Does MRSA Spread Quickly?
MRSA which stand for Methicillin resistant Staphylococcus aureus, is a gram positive bacteria, is that causes various infections in humans. These methicillin resistant Staphylococcus aureus are difficult to treat. The usual presentation of infection with these bacteria’s depending on organ involved. Usually it causes Mai infection of skin like boils and sores. But can also cause serious infections like infected surgical scars, septicemia, lung infections and urinary tract infection. Though infections caused by staphylococcus aureus are usually mild, but may be life threatening sometimes. Infections caused by methicillin resistant staphylococcus aureus are difficult to treat because the empirical therapy for staphylococcus aureus is ineffective these bacteria. So, health experts referred to as superbug.(1)
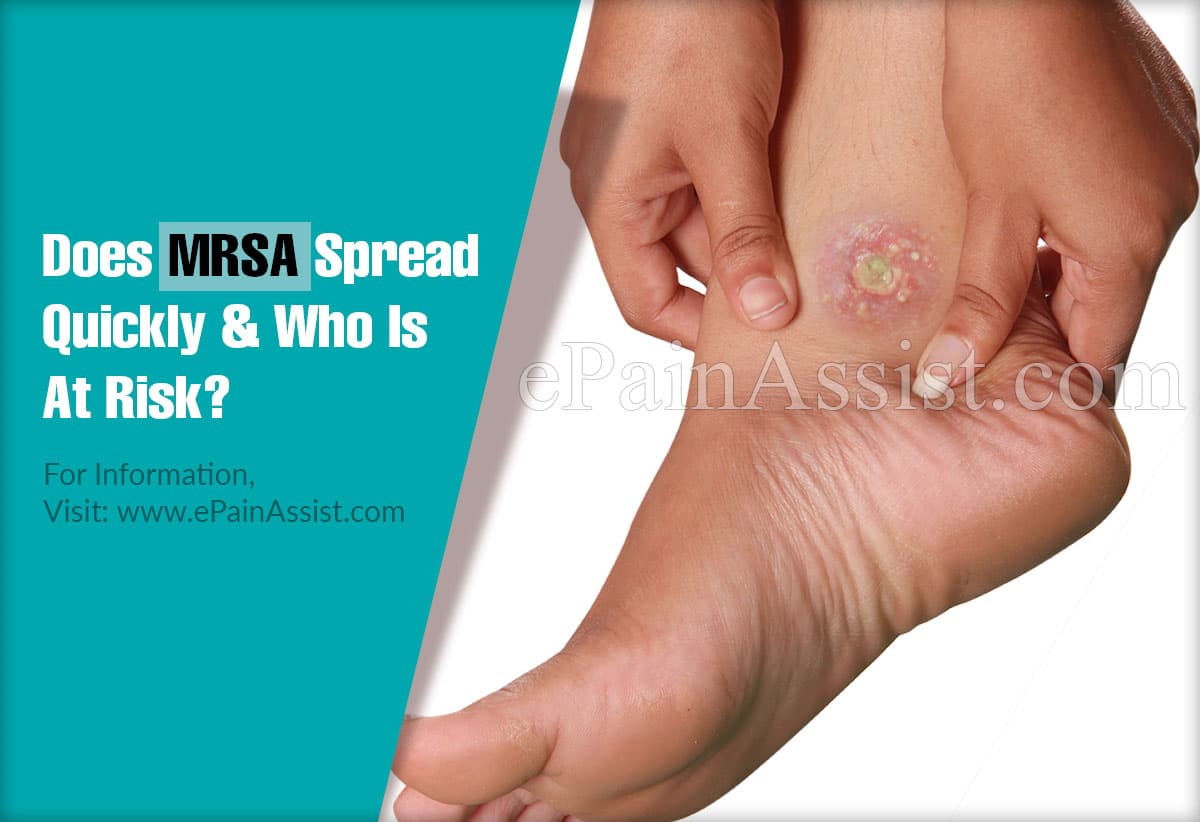
MRSA usually spreads by coming in contact with the person carrying these bacteria. Methicillin resistant variety of staphylococcus is predominantly found in hospital settings or other Healthcare settings such as Nursing Home, dialysis Center, blood banks. When this infection is acquired in these Hospital settings it is known as healthcare-associated MRSA. Another variety of MRSA infection which occur in communities is community associated MRSA.(2)
Who Is At Risk?
Methicillin resistant is a result of overzealous uses of antibiotics. The appropriate use of antibiotics caused the elimination of drugs sensitive bacteria and result in the drug resistant bacteria.
In healthcare-associated MRSA infection, prolonged hospitalization is a great concern for this. MRSA remains common pathogen in hospital setting. Extremes of Ages and immunocompromised status of an individual predisposes them for MRSA Infection. Many invasive procedures in hospital setting likes tubing, intravenous lines, and urinary catheterization may cause these bacteria to gain access to body. Contact with the carriers of methicillin resistant strains causes the spread of infection to individuals with weakened immune status or debilitated individuals.(3)
In community acquired methicillin resistant staphylococcus aureus infection, various factor plays role. MRSA spreads rapidly through any skin to skin contact or through cuts or abrasion of the skin. Overcrowding in families predisposes the infection. Intravenous drug abusers are also at greater risk for acquiring MRSA Infection.
Colonization
In hospital setting, fomites and medical devices contaminated with methicillin-resistant strain of staphylococcus aureus serve as a source of MRSA infections, which usually got contaminated from patients or Healthcare workers infected or carrying these strains. Many streams of staphylococcus aureus colonize anterior nares most frequently. Other common sites include perineum and throat. As Healthcare associated MRSA infections are usually transmitted from an infected patient most of these infections have multidrug resistance. This multidrug resistance strain is very difficult to treat as majority of antibiotic agents are ineffective. Various factors are implicated in Rapid spread and pathogenesis of the disease like immunocompromised status of the patient, pre-existing diseases, acute infection with staphylococcus aureus in a patient having a chronic disease, infection acquired during visit or stay in a health care facilities.
There are various bacterial factors which causes the colonization in humans like surface anchoring proteins, clumping factor B. Teichoic acid, a surface polymer of S.aureus, is been shown to determine the capacity of bacteria to colonize the nasal mucosa.
Community acquired MRSA infections usually present with moderately severe infection of skin and soft tissue. The strains of community acquired MRSA can infect otherwise healthy individual. The increasing number of cases with community-acquired strain is supposed to be due to higher virulence and increased capability of its transmissibility when compared with Healthcare associated strain.
Conclusion
Methicillin-resistant staphylococcus aureus, nowadays, is a common inhabitant in the hospital and more recently in communities. MRSA clones keep occurring in hospital setting and these settings functions as a reservoir for bacteria. These Reservoirs often lead to sustained epidemics of staphylococcus. Genetic Optimization and expression leads to development of new strains with optimized Virulence and colonization capacities. Multidrug resistance makes the treatment of staphylococcus difficult which results in sever disease outcome and complications along with increased number of carriers in the population. With continuous and injudicious use of antimicrobial agents, there is constantly accumulation of genetic information of antibiotic resistance or there is a constant changes taking place in the genetic material of these bacteria which provide them resistance against antibiotics. MRSA is now most common pathogen for hospital associated or Hospital acquired infections.
Also Read:
