Pain is an agonizing perception of injury or feeling of hurt. Pain is felt with different intensity. Pain is a symptom, which diverts attention to recognition of injury to normal tissue or organ. It is essential to identify cause of distress as soon as possible for treatment as well as prevention of further tissue damage. Chronic pain could be secondary to cancer or non-cancer in etiology. Chronic pain is presented as nociceptive, neuropathic or mixed pain.
Types of Chronic Pain:
- Nociceptive
- Neuropathic
- Mixed
- Epidemiologic studies (cont.)
Epidemiological Studies Have Revealed Following Incidence and Prevalence of Chronic Pain
- 70 Million adult in United States suffer with chronic pain.
- 35% of population suffers with chronic back pain and spine pain.
- 10% of population in USA are diagnosed of arthritis.
- 12% suffer with chronic joint syndrome includes 10% of arthritis.
- 70% of adult suffer with low back pain at least once or more and common age group is 35 to 55 years of age.
Classifications and Epidemiology of Chronic Nociceptive Pain
Types of Chronic Nociceptive Pain:
- Cutaneous.
- Somatic.
- Visceral.
Pathophysiology and Anatomy of Chronic Nociceptive Pain
Somatic and Sympathetic Nerves:
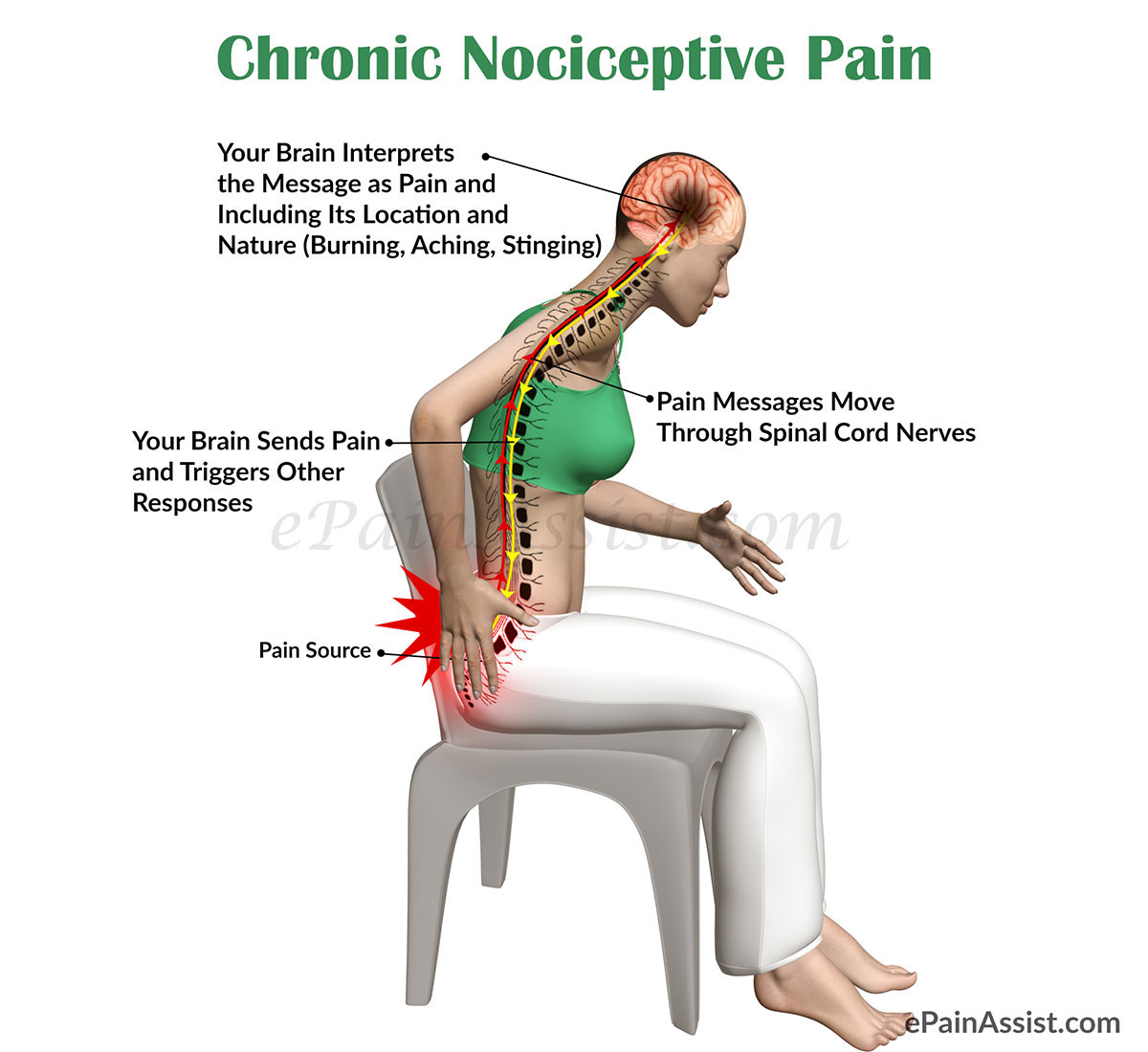
Peripheral nerves transmitting pain are somatic and sympathetic nerves. Pain is transmitted from pain receptors by somatic and sympathetic nerves to spinal cord and brain. Somatic nerve transmits massages from receptors located over skin, subcutaneous tissue, muscles, tendons and bones. Massage is relayed to nerve cells (neurons) in spinal cords. Sympathetic nerve transmits pain massages from pain receptors to neurons in spinal cord. Somatic and sympathetic nerves of neck, thorax (chest), abdomen, upper and lower extremities originate from spinal cord. Somatic and sympathetic nerves to face and head come from cranial nerves.
Anatomy of Nociceptive Pain:
- Nociceptor: Pain receptors located at peripheral end of pain carrying fibers.
- Neurotransmitters secreted by damaged tissues following trauma.
- These neurotransmitters are kinin, prostaglandin, and calcium.
- These neurotransmitters activate pain receptors.
- Nociceptor nerve carries pain stimulation from nociceptor receptors to the spinal cord.
Chronic State Of Nociceptive Pain:
Nociceptive pain starts off instantaneously after tissue injury. Healing of injured tissue if inadequate and tissue trauma continues beyond six months nociceptive pain become chronic in nature. Chronic state of nociceptive pain relates to continuous secretion of neurotransmitters within injured scar tissues or healing tissues. Information carried by nociceptor nerve is exchanged in spinal cord between nociceptor nerve and nerve fibers continue to brain. Stimulation of nociceptor receptors by neurotransmitter following injuries causes severe intractable pain. Nociceptive pain disappears as the tissue damage heals.
Causes And Risk Factors of Chronic Nociceptive Pain
Causes of Chronic Nociceptive Pain
Nociceptive pain is an acute pain for 3 to 6 months. Nociceptive pain is considered chronic if continues for over 6 months.
Cutaneous Nociceptive Pain:
- Confined within skin and subcutaneous tissue.
- Tissue trauma such as laceration, abrasion, Repeat injury- increases pain intensity and duration (chronic) Nonhealing skin ulcers, skin burns, bump, bruise, or inflammations.
Somatic Nociceptive Pain:
- Triggered due to injury or trauma of muscles or ligaments. Fracture, joint dislocation Muscle tear or injury, Tendon rupture.
- Arthritis : rheumatoid and osteoarthritis.
- Sprains: To the ligaments or muscles.
- Inflammation: Of muscles following injury or infection.
- Muscle disease: myofascial pain, fibromyalgia and myofascitis.
- Bones and joints pain: Arthritis, fractures, injuries and laceration of periosteum.
Visceral Nociceptive Pain:
- Involves: Injury, inflammation or trauma to the interior organs.
- Secondary to obstruction, inflammation and lack of blood supply (ischemic) Sudden in occurrence.
- Obstructions: These can be strictures, adhesions, or impacted stones causing obstruction of gallbladder, the bile duct, ureter, kidney, or bladder.
- Inflammation: This can be due to peritonitis, appendicitis, gastric ulcer, or inflammation of gallbladder.
- Ischemic: This can be due to myocardial infarction, non-healing ulcers, or ischemic colitis.
Symptoms and Prognosis of Chronic Nociceptive Pain
Nociceptive Pain
- Well localized
- Constant
- Aching or throbbing quality
- Reduced joint, ligament or muscle function
- Moderate pain at rest.
Activities Of Joint, Muscles Or Ligament:
- Pain may be severe and intractable.
- Time limited pain: Pain resolves with healing of tissue damage.
- Arthritis is an exception as it is not time limited.
- Nociceptive pain responds successfully if treated with NSAIDs or opioids.
Cutaneous Nociceptive Pain:
- Character of pain- sharp, well localized.
- Duration of pain- short (acute).
- Location- limited to area of injury or inflammation.
- Duration of pain could be short.
- Repeat injury will increase intensity of pain.
Somatic Nociceptive Pain:
- Somatic pain is sharp and well localized aching pain.
- Duration of pain is longer compared to cutaneous pain. Pain is experienced as sharp and aching pain.
- Duration of pain is longer compared to cutaneous pain (chronic).
Visceral Nociceptive Pain:
- Severe intractable pain needs immediate attention or hospitalization.
- Dull and aching.
- Throbbing and colicky pain at time.
- Difficult to localize.
- Episodic and poorly localized.
- Dull and aching pain.
- Referred to adjacent or distal part of the body e.g. gallbladder pain.
- Referred to the scapula.
- Localized in the internal organs.
- Poorly localized.
- Duration of pain- short or prolong.
- Referred pain- Referred to adjacent part of the body e.g. gallbladder pain may referred to the scapula.
Treatment for Chronic Nociceptive Pain
Medications for Chronic Nociceptive Pain
- Antibiotics: Appropriate antibiotics are used.
- NSAIDs-Pain due to tissue inflammation: Recommend nonsteroidal antiinflammatory drugs.
- Opioids: If there are side effects or not enough pain relief with NSAIDs, this can be used.
- Muscle Relaxants: Baclofen, Flexeril etc.
- Adjuvant Pain Medications: Lyrica, Neurontin, Cymbalta etc.
Manual Therapy for Chronic Nociceptive Pain
- Massage.
- Chiropractic treatment.
- Osteopathic joint manipulations.
- Acupuncture.
- Physical therapy.
Interventional Rx Treatment for Chronic Nociceptive Pain
- Peripheral nerve blocks with cortisone injections.
- Epidural/caudal cortisone injections.
- Sympathetic ganglion blocks.
- Nerve Ablation: using radiofrequency techniques or chemical nerve ablation.
Surgery for Chronic Nociceptive Pain
- Incising the abscess for removing skin lesions.
- Excision of appendix, gallbladder etc.
- Surgical procedure for treatment of fracture.
Investigation And Lab Studies for Chronic Nociceptive Pain
Investigations for Chronic Nociceptive Pain
- Blood examination: Check infection, peritonitis and abscess related pain
- X-ray: check tissue trauma, bone injury, fracture, arthritis, air in peritoneum
- MRI: check fracture or dislocation of joint, differential diagnosis of rheumatoid and osteoarthritis.
- CAT Scan: bowel obstruction, perforation
- Ultrasound: abdominal bleeding, aneurysm, obstruction; stones in gall balder, Kidney, ureter, bladder and urethra.
- EKG- rule out angina.
- Echocardiography: rule out cardiac causes of pain.
Also Read:
