routinely for onset of symptoms.
Ocular hypertension is generally confirmed if the following parameters are positive:
- Intraocular pressure above 21 mm Hg in one or both eyes, in two or more consecutive visits.
- No abnormalities in the optic nerves.
- No evidence of glaucoma or visual loss noted on visual field testing.
- Anatomically normal open angles on Gonioscopic examination.
- Absence of any other ocular abnormalities.
Symptoms of Ocular Hypertension
Ocular hypertension does not have any obvious symptoms. It usually goes unnoticed by the patient. It is detected by an ophthalmologist during routine eye examination. Ocular hypertension does not cause any visual changes or other abnormalities and thus goes undetected.
Epidemiology of Ocular Hypertension
Studies have proven that about 3 to 6 million of the population including 4.5 to 9.4 percent of the individuals above 40 years in the United States of America have ocular hypertension. Post-menopausal women are more prone to ocular hypertension than other women. Men who have ocular hypertension are at a higher risk for developing glaucoma. Also, the incidence of ocular glaucoma is more among African-American than other races.
Prognosis of Ocular Hypertension
Ocular hypertension, if left untreated can lead to glaucoma and other complications. The risk of glaucoma increases with higher intraocular pressure and lower central corneal thickness.
Causes of Ocular Hypertension
- Ocular Hypertension Caused Due to Excessive Aqueous Production: The aqueous humor is a clear fluid that is produced by a structure behind the iris called the ciliary body. The aqueous humor flows through the iris and fills the space between the cornea and the iris. Increased production of the aqueous humor by the ciliary body causes ocular hypertension.
- Ocular Hypertension as a Result of Inadequate Drainage of Aqueous Humor: Inadequate drainage of the aqueous humor from the eyes can lead to disruption of the normal production and drainage of fluids in eyes. This in turn can increase the eye pressure.
- Ocular Hypertension Caused Due to Side Effects of Medications: Certain medications such as steroids that are prescribed for asthma and post LASIK and refractive surgeries can elevate the eye pressure leading to ocular hypertension.
- Ocular Hypertension Caused Due to Trauma and Injuries: Injuries and trauma to the eyes can lead to imbalance in production and drainage of eye fluids causing ocular hypertension.
- Eye Disorder as a Cause of Ocular Hypertension: Ocular hypertension is more common in individuals with eye conditions such as pigment dispersion syndrome, corneal arcus and pseudoexfoliation syndrome.
Risk Factors of Ocular Hypertension
Ocular hypertension is more common among individuals with a family history of glaucoma and in presence of personal history of short sightedness and diabetes. Possible risk factors include:
- Past eye surgeries or illness
- Prolonged use of certain medications
- Ageing
- African-American descent
- Genetic inheritance
- Family history glaucoma
- Myopia/near-sightedness
- Underlying systemic disorders such as cardiac disease, migraine, diabetes, elevated blood pressure, vascular disorders.
- Lifestyle induced factors such as obesity, alcohol consumption, smoking, stress and anxiety.
Complications in Ocular Hypertension
Ocular hypertension can damage the optic nerve gradually. This leads to a condition called glaucoma. The optic nerve transmits images to the brain. If the damage to the optic nerve continues, it can lead to vision changes and even permanent blindness. The most common type of glaucoma caused by ocular hypertension is the open-angle glaucoma. Here the structure of the eye remains normal, but there is abnormal flow of fluid in the eye.
Diagnosis of Ocular Hypertension
Ocular hypertension is usually detected during a regular visit to an ophthalmologist. A wide series of eye tests and examination is carried out for further evaluation and management. This includes:
- Tonometry to Diagnose Ocular Hypertension: This test is done to measure the pressure in eyes. It is done with an instrument called tonometer.
- Gonioscopy Helps to Diagnose Ocular Hypertension: This helps is assessing the drainage angle of the eyes. This is done by using a mirrored lens.
- Ophthalmoscopy to Identify Ocular Hypertension: An ophthalmoscope is used to inspect and detect optic nerve damages.
- Visual Field Test for Diagnosing Ocular Hypertension: This study helps in detecting blank spots in the visual field. A bowl shaped instrument called the perimeter is used to carry out this test.
- Pachymetry to Diagnose Ocular Hypertension: A probe called pachymeter is used to measure the thickness of the cornea.
- Other Tests to Diagnose Ocular Hypertension: Such as split lamp test.
Treatment of Ocular Hypertension
Once diagnosed, it is important to monitor the condition closely to prevent further complications such as loss of vision or damage to the optic nerve. It is also very important to educate the patient about possibility of progression to glaucoma. A visual field test should be done on a regular basis to determine the ideal intraocular pressure of the individual. It is advised to maintain the patient at his or her ideal intraocular pressure. Intraocular pressure lowering medications such as Pilocarpine, Timolol, Acetazolamide and Clonidine is prescribed. In advanced cases, surgical therapy and laser therapy (selective laser trabeculoplasty) may be considered. Referral to a glaucoma specialist or neuro-ophthalmologist is recommended. The patient is asked to follow up on a regular basis for lifetime to avoid glaucoma related damage to the eye.
Prevention of Ocular Hypertension
It is difficult to prevent ocular hypertension; however, regular eye examination can help in early detection and prevent further complications.
Conclusion
Ocular hypertension is a condition characterized by increase in intraocular pressure above 21 mmHg. This condition does not present itself with particular symptoms and thus usually goes unnoticed by the patient. It is usually detected during a regular eye examination visit. Ocular hypertension if left untreated can cause complications such as glaucoma, optic nerve damage and visual loss. The condition is usually treated with medication that lowers the eye pressure. In certain cases, surgical intervention may be required. Once detected, it is advised to visit an ophthalmologist on a regular basis to avoid complications in future.
- American Academy of Ophthalmology. “Ocular Hypertension: When the Pressure in Your Eyes Is Too High.” https://www.aao.org/eye-health/diseases/ocular-hypertension
- Mayo Clinic. “Ocular Hypertension.” https://www.mayoclinic.org/diseases-conditions/ocular-hypertension/symptoms-causes/syc-20375787
- Glaucoma Research Foundation. “Ocular Hypertension.” https://www.glaucoma.org/glaucoma/ocular-hypertension.php
