Is Portal Vein Thrombosis Life Threatening?
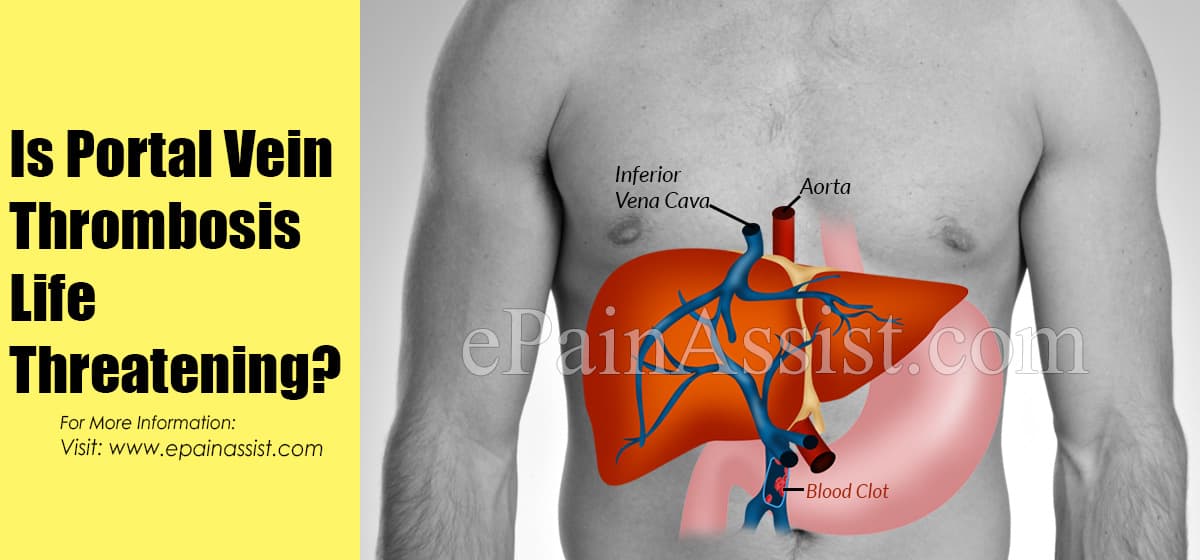
Portal vein thrombosis (PVT) is the narrowing or blockage of portal vein by a thrombus or blood clot. Portal vein is the blood vessel that carries blood from intestines to liver and a thrombus cuts this blood supply. In most cases, the portal vein thrombosis is a treatable condition, but in cases of acute thrombosis, it can become life threatening and might lead to intestinal ischemia and/or infarction that require immediate treatment.
Portal vein thrombosis can be caused due to either reduced flow of blood or portal hypertension, endothelial disturbance or hypercoagulable state. The most common cause of PVT is cirrhosis and about 1/4 patients with cirrhosis have a tendency to develop thrombosis due to severe scarring of liver. Other causes include hepatocelllular carcinoma, cholangiocarcinoma, gastric carcinoma, pancreatic ductal carcinoma, acute pancreatitis, chronic constrictive pericarditis, chronic heart failure, Budd-Chiari syndrome, polycythemia vera, appendicitis, abdominal surgery, ascending cholangitis, umbilicus (navel) infection in newborns, antiphospholipid syndrome, dehydration, inflammatory bowel disease, myeloproliferative disorders, oral contraceptive pills, pregnancy and/or trauma.
Symptoms of Portal Vein Thrombosis
Portal vein thrombosis is the most common cause of portal hypertension. A portal vein thrombus can be either a bland thrombus or a tumor (malignant) thrombus. Most of the times, PVT is asymptomatic and in minor thrombus will present with symptoms of fever, upper abdominal pain, and abdominal swelling due to excessive abdominal fluid accumulation. In severe clots, there might be splenomegaly with the development of portal hypertension and symptoms include esophageal varices and gastric bleeding, fever, and chills, vomiting of blood, pain in the liver (in the right upper quadrant), jaundice and tarry, bloody and foul smelling stools.
Diagnosis of Portal Vein Thrombosis
The diagnosis of portal vein thrombosis is done with the help of medical history and a combination of signs and symptoms of enlarged spleen, hematemesis, variceal bleeding and liver infections. Liver function tests are done to check the functionality of liver, but in PVT they are generally normal. Imaging including ultrasound, CT scan, MRI and angiography is done for the definite diagnosis of portal vein thrombosis.
Doppler ultrasound uses sound waves for the detection of blood flow within the vessels and can be used to diagnose portal vein thrombosis and its severity. In cases of PVT, it shows reduced/absent blood flow through portal veins.
CT scan uses X-rays for demarcation of bones and blood vessels and a dye is injected in veins for the identification of blood clots.
MRI of abdomen uses magnets and radio waves, which is used for the identification of blood flow and circulation irregularity, masses in various abdominal organs and abdominal swelling.
Angiography is an invasive test that uses X-rays and injection of a special dye for the production of images of blood flow/circulation within a vein or an artery and for the identification of blood clots.
Treatment of Portal Vein Thrombosis
The treatment of portal vein thrombosis depends on the primary cause of it and aims at dissolving the clot or prevention of gradual thrombus growth over time. The clot is dissolved through thrombolysis with the help of plasminogen activator and to prevent thrombus growth or recurrence, anticoagulants such as heparin are used.
In cases of umbilicus infection or appendicitis, antibiotics are used to clear the infection and PVT too.
The treatment is also aimed at lowering the symptoms of portal vein pressure and prevention of esophageal varicose bleed. Antihypertensives such as beta-blockers and nitrates are used to reduce portal vein pressure; octreotide is used to reduce the blood flow to the liver, thus reducing pressure in the portal vein. The reduced blood pressure in the portal vein also reduces the chance of esophageal varicose bleeding. Banding of esophageal varicose veins is also undertaken to prevent bleeding of variceal veins. Shunt surgery is used as a last resort for the prevention of excess bleeding and pressure reduction in veins. Some cases of the liver damage might also require liver transplant.
Also Read:
