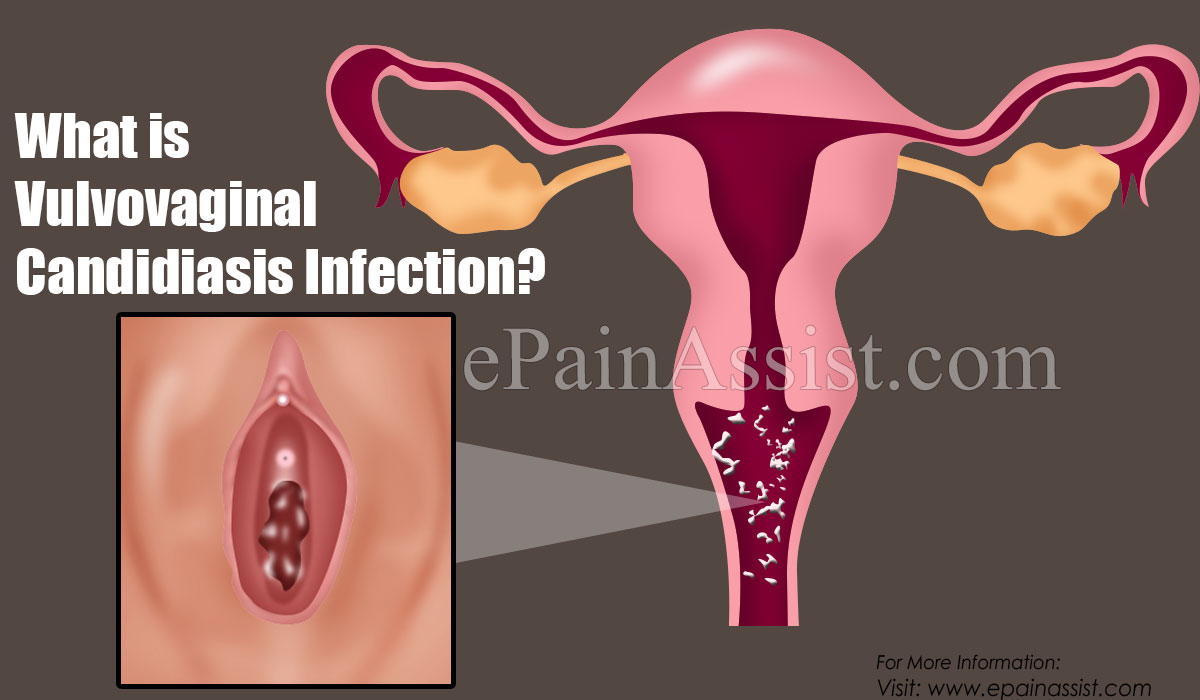
What is Vulvovaginal Candidiasis Infection?
Candidiasis is a common yeast infection caused by a type of fungus known as Candida. Candida tends to typically live inside the body in places such as the throat, mouth, gut, and vagina, and on the skin without causing any problems. However, in some cases, Candida can multiply and cause an infection if the vaginal environment changes in a way that encourages the growth of Candida. Candidiasis in the vagina is usually referred to as a vaginal yeast infection. This type of yeast infection of the vagina is also known as vulvovaginal candidiasis, vaginal candidiasis, or candida vaginitis.1,2
Most cases of vaginal yeast infections are caused by the fungi Candida albicans. However, there are several other strains of Candida that can also cause infections. These include:
- Candida parapsilosis
- Candida glabrata
- Cryptococcus neoformans
- Candida tropicalis
- Candida krusei
A healthy vagina contains various types of bacteria, along with some yeast cells. However, when this healthy balance of yeast and bacteria changes, it can cause the yeast cells to rapidly multiply, causing swelling, itching, and irritation. Treating a vaginal yeast infection such as vulvovaginal candidiasis can help alleviate the symptoms within a couple of days. In more severe cases, it may take at least two to three weeks to treat the vulvovaginal candidiasis infection.
Such types of vaginal yeast infections are not considered to be a type of sexually transmitted infections (STIs) or a sexually transmitted disease (STD). However, it is possible for vulvovaginal candidiasis to spread through sexual contact, but even women who are not sexually active can get such an infection. It is essential to know that once you get a yeast infection like vulvovaginal candidiasis, you become more prone to getting another one. It is estimated that three out of four women will experience candidiasis at some point in their lifetimes. Many women even experience at least two or three episodes.3
However, some evidence shows there is a higher risk of getting a vaginal yeast infection when you first start having regular sexual activity.
There is also evidence that suggests that vulvovaginal candidiasis may be linked to mouth to genital contact or oral-genital sex.4
Symptoms of Vulvovaginal Candidiasis
The common symptoms of vulvovaginal candidiasis include:
- Swelling around the vagina
- Vaginal itching
- Soreness in and around the vagina
- Burning during sex or urination
- Painful sexual intercourse
- Redness
- Rash
Another telltale symptom of a vulvovaginal candidiasis or vaginal yeast infection is having a yellowish or whitish-grapy and clumpy vaginal discharge. Many women describe this discharge as appearing like cottage cheese. Sometimes, you may also experience whitish and watery discharge.5
The longer you leave this type of yeast infection untreated, the greater will be the impact on how severe your symptoms of vulvovaginal candidiasis become. This is why it is recommended that you seek early treatment when you first experience any of the symptoms.
Causes of Vulvovaginal Candidiasis
As mentioned above, a fungus called Candida is the primary cause of candidiasis. Candida is a naturally growing microorganism that is found in the vaginal region. A bacteria known as Lactobacillus is responsible for keeping the growth of Candida in check in the body. However, if an imbalance occurs in the body, Lactobacillus and other bacteria stop working effectively. This leads to an overgrowth of yeast, which causes the symptoms of vulvovaginal candidiasis.6
There are many factors that are responsible for causing vulvovaginal candidiasis. These include:
- Hormonal imbalance, especially around the time of your menstrual cycle or during pregnancy
- Hormonal imbalances are linked closely to yeast infections like vulvovaginal candidiasis. Women are more likely to get candidiasis if they are on hormonal contraception, around their period, or if they are pregnant. This is because these can disrupt the body’s natural balance of the hormones estrogen and progesterone. High levels of estrogen are known to cause Candida to multiply rapidly.7
- It is also common to get a vaginal yeast infection around the time of your menstrual cycle. Hormonal changes that happen during your period can potentially kill the ‘friendly’ bacteria that live in the vagina, causing an imbalance. In fact, some women get candidiasis at around the same time as their period every month, a condition that is known as cyclic vulvovaginitis.8
Antibiotics
Antibiotics are prescribed for killing off any harmful bacteria in the body. However, at the same time, they can also destroy the helpful bacteria in the body, leading to a vaginal yeast infection.
The vagina has its own balance of bacteria and yeast. Lactobacillus is responsible for keeping the vagina in a slightly acidic state, which does not allow the yeast to grow. This slightly acidic environment also helps keep the yeast present in the vagina under control.
When you are on broad-spectrum antibiotics, commonly prescribed for a sinus infection or bronchitis, it can throw off the body’s natural balance of bacteria. While they kill off the harmful bacteria causing the illness, they also wipe out the beneficial bacteria, such as Lactobacillus. When there is not enough Lactobacillus, the vagina becomes less acidic, allowing for yeast to thrive and grow.
If you are taking antibiotics, there are several things you can do to lower the risk of getting vulvovaginal candidiasis. The first thing is to let your doctor know if you experience chronic yeast infections. If you have a history of getting a yeast infection every time you are on antibiotics, your doctor may prescribe an oral antifungal medicine like fluconazole (brand name Diflucan). You will need to take the medication during the course of antibiotics. Such medications help prevent an overgrowth of yeast while you are taking the antibiotics.9
If antibiotics are causing you to develop chronic candidiasis, you can use an over-the-counter (OTC) antifungal suppository or cream to prevent yeast infections. Antifungal agents present in such medications take the place of the killed good bacteria and keep working to prevent the overgrowth of yeast. You should start the antifungal medicines at the same time as you begin your antibiotic course to avoid a yeast infection.10
You can also undo some of the damage caused by antibiotics by replenishing the good bacteria in the body. This can be done by taking a probiotic supplement that contains Lactobacillus. Adding yogurt with live active cultures to your diet can also help. There are many probiotic yogurt brands that add Lactobacillus acidophilus, which increases the number of good bacteria in the body.
Uncontrolled Diabetes
People with uncontrolled diabetes are at a higher risk of having vulvovaginal candidiasis. This is because persistent high blood sugar levels are an ideal condition for yeast to grow. People with diabetes also have a weakened immune system, which also increases the risk of candidiasis. It is essential for people with diabetes to learn to recognize the symptoms of a fungal infection like vulvovaginal candidiasis and to receive prompt treatment as if left untreated, it can cause serious complications.
A 2018 study with data from over 300,000 people found that a person with type 1 or type 2 diabetes is at a higher risk of infection, including candidiasis, as compared to a person who does not have diabetes.11
Research is still going on to establish the exact link between the overgrowth of yeast and diabetes. It is believed to involve various factors, including:
- A weakened or compromised immune system
- Persistent yeast infections
- Presence of high blood sugar in yeast-friendly areas such as the vagina
It is especially necessary for people with diabetes to recognize the symptoms of vulvovaginal candidiasis because the infection can worsen more quickly in diabetics than in people without diabetes. Also, it is more challenging to treat infections in people with diabetes. Keep in mind that if an infection does not heal, it can cause various other diabetes-related complications as well.
Weakened Immune System
Having a weakened immune system makes it more likely to develop a yeast infection and also makes it more challenging to fight off such vulvovaginal candidiasis infections. For example, women who take certain medications like TNF inhibitors for autoimmune conditions like lupus or rheumatoid arthritis, or corticosteroids for asthma, are more likely than others to have an overgrowth of yeast.
Women with diseases such as cancer or HIV/AIDS, or even diabetes, or those who have had an organ transplant are at a greater risk of having recurring vulvovaginal candidiasis.12
In people with weakened immune systems, candida infections are also more challenging to treat and tend to return after treatment. It is important that people with weakened immune systems recognize the signs of such infections because candidiasis can prove to be life-threatening if it passes into the bloodstream and spreads to any vital organs.13
Poor Eating Habits
Eating foods that are very high in sugar is known to increase the risk of developing yeast infections. In fact, if you suffer from recurring yeast infections or vulvovaginal candidiasis, you may want to reflect on your eating habits. A poor diet that does not include enough iron or if you have a deficiency of iron (anemia), you become more prone to having candidiasis.14
A poor diet also increases the risk of obesity, which, in turn, increases the risk of yeast infections. Overweight or obese people have more areas of moisture and warmth in their skin folds, which may contribute to infections like candidiasis.
Doctors frequently recommend a healthy and well-balanced diet for people with recurring yeast infections. These including a lower intake of sugar, taking probiotics and increasing the amount of yogurt in their diet. A well-balanced, healthy diet can significantly decrease the risk of candidiasis.
Diagnosis of Vulvovaginal Candidiasis
Vulvovaginal candidiasis is easy to diagnose. Your doctor will first take down your medical history, including asking you about whether you have had yeast infections before. They will also enquire about your sex life and if you have ever had an STD/STI before.
Your doctor will also conduct a pelvic examination to examine your cervix and vaginal walls. They will also check the vagina for any external signs of infections. Depending on what your doctor sees, they may collect a sample of cells from the vagina. These cells are sent to a laboratory for further examination. If you have recurring yeast infections or have infections that don’t go away easily, your doctor may order more extensive diagnostic tests. In such cases, it could be possible that a different version of Candida is causing your infection. Your doctor will then also order a lab test to identify what type of Candida is causing your infection.15
Treatment of Vulvovaginal Candidiasis
Every case of candidiasis is different, which is why doctors suggest other treatments that best suit the individual case. The exact treatment also depends on the severity of the symptoms.
In cases of simple candidiasis, your doctor is likely to prescribe a one to a three-day course of an antifungal ointment, cream, suppository, or tablet. Some of the commonly prescribed medications for treating vulvovaginal candidiasis include:
- Fluconazole (brand name: Diflucan)16
- Clotrimazole (brand name: Lotrimin)17
- Terconazole (brand name: Terazol)18
- Miconazole (brand name: Monistat)19
- Butoconazole (brand name: Gynazole)20
However, even with simple vulvovaginal candidiasis, women should still follow up with their doctor after completing the course of the antifungal agent to ensure that the medication has worked.
If your symptoms of vulvovaginal candidiasis return within two to three months, you will need to again show your doctor.
In cases of complicated yeast infections, your doctor will follow a different course of treatment. Some of the signs that you have a severe case of candidiasis include:
- If there is severe swelling, redness, and itching that causes tears or sores in the vaginal tears.
- If you have experienced more than four yeast infections in one year.
- If your infection is caused by another Candida strain other than the more common Candida albicans.
- If you are pregnant.
- If you have HIV/AIDS.
- If you have a weak immune system from medication.
- If you have uncontrolled diabetes.
In such cases, the possible treatments for vulvovaginal candidiasis would include:
- Two or more doses of the antifungal fluconazole (brand name Diflucan).21
- A 14-day course of vaginal treatment through ointment, cream, or tablet.
- Long-term prescription treatment with fluconazole to be taken once a week for six weeks.
- Long-term treatment with a topical antifungal medication.
If you have recurring candidiasis, you may also need to see if your sexual partner has a yeast infection. It is best to use barrier contraception such as condoms while having sex, especially if you suspect either you or your partner has a yeast infection.
Your doctor is the best person to talk to about all the possible treatment options for vulvovaginal candidiasis.
Summing Up
Vulvovaginal candidiasis is a form of yeast infection that commonly affects women. Prompt treatment can help alleviate the uncomfortable symptoms within a week. It is essential to recognize the risk factors for vulvovaginal candidiasis to prevent such infections. Apart from prescription medications, there are various natural home remedies you can try to treat simple candidiasis. However, these may not be as reliable or effective as the prescribed medications. Some of the popular home remedies for candidiasis include:
- Tea tree oil cream
- Coconut oil
- Boric acid vaginal suppositories
- Garlic
- Plain yogurt taken orally or inserted into the vagina
- It is vital that you talk to your doctor before you try any natural remedies.
Remember, yeast infections like candidiasis can be contagious, and it is possible to pass on the infection during vaginal or oral intercourse. If you are concerned about any possible transmission, you should talk to your doctor about how candidiasis could be contagious. Remember, if left untreated, vulvovaginal candidiasis can be life-threatening in some instances.
- Sobel, J.D., Faro, S., Force, R.W., Foxman, B., Ledger, W.J., Nyirjesy, P.R., Reed, B.D. and Summers, P.R., 1998. Vulvovaginal candidiasis: epidemiologic, diagnostic, and therapeutic considerations. American journal of obstetrics and gynecology, 178(2), pp.203-211.
- Eckert, L., Hawes, S.E., Stevens, C.E., Koutsky, L.A., Eschenbach, D.A. and Holmes, K.K., 1998. Vulvovaginal candidiasis: clinical manifestations, risk factors, management algorithm. Obstetrics & Gynecology, 92(5), pp.757-765.
- 0857;year=2007;volume=25;issue=2;spage=175;epage=176;aulast=Jindal
- Jindal, N., Gill, P. and Aggarwal, A., 2007. An epidemiological study of vulvovaginal candidiasis in women of childbearing age. Indian Journal of Medical Microbiology, 25(2), p.175.
- Foxman, B., 1990. The epidemiology of vulvovaginal candidiasis: risk factors. American journal of public health, 80(3), pp.329-331.
- Odds, F.C., Webster, C.E., Mayuranathan, P. and Simmons, P.D., 1988. Candida concentrations in the vagina and their association with signs and symptoms of vaginal candidosis. Journal of medical and veterinary mycology, 26(5), pp.277-283.
- Parolin, C., Marangoni, A., Laghi, L., Foschi, C., Ñahui Palomino, R.A., Calonghi, N., Cevenini, R. and Vitali, B., 2015. Isolation of vaginal lactobacilli and characterization of anti-Candida activity. PloS one, 10(6), p.e0131220.
- Aguin, T.J. and Sobel, J.D., 2015. Vulvovaginal candidiasis in pregnancy. Current infectious disease reports, 17(6), p.30.
- Vagina, M., Vadge, A.A., Killing, B.V. and Killing, B.V., Cyclic vulvovaginitis.
- Seelig, M.S., 1966. The role of antibiotics in the pathogenesis of Candida infections. The American journal of medicine, 40(6), pp.887-917.
- Khosravi, A.R., Eslami, A.R., Shokri, H. and Kashanian, M., 2008. Zataria multiflora cream for the treatment of acute vaginal candidiasis.
- International Journal of Gynecology & Obstetrics, 101(2), pp.201-202.
- Carey, I.M., Critchley, J.A., DeWilde, S., Harris, T., Hosking, F.J. and Cook, D.G., 2018. Risk of infection in type 1 and type 2 diabetes compared with the general population: a matched cohort study. Diabetes Care, 41(3), pp.513-521.
- Anwar, K.P., Malik, A. and Subhan, K.H., 2012. Profile of candidiasis in HIV infected patients. Iranian journal of microbiology, 4(4), p.204.
- Marr, K.A., 2004. Invasive Candida infections: the changing epidemiology. Oncology, 18(14_Suppl_13).
- Galland, L., 1985. Nutrition and candidiasis. J. Orthomol. Psychiat, 14, pp.50-60.
- Ellepola, A.N. and Morrison, C.J., 2005. Laboratory diagnosis of invasive candidiasis. The Journal of Microbiology, 43(1), pp.65-84.
- Sobel, J.D., Wiesenfeld, H.C., Martens, M., Danna, P., Hooton, T.M., Rompalo, A., Sperling, M., Livengood III, C., Horowitz, B., Von Thron, J. and Edwards, L., 2004. Maintenance fluconazole therapy for recurrent vulvovaginal candidiasis. New England Journal of Medicine, 351(9), pp.876-883.
- Sawyer, P.R., Brogden, R.N., Pinder, K.M., Speight, T.M. and Avery, G.S., 1975. Clotrimazole: a review of its antifungal activity and therapeutic efficacy. Drugs, 9(6), pp.424-447.
- Stein, G.E., Mummaw, N.L. and Schooley, S.L., 1996. Prevention of recurrent vaginal candidiasis with weekly terconazole cream. Annals of Pharmacotherapy, 30(10), pp.1080-1083.
- Bradbeer, C.S., Mayhew, S.R. and Barlow, D., 1985. Butoconazole and miconazole in treating vaginal candidiasis. Sexually Transmitted Infections, 61(4), pp.270-272.
- Jacobson, J.B., Hajman, A.J., Wiese, J., Gandrup, P. and Forsström, S., 1985. A new vaginal antifungal agent–butoconazole nitrate. Acta obstetricia et gynecologica Scandinavica, 64(3), pp.241-244.
- Inman, W., Pearce, G. and Wilton, L., 1994. Safety of fluconazole in the treatment of vaginal candidiasis. European journal of clinical pharmacology, 46(2), pp.115-118.
Also Read:
- Cutaneous Candidiasis or Skin Candidiasis: Causes, Signs, Symptoms, Investigations, Treatment
- What is Esophageal Candidiasis: Symptoms, Causes, Treatment, Prognosis, Pathophysiology, Prevention
- What Is Candidiasis Hypersensitivity Syndrome & Why is it Difficult to Treat It?
- What Are The Presenting Features of Candidiasis in Men & How is it Treated?
