Optochiasmatic arachnoiditis, happens when the arachnoid behind the optic nerve and the optic chiasm gets thickened abnormally. It also affects the adjoining nerves as well as the pons. The arachnoid exists in the form of thin inflamed films on the optic nerves or on the adjoining blood vessels. Optochiasmatic arachnoiditis, if not addressed in time can lead to complete loss of vision.
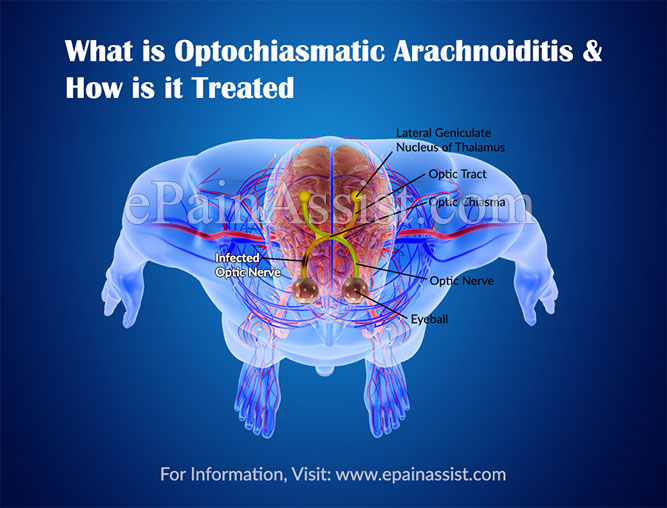
What is Optochiasmatic Arachnoiditis?
Our brain, spinal cord and the optic nerves are covered with three kinds of membranes, to protect them from any external damage. These layers are called meninges. The innermost layer is called the pia mater, middle layer is called arachnoid and the outermost layer is called dura mater.
At the back of the eyes, lies the optic chiasm which is the junction between the two optic nerves. When this arachnoid present on the optic nerve or the optic chasm gets infected, usually due to a viral infection, then the condition is known as optochiasmatic arachnoiditis. Apart from infection, arachnoiditis may also be of a traumatic origin or post the surgery of the eye.
The occurrence of optochiasmatic arachnoiditis usually constitutes three phases, which are inflammatory phase or the phase of inflammation of the arachnoid, followed by fibrous phase which witnesses fibrosis and lastly, the hyperplastic phase which marks the excessive proliferation of the cells of the arachnoid membrane leading to the thickening of the arachnoid membrane. This leads to compression of the arachnoid membrane as well as obstruction of the supply of blood to the optic nerve which further result into progressive impairment of vision.
Symptoms of Optochiasmatic Arachnoiditis
The common symptoms of optochiasmatic arachnoiditis are:
- Headaches
- Slow and progressive loss of vision
- Change in the visual field
- Paralysis of eye muscles
- Pain in the sockets of the eye
- Visible difference in the size of both the pupils
- Reduction or loss of the blinking reflex
- Obesity
- Disturbances in vision.
Epidemiology of Optochiasmatic Arachnoiditis
The population affected by optochiasmatic arachnoiditis is mostly females, accounting approximately sixty to sixty five percent of the affected individuals. The incidence rate of optochiasmatic arachnoiditis is over ten thousand cases each year and the most common causative factor behind the condition is surgery related to brain, spinal cord and optic nerves.
Prognosis of Optochiasmatic Arachnoiditis
The outlook for optochiasmatic arachnoiditis is not good, because most cases result in loss of vision. The condition is usually left undiagnosed or poorly diagnosed.
Risk Factors for Optochiasmatic Arachnoiditis
The probable risk factors that pose a threat of optochiasmatic arachnoiditis are:
- Infection in the eyes, especially around the sockets.
- Trauma to the eyes or the brain, causing bleeding around the eye sockets.
- Surgical procedure in close proximity to the optic nerves.
- Exposure of eye to radiation or chemotherapy.
- Condition is more prominent in females, especially the pregnant females.
Complications of Optochiasmatic Arachnoiditis
The one and the only common complications of the optochiasmatic arachnoiditis is the visual impairment. The degree of visual impairment depends upon the phase of optochiasmatic arachnoiditis the patient is suffering form.
Diagnosis of Optochiasmatic Arachnoiditis
The proper diagnosis of optochiasmatic arachnoiditis is quite difficult. The diagnostic procedures that are utilized for the diagnosis of optochiasmatic arachnoiditis are:
- Physical Examination to Diagnose Optochiasmatic Arachnoiditis: The physical examination checks for the existing symptoms as well as the history of the patient, to identify the condition.
- CAT scan: The computerized tomography scan is a commonly used diagnostic procedure that checks for aneurysms around the optic nerve and the optic chiasm.
- MRI to Detect Optochiasmatic Arachnoiditis: This is another imaging technique which utilizes magnetic field to provide a precise and localized image of the arachnoid membrane and the extent of optochiasmatic arachnoiditis.
- Cisternography: Cisternography is an imaging technique which introduces a radionuclide into the cerebral spinal fluid. The flow of the cerebrospinal fluid to the nerves, brain and spinal cord is then studied. This gives a clear image of the optochiasmatic arachnoiditis.
How is Optochiasmatic Arachnoiditis Treated?
There is no proper cure for optochiasmatic arachnoiditis, but there are certain treatment methods which are followed; however, their effectiveness is quite controversial.
The treatment options are as follows:
- Medications: Drugs like dexamethasone, cyclophosphamide and several other Schedule III drugs are prescribed to provide relieve from the symptoms of optochiasmatic arachnoiditis. It is imperative to know that these drugs develop dependence; thereby, caution should be exercised while prescription drugs are administered.
- Physical Therapy for Optochiasmatic Arachnoiditis: It is a mild therapy that aims at recovering and restoration of the lost functions of the eye as well as preserving them. It involves mild massaging of eyes, water therapy and compression using hot as well as cold agents.
- Surgical Lysis to Treat Optochiasmatic Arachnoiditis: It is a surgical measure that is used to remove the cysts formed on and around the arachnoid region behind the optic nerves, but it only helps to a small extent.
Conclusion
Optochiasmatic arachnoiditis is a condition of the eye in which the arachnoid present in the eye socket behind the eye gets thickened due to infection or trauma. The arachnoid membrane at the optic chiasm gets affected, which leads to loss of vision with the passage of time. Optochiasmatic arachnoiditis is usually accompanied by headaches, pain in the eye sockets and difficulty in vision. It is often misdiagnosed, which then leads to complete blindness. Though there are treatments available for optochiasmatic arachnoiditis, but there is no defined cure for it and the treatments aim to provide just symptomatic relief.
- American Academy of Ophthalmology. Optochiasmatic Arachnoiditis. https://www.aao.org/disease-review/optochiasmatic-arachnoiditis-review
- JAMA Ophthalmology. Metamorphopsia and Optochiasmatic Arachnoiditis. https://jamanetwork.com/journals/jamaophthalmology/article-abstract/640898
- National Center for Biotechnology Information. Optochiasmatic Arachnoiditis: Clinical Presentation, Radiological and Surgical Features. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4217776/
Also Read:
