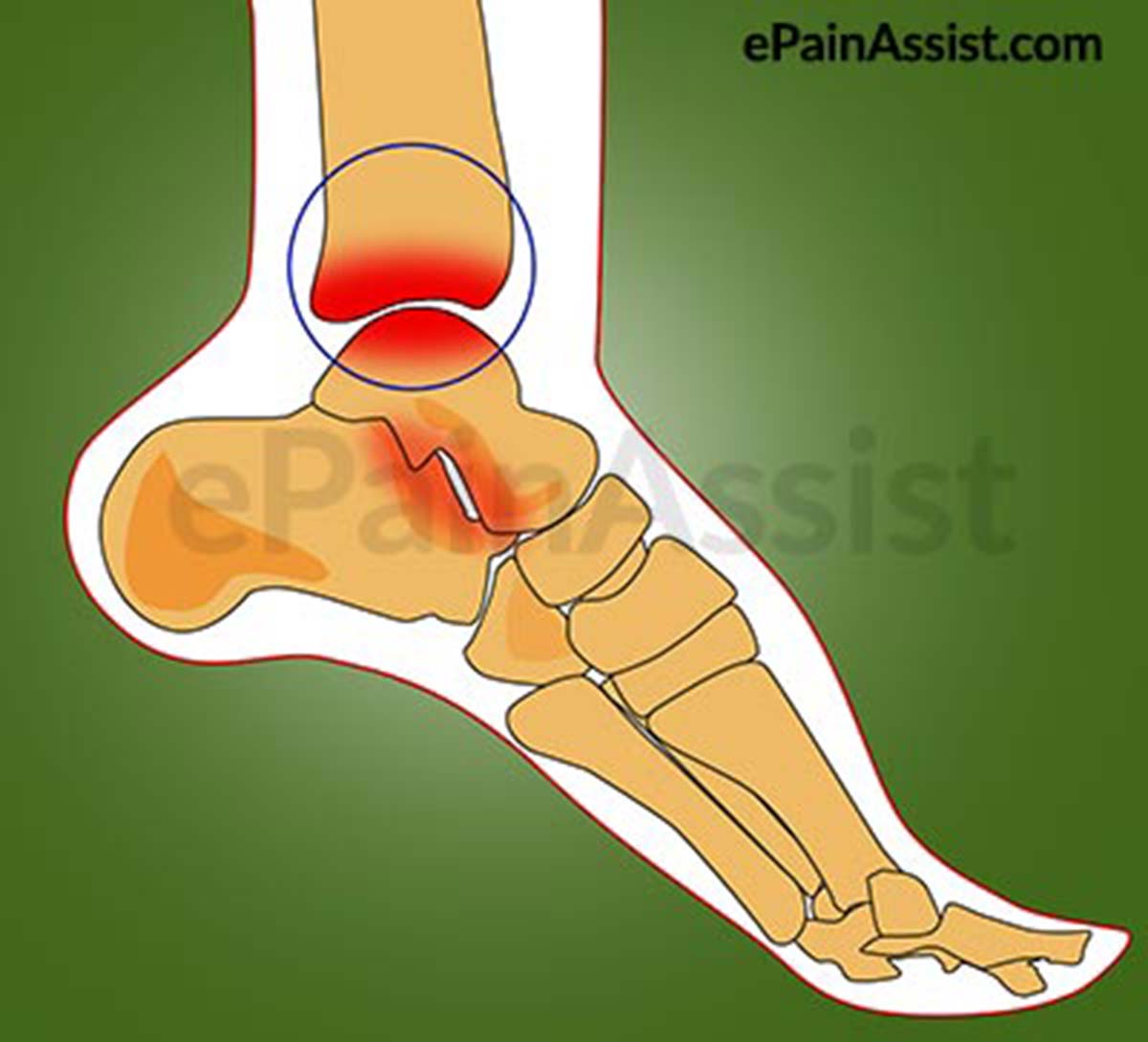
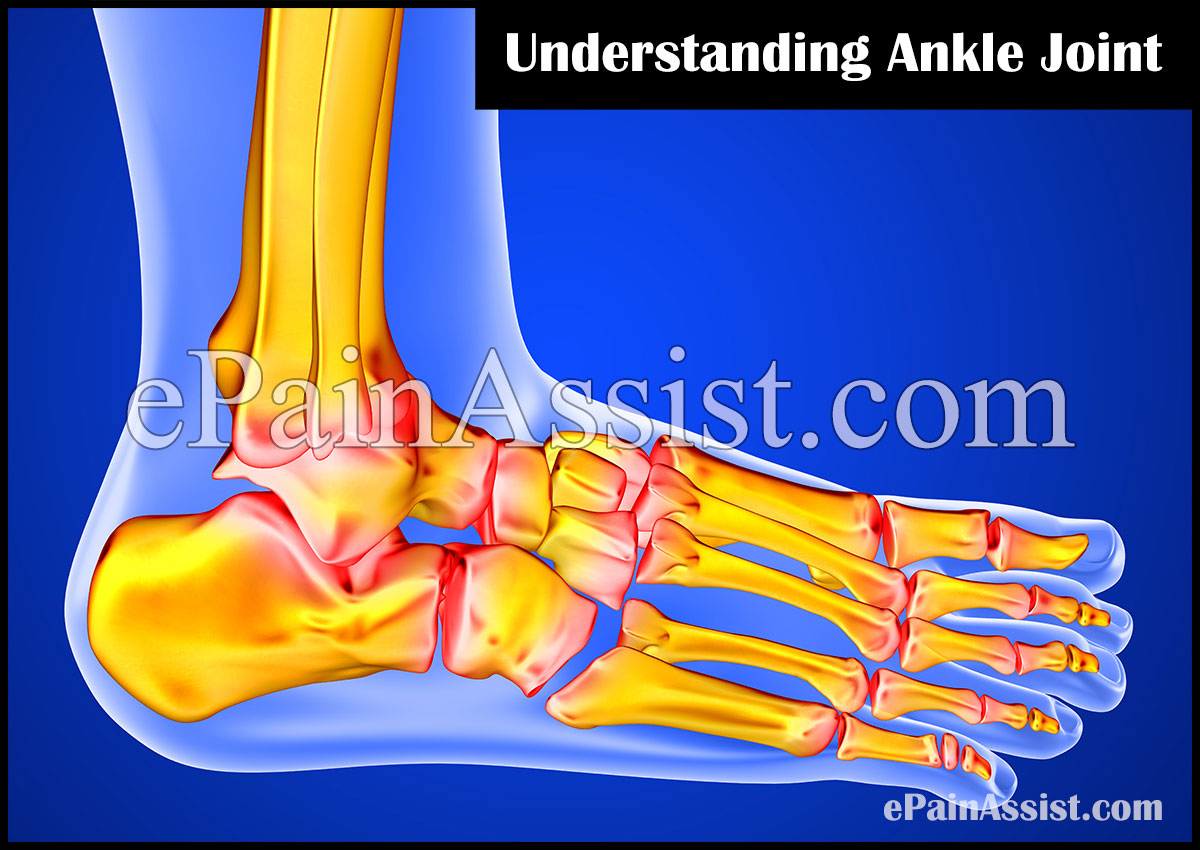
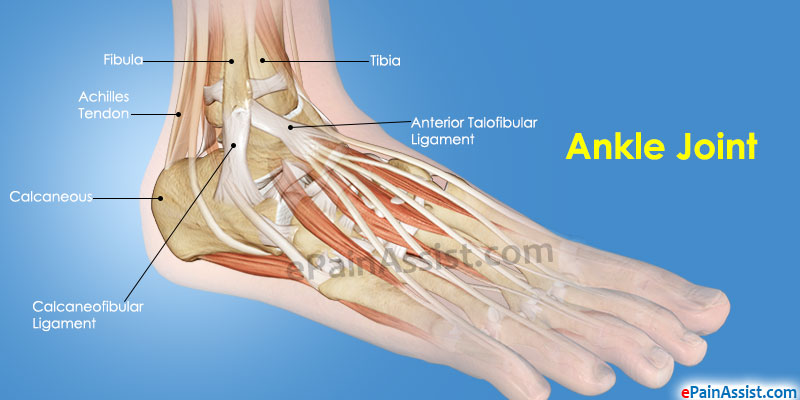
The function of the stomach is to digest food, which you have consumed. It is located in the upper left side of the abdomen. Abdominal Pain or Stomach Ache After Eating can occur from various causes. It could be from food poisoning, stomach flu or from something as simple as overeating. Abdominal Pain or Stomach Ache after eating can be severe or mild and its treatment depends on the cause of the pain.
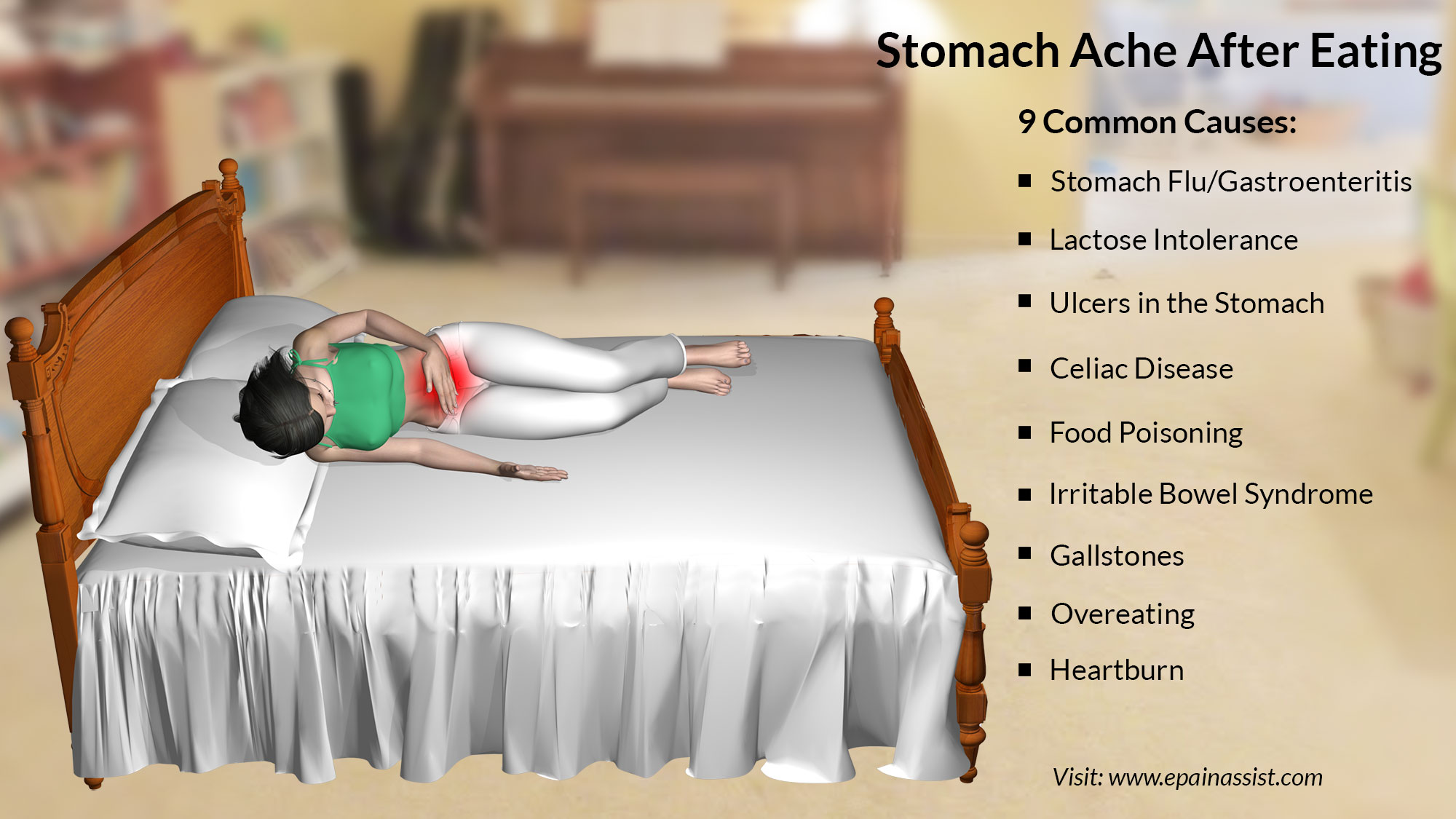
9 Causes of Abdominal Pain or Stomach Ache After Eating
- Stomach flu / Gastoenteritis
- Lactose Intolerance
- Stomach Ulcer
- Celiac Disease
- Food Poisoning
- Irritable Bowel syndrome
- Gall Stone
- Overeating
- Heartburn
Stomach Flu/Gastroenteritis: Cause of Abdominal Pain or Stomach Ache After Eating
This is a stomach infection resulting from consuming contaminated food by viruses.1 The symptoms are caused by rapid multiplication of viruses in stomach mucosal epithelial cells that follows virus attacking the entire adjacent layer of stomach mucosa. The condition is also known as stomach flu or gastroenteritis. Stomach flu is one of the common cause for abdominal pain or stomach ache after eating.1
Symptoms of Stomach Flu-
Investigations to Diagnose Stomach Flu
Physical Exam- Physical examination is performed to rule out
dehydration and low blood pressure that may have caused by vomiting and diarrhea.
Stool Exam- Detects rotavirus or norovirus.
Blood Test- In most cases white blood cell count is high.
Treatment of Stomach Flu
- Rest- Plenty of rest
- Antiviral Medications- Antiviral medication do not help and avoided.
- Antibiotics- Viral gastroenteritis doesn’t benefit from antibiotics.
- Fluid- Patient is advised to drink lot of non-carbonated liquid like water or juices.
- Anti-Diarrheal Medications- Imodium pills, Pepto-bismol or Kaopectine syrup.
- Anti-Spasmodic Medication- Prescribed for abdominal cramp and pains. Medications available as anti-spasmodic are Loperamide (Imodium), Belladonna, Dicyclomine and promethazine (Phenergan)
Lactose Intolerance As A Cause of Abdominal Pain or Stomach Ache After Eating
This is a condition where a person doesn’t have the enzyme lactase resulting in them becoming lactose intolerant. Person having lactose intolerance may get abdominal pain or stomach ache after eating milk products or consuming milk.
Symptoms of Lactose Intolerance
- Abdominal pain and cramping
- Diarrhea
- Nausea
- Abdominal bloating
- Flatulence
Investigations to Diagnose Lactose Intolerance
Stool Acidity Test- The acid concentration in stool is higher because of increased concentration of lactose acid in stool.
Lactose Tolerance Test- Lactose is converted to glucose in our body. Increased lactose intake causes increased blood sugar. Individual is asked to drink high concentrated lactose containing fluid. After 2 hrs, blood test is performed. No change of blood sugar level suggests lactose intolerance.
Hydrogen Breath Tests- Higher concentration of hydrogen ions are found in expired breath of patient suffering with lactose intolerance. The unabsorbed lactose ferments in bowel and produces excessive amount of hydrogen that gets absorbed. The excess hydrogen in blood is discharged in expired air that is absorbed in intestine
Treatment of Lactose Intolerance
Currently there is no specific treatment for lactose intolerance.
- Fluid- Drink adequate amount of water, apple juice or non-gaseous soft drink.
- Avoid milk product or any food that contains lactose.2
- Abdominal pain is treated with antispasmodics. You must consult physician before trying over the counter antispasmodics. Most common antispasmodics used are belladonna, Librium, dicyclomine (bentyl) and hyoscyamine (levsin).
Ulcers in The Stomach As A Cause of Abdominal Pain or Stomach Ache After Eating
Ulcers in the stomach can cause abdominal pain or stomach ache immediately after eating. Ulcers are erosions in the soft lining of stomach or intestines. Stomach ulcer is also known as gastric ulcer. In most cases stomach pain is also caused by ulcers in duodenum. Duodenum is a proximal part of small intestine. It is often difficult to differentiate gastric and duodenal ulcer by just clinical examination. The gastroscopy helps to diagnose site of ulcer either in stomach or duodenum. The peptic ulcer is the common diagnosis that suggests ulcer is either gastric or duodenal in origin. Food with high acid content irritates and aggravates the ulcers that causes pain in the abdomen after eating.
Symptoms of Peptic Ulcer or Stomach Ulcer
Abdominal Pain or Stomach Ache- Pain is burning in character and severe in intensity.
Abdominal Cramping- Pain like abdominal cramp is felt few minutes after eating.
Nausea- Occasional pain is associated with nausea.
Vomiting- Vomiting is rare but observed when abdominal cramps causes reverse peristalsis.
Black or Tarry Stools- The stool often turns into dark brown or dark chocolate color when stool is mixed with blood. The mucosal surface of ulcer starts oozing blood when ulcer is associated with erosion of gastric mucosa.
Investigations to Diagnose Peptic Ulcer or Stomach Ulcer
Blood Tests- Low hemoglobin concentration is observed in most cases of chronic ulcer because of prolong blood loss from eroded ulcer.
Stool Tests- Stools examination shows present of blood in stool.
Endoscopy- Endoscopy is an examination of stomach and duodenum using endoscope. Endoscope is a small tubular and flexible camera. Procedure is performed under sedation in surgical center. The long tubular thin camera is passed through the mouth into stomach and duodenum. The images of stomach and duodenal mucosa is observed over television screen. In most cases suffering with ulcer, ulcer is seen during the procedure.
CT Scan and MRI– The radiological examination like computerize tomography (CT scan) or magnetic resonance imaging (MRI) does not show ulcer but the study helps to rule out other causes of stomach pain and bleeding like cancer of stomach and intestine.
Ultrasound Study- Ultrasound study helps to see the stomach content and also observe bleeding ulcer.
Treatment of Abdominal Pain or Stomach Ache Due to Peptic Ulcer or Stomach Ulcer
You must see your physician if abdominal pain does not respond to antacid and pain continues after 24 hours.
Antibiotics- Antibiotics are prescribed if stomach content shows presence H. pylori bacteria.
Anti-Acid Medications- The ulcer is irritated by hydrochloric acid secreted by stomach mucosa. Antacids neutralizes the hydrochloric acid. The food intake causes increased secretion of histamine in stomach and histamine stimulates secretion of stomach acid. The stomach acid secretion is reduced by blocking action of histamine and production of histamine in stomach.
Antacids- Antacids neutralizes stomach acid and prevents irritation of ulcer that helps to reduce intensity of pain. The ulcer healing is also promoted by less acid in the stomach content. Antacids are available over the counter in most pharmacies. The antacids most often used for treatment of peptic ulcers are Alka-Seltzer, Milk of Magnesia, Maalox, Mylanta, Rolaids, Pepto-Bismol and Tums.
H2 Blocker- Histamine receptors are classified as H1 and H2 receptor. Stimulation of these receptor increases secretion of stomach hydrochloric acid. Medication that blocks H2 receptor causes less secretion of hydrochloric acid. H2 blocker prescribed to treat peptic ulcer are Nizatidine, Pepcid and Tagamet.
Proton Pump Blocker- Stimulation of H2 receptor initiates mechanism of proton pump to secret hydrochloric acid by stomach mucosa. There are medications that directly block the proton pump and stops production of hydrochloric acid in stomach. The drugs that blocks proton pump are Nexium, prevacis and Prilosec.
Celiac Disease Causing Abdominal Pain or Stomach Ache After Eating
Celiac disease is another common condition which can be the reason for abdominal pain or stomach ache after eating. This is an immune system reaction which occurs after consuming gluten.3 Gluten is a protein present in barley, wheat, malt, semolina and rye.
Symptoms of Celiac Disease
- Abdominal Pain- Pain is mostly observed following 1 to 2 hours after eating food. Pain intensity is moderate to severe. Pain is felt like burning and squeezing pain.
- Diarrhea
- Weight loss
- Dehydration
- Osteoporosis– osteoporosis is caused by lack of calcium and vitamin D. Osteoporosis causes multiple joint pain when patient is suffering with celiac disease.
- Fatigue
- Headache
- Acid reflux.
Investigations to Diagnose Celiac Disease
- Blood Tests
- Antibody Test- Increased level of antibodies are found in blood serum.
- Genetic Test- Genetic test is performed to evaluate gluten as the cause of disease.
- Endoscopy- Endoscopy is performed in outpatient surgery to examine stomach, small and large intestine. Patient is also given a choice of capsule endoscopy. Capsule endoscopy procedure involves swallowing of small camera that is capsule like in shape. The images are transmitted electronically and examined by gastroenterologist. The images give the impression of internal structure of stomach and entire intestine.
Treatment of Abdominal Pain or Stomach Ache Due to Celiac Disease
- Gluten Free Diet– Patient should follow a diet which is gluten free in order to avoid getting abdominal pain or stomach ache after eating.
- Corticosteroid Pills- Steroids pills like prednisone is prescribed to relieve the bowel inflammation.
- Vitamin Supplements.
- Calcium Pills.
Food Poisoning
Food poisoning occurs after consuming contaminated food and drinks. This is a very common cause of abdominal pain or stomach ache after eating stale foods or contaminated food and drinks. The symptoms are caused by the toxins that is present in contaminated food. The food when kept outside refrigerated and open get contaminated with bacteria and viruses. These organism produces toxins that is mixed with exposed food. The contamination of food by toxin is often caused by Campylobacter, Clostridium botulinum, salmonella Shigella, rotavirus, norovirus and Giardia lamblia.
Symptoms of Food Poisoning
Abdominal Pain and Cramps- Pain appears 1 to 2 hours after intake of food. Symptoms may last for 1 to 5 days.
- Diarrhea
- Nausea
- Vomiting
- Fever.
Investigations to Diagnose Food Poisoning
- Blood Tests- White blood cell count is elevated,
- Stool Tests- Stool examination isolates the cause of food poisoning.
- Specific stool test shows the presence of bacteria or viruses.
Treatment of Abdominal Pain or Stomach Ache Caused Due to Food Poisoning
- Rest- Patient is advised rest until symptoms are absent.
- Fluid- Drink lots of water or non-carbonated soft drink. Avoid alcohol.
- Fiber Diet- Increase intake of food containing fibers for next few days. Avoid fatty food.
- Antibiotics- Antibiotics are prescribed if the cause of food poisoning is bacterial infection. The bacterial culture and antibiotic sensitivity test helps to select the appropriate effective antibiotics.
Irritable Bowel Syndrome (IBSP): Cause of Abdominal Pain or Stomach Ache After Eating
Irritable Bowel Syndrome is a disorder of the large intestine and causes abdominal pain, cramping, bloating and gas after eating. The irritable bowel syndrome is a disease of large bowel. The cause of the intestinal mucosal irritation and inflammation is unknown. The stool examination and blood examination does not indicate cause is infection. The disease is thought to be caused by disruption of signals between brain and gastrointestinal system. Patient suffering with anxiety disorder or depression often shows symptoms of irritable bowel syndrome.
Symptoms of Irritable Bowel Syndrome
- Pain- Abdominal cramping and pain.
- Diarrhea- Multiple loose motion discharges stool mixed with mucus
- Flatulence and gas
- Constipation
- Food Intolerance
- Fatigue
- Insomnia
Investigations to Diagnose Irritable Bowel Syndrome
- Blood Tests- Blood examination is normal.
- Flexible Colonoscopy- The endoscopy procedure is performed to examine anus, rectum, sigmoid colon and entire large intestine. The images are observed over large television screen. The images show multiple inflammatory lesions in the large intestine.
- CT Scan and MRI- Examination is performed to rule out cancer related diseases.
- Lactose Intolerance Tests- Test is frequently positive.
Treatment of Abdominal Pain or Stomach Ache Caused Due to Irritable Bowel Syndrome
- Diet- Dietary changes may help to reduce symptoms.
- Diet should include fiber or fiber supplements.
- Patient is advised to eliminate gas forming foods.
- Avoid food that contains gluten
- Fluid- Patient is advised to drink plenty of fluid to compensate loss of fluid because of daily episodes of multiple diarrhea.
- Antidiarrheal Medications- Prevalite, Colestid and Welchol
- Anticholinergic Medications- Prescribed for abdominal cramps. Anticholinergic Medication prescribed is Bentyl.
- Antidepressant medications- Prozac, Imipramine, desipramin or nortriptyline.
- Regular exercise
- Sleep- Patient is advised to sleep for minimum 6 to 7 hours every day.
Gallstones Can Cause Abdominal Pain or Stomach Ache after Eating
Stones in the gallbladder are formed upon hardening of the digestive fluids. Presence of gallstones causes excruciating abdominal pain or stomach ache after eating.
Symptoms Caused By Gallstone Disease
Abdominal Pain- Pain is mostly localized over right upper abdomen. Pain occasionally refers to right shoulder.
Jaundice- The bile stone blocks the gall bile duct. Bile duct carries bile produced by bile duct into intestine that helps to digest food. The gall bladder gets absorbed into blood once gall bladder is filled with bile. The bile content in blood causes symptoms of jaundice. The symptoms of jaundice include yellow eye and skin as well as urine yellow discoloration.
- Yellow dark urine
- Nausea and vomiting
Investigations to Diagnose Gallstone Disease
CT scan and MRI- The CT scan and MRI shows the gall stone in gall bladder as well as swelling of bile duct. CT scan MRI also helps to rule out any cancer mass in the liver, intestine. gall bladder or bile duct.
HIDA scan- Hepatobiliary Iminodiacetic Acid (HIDA) scan shows the image of liver, gallbladder, biliary tract and small intestine. The scan shows presence of bile duct in gall bladder as well as in bile duct. Scan also shows the thickness of gall bladder and any signs of cancer.
ERCP (Endoscopic Retrograde Cholangiopancreatography)- ERCP is a procedure performed in surgical center under sedation. Endoscope is a tubular camera of diameter 2 to 5 cm. The camera is passed through mouth into intestine and then into opening of bile duct. At this time dye is passed to take the dye image of bile duct and pancreas. The camera has lens at the tip of the tube and images are transmitted over large television. Gastroenterologist then can see bile stone and also assist to remove bile stone by widening the bile duct passage.
Blood Tests- Shows increase level of bilirubin
Treatment for Gallstone Disease
- Rest
- Diet- Fiber rich diet is advised.
- Ursosdeoxycholic Acid- Individual suffering with repeated gall stone and following surgical removal of stone are treated with Ursosdeoxycholic acid. Ursosdeoxycholic acid prevents formation of gall stone.
Surgery-
- Open Cholecystectomy- Skin incision is taken to remove gall bladder.
- Laparoscopic Cholecystectomy- The endoscope is passed into abdominal cavity and gall bladder is removed through very small incision. is done for larger stones. There are also medications available which disintegrate the stones.
- Lithotripsy- Ultrasound treatment is used to break the bile stone.
- Ursosdeoxycholic Acid- Ursosdeoxycholic acid lowers the cholesterol content of bile.
Abdominal Pain or Stomach Ache Caused Due to Overeating:
This is a condition where an individual consumes excess food than one needs or expends. Eating more than required or eating too fast results in indigestion, this in turn results in pain in the abdomen after eating.
Symptoms Caused By Overeating
- Abdominal pain and discomfort
- Indigestion- Feeling of nausea and abdominal distension
- Abdominal distension
- Vomiting
- Flatulence
Treatment of Overeating
Rest
Antacids
Antispasmodics- Antispasmodics are prescribed if pain is severe and intolerable.
Eat Small Portions- It is better to avoid abdominal pain that may cause from over eating. Thus, eat less quantity of healthy diet. Eat your meals on proper time.
Hydration- Drink lots of water to keep yourself hydrated.
Activities and Improve Digestion- Engage in mild activity, such as walking after eating, especially after large meal to help with digestion.
Heartburn Can Cause Abdominal Pain or Stomach Ache After Eating
Heartburn is felt as a burning sensation below the sternum and causes pain in epigastrium (just below sternum) and stomach after eating. Heartburn is also known as GERD (Gasto-esophageal reflux disease). The stomach content or juice containing acid regurgitate into lower 1/3rd section of esophagus and causes irritation of mucosal membrane resulting in ulcer formation. Such condition causes severe abdominal pain or stomach ache after eating.
Symptoms of Heartburn
- Abdominal Pain- Pain is mostly localized behind lower end of sternum and upper abdomen. Pain is often severe and continuous. Pain is felt like burning and squeezing pain.
- Nausea
- Hematemesis- Rarely patient may vomit or spit stomach mucosa that contains spots of blood.
- Belching- Occasional individual emits stomach gas through mouth that contain stomach juice and causes acidic taste.
- Acidic stomach juice regurgitation in mouth
Investigations to Diagnose Heartburn
Radiological Studies- X-ray, CT scan and MRI images are examined to rule out cancer or several other gastrointestinal diseases.
Blood Examination- Most blood examination results are normal
Endoscopy- Esophagus and stomach examination is performed using gastroscopy. The procedure is known as esophagascopy and gastroscopy. The images of esophagus shows inflamed mucosal membrane, mucosal erosion or ulcer.
Esophageal Motility Test- Test shows abnormal esophageal muscle contraction and peristalsis.
Ambulatory Acid (pH) Probe Tests- Patient suffering with celiac disease may show abnormal esophageal pH.
Treatment of Heartburn
Antacids- Alka-Seltzer, Maalox, Pepto Bismol, Tums and Mil of magnesia.
H-2 Receptor blocker- Axid, Pepcid, Tagamet and Zantac
Proton Pump Inhibitor- Prilosec, Prevacid and Protonix
Avoid Fatty and Spicy Food- Small meals every couple of hours are better than consuming 3 heavy meals a day.
Reduce consumption of coffee, tea and alcohol
Smoking- Smoking should also be avoided.
Other Causes of Abdominal Pain or Stomach Ache After Eating Are:
When Should I See My Physician For Abdominal Pain?
You should see your physician as soon as possible if abdominal pain does not respond to antacids and lasts for more than 48 hours. Also you must see your physician, if you are suffering from severe abdominal pain accompanied with blood in the stool, vomiting and feeling dizzy. You should visit ER during weekend and after physician office hours if your primary care physician is not available.
References
How can you tell the difference between stomach flu and food poisoning?
Rosen DS., Health News. 2001 Feb;7(2):10.
Lactose intolerance: what is a correct management?
Santos GJ1, Rocha R1, Santana GO2., Rev Assoc Med Bras (1992). 2019 Feb;65(2):270-275. doi: 10.1590/1806-9282.65.2.270.
Pediatric Celiac Disease – A Review.
Meis M1,2, Adamiak T1,2., S D Med. 2018 Dec;71(12):559-564.
Irritable bowel syndrome: a review of the general aspects and the potential role of vitamin D.
Barbalho SM1,2, Goulart RA3, Araújo AC1, Guiguer ÉL1,2, Bechara MD1.,
Expert Rev Gastroenterol Hepatol. 2019 Apr;13(4):345-359.
Also Read: