Have you heard or known about the Asherman’s syndrome? If not, then read below to know about the condition, its stages, causes, symptoms and treatments. We will also talk if Asherman’s syndrome can cause miscarriage.
About Asherman’s Syndrome
Asherman’s syndrome is a rare gynecological disorder in which scar tissue forms within the uterus. It causes pain, abnormal menstrual bleeding and in some cases amenorrhea which decreases the chances of the affected female getting pregnant. The main concern with Asherman’s syndrome is that it can result in problems of becoming pregnant or pelvic pain because of the intrauterine scarring.
There are primarily four stages of the syndrome, i.e. stage 1, stage 2, stage 3 and stage 4. Treating the condition is done by a surgical procedure. More about the stages and treatments are explained in the following sections.
Stages of Asherman’s Syndrome
Stage 1:
In this first stage of Asherman’s syndrome, there is very little scarring in cervical canal and/or uterine cavity. Unless the isthmus which is a part of the uterus gets affected, there is little to no impact on normal functioning of the uterus. No treatment is required for Stage 1 Asherman’s Syndrome.
However, if the isthmus gets affected then the functioning of the uterus also gets affected and treatment for such instances becomes necessary. Females with Stage 1 Asherman’s Syndome n most cases are able to conceive again.
Stage 2:
In the stage 2 of Asherman’s syndrome, there is obstruction of the inner part of the Os which is a tiny structure within the cervix which opens into the uterus. The Os tends to normally get blocked pretty easily. In some females, this obstruction may be just a fraction of a millimeter but in some cases it may range to several centimeters.
If the scarring involves the isthmus, there is no pain but also there will be no production of blood for menstruation. In some cases, mild cramps canbe observed in some females even though such cases are few and far between with no bleeding; however, this is not pretty common.
Females with stage 2 Asherman’s syndrome have 60% of chance to become pregnant again after appropriate treatment.
Stage 3:
In this stage of Asherman’s syndrome, scar tissue blocks approximately half of the uterus. The tubal orifices may also get affected by the scar tissue.
It should be noted here that the more the scar tissue formation he greater challenge it poses for a successful treatment. With stage 3 of Asherman’s syndrome, females have around 20% chance of conceiving and successfully delivering.
Stage 4:
In the 4th stage of Asherman’s syndrome, more than 3/4th of the uterus gets blocked and its size becomes extremely small. Treatment at this stage requires frequent visits to the physician with a very low percentage of females being successfully treated. However, with the introduction of stem cell technology the success rate has improved somewhat.
Causes of Asherman’s Syndrome:
More than 90% of cases in Asherman’s syndrome are caused due to infections or any complication that arises during or after a surgical procedure which involves a pregnant female or a female who has recently delivered. In cases of miscarriages or abortions between 12 to 20 weeks, the likelihood of developing Asherman’s syndrome is relatively high.
It must also be noted that some females may be genetically predisposed to scar tissue formation in the uterus. Age also plays a role in females developing Asherman’s syndrome.
The formation of scar tissue is normally seen on the inner aspect of the uterus. This is a part of the uterus which does not regenerate after a menstrual period which is the case with cervical canal and tubal ostia. Scar tissue formation is also seen on the endometrium, especially during pregnancy when the endometrium is most vulnerable due to its inability to adequately respond to injuries.
A female who is not pregnant also may be at risk for developing Asherman’s Syndrome as a result of uterine fibroids which needs to be surgically removed. Uterine fibroids cause the uterus to get enlarged and stretch the blood vessels which can lead to blockages. This results in a lack of supply of oxygenated blood and other vital nutrients to the tissues causing them to become necrotic resulting in formation of scar tissue.
There are also hypothetical information which points that radiation treatment to treat certain cancers within the abdominopelvic region can cause scar tissue formation, as blood flow to the uterus gets reduced causing the uterus to produce less estrogen. A low level of estrogen promotes scar tissue formation within the uterus.
Presenting Features of Asherman’s Syndrome:
Reduced or Absent Menstrual Flow
The most important symptom of Asherman’s syndrome is that there is reduced menstrual flow or in some cases amenorrhea, most notable after a recent pregnancy with successful delivery, a recent miscarriage, abortion, or history of a known infection in the abdominopelvic region.
Pelvic Pain And Hematometra:
One more common symptom of Asher’s syndrome is pelvic pain. The pain occurs due to intense pressure being applied on areas where the menstrual fluid has been trapped by the walls of the uterus. In cases of a complete block in the cervix due to scar tissue, then the gradual of fluid buildup behind the obstruction gets trapped and the ensuing pressure results in pain which can at times be so severe that the patient may have to go to the emergency room for evaluation. This is the condition known as Hematometra and it is like a big bruise within the uterus.
A pelvic ultrasound normally confirms the obstruction and treatment requires a surgical procedure for removal of the obstruction.
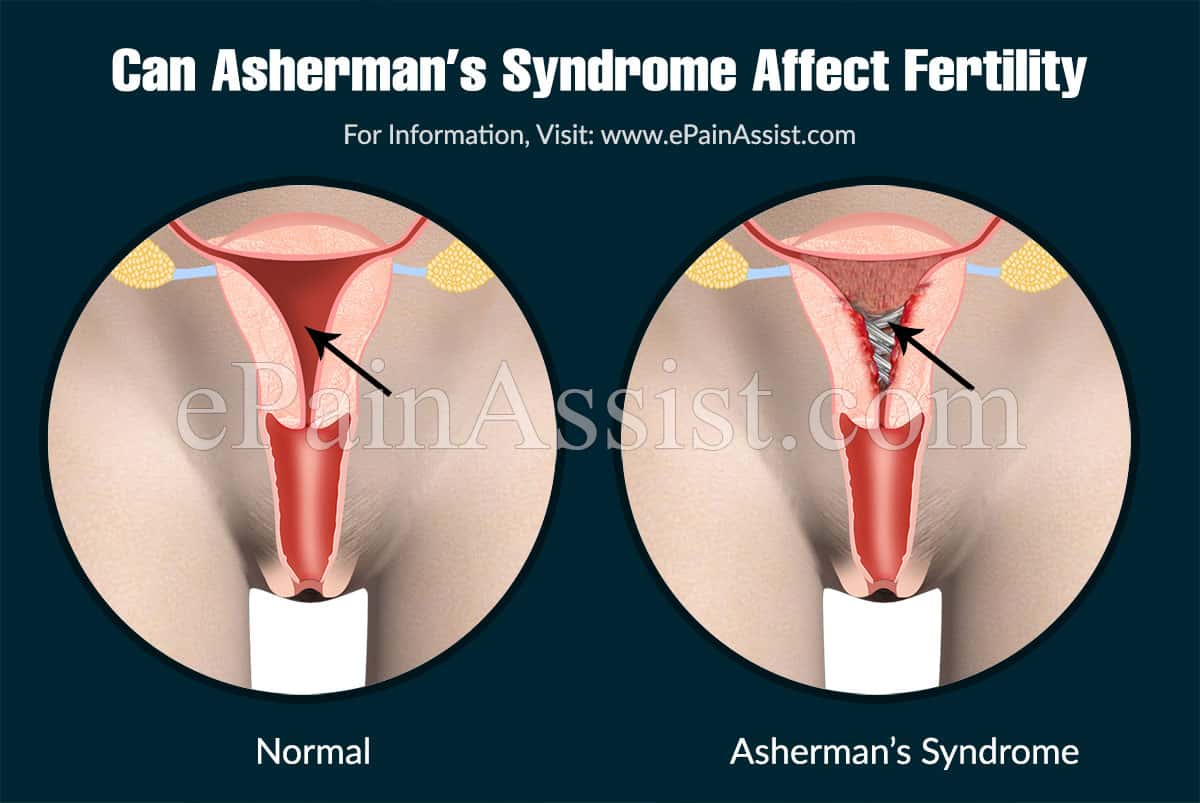
Can Asherman’s Syndrome Affect Fertility:
It is presumed that Asherman’s syndrome in its later stages can affect fertility. There are also chances of miscarriages and stillbirth.
Diagnosis of Asherman’s Syndrome:
The diagnosis may be done in two different ways. One is by an indirect test that uses an ultrasound or an X-ray, where the inside of the uterus may be assessed. In these tests, a thin tube is place via the cervix into the uterus and a fluid is pushed into the uterine cavity. The fluid or the dye flows all around the cavity, and in the presence of scar tissue it causes an abnormal shape or shadow that is seen on the X-ray or the Ultrasound.
The second diagnostic test is known as Hysteroscopy. In this, a thin telescope is placed into the uterine cavity via the cervix. It must be noted that this does not require any incisions. The telescope is then able to locate any adhesions, which may be present and then they can be treated.
Treatments of Asherman’s Syndrome:
The best treatment for Asherman’s syndrome is the surgery that is used to remove scar tissue from the uterine cavity and restore it to normal function. You will be admitted to hospital and have the procedure of surgery performed under a general anesthetic, if you are diagnosed with Asherman’s syndrome.
Your surgery will generally be scheduled between day 3 and day 12 of your menstrual cycle. You will be prescribed with antibiotics so as to reduce the risk of infection. You need to start taking these antibiotics, 2 days before your surgery and need to continue for 5 days afterwards.
About Surgical Procedure :
You will be placed under general or local anesthesia at first. Once you are safely sedated, a thin telescope known as a Hysteroscope, is inserted into the uterus via the cervix (no cuts are made) and the presence and the extent of scarring is noted. Sometimes it is not possible to see inside the uterus immediately and thus Sonography or X-rays are used for the same.
If there is a presence of scar tissue in the cervix, it may be necessary to break this down before the tip of the hysteroscope could be advanced. In order to assist in this process, a fine hollow needle is used for finding the usual passage where there is no scar tissue. Your surgeon will slowly open up the endometrial lining in order to reconstruct as normal a cavity as possible.
Micro-scissors are used through the hysteroscope to start to remove the scar tissue. Normally, the patient is given estrogen medication for the next 2-3 weeks to hasten the repair of the endometrium and promote growth of new small vessels which overall reduces the likelihood of scar tissue formation. Hyaluronic acid gel is then placed in the uterus as it hastens the healing process and also acts as a barrier between the front wall and the back wall of the uterus.
In case of intense scarring seen normally in stages 2, 3 and 4 of this disease, the patient will require at least two surgeries for complete treatment. The patient will also have to take estrogen supplement between operations, which are normally done within a gap of 2-3 months.
Once the patient is through with the course of estrogen supplements, the menstrual periods begin within a month after stopping the medication. Once the periods start, the surgeons will perform another ultrasound to monitor he functioning of the uterus. A repeat surgery is done if the ultrasound shows scarring or if menstrual periods do not begin even after 30-40 days after the initial procedure.
Can Asherman’s Syndrome Cause Miscarriage?
Some females with Asherman’s syndrome are not able to ever conceive and even if they do they almost always end up having a miscarriage. Though it is possible for you to become pregnant if you have Asherman’s syndrome, but the adhesions in the uterus might pose a risk to the developing feuts. It is also true that your chances of miscarriage and stillbirth will be greater than in women without the Asherman’s syndrome.
Apart from this, the condition also increases the risk of placenta previa, placenta increta and excessive bleeding, during pregnancy.
Your doctor will diagnose the condition and let you know about the best possible treatment. The surgical procedure done to treat Asherman’s syndrome, will usually increase your chances of conceiving and having successful pregnancy without miscarriage or stillbirth. However, doctors recommend waiting a full one year after the surgical treatment before you begin trying to conceive.
Conclusion:
Asherman’s syndrome is usually treatable. So, if you feel you might have the condition or if you are diagnosed with the condition, do take the advice from your healthcare provider and take the best possible treatments to get rid of it. Also know from them what all precautions you must take so as to conceive once again. If it is that you are unable to conceive, still want children, you can try options like, surrogacy and adoption.
