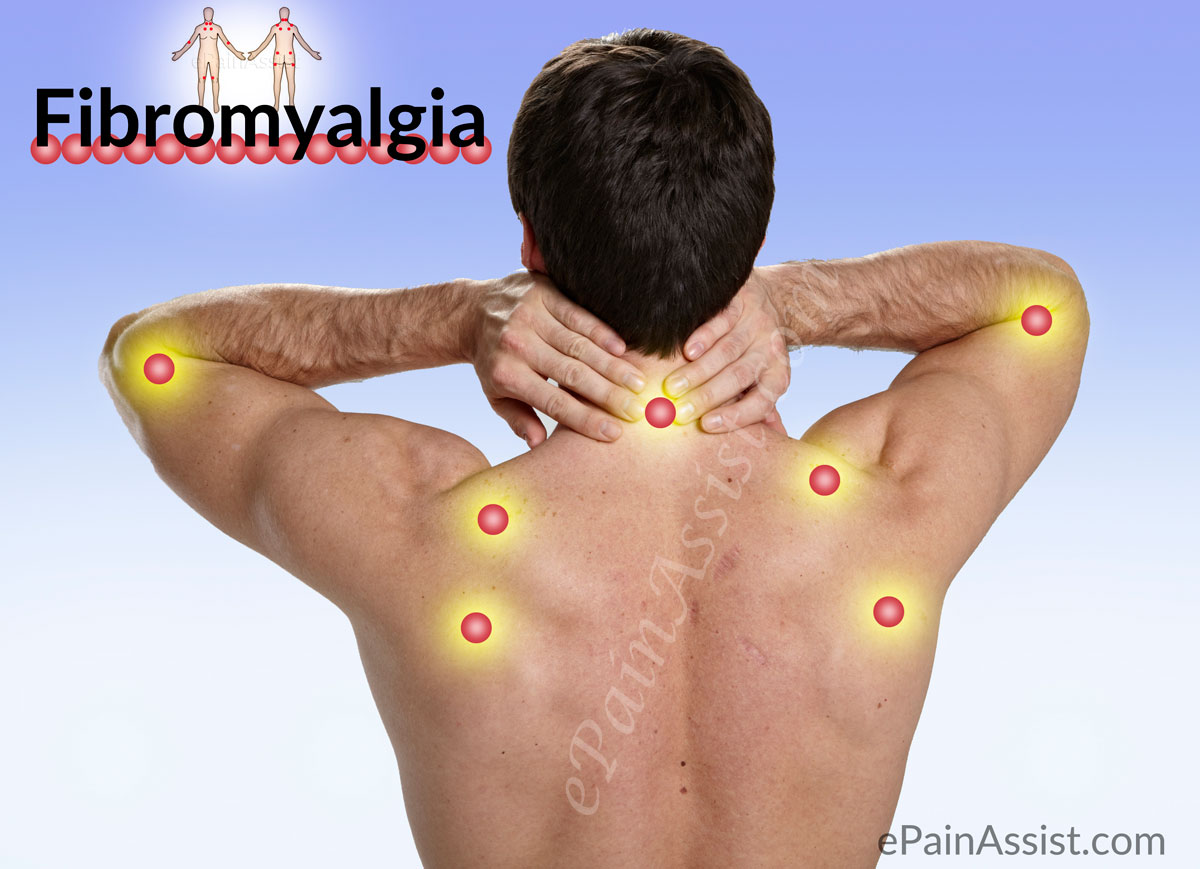
What is Fibromyalgia (FM or FMS)?
Fibromyalgia is a chronic somatic disease of muscles, tendons, ligaments and joints.1 Pain observed is widespread and localized over muscle mass of the trunk, arms and legs. Pain is described as allodynia and may not respond to pain medications. Fibromyalgia is a common musculoskeletal pain syndrome associated with few other symptoms such as fatigue, sleep disturbance, joint pain and stress.2 Cognitive symptoms may be depression or anxiety. Tingling, numbness, and weakness in extremities are other associated symptoms. Joint stiffness, difficulties in swallowing, bowel and bladder abnormalities are occasional symptoms found in 1/3rd of patients. Activities are voluntarily restricted since movements can increase the severity of pain. Co-morbid pain condition with feeling of invalidation and isolation among women is one of the common symptoms of fibromyalgia.
Fibromyalgia is a word that comes from Latin and Greek language expressing pain of muscles and fibrous tissues (tendons and ligaments). Fibromyalgia is expressed as disease of fibro-, meaning “fibrous tissues” in Greek and Algos means “pain” in Greek language. Fibromyalgia is an established diagnosis of diseased muscle and central nervous system. National Institute of Health and American College of Rheumatology has identified the disease code. It is yet a very difficult disease to diagnose and treat. Fibromyalgia is also a symptom commonly adopted by drug seeking patients.
Epidemiology of Fibromyalgia (FM or FMS)
Common in females between age 20 and 50. Fibromyalgia is also seen among elderly and younger female patients. Chronic wide spread pain is rarely observed in children. Diagnosis of fibromyalgia in pediatric patients is often difficult to diagnose because of difficulties to get a detailed history of pain and tender points. In Sweden and Britain 1% of the population is affected by fibromyalgia.
In the United States, approximately 4% of the population has fibromyalgia. Fibromyalgia syndrome (FMS) affects approximately 3 million to 8 million Americans.
Fibromyalgia is third most common musculoskeletal disease after low back pain and osteoarthritis. Prevalence rates of 7.3% to 12.9% were observed in general population across different countries. Prevalence of general population was reported to be up to 15.7%. Up to 65% of patients with Systemic Lupus Erythematosus meet the criteria for fibromyalgia. FM is considered a member of the family of functional somatic syndromes. A high prevalence of FM was demonstrated among relatives of patients with FM and it may be attributed to genetic and environmental factors. The most recent estimates from the United States suggest that FM affects about 5% of all women, In a more recent study from Europe, the estimated overall prevalence of FM was 4.7% for chronic widespread pain, and was 2.9% when stronger pain and fatigue criteria were simultaneously used. Fibromyalgia is seen more often in females than males, with a ratio of 9:1 by ACR criteria. It is most commonly diagnosed in individuals between the ages of 20 and 50, though onset can occur in childhood.
Pathophysiology of Fibromyalgia (FM or FMS)
Advanced studies such as MRI, PET scan of the patients diagnosed of fibromyalgia have shown abnormal structural changes in brain. Research has not concluded if the change observed in brain is secondary to fibromyalgia or fibromyalgia is a disease secondary to abnormal structural changes in central nervous system. Some studies have concluded childhood stress or prolong severe physical strain may have cause a change in brain and neuroendocrine secretions in central nervous system leading to fibromyalgia.
Alteration of biological signals at neuro-receptors and within synapsis of spinal cord triggers multiple pain syndromes in trunk and limb muscles. Genetic research has indicated similarities between depression and fibromyalgia indicating chemical imbalance at neurotransmitter levels. Changes in neurotransmitters and neuroreceptors are triggered by either psychological stress or physical stress. Some studies have suggested that people with fibromyalgia may perceive pain differently than healthy people. Fibromyalgia may involve abnormal neuro-endocrinal activities in the central nervous system that process pain (the nociceptive system). Brain scans of fibromyalgia patients have found abnormalities in pain processing centers. Researchers have detected up to three times normal level of substance P (a chemical messenger associated with increased pain perception) in the cerebrospinal fluid of fibromyalgia patients.
Research and clinical studies do indicate it is a disease caused by abnormal function of neurotransmitter and receptors in central and peripheral nervous systems. Fibromyalgia is a disease, which involves somatic syndrome with a strong psychological and/or emotional component. Research has not concluded if the change observed in brain is secondary to fibromyalgia or fibromyalgia is a disease secondary to abnormal structural changes in central nervous system. Some studies have concluded childhood stress or prolong severe physical strain may have caused a change in brain and neuroendocrine secretions in central nervous system leading to fibromyalgia.
Causes and Risk Factors of Fibromyalgia (FM or FMS)
Etiology of fibromyalgia is not distinctly described through clinical research or through lab studies. Causes of fibromyalgia may be related to biologic, genetic, and environmental factors.
- Gender – Most common among women.3
- Chronic Smoker.
- Education – High school or less.
- Physical activities – Restricted.
- Social Interaction -Insufficient, recent immigrant.
- Family Income – Unsatisfactory.
- Depression Associated Disorder.
- Anxiety Associated Disorder.
- Stress – Emotional.
- Stress – Physical, labor-intensive work.
- Sleep Deprivation.
- Marital Status – Widowed, separated or divorced.
- Infection – Viral infection.
- Hypothyroidism.
- Lyme Disease.
- Chronic fatigue syndrome.
- Depression.
- Sleep disorders.
- Injury.
Symptoms and Signs of Fibromyalgia (FM or FMS)
Fibromyalgia has symptoms that resemble symptoms of autoimmune diseases such as rheumatoid arthritis and lupus (systemic lupus erythematosus). Autoimmune diseases are diseases in which a defective immune system mistakenly attacks the body’s own healthy tissues producing inflammation and damage. The pain in fibromyalgia; however, does not appear to be due to autoimmune factors, and there is little evidence to support a role for an inflammatory response in fibromyalgia.
Symptoms of Fibromyalgia (FM or FMS)

Chronic Pain – Is mild to severe and characterized as allodynia and hyperalgesia. Pain is localized over several muscles and joints. Joint disease is not found to be a cause of pain. Pain may be localized in areas such as shoulders, arms, neck, lower back, gluteal areas, thighs and legs. Pain is characterized as shooting, burning and deep ache. Body aches and stiffness are most commonly observed during morning. For some patients, pain improves during the day and gets worse at night. Others have pain all day long. Pain may get worse with activity, cold or damp weather, anxiety and stress. Pain is felt as somatic and sympathetic pain with nociceptive and neuropathic characters. Neuropathic pain triggers abnormalities in moods such as depression and anxiety.
Tender Points: Found in the soft tissues and muscles on the back of the neck, shoulders, arms, elbows, forearms, chest, lower back, gluteal areas, hips, shins and knees. The pain then spreads out from these areas to adjacent anatomical areas. Fibromyalgia may be predominant in 20 to 30 % of patients suffering with rheumatoid arthritis and systemic lupus erythematosus.
Sleep Problems: Difficulty to fall asleep. Few patients who fall asleep during initial phase complain of difficulty to fall asleep if they wake up in the middle of the night. Most of the time these patients wake up in two hours. Majority of patients complain that they cannot fall asleep or stay asleep and they feel tired when they wake up.
Chronic Fatigue Syndrome (CFS): Predominantly associated with fatigue and less of pain. Fibromyalgia is predominantly associated with severe pain and less of a fatigue. Fibromyalgia syndrome (FMS) has a significant negative impact on daily functioning and quality of life (QOL). Activities are restricted- Difficulty with climbing stairs (62% of patients), walking 2 blocks (55%), and activities of daily living (35%).
Comorbid Symptoms: Irritable Bowel Syndrome (IBS), functional bowel disturbances, genitourinary symptoms and interstitial cystitis.
Cognitive Dysfunction:
- Depression.
- Anxiety.
- Memory and concentration problems- impaired short term and long-term memory.
- Impaired speed of performance.
- Inability to multi-task.
- Attention span – Diminished.
- Stamina – Reduced ability to exercise.
Neurological Symptoms – Numbness and tingling in hands and feet.
Cardiac Symptoms – Palpitation.
Headache – Tension or migraine headaches.
Signs of Fibromyalgia (FM or FMS)
Tender Points
- Widespread pain with tenderness over 11 to 18 areas lasting for 3 months or longer.
- Tender point may be unilateral or bilateral.
- Predominant area of pain may concentrate at one area such as upper extremity or lower extremity or middle of the body.
- Anatomical region of tender points may change with time.
- Non-synchronizing tender points with each follow up visit.
- Dermatomal distribution depends on anatomical neuroendocrine changes within central and peripheral nervous system causing pain.
- Dermatomal distribution of pain over 18 points includes following anatomical areas.
- Tenderness could be present over anterior (front) or posterior (back) of the neck, shoulders, arms, chest, rib cage, buttocks, lower back, thighs and knees.
Diagnosis of Fibromyalgia (FM or FMS)
- Diagnostic criteria include complaints of pain for more than 3 months and at least at 11 tender points approximately out of 18, bilaterally distributed. The patient must feel pain at 11 or more of these points for fibromyalgia to be considered as diagnosis.
- Similar clinical findings as of rheumatic conditions, myofascial disease, arthritis and osteoporosis.
- Risk factors are helpful in diagnosis of fibromyalgia in association with complaints of pain and tender points.
- Difficult to diagnose since there is no diagnostic lab study specific for the disease.
- Diagnosis depends on examination and history of symptomatology.
Prognosis of Fibromyalgia (FM or FMS)
- Fibromyalgia is not a life threatening disease.
- Disease associated with continuous progressive intense pain may remain for prolonged period of time with intermittent breaks of less severe pain or no pain.
- Most fibromyalgia patients report that their symptoms do not improve over time.
- Clinical study of 332 consecutive new fibromyalgia patients found severity of symptoms such as pain depends on psychological factors like work status, helplessness, education, and coping ability.
Treatment of Fibromyalgia (FM or FMS)
Medications for Fibromyalgia (FM or FMS)
1. Antidepressants- Antidepressants were “associated with improvements in pain, depression, fatigue, sleep disturbances, and health-related quality of life in patients with fibromyalgia syndrome (FMS).
” Drugs that simultaneously increase the amount of two brain nerve transmitters, serotonin and norepinephrine, have been approved to treat fibromyalgia in adults.
These drugs include Elavil, duloxetine (Cymbalta), Prozac, Desyrel (trazodone) and milnacipran (Savella).
2. Antianxiety – Enhances effects of neurotransmitter GABA (gama-aminobutyric acid). GABA receptors are responsible for gate control of chloride channel. Several GABA receptors and subtype of GABA receptors are identified. Benzodiazepam acts specific to these GABA receptors. Benzodiazepam is therapeutically effective in treating anxiety, insomnia, agitation, seizures, muscle spasms and alcohol withdrawal.
3. Antiepileptic – Antiepileptics are GABA agonists. Mechanism of action as an analgesic is not known. Several pharmacological actions were observed such as GABA agonist, interaction with voltage gated calcium channel and it halts the formation of new synapses. Gabapentine (Neurontin) and pregabalin (Lyrica) are very effective in 1/3rd of fibromyalgia and chronic neuropathic pain. Neuropathic pain caused by cancer, HIV, radiation treatment and complex regional pain syndrome is treated with gabapentin.
4. Tramadol – Also known as Ultram, Ultracet, Ryzolt and ConZip in USA, Ralivia in Cananda, is used commonly to treat mild to moderate pain of fibromyalgia, restless leg syndrome and rheumatoid arthritis.
5. Nonsteroidal Anti-inflammatory Drugs (NSAIDs) – NSAIDS are anti-inflammatory medications abbreviated as NSAIDs. NSAIDs are not effective in severe pain and non-inflammatory origin pain. Fibromyalgia only has a limited value. Most common NSAIDs used in fibromyalgia treatment are Celebrex, ibuprofen (Motrin, Advil) and naproxen (Aleve).
6. Muscle Relaxant – Mechanism of action of most of the muscle relaxants is debated and unclear. Muscle relaxants stimulate locus ceruleus in brainstem that leads to increased release of norepinephrine in spinal cord. Norepinephrine inhibits alpha motor neuron leads to relief of spasm in skeletal muscles. Muscle relaxants blocks reuptake of norepinephrine. It is structurally related to tricyclic antidepressants such as an amitriptyline. Muscle relaxants used to treat fibromyalgia are Flexeril, Soma and Skelaxin.
7. Dopamine Antagonist – Dopamine antagonist like pramipexole (Mirapex), ropinirole (Requip) are effective in treating selected cases of fibromyalgia.
8. Opioids – Opioids are considered only after all other medicinal and nonmedicinal therapies have been exhausted. There is no evidence that opioids are of any benefit in fibromyalgia. Opioids are not recommended as they can worsen and enhance mood disorder. Opioid may cause serious side effects like abuse and dependence.
9. Naltrexone – Naltrexone at very low dosage has been found to be effective in reducing fibromyalgia symptoms by more than 30 percent in a small controlled trial.
10. Quercetin– Quercetin is a flavanoid pharmacological active anti-inflammatory natural compound. It is effective in fibromyalgia since it inhibits inflammation and mast cells. It is not approved by DEA (Drug enforcement agency). There is nonscientific paper published of therapeutic use of quercetin and demonstrating pain relief in fibromyalgia patients.
11. Guaifenesin– Also known as Robitussin, Fenesin, Organidin and Humibid is commonly used as cough suppressant. Removes excessive phosphate from the body and thus is effective in the treatment of fibromyalgia.
FDA does not approve Guaifensin for fibromyalgia treatment.
Massage Therapy For Fibromyalgia (FM or FMS)
Massage helps to improve blood supply to muscles as well as relieves muscle spasms. Target tissues may include muscles, tendons, ligaments, fascia, skin, joints, and connective tissues. Massage can be applied with the hands, fingers, elbows, knees, forearm, and feet.
Interventional Pain Treatment for Fibromyalgia (FM or FMS)
Trigger Point Cortisone Injection: Cortisone injection is beneficial in treating fibromyalgia only when pain is extremely severe and is associated with severe muscle spasm which is localized over 2 or 4 tender spots. Wide spread muscle pain over 5 to 6 tender points or more of equal intensity may not respond to trigger point injections.
Cortisone injection has limited value in treating fibromyalgia except to relieve severe pain, which may need hospitalization and I.V. opioid therapy.
Alternative Treatment for Fibromyalgia (FM or FMS)
Biofeedback- Biofeedback is the method of treatment used by physical therapist and psychologist. Biofeedback involves teaching of physiological method to control certain involuntary bodily processes such as heart rate, blood pressure, muscle tension and skin temperature. Information’s are monitor and feedback to patients. Patients are taught to manipulate the reading of these instruments by using involuntary physiological mind to body control.
Monitoring Devices are:
- Electroencephalograph (EEG) measures electrical activities of brain
- Electromyography (EMG) measures skin electrical activities
- Photoplethysmograph – feedback thermomete
- Electrocardiograph EKG) monitors heart rate variability
- Pneumograph monitors respiration rate
- Rheoencephalograph monitors brain blood flow
- Hemoencephalography monitors oxygenated or deoxygenated blood in brain by using infrared imaging technique.
Electroacupuncture for Fibromyalgia (FM or FMS)
It is a modified acupuncture. Electrical current is passed between acupuncture needles. It is different than percutaneous electrical stimulation since the acupuncture needle is placed over acupuncture points. There is no scientific evidence suggesting it is useful in treating fibromyalgia.
Stretching Exercises for Fibromyalgia (FM or FMS)
Stretching is a group exercise or individual exercise. Group of muscles are deliberately stretched out by extension or flexion of joint. After initial stretching exercise for few weeks, hyperextension, flexion, abduction and adduction of these muscles are achieved by joint movements. Goal is to increase flexibility. Yoga is an example of therapeutic stretching. Swimming and aquatic exercises are also beneficial if water temperature is not too cold or warm. Patients with symptoms of fibromyalgia do not tolerate cold water. Warm water can cause tiredness sooner. Tai chi was studied in a small single blinded randomized controlled trial, resulting in a relative benefit ratio of 2.0 on the Fibromyalgia Impact Questionnaire.
Magnet Therapy for Fibromyalgia (FM or FMS)
Principle of treatment is to use static magnetic field created by placement of magnet over certain part of body inducing pain to treat chronic pain. Magnet improves blood flow in underlying tissue. Magnetic field is limited in spread and thus does not cause any long-term harm to hemoglobin or any other blood contents.
Healthy Diet and Herb Therapy for Fibromyalgia (FM or FMS)
Fibromyalgia pain may not respond to conventional treatment. Non-responding disease to conventional medicine may respond by changing daily habits of eating, relaxation, and stress.
Lifestyle Changes for Fibromyalgia (FM or FMS)
- Treatment with herbs
- Spiritual practice
- Healthy eating
- Avoid caffeine
- Practice good sleep
- Adopt cultural traditions.
- Establish treatment as an alternative medicine – homeopathy, ayurvedic medicine, aromatherapy, music therapy, prayer therapy, reflexology, massage therapy, biofeedback, myofascial trigger point therapy and magnet therapy.
Combination Therapy for Fibromyalgia (FM or FMS)
Fibromyalgia is a wide spread pain syndrome. There are no magic pills available to stop pain. Treatment options are multiple as discussed earlier. Combination of some of these treatment modalities may assist to decrease pain and sufferings. Treatment package would include medications and non-pharmacological adjuvant treatment. Most of the institution and expert in treating fibromyalgia advise multi-treatment combination. There is no research supporting multimodal treatment being helpful in controlling or minimizing symptoms of fibromyalgia. Most common combination of treatment is medications, physical therapy and cognitive behavior treatment. Each patient may have combination of pain and muscle spasm with different cognitive symptoms. Thus, combination of treatment cannot be “one for all”; each patient is evaluated and considered for different combination of treatment.
Tests to Diagnose Fibromyalgia (FM or FMS)
- Blood and urine tests.
- Electrodiagnostic testing (EMG).
- Imaging studies e.g. X-Ray, CAT scan and MRI based on the individual indications.
- Blood examination – CBC and electrolytes, blood glucose level.
- Sleep study.
Investigations for Fibromyalgia (FM or FMS)
- Neuroimaging – Hyperactivities were observed in somatosensory cortex, anterior cingulate gyrus, and insular cortex in response to noxious stimulation.
- Blood Supply to Brain – Decreased blood flow in thalamus and pontine nuclei of mid brain.
- Magnetic Resonance Spectroscopy (1H-MRS)- Increased neural activities and decreased brain metabolite ratio in hippocampal centers as well as in motor and cingulate cortex were observed in fibromyalgia. Similar study using 1 H-MRS also indicated increased concentration of the excitatory neurotransmitter amino acid glutamate within the insulate cortex.
- Voxel-Based Morphometry (VBM)– Study indicates loss of grey matter in brain of fibromyalgia patient is 9.5 times the normal rate. Grey matter was also found to be reducing in volume in cingulate cortex, insula and parahippocampal gyrus.
- Positive Emission Tomography- Study has recorded reduced dopamine synthesis in brainstem and limbic cortex. Negative co-relation was observed between severity of pain and dopamine secretion in insular cortex.
Also Read:
- FAQ on Fibromyalgia: Symptoms, 11 Painful Trigger Points, Causes, Risk Factors
- 10 Best Exercises for Fibromyalgia
- Is Fibromyalgia Pain Real?|Are Opioids an Effective Treatment for Fibromyalgia
- Yoga for Fibromyalgia: 4 Best Asanas To Relieve Painful Tender Points
- Can You Get Disability Benefits for Fibromyalgia
Also Watch: