Pain or discomfort in the abdomen, below the level of umbilicus (belly button) is known as lower abdominal pain. Lower abdominal pain is spread below the umbilicus in midline as well as on right and left side. The midline lower abdominal pain is spread between belly button and pubic symphysis. Pubic symphysis is a prominent pelvic bone that lies in lower abdomen close to midline. The pain felt above the pubic symphysis is known as suprapubic pain.
Lower abdominal pain is quite common, particularly in the women. The female reproductive organ lies in lower abdomen and pelvis. The reproductive organs are uterus, vagina, ovaries and fallopian tubes. The pain caused by diseases of these organs are referred to lower abdomen. Thus lower abdominal pain is observed more often in female than male.
9 Most Common Causes of Lower Abdominal Pain
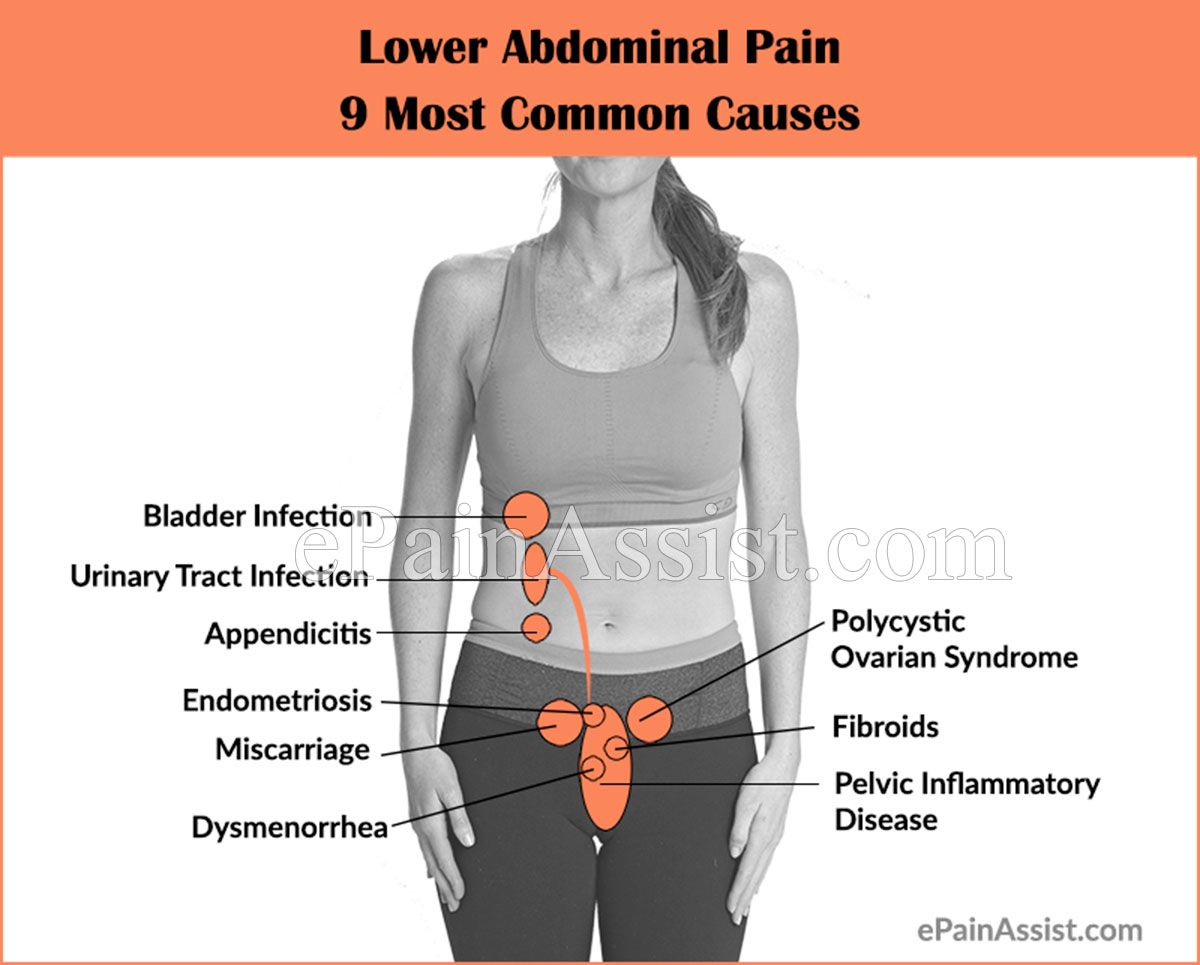
- Appendicitis
- Cystitis (Bladder Infection)
- Pelvic Inflammatory Disease
- Dysmenorrhea (Menstrual Pain/Cramps)
- Miscarriage
- Endometriosis
- Urinary Tract Infection (UTI)
- Fibroids
- Polycystic Ovarian Syndrome
9 Most Common Causes, Symptoms, Investigations and Treatment of Lower Abdominal Pain
Appendicitis. Inflammation of appendix is a painful condition. If initial symptoms are ignored then infected appendix may rupture and spread infection in peritoneal tissue. Appendicitis pain occurs in the lower right abdomen and can radiate to other regions of the abdomen. The abdominal pain can worsen within a span of a few hours.
Symptoms of Appendicitis-
- Right lower abdominal pain
- Nausea
- Vomiting
- Abdominal wall guarding
- Abdominal wall rigidity
- Fever
Pain-Pain is localized over lower right abdominal quadrant. Pain is also referred to area of umbilicus. Pain is burning in character and moderate to severe, when appendix is inflamed and not ruptured. Abdominal pain becomes severe and excruciating with character of burning, throbbing and piercing pain when appendix is ruptured. The area of abdominal pain become wider when appendix is.
Nausea and Vomiting- The symptoms of nausea and vomiting is observed when appendix is ruptured.
Abdominal Wall Guarding- The lower right abdominal muscle contracts when appendix is ruptured. The inflammation and infection spreads from lumen of infected appendix to surrounding peritoneal tissue. Any touch or palpation during examination increases pain and triggers muscle contraction. Such a severe muscle contraction causes contraction of overlying muscle and the condition is known as guarding. Guarding is often wide spread muscle contraction resulting in tight generalized abdominal wall.
Abdominal Wall Rigidity- The contraction of muscle causes tight or rigid right lower abdomen. Abdominal wall guarding is observed when inflamed swollen or ruptured appendix is irritating the overlying peritoneum and abdominal wall. The muscle contraction is often observed when abdominal organ is inflamed and such contraction protect the organs from spreading the infection and also prevents sudden increased pain by guarding the inflamed organ such as appendix. Abdominal wall rigidity is more local and observed over right lower abdomen.
Fever-The infection of appendix causes fever.
Investigations to Diagnose Appendicitis.
Full Blood Count-
White Blood Cell Count (WBC)-Increased WBC count indicates presence of infection.
Erythrocyte Sedimentation Rate (ESR)- The ESR is increased. The blood is collected in a special test tube. The ESR is a time taken by cells in blood to settle at the bottom of the tube. The faster ESR suggest presence of infection and tissue inflammation.
Electrolyte and Urea-In most cases electrolytes and blood urea nitrogen level are normal. Occasionally patient may suffer with severe dehydration and electrolyte abnormalities because of severe nausea and vomiting. In such cases abnormal level of sodium, potassium and blood urea nitrogen is found in blood examination.
C Reactive Protein (CRP)- CRP is increased in patient suffering with most infection such as appendicitis.
Ultrasound Scan- Ultrasound scan images show soft tissue abnormalities. Infected appendix is seen as a swollen finger like organ close to cecum and terminal part of small intestine. Ultrasound image can differentiate ruptured appendix and surrounding issue inflammation.
CT-scan and MRI-Computerized tomography scan (CT-Scan) images and Magnetic resonance images (MRI) show the swelling and abnormalities of appendix.
Laparoscopy- Laparoscopy study involves skin incision and then insertion of tubular camera known as laparoscope in to abdominal cavity. Surgeon then can see the color image of appendix on television. The study is performed in outpatient or hospital surgery room.
Treatment of Appendicitis.
Pain Medications-
- NSAIDs- Motrin, Naproxen or Celebrex
- Opioids-Severe lower abdominal pain due to appendicitis may not respond to NSAIDs. Severe lower abdominal pain is treated with opioids for 7 to 10 days.
- Antibiotics-Bacterial infection resulting in appendicitis is treated with antibiotics.
- Intravenous Fluid-Dehydration and electrolyte abnormalities are treated with saline (sodium chloride) intravenous fluid.
- Surgery-Surgery is performed to remove the inflamed appendix.1
Cystitis (Bladder Infection)
Bacterial infection of urinary bladder is known as cystitis which can cause lower abdominal pain. Cystitis is a non-infectious or infectious condition. Non-infectious cystitis is caused by bladder mucosal trauma and irritation. Bladder mucosal trauma is caused by endoscope during cystoscopy procedure or prostate surgery. Cystitis causes mild to severe suprapubic lower abdominal pain.2
Symptoms of Cystitis.
- Pain and feeling of pressure like symptom in lower abdomen above pubic symphysis.
- Fever
- Burning sensation while passing urine is felt in lower abdomen.
- Increased urinary frequency
- Small amount of urine is passed each time one feels urge of urination
- Blood in urine
- Cloudy urine
Investigations to Diagnose Cystitis-
- Urine examination
- Blood examination
- Cystoscopy
- CT scan and MRI.
Treatment of Cystitis.
- Pain Medication
- NSAIDs
- Tylenol
- Opioids
- Antibiotics are given to treat the infection
- Intravenous fluid
- Heating pad
Pelvic Inflammatory Disease Causing Lower Abdominal Pain
Pelvic inflammatory disease involves infection of female reproductive organs. The pelvic organ infection causes lower abdominal pain. Pelvic inflammation is observed in uterus, fallopian tube and ovaries. Pelvic inflammatory disease in male is caused by inflammation or infection of prostate. Moderate to severe lower abdominal pain is felt above and below pubic symphysis when pain is caused by diseases of uterus and prostate. Lower abdominal pain on left or right side is caused by diseases of ovary and fallopian tube.
Lower abdominal pain caused by diseases of female reproductive is often referred to lower back. Pain intensity is increased during intercourse. Pain is felt during act of urination. Intensity of lower abdominal pain caused by diseases of pelvic organ increases when urinary bladder muscle is contracting to urinate.
Symptoms.
- Pain- Mild to severe lower abdominal pain is felt in midline on the right and left side.
- Fever
- Increased vaginal discharge
- Feeling weakness
- Nausea
Investigations of Pelvic Inflammatory Disease.
- Blood examination
- CT scan or MRI examination
- Pelvic ultrasound 3
- Endometrial biopsy and
- Laparoscopy
Treatment of Pelvic Inflammatory Disease.
- Pain medications
- NSAIDs– Motrin, Naproxen or Celebrex
- Tylenol
- Opioids for severe pain
Antibiotics- Antibiotics are the main line of treatment for lower abdominal pain caused due to pelvic inflammatory disease.
- Surgery
- Excision of pelvic abscess
- Removal of fallopian tube
- Excision of uterus
- Removal of ovaries
- Removal of prostate
Dysmenorrhea (Menstrual Pain/Cramps)
Dysmenorrhea is a cramping pain in the lower abdomen during and before a woman’s monthly period. Dysmenorrhea is caused by increased level of prostaglandin. Prostaglandin increases frequency and force of uterus muscle contraction. Dull and throbbing pain is felt in lower abdomen during menstrual period. Pain often radiates to the lower back and thigh. Fibroid disease of uterus also causes dysmenorrhea during menstruation. Symptoms of dysmenorrhea are often tolerable in individual who are involved in daily exercise and take daily hot water tub bath during menstrual period.
Symptoms of Dysmenorrhea.
- Pain- Pain is mostly spread over lower abdomen and referred to back.
- Abdominal Cramping- Cramping pain is felt in lower abdomen during menstrual periodic.4 Pain is frequently felt as squeezing and stabbing pain.
- Nausea and vomiting
- Feeling tired and fatigue
Investigations to Diagnose Dysmenorrhea.
- Ultrasound
- CT scan
- Magnetic Resonance Imaging (MRI)
- Hysteroscopy and
- Laparoscopy.
Treatment of Dysmenorrhea.
- Analgesics (pain medications)
- NSAIDs such as ibuprofen and naproxen
- Tylenol
- Oral Contraceptive Pills
- Pills are given to prevent ovulation.
- Heating pad
Surgery-
- Excision of uterus fibroid
- Excision of uterus
- Preventive Therapy-
- Regular exercise
- Rest
- Hot tub bath during menstruation
- Miscarriage
Spontaneous pregnancy loss before the 20th week is known as miscarriage and it causes pain in the lower abdomen. Uterus contracts during miscarriage that results in lower abdominal pain.
Symptoms to Diagnose Miscarriage.
- Lower abdominal cramping pain.
- Vaginal spotting or bleeding.
- Amniotic fluid discharge from vagina.
- Investigations to Diagnose Miscarriage.
- Pelvic Exam- Check bleeding from uterus and remove any specimen of miscarriage.
- Ultrasound Examination- Check the presence or absence of any tissue in uterus.
- Hemoglobin- Check level of hemoglobin to evaluate loss of blood.
- Human Chorionic Gonadotropin Hormone (HCGH)- Check the level and pattern of HCGH to confirm diagnosis of pregnancy.
- Biopsy or lab study of discharged tissue.
Treatment of Miscarriage.
- Rest is recommended for threatened miscarriage.
- Pain medications if needed
- Surgery- Patient is considered for dilatation and curettage procedure to remove any remains of incomplete miscarriage.
Endometriosis
Uterus is the major female sex organ. Fetus grows within uterus. The inner mucosal lining of uterus is known as endometrium. Occasionally endometrial mucosa starts growing within uterus and also outside uterus. The spots of endometrium travels through fallopian tube and spills outside fallopian tube over ovaries and pelvic floor.
Endometrial mucosa also lodges over the mucosal layer of fallopian tube. The deposited endometrial mucosa starts growing in size during menstrual cycle. Such condition is then known as endometriosis. Endometriosis involves ovary, fallopian tube and floor of pelvis. Endometrial tissue causing endometriosis is found over appendix and colon.5
Symptoms of Endometriosis.
- Pain- Severe lower abdominal pain is felt during menstrual period.
- Dysmenorrhea– Dysmenorrhea is a cramping pain in the pelvis that may refer to lower back and abdomen.
- Dyspareunia– Intolerable pain is felt during intercourse.
- Lower Abdominal Pain- Increased lower abdominal pain is felt during urination and defecation,
- Heavy menstrual periods
- Infertility.
Investigations to Diagnose Endometriosis-
- Pelvic exam
- Ultrasound
- Laparoscopy.
Treatment of Endometriosis Causing Lower Abdominal Pain.
Analgesics- Analgesic are used to treat lower abdominal pain caused due to endometriosis.
- NSAIDS
- Tylenol
- Opioid
- Hormone therapy also helps in relieving endometriosis pain.
- Surgery
- Excision of Uterus when endometriosis is not responding to medication and not spread to other area.
- Removal of fallopian tube and ovaries
- Urinary Tract Infection (UTI)
Urinary tract infection involves infection of kidney, bladder, ureter and urethra. Urinary Tract Infection causes lower abdominal pain.
Symptoms of Urinary Tract Infection.
- Pain in the lower abdomen and pelvis
- Persistent urge to urinate
- Burning micturition
- Cloudy urine
- Hematuria
- Rectal pain.
Investigations to Diagnose Urinary Tract Infection.
- Complete urine examination (CUE)
- Culture and sensitivity test (C and S)
- CT scan
- Intravenous pyelogram (IVP)
- Cystoscopy.
Treatment of Urinary Tract Infection.
- Pain medication
- Antibiotics- Antibiotics are the first line of treatment. Antibiotics are given as pills and I.V. antibiotics.
- Fibroids
These are the noncancerous growths occurring in the uterus commonly seen during childbearing age in women. Fibroid causes severe lower abdominal pain during menstruation and severe bleeding.
Symptoms Caused By Fibroid.
- Pain or pressure in the pelvis
- Severe menstrual bleeding
- Frequent urination
- Constipation
- Referred pain in the back and legs.
Investigations to Diagnose Uterine Fibroid.
- CBC
- Ultrasound
- Magnetic Resonance Imaging (MRI)
- Hysterosonography
- Hysterosalpingography
- Hysteroscopy.
Treatment to Diagnose Uterine Fibroid.
- Pain
- Hormone Therapy- Treatment comprises of hormonal therapy,
- Uterine artery embolization,
- Surgery-
- Myolysis- removal of fibroid,
- Laparoscopic or robotic myomectomy,6
- Removal of uterus
- Hysteroscopic Myomectomy
- Endometrial ablation of fibroid
- Resection of submucosal fibroids
- Abdominal myomectomy
- Hysterectomy.
Polycystic Ovarian Syndrome
Polycystic Ovarian Syndrome (PCOD) is a hormonal disorder commonly seen in women of childbearing age an can cause sever lower abdominal pain. The disease is associated with prolonged menstrual cycle. One of the reason for prolonged menstrual cycle is physiological increased secretion of male hormone known as androgen. The hormonal imbalance causes increased number of follicles in ovaries and also causes irregular release of eggs from ovaries.
Symptoms of Polycystic Ovarian Syndrome.
- Pelvic pain
- Irregular menses
- Heavy periods
- Excessive facial, male pattern baldness and body hair caused by increased secretion of male hormone (androgen).
Investigations to Diagnose Polycystic Ovarian Syndrome.
- Blood tests
- Pelvic exam
- Pelvic endoscopy
- Pelvic ultrasound.
Treatment of Polycystic Ovarian Syndrome.
Birth Control Pills- Low dose birth control pills are given in order to regulate the cycle.
Hormone Therapy-
- Progestin is prescribed for 2 weeks every 2 months for 6 months. The treatment often helps to regulate the hormonal cycle.
- Antiestrogen therapy- Patient is prescribed pills of clomiphene (cloid). Clomiphene acts as anti-estrogen and helps to decrease symptoms.
- Letrozole (Femara) treatment often helps to relieve the symptoms. Letrozole stimulates ovaries to secrete normal estrogen and progesterone hormone.
- Gonadotropine- Intravenous gonadotropin helps to correct the hormone irregularities.
- Spironolactone (Aldactone)
- Intravenous Fluid- IV fluid is given to correct electrolyte imbalance.
- Surgery
- Excision of ovaries
- Excision of uterus
As you can see, lower abdominal pain is a symptom which indicates other underlying medical conditions. Treatment of lower abdominal pain depends on the cause and condition. We have given some of the common causes for lower abdominal pain with symptoms and treatment. For correct diagnosis and treatment, you have to undergo various investigations and exams by your doctor before arriving at the right diagnosis so that appropriate treatment can be provided.
- Disease burden of appendectomy for appendicitis. a population-based cohort study. de Wijkerslooth EML1, van den Boom AL2, Wijnhoven BPL2., Surg Endosc. 2019 Mar 27.
- Interstitial cystitis. epidemiology, pathophysiology, and clinical presentation. McLennan MT1., Obstet Gynecol Clin North Am. 2014 Sep;41(3).385-95.
- Ultrasound of Pelvic Pain in the Nonpregnant Woman. Patel MD1, Young SW2, Dahiya N2., Radiol Clin North Am. 2019 May;57(3).601-616.
- Menstrual characteristics and prevalence of dysmenorrhea in college going girls. Kural M1, Noor NN1, Pandit D2, Joshi T1, Patil A1., J Family Med Prim Care. 2015 Jul-Sep;4(3).426-31.
- Appendiceal endometriosis invading the sigmoid colon. a rare entity. Lainas P1,2, Dammaro C3,4, Rodda GA3, Morcelet M5, Prevot S4,5, Dagher I3,4., Int J Colorectal Dis. 2019 Jan 21. doi. 10.1007/s00384-019-03242-0. [Epub ahead of print] Massive prolapsed submucous fibroid treated with laparoscopic surgery. A case report.
- Yabumoto K1, Ito F1, Matsushima H1, Mori T1, Kusuki I1, Kitawaki J1., J Obstet Gynaecol Res. 2019 Apr;45(4).942-946.
Also Read:
- What Can Cause Lower Right Abdominal Pain?
- What Can Cause Left Side Abdominal Pain?
- What Can Cause Right Side Abdominal Pain?
- 19 Safe and Natural Home Remedies for Abdominal Pain or Stomach Ache
- Belly Button Pain or Umbilical Pain: What Causes Pain Around Belly Button?
- Diagnosis of Belly Button Pain or Umbilical Pain: Acute Pain, Chronic Pain
- Treatment For Belly Button Pain Caused By 12 Different Medical Conditions
