Portal vein thrombosis (PVT) is the narrowing or blockage of portal vein by a thrombus or blood clot. Portal vein is the blood vessel that carries blood from intestines to liver and a thrombus cuts this blood supply. The most common cause of PVT is cirrhosis. Other causes include hepatocelllular carcinoma, cholangiocarcinoma, gastric carcinoma, pancreatic ductal carcinoma, acute pancreatitis, chronic constrictive pericarditis, chronic heart failure, Budd-Chiari syndrome, polycythemia vera, appendicitis, abdominal surgery, ascending cholangitis, umbilicus (navel) infection in newborns, inflammatory bowel disease, myeloproliferative disorders, oral contraceptive pills, pregnancy and/or trauma.
In most cases, PVT is asymptomatic, but when symptoms are present, they include fever, upper abdominal pain and abdominal swelling, ascites, splenomegaly with the development of portal hypertension and symptoms include esophageal varices and gastric bleeding, fever and chills, vomiting of blood, pain in the liver (in the right upper quadrant), jaundice and tarry, bloody and foul smelling stools.
Diagnosis
The diagnosis of portal vein thrombosis is done with the help of medical history and a combination of signs and symptoms of enlarged spleen, hematemesis, variceal bleeding and liver infections. Liver function tests are done to check the functionality of liver, but in PVT they are generally normal. Imaging including ultrasound, CT scan, MRI, and angiography is done for the definitive diagnosis of portal vein thrombosis. In most cases, the PVT is diagnosed incidentally on imaging.
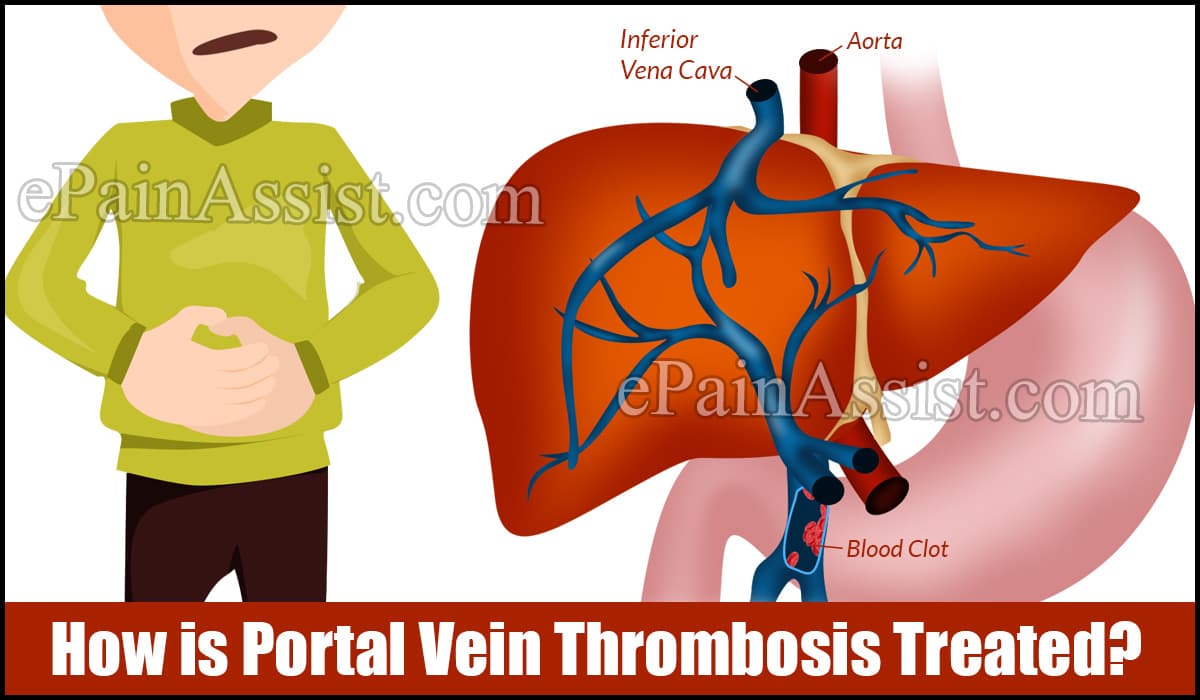
How is Portal Vein Thrombosis Treated?
The primary goal of portal vein thrombosis or PVT treatment consists of resolving the symptoms, prevention of thrombus growth and prevention and treatment of mesenteric ischemia. The treatment for portal vein thrombosis ranges from observation with no active therapy to conservative therapy with anticoagulants and/or thrombolytic therapy to surgical intervention in the form of thrombectomy and placement of transjugular intrahepatic portosystemic shunt (TIPS). The treatment and results of acute portal vein thrombosis depends on factors such as involvement of remaining splanchnic circulation, liver cirrhosis and/or presence of tumor.
Generally, a multidisciplinary approach with the involvement of vascular medicine (thrombosis specialist), gastroenterologist, interventional radiologist and colorectal surgeon is needed for optimal treatment guidance and options. Management of portal vein thrombosis is a complicated decision making since it requires consideration of various factors including involvement of other splanchnic veins, hypercoagulable states, presence or absence of infections, inflammatory disorders, bleeding risk due to presence of varices or decreased platelet count, cirrhosis and/or active malignancy.
Acute portal vein thrombosis with no cirrhosis or malignancy, but symptomatic, is treated with anticoagulation therapy such as warfarin or low molecular weight heparin. For asymptomatic PVT involving mesenteric veins, hypercoagulable states, non-reversible risk factors and increase in thrombus burden anticoagulation therapy is considered. However, with reversible risk factors (pancreatitis and abdominal infections), the patient is monitored conservatively without any anticoagulation therapy. Thrombolytic therapy and/or thrombectomy can also be considered where there is a risk of thrombus extension and worsening pain while on anticoagulation therapy.
Patients with liver cirrhosis have a higher risk of developing portal vein thrombosis and most of the times these patients are asymptomatic and are accidentally diagnosed. PVT also worsens liver function and increases the mortality and morbidity of patients with cirrhosis; it also negatively affects liver transplant. The treatment of cirrhotic patients with PVT requires consideration of various factors such as thrombosis acuity, bleeding risk factors, presence of any inherited coagulopathy, candidature for transplant and/or any other co-morbidities. Keeping all these factors in mind, anticoagulation therapy with low molecular weight heparin is started. TIPS (transjugular intrahepatic portosystemic shunt) surgery is considered as a useful adjunct in patients with occlusive PVT and worsening portal hypertension and esophageal varices; however, the pros and cons are thoroughly studied and when the pros outweigh cons, then the surgery is proceeded with.
In cases of acute portal vein thrombosis along with malignancy, the patient is preferably treated with low molecular weight heparin except for cases of active bleeding, severe bleeding risk and/or minimal thrombus burden.
The patients with acute variceal bleeding are treated with variceal banding or sclerotherapy. The bleeding can also be controlled with octreotide medication too. Liver transplant can also be considered in cases of cirrhosis.
Also Read:
