What is Osteoarthrosis?
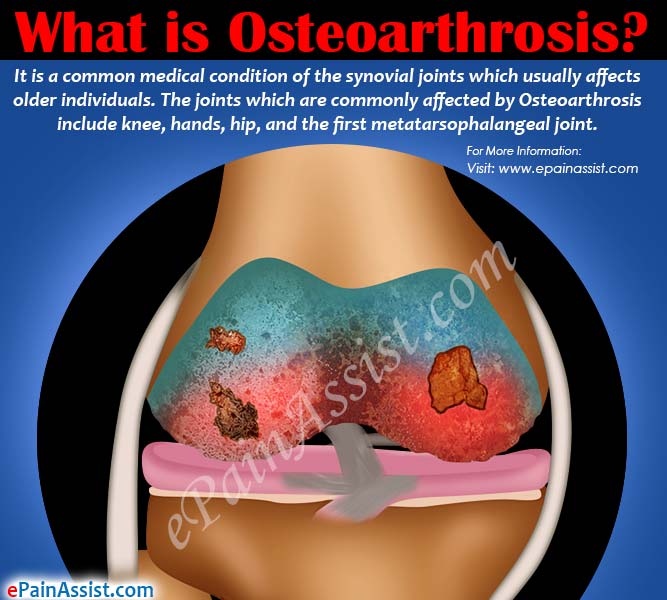
Osteoarthrosis is a common medical condition of the synovial joints which usually affects older individuals. The joints which are commonly affected by Osteoarthrosis include knee, hands, hip, and the first metatarsophalangeal joint. It is uncommon for other joints such as wrist, ankle, and shoulder to get affected and even if they are affected, it is due to a secondary etiology. Even if osteoarthrosis affects multiple joints, the patient experiences the symptoms in one or two joints at the most. The 3 primary symptoms of osteoarthrosis are morning stiffness, pain and difficulty in moving the affected joint. Treatment of osteoarthrosis consists of weight loss, rest, physiotherapy, use of assistive devices, such as shoe lifts, canes, elastic knee support and medications such as NSAIDs.
It is important to diagnose osteoarthrosis early, as sooner the treatment is started the better the progression of the disease can be slowed. The different types of treatment used in osteoarthrosis are non-weight bearing exercises, balneology and physiotherapy.
Pathophysiology of Osteoarthrosis
The articular cartilage is initially affected with degenerative changes and the patient does not feel pain because there are no sensory nerves in the articular cartilage. When there is increase in the degenerative changes, which causes damage to the cartilage or when there is substantial decrease in its elasticity, then the patient experiences pain due to compression of the innervated subcartilage bone. Patient experiences restricted range of motion and pain due to overburdening of ligaments, degenerative processes, shrinking of the articular muscles or capsule and synovial inflammation with exudation into the joint. At this stage of osteoarthrosis, patient has inflammatory substances present in the joint, which exacerbate the degenerative process of the joint. There is production of osteophytes as a result of the joint’s defense mechanism, which further increases the patient’s pain and restricts the patient’s range of motion. In the later stages of osteoarthrosis, there is gradual development of contractions and immobility of the joint. Osteoarthrosis gradually progresses and is felt as stiffness after prolonged immobilization, such as after sleeping during the night and waking up in the morning.
What are the Causes of Osteoarthrosis?
The exact cause of osteoarthrosis is not clear. Osteoarthrosis occurs as a result of multiple factors, which affect the joint as well as the patient. Osteoarthrosis can also develop in patients who are between the ages of 20 and 30. More than half of the patients above the age of 60 suffer from some sort of degenerative joint diseases, which causes joint pain and other joint ailments. The various factors which are thought to cause osteoarthrosis are: old age, congenital conditions or genetic which increases the risk of osteoarthrosis, ethnicity of the patient, abnormal articular biomechanics, occupation, obesity and hormone levels.
Both men and women can be affected by Osteoarthrosis. Osteoarthrosis can occur in men before 45 years of age and women tend to suffer from osteoarthrosis later in life.
What are the Symptoms of Osteoarthrosis?
In Osteoarthrosis, there is wear and tear and degeneration of the tissues of the joints which include the cartilage, subcartilage, articular fluid, ligaments, capsule and muscles. As osteoarthrosis progresses, there is damage to the articular cartilage with restructuring of the bone and development of osteophytes. Hardening of the subcartilage layer occurs with development of subcartilage cysts. There is also impairment of the function of the synovial fluid.
The initial symptom of osteoarthrosis is pain. The pain aggravates during movement or when there is any stress on the joint and the pain is relieved with rest. X-ray test shows extensive changes in the joint and there is also periodic exudations seen in the joint, which alter the natural shape of the joints.
- Radiological tests reveal the following findings in osteoarthrosis
- There is narrowing of the joint space.
- There is thickening of the subcartilage bone layer.
- There are also intra-articular loose bodies and osteochondromas seen.
In osteoarthrosis, patient experiences pain during initial movements followed by crackling in the joints.
Types of Osteoarthrosis
Differentiation of degenerative changes in Osteoarthrosis can be done according to their character:
Primary or Idiopathic Osteoarthrosis
The cause of Primary Osteoarthrosis is not known. It is thought that Primary Osteoarthrosis may occur as a result of irregularities in the local blood circulation in the joints, which cause imbalance in the articular fluid resulting in decreased nourishment to the joint cartilage. People who indulge in activities which overburden the joints, such as playing competitive sports or doing hard physical work are at increased risk for Primary Osteoarthrosis. The main reason for Primary Osteoarthrosis is thought to be patient’s inborn susceptibility to developing osteoarthrosis.
Secondary Osteoarthrosis
- In Secondary Osteoarthrosis the underlying cause is known and it is a class of deformities, which occur as a result of:
- Hereditary or inborn factors, such as hemophilia, inborn hip dysplasia, alcaptonuria or hemochromatosis.
Acquired Systematic and Local Factors such as:
- Local. Injuries, such as recurring joint sprains, multiple small injuries, aseptic necrosis, one great injury, tubercular or septic articular inflammation.
- Systematic. Metabolic diseases, such as chronic rheumatic arthritis, gout, neurological disorders and chronic corticotherapy.
How is Osteoarthrosis Diagnosed?
Imaging tests such as X-rays, CT scan, MRI scan, arthroscopy and isotopic scintigraphy are done. X-ray reveals the characteristic changes in the osteoarthrosis, which are wear and tear of the joints, thickening of the subcartilage bone layer, narrowing of the joint space and presence of intra-articular loose bodies and osteochondromas.
How is Osteoarthrosis Treated?
If the cause of Osteoarthrosis is not known, then the aim of treatment is reducing and managing the symptoms and slowing the progression of osteoarthrosis. If the cause of osteoarthrosis is identified, then the aim of treatment is treating the cause along with the symptoms of osteoarthrosis and managing the progression of this disease. Treatment is modified according to each and every patient depending on the type and progression of osteoarthrosis.
Conservative Treatment of Osteoarthrosis
Medications & Physiotherapy: Conservative treatment of osteoarthrosis consists of medications and physiotherapy to help relieve pain and other symptoms of osteoarthrosis. Physiotherapy in osteoarthrosis consists of electrotherapy, iontophoresis, interferential currents and TENS units.
Sitting and Sleeping on Firm Surface: Patients suffering from osteoarthrosis of knees and hips should avoid sitting in deep soft armchairs and should instead sit on simple and hard chairs and even sleep on hard mattresses.
Avoiding Straining the Joints: Patient should also adopt correct posture and engage in some sort of mild physical activities. Patient should avoid undue stress to the joints and rest appropriately and make use of crutches or cane as and when needed.
Exercises: Exercises, which improve muscle strength and elasticity, should be done to help maintain maximum mobility without pain. Exercise also helps in preventing muscle contractions and especially non-weight bearing exercises help in slowing the progression of osteoarthrosis.
Rest: Rest should be taken to avoid overburdening of the joints. Immobilization for extended periods or short periods should be avoided as it aggravates osteoarthrosis and can lead to complete arthrodesis when remaining in a restricted posture.
Weight Loss: Obese patients should lose excess weight to prevent stress on the joints.
Medicines Used in Treating Osteoarthrosis
Pain is the main and the most annoying symptom in osteoarthrosis. The degree of pain felt in osteoarthrosis differs from patient to patient. Medications used to treat the pain and inflammation in Osteoarthrosis are:
Non-Steroidal Anti Inflammatory Drugs (NSAIDs): These medicines help in relieving pain, inflammation and fever. NSAIDs, which can be used in osteoarthrosis, are ibuprofen, indomethacin, acetylsalicylic acid, naproxen and ketoprofen. NSAIDs can be used orally, rectally or topically (in the form of ointments, creams or gels). If there is only mild pain, then patient can use topical form of NSAIDs. In case of severe pain, NSAIDs should be administered orally or rectally.
Disease-Modifying Anti-Rheumatic Drugs (DMARDs): These medicines contain steroid and are much stronger. DMARDs consist of medicines, such as suflazaladine, gold preparations, D-penicillamine and immunosuppressants, such as methotrexate. These medicines have side effects such as: nausea, vomiting, headaches, skin rash/ irritation, diarrhea or intestinal disorders.
Glucocorticoids: This medicine can be injected directly into the joint or into the affected area and should be used only twice or thrice a year. Excessive use of Glucocorticoids causes further joint damage.
Hyaluronic Acid Injections: These injections are given into the joint about 2 to 5 times in a week’s intervals. Hyaluronic Acid is a natural component of the synovial fluid and improves the sliding of the articular cartilage and provides nutrition to the tissue. The effects of these injections can last up to 6 months.
Muscle Relaxants: These medicines have soothing effect and helps in relieving the pain in osteoarthrosis. Muscle Relaxants which can be used in osteoarthrosis are tolperisone or tetrazepam.
Medicines Which Contains Features Of Articular Cartilage: These medicines consist of glucosamine, collagen, chondroitin sulfate and vitamin C. These drugs are thought to help in construction of elements of cartilage to benefit patients suffering from osteoarthrosis or other joint diseases.
Medicines Which Improve Blood Circulation & Tissue Metabolism: These medicines are used in osteoarthrosis when the cause of osteoarthrosis is thought to be a pathological problem in the blood vessels.
Injections of Autologous Growth Factors: These injections promote healing, help in regeneration of cartilage and reduce inflammation.
Homeopathic Injections: These injections contain herbal extracts and animal placenta extracts, which helps in reducing inflammation and promoting healing.
Surgical Treatment in Osteoarthrosis
If the conservative treatment does not provide relief and the patient still has persistent pain or if there is severe damage to the joint, then surgery is recommended. Surgical procedures done in osteoarthrosis include:
Arthroscopy: This is a surgical procedure, which helps in removing the damaged tissues from the joint.
Endoplasty: This surgical procedure replaces the surface of the joints and excises the damaged joint and replaces them with new plastic or metal.
Osteotomy: This surgery helps in correcting the placement of joint and bones surfaces.
Corrective Surgeries: In case of extensive damage to the joint, corrective surgeries are done to fix the bone placement and ligaments to improve the function of the limb.
Treatment of Osteoarthrosis in Young Patients
In young patients experiencing pain due to connective tissue changes, treatment consists of increasing blood circulation locally. Treatment for this consists of exercises, peat poultices, hot baths, massages, warm gel wraps and solux. In case if the osteoarthrosis is very severe, then patients should avoid hot baths, paraffin, peat and Fango poultices, as these can aggravate the coexisting osteoporotic changes. Kriotherapy helps in relieving inflammation and swelling. Other than this magnetic field and laser therapy also can be used in treating osteoarthrosis.
Prevention of Osteoarthrosis and Other Degenerative Joint Diseases
The following things need to be followed in order to prevent Osteoarthrosis:
- Maintaining proper body weight.
- Following healthy nutrition and diet.
- Avoiding stressing or overburdening of the joints.
- Engaging in moderate physical activity.
- Avoiding unnecessary stress and weight bearing of the joints.
- Addressing any infection of the joints immediately.
- “Osteoarthritis (OA)” – Arthritis Foundation https://www.arthritis.org/diseases/osteoarthritis
- “Osteoarthritis” – Mayo Clinic https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925
- “Osteoarthritis: Symptoms and Causes” – Cleveland Clinic https://my.clevelandclinic.org/health/diseases/18009-osteoarthritis
- “Osteoarthritis” – OrthoInfo, American Academy of Orthopaedic Surgeons https://orthoinfo.aaos.org/en/diseases–conditions/osteoarthritis
Also Read:
