Cellulitis is a common infection of the skin, dermis, and subcutaneous tissue.1 The skin is divided into two layers. The outer layer is known as the epidermis, and the inner layer is known as the dermis. Skin lies over the subcutaneous tissue. The epidermis is formed by layers of epithelial cells and the overlying layer of keratin that covers the top layer of epithelial cells. The dermis contains connective tissue, sweat glands, and hair follicles. Subcutaneous tissue is formed by connective and areolar tissue.
Branches of arteries, veins, lymphatics, and nerves spread within the subcutaneous tissue. Cellulitis rapidly spreads through the dermis and subcutaneous tissue. Cellulitis is more often observed in foot and hands. Cellulitis around face and orbit is less common but can cause life-threatening complications if not treated. Occasionally cellulitis is also seen over the chest wall, abdomen and back. Cellulitis is rarely bilateral.
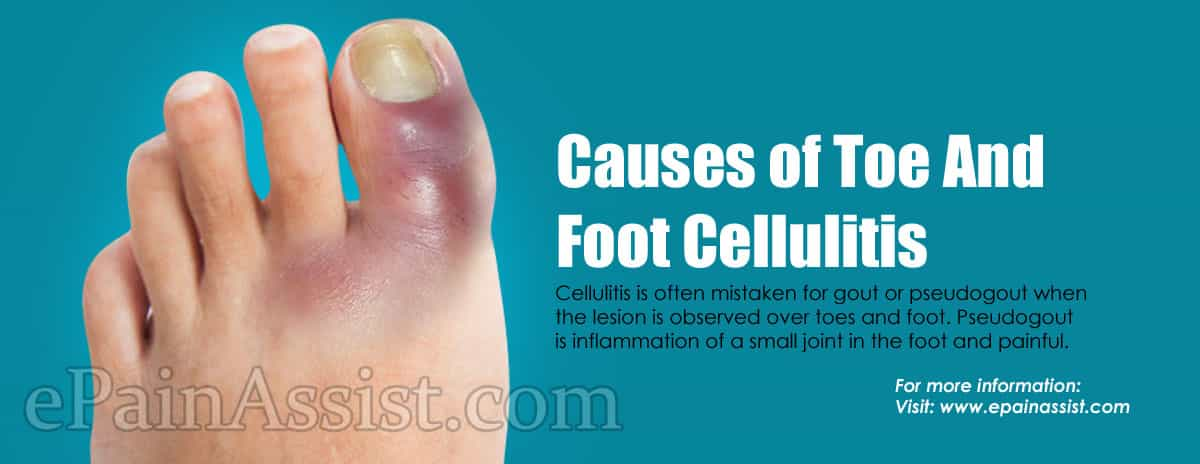
Cellulitis is often mistaken for gout or pseudogout when the lesion is observed over toes and foot. Pseudogout is inflammation of a small joint in the foot and painful. The skin that lies over the toe and foot following infection resulting in cellulitis shows signs of inflammation that is similar to pseudogout. Most cellulitis infection of toe and foot is caused by group A beta-hemolytic streptococcus (i.e., Streptococcus pyogenes).2 Similarly, few cases are also caused by staphylococcus bacteria. In the United States, over 14 million cases of cellulitis are treated annually. It accounts for approximately 3.7 billion dollars in ambulatory care costs.
Causes of Toe And Foot Cellulitis
- Trauma-
- Blunt trauma-
Blunt trauma of toe and foot follows tripping while walking or fall on slippery ground. Excessive twist and turn of joint in toe and foot causes contusion and microscopic tear of ligament or tendon. In a few cases, blunt trauma may cause non-displace or hairline fracture. Lacerated or injured ligament and tendon cause bleeding from torn blood vessels. The clotted blood in few cases causes infection of ligament and tendon. Such infection spreads into subcutaneous tissue that results in cellulitis.
- Penetrating Injury-
Penetrating injury is caused by a sharp object. Stepping on a broken piece of glass or sharp objects like nail causes penetrating trauma. Penetrating injury of foot and toe is also observed following work and car accidents. The contaminated object or poor wound care causes infection of penetrated deep soft tissue. The disease spreads into subcutaneous tissue and causes cellulitis.
Nailbed Infection-
Most nailbed infections are fungal infections. Occasionally the fungal infection is also associated with bacterial infection and results in cellulitis.
Sweat Gland Infection3–
Sweat gland infection is common in axilla and scalp but occasionally also observed over the dorsal surface of foot and toe. Sweat gland infection is often caused by staphylococcus and streptococcus bacteria.
Hair Follicle Infection-
Infection of hair follicle is known as folliculitis. Folliculitis is frequently caused by Staphylococcus aureus and pseudomonas bacteria.
Surgical Incision-
Surgical infection rarely gets infected, resulting in cellulitis when the infection spreads in surrounding skin and subcutaneous tissue. Most surgical incisions get infected when the proper protocol of wound care is not followed.
Intravenous Puncture Site-
An intravenous puncture site gets infected when a contaminated needle is used. The infection spreads in surrounding soft tissue.
Animal Bite-
Animal bite gets infected if animal saliva contains bacteria that passes into the skin and subcutaneous tissue following a bite. Inappropriate would care often causes infection. Infection, if ignored, then spreads from the injured site to surrounding tissue as cellulitis.
Mosquito Bite-
Mosquito bite causes irritation of skin. Chronic irritation results in scratching. Frequent scratching causes superficial wound that rarely gets infected and causes cellulitis.
Symptoms Caused by Cellulitis of Foot and Toe
Infection of a wound, hair follicle, and sweat gland rapidly spreads through the individuals suffering from chronic systemic diseases that are considered as high risk for developing cellulitis. Symptoms are generalized and local. Local symptoms are specific and spread over toe as well as foot.
- History of Risk Factors4–
The examination of a patient suffering from cellulitis must include a history of symptoms and risk factors. The following risk factors are occasionally observed in patients suffering from cellulitis of foot and toes.4
- Diabetes- High blood sugar promotes bacterial growth in soft tissue.
- Skin Laceration Or Wound- Injury of toe and foot introduces external bacteria in the soft tissue of dermis and subcutaneous tissue resulting in infection and cellulitis.
- Peripheral Vascular Disease- Peripheral vascular disease slows the blood return from toe and foot. The stagnant blood flow in individuals suffering from peripheral vascular disease occasionally results in squeezing of serous fluid out of blood vessels. In such cases, bacteria when mix in a serous fluid are transmitted in peripheral tissue resulting in infection and cellulitis.
- Lymphedema- Lymphedema is caused when lymphatic vessels are blocked, or lymph node is atrophied or necrosed. Such condition is observed following surgical removal of the lymph node as well as following radiation therapy that causes scarring of lymph vessels and lymph nodes.
Generalized Symptoms Associated With Cellulitis of Toe and Foot-
- Fever
- Body aches
- Generalized weakness and fatigue
Specific Symptoms of Cellulitis of Toe and Foot
- Pain
- Warm skin to touch
- Edema or swelling
- Tenderness
Signs of Cellulitis Over Foot and Toe-
- Warm skin
- Tenderness
- Purulent discharge
- Signs of injury
- Skin laceration
- Skin incision
- Surgical incision
- Venepuncture
- Insect bite
- Animal bite
Investigations to Diagnose Cellulitis Of Toe And Foot
The infection causes an increase of white blood cells as well as an increase in the erythrocyte sedimentation rate.
- Blood Examination
- White blood cell count- increase
- Erythrocyte sedimentation rate- increase
- X-Ray Toe And Foot- No fracture or dislocation.
- MRI of Toe And Foot Ligament and tendon tear can be observed in MRI films when an image is targeted over soft tissue. MRI may show fluid collection if cellulitis has caused an abscess.
- Ultrasound Examination Of Toe And Foot- Ultrasound images show fluid collection and soft tissue edema. The examination helps to diagnose cellulitis resulting in abscess formation as well as diagnosed lymphedema.
- Bone Scan of Toe And Foot- A bone scan helps to rule our fracture, osteoporosis, and dislocation that may be associated with cellulitis.
Treatment of Toe and Foot Cellulitis
Hygiene-
Cover toe and foot by a clean dressing or socks. Change the dressing every day once or twice. Wash the foot gently with soap and water at least twice a day, if you don’t see any open wound or discharge of pus.
Foot Abscess-
Consult your primary care physician or wound care physician. You may need dressing change every day or alternate day. The open wound dressing needs sterile cotton gauge to cover would, in a few cases, an antibiotic ointment used to covers the skin over cellulitis.
Foot Elevation-
Keep the foot elevated if the pain is moderate to severe during day time.
Cold Therapy-
Cover toe and foot with a wet damp cloth. Avoid ice-cold water to damp the cloth.
Fever-
Fever is treated with Tylenol. Tylenol dosage recommended for an adult is 350 to 750 mg every 8 hours as long as fever is above 98.50 F. Higher dosage of Tylenol is used if fever is not responding to lower dosage. The maximum single dose recommended is not more than 1000 mg. Consult a pediatrician if cellulitis in children is causing fever. In children, the Tylenol dosage prescribed depends on the weight of the child. Tylenol is sold over the counter in most of the pharmacies in the USA.
Pain and Inflammation-
Inflammation of surrounding and infected tissue causes mild to severe pain. Pain is treated with non-steroidal anti-inflammatory drugs, also known as NSAID. Most frequently, pain caused by cellulitis is treated with Motrin or naproxen.
- Motrin-The dosage of Motrin in an adult is 200 to 600 mg of Motrin every 8 hours. Motrin is also known as Ibuprofen.
- Naproxen- The dosage of naproxen suggested is 220 mg every 6 to 8 hours. Naproxen is also known as Aleve. Aleve and Motrin are sold on shelves in all pharmacies in the USA.
Infection
- Antibiotics
The individual suffering from cellulitis of foot and toe is advised to consider the bacterial culture and antibiotic sensitivity test. Such a lab test is recommended when the infection is not responding to prescribed antibiotics or cellulitis is associated with abscess. In the lab, blood is drawn and sent to a lab to culture bacteria. The cultured bacteria is then treated with several antibiotics. The test indicates which antibiotics eliminate bacterial growth. In most cases, more than one medicine is effective. Then, the recommended antibiotics are prescribed an intravenous or oral route.
Following antibiotics are frequently used to treat cellulitis caused by streptococcus and staphylococcus bacteria:
- Amoxicillin (Augmentin)
- Ampicillin,
- Azithromycin,
- Cefazolin,
- Cephalexin (Keflex),
- Ciprofloxacin (Cipro)
- Erythromycin (Erythrocin)
- Penicillins and
- Vancomycin
The published article suggests cellulitis caused by Enterococci, Staphylococcus aureus, and Pseudomonas aeruginosa was treated with Ciprofloxacin, and results were favorable.5 Ciprofloxacin and clindamycin is most often used to cellulitis.6,7
- Antifungal Medication
Bacterial infection of toe and foot is frequently associated with fungal infection. A lab study confirms the fungal infection.
Fungal infection associated with cellulitis of toe and foot is treated with the following anti-fungal infection-
- Amorolfine,
- Clotrimazole
- Econazole
- Ketoconazole
- Miconazole and
- Tioconazole
Physical Therapy
Physical therapy is advised when toe and foot become stiff because of prolonged immobilization of foot and toe. In most cases, ligaments and tendon become stiff when great toe and foot is not moved for several days. Physical therapy is advised when the pain is tolerable or disappears. Loss of pain suggests infection is cured and inflammation has reduced. Physical therapy is performed 3 times a week. Physical therapy for toe and foot stiffness caused by cellulitis includes:-
- Stretching of toe and foot joint
- Heat therapy and
- Ultrasound therapy.
- Cellulitis Brandon D. Brown; Kristen L. Hood Watson., Last Update: November 23, 2019. https://www.ncbi.nlm.nih.gov/books/NBK549770/
- Infectious Diseases Society of America. Clinical practice guidelines by the infectious diseases society of America for the treatment of methicillin-resistant Staphylococcus aureus infections in adults and children. Liu C, Bayer A, Cosgrove SE, Daum RS, Fridkin SK, Gorwitz RJ, Kaplan SL, Karchmer AW, Levine DP, Murray BE, J Rybak M, Talan DA, Chambers HF., Clin. Infect. Dis. 2011 Feb 01;52(3):e18-55.
- Pathogenesis, clinical features, and management of hidradenitis suppurative. Ann R Coll Surg Engl 1997; 79: 83-89 REVIEW R W Parks FRCS Surgical Registrar T G Parks MCh FRCS Professor of Surgical Science Department of Surgery, The Queen’s University of Belfast
- Risk factors for nonpurulent leg cellulitis: a systematic review and meta-analysis. Quirke M, Ayoub F, McCabe A, Boland F, Smith B, O’Sullivan R, Wakai A. Br. J. Dermatol. 2017 Aug;177(2):382-394.
- Treatment of skin and soft tissue infections with oral ciprofloxacin. Fass RJ, J Antimicrob Chemother.. 1986 Nov;18 Suppl D:153-7.
- J Antimicrob Chemother.. 1986 Nov;18 Suppl D:159-64. Ciprofloxacin for soft tissue infections. Wood MJ, Logan MN..
- Oral ciprofloxacin for treatment of infection following nail puncture wounds of the foot. Clin Infect Dis.. 1995 Jul;21(1):194-5., Raz R1, Miron D.
Also Read:
